INTRODUCTIONThe benign paroxysmal positional vertigo (BPPV) is a common syndrome, and it corresponds to a 17% of patients complaining of dizziness as a main symptom(1,2). It was first described by Barany and defined by Dix and Hallpike as a short-term vertigo and paroxysmal that arises when head remains in a certain position. BPPV can have different etiologies, but the idiopathic way is the most frequent, with around 50 to 70% of the cases(2). It is auto-limited developed, from weeks to months, and it does not respond to antivertigo drugs(3,4). Therapy consists of canalith repositioning maneuvers, associated or not with Vestibular Habituation Training, which represents favorable responses in 70 to 90% of the cases(7).In a short percentage of patients who do not respond to a conservative treatment, it can be proposed surgical corrections such as singular neurectomy or occlusion of posterior semicircular canal(8,9).
During the late decades, the best knowledge and effectiveness on canalith repositioning maneuvers has turned BPPV a vestibular syndrome considered as a simple clinical procedure. Nevertheless, some syndromes arising from CNS that mimic BPPV presenting good response to canalith repositioning maneuvers are described. Some Central Nervous System Diseases (CNS) can clinically develop as a syndrome that holds positional nystagmus, but they usually have different feature from those found in BPPV. The diseases that can develop in this way are cerebellopontine angle tumor, Arnold-Chiari malformation, multiple sclerosis, brainstem contusion or vascular accident(10,11). The presence of such CNS syndromes makes us to disregard them before doing a definite diagnosis of BPPV, even when there are good responses to repositioning maneuvers.
TARGET The target of this study is to report a case of a non-benign paroxysmal positional vertigo (nBPPV) with clinical features of BPPV, in which patient presented symptom improvement after Eppley maneuver, whose investigation revealed CNS involvement, and also to discuss the used diagnosis procedures base on mentioned literature.
CASE REPORTA 43-year-old male patient searched for ENT service at Hospital das Clínicas - FMUSP complaining of rotatory dizziness for 3 years with crisis lasting for up to 20 minutes, followed by nausea, especially when lying on the left side and when turning head to left. Patient also complained of acute and continuous tinnitus in both ears beginning at the same time, hypoacusis at the left side for 5 years and occasional cervicalgia (pain in the neck) with no complaint of headache. Patient had cinarizine and flunarizine with no improvement after he was medicated with Ginkgo-biloba, 160mg per day, and crisis frequency was reduced.
In the initial evaluation, patient presented general ENT exam, cranial pair exam in normal condition, non-visible spontaneous and semi-spontaneous nystagmus, Romberg Unterberger-Fukuda e Babinsky-Weil tests with no alterations and cerebellar tests with eumetria and adiadochokinesia. In that time, Dix-Hallpike test presented positive result to the left side with horizontal-clockwise rotatory nystagmus and dizziness, with latency for few seconds and vestibular habituation with Repositioning maneuver suggesting canallithiasis of posterior semicircular canal. Epley maneuver was performed and resulted in vertigo disappearance up to the last evaluation. As a routine, laboratory exams, cervical radiography, audiometry and eletronystagmography were also required.
Results from hemogram, triglycerides, fasting glycemia, VDRL and FTABS, thyroid hormones tests were in normal condition. Total cholesterol was 213 mg/dl and LDL was 153mg/dl. Radiography from cervical column showed inversion of cervical lordosis, discal space reduction between C5-C6 and osteophytosis on C5 and C6. Tonal audiometry (Picture 1) presented bilateral sensorineural hearing loss with reduction in high and low frequencies and worse threshold to left. Acoustics immittance presented curve type A, estapedial reflexes with normal threshold. Eletronystagmography confirmed regular calibration, absence of spontaneous nystagmus, pendular tracking type I, optokinetic nystagmus at cervical torsion to left. Caloric tests performed with water, according to Fitzgerald and Hallpike´s criteria, showed alteration on post-caloric rhythm in all tests and also labyrinth preponderance of 45% to right.
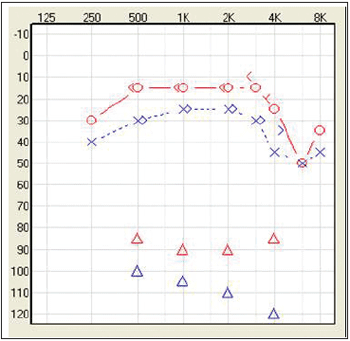
Picture 1. Audiometry tonal curve shows asymmetric, the worst left.
Regarding the findings of audiometric and ENG exam, research of brainstem auditory potential (BAP) and cervical column tomography were required.
In the BAP exam (Picture 2) one might find latency of wave V and interval I-V in the superior limit of normality in the right ear; increase of latencies of waves III and V and of the intervals I-III and I-V; scarce morphology especially of wave III in the left ear. These findings suggest retrocochlear disease to the left and do not disregard retrocochlear dysfunction to the right.
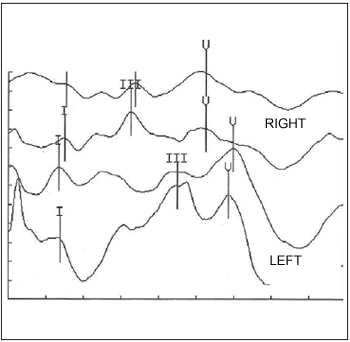
Figure 2. PATC suggests affection retrococlear left.
Cervical column tomography presented uncoarthrosis signs in C5 and C6 and normal craniovertebral transition.
Due to BAP result, it was required cranioencephalic magnetic resonance imaging.
Magnetic resonance imaging (Pictures 3 and 4) showed infiltrative lesion affecting white and gray substance on cerebellar hemisphere and worm affecting right cerebellar hemisphere, but in less grade, heterogeneous texture and cerebellar sulcus distinction. There was hypersignal at diffusion. Lesion caused compression and deformity on ventricle IV.
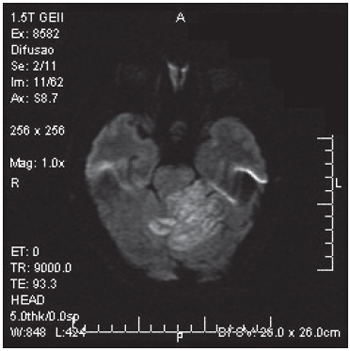
Picture 3. Magnetic resonance imaging-diffusion. Injury widens cerebellar cell layers, partially characterized. Displacement of the mesencéfalo with partial obstruction of the ventricule IV.
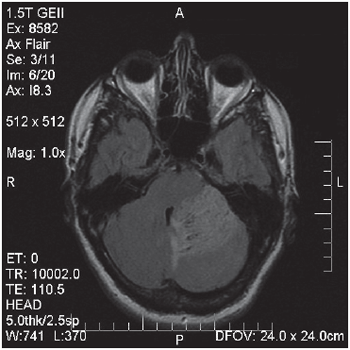
Picture 4. Magnetic resonance imaging with Flair technique. Presence of infiltrative cerebelar injury to the left with an unspecified hypersignal.
Stean and Press technical spectroscopy, single voxel showed reduction on the relations n-acetyl aspartate/creatinine, choline/creatinine and mioinosito/creatinine in normal condition. Lactate peak was high. By the high signal of diffusion, the exam suggests lymphoma or medulloblastoma, though there was no sign of choline peak in the spectrography, and as a differential diagnosis it suggests glioma or Lhermitte-Duclos disease.
Patient, with no symptoms, was sent to Neurosurgery service where he remains with no dizziness and under Expectant Management.
DISCUSSION BPPV is one of the most common causes of peripheral vertigo, and posterior canal involvement is the most frequent. Its diagnosis is based on clinical history and on physical exam and it is confirmed by Dix-Hallpike test.
Basically, its clinical history is vertigo episodes depending on position of the head acquired by the patient, and they are improved spontaneously after few seconds with no concomitant hearing alteration. In Dix-Hallpike maneuver, one might observe the presence of nystagmus and/or vertigo when patient acquires head position. Latency, exhaustion and habituation of nystagmus and vertigo are features of BPPV.
Besides such typical occurrences, nystagmus direction should be observed, what suggests the affected semicircular canal. CNS pathologies can develop positional nystagmus or vertigo due to compression or traction of vestibular nerve. In more extensive focal diseases, failure on cerebellar control and involvement of vestibular nuclei should be considered. For being a frequent syndrome, one cannot assume the possibility of BPPV excludes the presence of CNS involvement(10).
Some findings on Dix-Hallpike test such as long-lasting nystagmus (over 1 minute), vertigo or nystagmus present on both sides of the test, absence of latency or presence of nystagmus in a non-expected direction are not considered typical and should be more deeply investigated. History data to hearing loss, to tinnitus and concomitant headache and/or alterations on audiometric exam present in around 25% of the cases with no CNS alteration should be considered(11).
Literature describes several cases of non-typical positional vertigo associated with CNS disease, though only 6 patients who presented typical condition of BPPV are described. One of them improved from symptoms spontaneously and two improved after canalith repositioning. The final diagnosis of one of these cases was lipoma of right cerebellopontine angle and left posterior canal BPPV, what suggests that diseases were not related but an incidental finding(12,13).
The worry to submit patients to an otoneurological evaluation which covers audiometric and electronystagmographic evaluation, besides anamnesis and clinical exam, presented extremely useful in these cases. The presence of asymmetric hearing loss and dysrhithmia of post-caloric nystagmus led to a more deeply investigations through researches of Brainstem Auditory Evoked Potential and cranioencephalic magnetic resonance imaging, which allowed the identification of a lesion of a cross striated pattern with thickening of cerebellar cell layers, suggesting Lhermitte-Duclos disease.
Lhermitte-Duclos disease was first described in 1920(14). It is a rare and slow-development cerebellar disease; sometimes it is considered neoplasy, sometimes congenital malformation. Its histochemical features suggest hamartoma. The hypotheses that are compatible with such disease are: it is slow, no malignization records, frequent recurrent after partial resection and its association with Cowden disease (multiple hamartomatosa)(15).
CONCLUSIONThis case confirms the performance of observation and investigation of the cases with initial diagnosis of BPPV, even if they present good development after canalith repositioning maneuvers. For being a kind of syndrome, searching an etiological factor is essential in all BPPV cases.
REFERENCES1. Katsarkas A. Benign Paroxysmal Positional Vertigo (BPPV): idiopathic versus post-traumatic. Acta Otolaryngol 1999, 119(7):745-9.
2. Parnes LS, Agrawal SK. Atlas J Diagnosis and Management of Benign Paroxysmal Positional Vertigo. CMAJ 2003, Sept 3, 169(7):681-693.
3. Asawavichianginda S, Isipradit P, Snidvongs K, Supiyaphun P. Canalith repositioning for benign paroxysmal positional vertigo: a randomized, controled trial. Ear Nose Throat J 2000, 79:732-4.
4. Fujino A, Tokumasu K, Yosio S, et al. Vestibular training for benign paroxysmal positional vertigo: its efficacy in comparison with antivertigo drugs. Arch Otolaryngol Head Neck Surgery 1994, 120:497-504.
5. Epley JM. The canalith reposiotioning procedure for the treatment of benign paroxysmal posicional vertigo. Otolaryngol Head Neck Surg 1992, 107:399-404.
6. Semont A, Freyss G, Vitte E. Curing the BPPV with a liberatory maneuvre. Adv Otorrinolaryngol 1988, 42: 290-293.
7. Steenerson RL, Cronin GW. Comparison of the canalith repositioning procedure and vestibular habituation training in forty patients with benign paroxysmal vertigo. Otolaryngol Head Neck Surg 1996, 114:61-4.
8. Gacek RR. Singular neurectomy update II: review of 102 cases. Laryngoscope 1991, 101:855-62.
9. Parnes LS, McClure JA. Posterior semicircular canal oclusion for intractable benign paroxysmal positional vertigo. Ann Otol Rhinol Laryngol 1990, 99:330-4.
10. Dunniway HM, Welling DB. Intracranial tumors mimicking benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 1998, 118(4):429-36.
11. Montero EH, Rodrigo JJF, Garcia FM, et al. Vertigo posicional paroxístico no benigno. Acta Otorrinolaryngol Esp 2003, 54:591-4.
12. Watson P, Barber HO, Deck J, Tebrugge K. Positional vertigo and nystagmus of central origin. Can J Neurol Sci 1981, 8(2):133-7.
13. Lyn S, Brey R. Benign paroxysmal positioning vertigo with indeterminate cerebellar lesion: case report. J Am Acad Audiol 1993, 4(6):384-91.
14. Williams DW III, Elster AD, Ginsberg LE, Stanton C. Recurrent Lhermitte - Duclos Disease: report of two cases and association with Cowdens disease. AJNR 1992, 13:287-290.
15. Smith RR, Grossman RI, Goldberg HI, Hackney DB, Bilaniuk LT, Zimmerman RA. MR imaging of Lhermitte - Duclos disease: a case report. AJNR 1989, 10:187-189.
1. Medical Specialist in Otolaryngology (Employee Medical Sector of Otoneurology Discipline of Otorhinolaryngology, HCFMUSP).
2. Doctor of Medicine (Assistant Doctor, Sector of Otoneurology Discipline of Otorhinolaryngology, HCFMUSP).
3. Medical Specialist in Otolaryngology (Student's Special Post-Graduate Discipline of Otorhinolaryngology, Hospital of the FMUSP).
4. Doctor of Medicine (PhD and Assistant Chief of the Division of Otoneurology Displina of Otorhinolaryngology, Hospital of the FMUSP).
5. Medical Specialist in Otolaryngology (Medical Complementation of the Stage for a DSB in HC-FMUSP).
Discipline of Otorhinolaryngology, Hospital of the FMUSP Service Professor of Aroldo Miniti.
John E. Greters
Mailing address: Department of Otolaryngology, HCFMUSP - Rua Dr. Enéas de Carvalho Aguiar, 255 to 6 floor - Room 6021 -- CEP 05403-000 - Sao Paulo / SP - Brazil - Fax (11) 3088-0299 - E-mail: gretersorl@ig.com.br
This article was submitted in Management System Publications in the R@io 3/5/2006 and approved on 21/8/2006 11:04:20