INTRODUCTIONFew surgical procedures can rival the efficiency of modern mastoidectomy as a life-saving procedure.
It is important for the new generation of otologists to be cognizant of the origins of mastoidectomy as well as the difficulties our predecessors encountered and the solutions they devised to improve otologic surgery.
Before the mid-19th century, mastoidectomy was performed only sporadically and in most cases as a desperate attempt to save the lives of people suffering from complications of infectious otitis. Mastoidectomy did not become part of otological practice until about 1870. Before that time, patients presented to "barber surgeons" with red, warm, and painful abscesses behind the ear that were occasionally drained through an incision. This procedure was described by Lucas van Leyden in 1524 (Figure 1).
The drainage of acute abscesses became a common procedure at the beginning of the 20th century, within the pre-antibiotic era.
Francis A. Sooy (1915-1986), a renowned surgeon from San Francisco, said that until 1940, he frequently completed his patient appointments and then crossed the street to the surgery room to "drain a couple of acute mastoiditis" (1) (Figure 2).
As treatment for infectionMastoidectomy was developed as a method for draining purulent secretions from the infected mastoid cavity. Throughout history, many surgeons have suggested (even without supporting documentation) that such abscesses should have been treated with mastoid surgery rather than by drainage. The Greek physician Galen (AD 129-217), among others, recognized the importance of draining an infected ear. In his writings, he suggested that otorrhea was beneficial for the infected ear because it allowed the drainage of purulent secretions from the ear and recommended against any procedure intended to impede otorrhea.
Adam Politzer (2) interpreted Galen's writings to mean that Galen had already been removing carious bone from infected mastoids. However, Lusting and Cols (3) found no proof of this when they revisited Galen's work. Politzer may have deliberately misrepresented Galen's recommendation to allow purulent secretions to drain from the ear in order to justify mastoidectomy to the conservative medical community.
Galen is considered to be the founder of experimental physiology. He based his work on an understanding of anatomy; however, this understanding was gained from studies of dissected animals rather than from humans (4-7).
The first documented surgical incision to drain an infected ear was described by the French physician Ambroise Paré in the 16th century (8-11). Paré is credited with recommending drainage to François II, King of France, in 1560 (12). The king died of ear infection soon after; he did not undergo surgery because his mother, Catherine de Medicis, would not allow it (13).
The first documented recommendation of mastoidectomy was found in the writings of Johannes Riolanus the Younger from 1671.
Riolanus was an anatomist at the University of Paris. He then became a medical professor, whereas his father with the same name was the Director of the Faculty of Medicine of Paris. In many of his writings, Riolanus recommended mastoidectomy unless the surgical procedure would endanger the life of the patient: "If an intolerable and throbbing inflammatory pain fills and obstructs the release of purulent secretion from the head, an incision in the posterior region of the head might be the only solution" (14, 15).
In his text Anthropographia, Riolanus describes the procedure as "a small and narrow incision that gradually expands to the carious bone with small depressions like cells of a honeycomb" (16).
The credit for performing the first mastoidectomy for the removal of purulent secretions went to Jean-Louis Petit. Unlike his predecessors, Petit clearly established the procedure as a method for drilling the bone with the deliberate intent of removing pus. Petit (1674-1750) was an 18th century French surgeon who received his surgical degree in 1700 and became a member of the Royal Academy of Sciences in 1715 (Figure 3). Subsequently, in 1731, the king of France founded the Royal Academy of Surgery and recommended Petit as its first director. According to his bibliography presented at the Academy, his great renown stemmed from his experience with several surgical procedures, including the surgical management of bone diseases.
Petit worked in a military hospital beginning in 1692 and mentored military surgeons throughout Europe. During this period, he created a type of tourniquet for which he became famous. This was applied as a "screw tourniquet" and was used to contain hemorrhage before and after surgical procedures. Petit is credited with a level of expertise in mastoid surgeries unequaled in his time (17).
Rather than simply making a hole in the bone, which led to the formation of a persistent fistulous tract, Petit advocated a deliberate search for purulent secretions in the mastoid. Petit described mastoid surgery in his "Traité des Maladies Chirurgicales," where he wrote, "the walls of bone cavities cannot expand when filled with purulent secretions; while there, the pus remains completely encapsulated by compression and forms caries that cannot be reached by any topical application, often inaccessible even by surgery" (18-19). Petit described using a chisel to remove the bone along the existing fistula. He then recommended drilling an intact mastoid. Petit advised that if signs of inflammation indicated an abscess under the cortical mastoid, the physician should not to hesitate to remove the external wall of the mastoid and open it by drilling with a chisel and hammer. He thought that trepanation was justified because drainage might result in decompression before the purulent secretions could spontaneously drain via perforation of the external wall, thus limiting the course of the disease. Petit observed that the patient would recover immediately upon the removal of the external wall of the mastoid by means of a chisel and hammer, as follows: "These abscesses may remain and develop in the diploic layer for a long time and lead to death of the patient. However, early abscesses may be opened without waiting for them to destroy the bone. This is always risky for the patient as purulent secretions do not drain spontaneously and other causes may lead the disease to become complicated and fatal."
This treatment for mastoiditis was very different from the method accepted at the time, which involved topical applications of different substances. Petit claimed that this was why his treatment method was not accepted among his colleagues. He also described the resistance that he encountered when he attempted to make incisions and open the skull when no signs of external injury were observed.
As treatment for tinnitus or deafness Historically, mastoidectomies were normally performed to treat infections. However, mastoidectomies were also carried out for other purposes, particularly for the treatment of deafness and tinnitus, during various periods. These cases in which the procedure was performed to treat conditions presenting no clear indications for mastoidectomy were responsible for the unpopularity of this procedure.
J. L. Jasser, a Prussian military surgeon of the 18th century, made a retroauricular incision into the mastoid of a soldier suffering from a retroauricular abscess. He found a large hole in the mastoid cells. While irrigating this area with a syringe inserted into the incision, Jasser observed a significant amount of purulent material exiting from the external ear canal and nose.
Three weeks later, the patient reported improvement in his hearing (20). Although Jasser performed the procedure to treat infection, this episode encouraged him to try this operation to treat hearing loss due to mastoiditis and, subsequently, deafness due to any cause.
Sir Charles Ballance (18) credited Johannes Riolanus the Younger with recommending mastoidectomy to treat tinnitus. Riolanus wrote in the book Anthropographia that "The noise developed as a consequence of a fresh air stream that was retained inside the ear. How could we release this air? Certainly, there was no other way except drilling the mastoid."
Further improvement in mastoidectomy was critically compromised by the death of Baron Johann von Berger, a Danish court physician, in 1833. According to several authors (13,18-21), the 68-year-old physician had suffered for many years from tinnitus and deafness and required mastoidectomy. Von Berger underwent surgery and died 2 weeks later from meningitis. This event brought attention to the possible complications of this procedure and was cited by its opponents for many years.
The combination of complications and surgery for questionable indications decreased the popularity of mastoidectomy. Nevertheless, the development of this procedure by many surgeons furthered their understanding of the pathophysiology of the disease and the effect of mastoidectomy.
The importance of mastoidectomy and its inherent potential are summarized in the optimistic feelings of Jasser, who wrote, "No good book or any good thing shows at first its best side." (13).
Retroauricular incisionInterest in mastoid surgery did not fade completely in the early 19th century. However, most surgeons performed mastoidectomy only in certain situations and for specific indications. In 1838, J. E. Dezeimeris wrote that reports describing complications due to mastoidectomies should be collected before the procedure was definitively abandoned. In his article "L'Éxperience," published in the Journal of Medicine and Surgery, Dezeimeris wrote, "Those who oppose the procedure of drilling the mastoid process reported that surgical complications that could possibly occur due to this procedure could be worse than the disease itself. Moreover, a simple drainage could also be efficient" (22).
The question was whether mastoidectomy was inherently risky or whether the real danger was the injuries that might occur in the inner ear before the removal of the purulent secretions.
Dezeimeris described several cases of successful surgeries as well as cases in which complications were referable to contraindications or in which negative outcomes were caused by the course of the disease itself. He noted that the poor outcomes in these cases did not reflect the safety or effectiveness of the surgical procedure (22-23).
A new era for mastoidectomy was inaugurated by Sir William Wilde with his introduction of the eponymous retroauricular incision (Figure 4).
Wilde was born and lived in Ireland. Building on his father's career, he entered the practice of medicine (Figure 5). As a young surgeon inspired by the need for infrastructure for the medical and surgical care of non-privileged individuals, Wilde founded a small hospital in Dublin that initially aimed to meet the ophthalmologic and otologic needs of the poor. The privileged classes learned of his talent and expertise from their servants. The hospital subsequently moved to larger facilities, and for a while it was the only facility in England to perform ear surgeries. Wilde published Aural Surgery, a series of essays about the most common diseases of the ear, and continued his leadership role until his death in 1864. His personal life was equally exciting, involving numerous lovers and illegitimate children; his own temperament was also rude and eccentric (24-25). Perhaps one of the most significant ironies of this pioneering surgeon's life was his difficult relationship with his famous son, the writer Oscar Wilde, who suffered from chronic otorrhea and died from meningitis caused by otitis.
Wilde stated that mastoiditis results from "what was originally otorrhea of the mucosa and occurs when the inflammation of the periosteal membrane reaches the bone." He recommended that physicians not hesitate to make an incision at least 1 inch long when "the mastoid process enlarges or even in the presence of a slight floating sensation." For safe separation of the periosteum, the head should be placed on a fixed support and the scalpel inserted to the bone. Because of the degree of inflammation, it is often necessary to insert the scalpel an inch deep. The relief and improvement are immediate even when the infection is not found.
This incision was the first step toward modern mastoidectomy. Wilde was not highly praised by all of his contemporary colleagues. Wilhelm Kramer (28) from Berlin, who also published a famous textbook on ear diseases and a review of the book Aural Surgery (written by Wilde in 1853), wrote that his "negative opinion as the state of the art of English otologic surgery did not improve after publication of his Aural Surgery." Kramer's criticism may well be considered retribution for Wilde's public disapproval of his own book, published 4 years earlier in the Journal of Medical Sciences of Dublin. The controversy between these 2 medical doctors can be attributed to the competition between the German and British schools.
However, the editor of the Lancet clearly supported Kramer and suggested that Wilde's book should be given "to the trunkmaker." We can speculate that the editor, based in London, was not concerned with any rivalry with continental Europe and was referring instead to the superiority of the English over the Irish.
Joseph Toynbee, who practiced at the same time but did not agree with Wilde about the performance of the incision, related afterwards the importance of draining the infection. This was reflected in his comment about a patient suffering from acute mastoiditis: "It is likely that somehow a large portion of the tympanic membrane is removed as soon as mastoiditis develops, thus allowing the content to be released from the mastoid cells. This clears the bone from the disease" (13-29). Toynbee supported drilling the mastoid in another patient, saying, "Drilling of the mastoid process also indicates that the surgery might be performed with almost no hesitation in patients in which the purulent secretion is filling so much of their ear cavity, causing severe symptoms that will lead to death, if not removed. I never performed this surgery, although I would not hesitate if the life of the patient were at risk" (29).
Amedee Forget, a French surgeon, attempted a different procedure to remove the infection in 1860. He dissected the antrum and transferred the tissue of the meatus to the antrum so that it passed to the other side through the surgical wound, thus allowing drainage in both directions. Despite periodic transfer of the tissue, the relief from symptoms was only temporary. Therefore, the patient underwent a second surgery in which bone and necrotic tissue were removed, after which a significant improvement in the symptoms was observed (13).
When the then-typical treatment of "bacon fat infusion twice a day" and subsequent irrigation of the external acoustic meatus failed to relieve the symptoms, German surgeon Anton Friedrich Baron von Troltsch (21) performed a retroauricular incision to the level of the bone. Von Troltsch, professor of otology at the University of Wurzburg in 1864, had studied ear diseases in Dublin with Wilde and in London with Toynbee (30). In 1861, he published a case report of a 16-year-old girl who presented with otalgia, deafness, erythema, and mastoid edema associated with scarlet fever. Von Troltsch reported that "as soon as the incision was performed, the purulent secretions quickly filled the meatus while fresh blood started to be released. There was no infection in the wound behind the mastoid." The symptoms were significantly relieved 2 days later. When the symptoms and pain increased, the retroauricular edema relapsed, forcing von Troltsch to explore the previous incision. He probed it with a cutting edge without success. He then inserted a tampon into the wound with the intention of trying again the next day. However, he then realized that the nidus of infection behind the ear was releasing fluid that was initially transparent but later became opaque. Small volumes of fluid were also released by the meatus. The following day, von Troltsch continued advancing with the probe, and the symptoms subsequently improved. Von Troltsch reported, "I was not successful using only a probe; I should have the courage to adopt measures with other instruments that proved to be more efficient. In situations that are similar, I now would perform deeper incisions and dissect the first bone layer with a chisel, as it seems thin and easy to break" (21).
Von Troltsch is credited with arousing interest in mastoidectomy among German surgeons. He encouraged them to study mastoidectomy, stating, "if this procedure was forgotten or disregarded it was due to misapplications that occurred in the last century and to the peculiar and unusual position of the otologic literature until a short time ago." Von Troltsch published an article describing a new method and its indications, as the procedures that other surgical disciplines consider necessary under certain circumstances could not be applied to diseases of the ear (21).
It is worth remembering that until that time, surgeons did not specialize; for the most part they were general surgeons and performed all kinds of surgical operations, including procedures in ears.
In particular, Von Troltsch motivated his student Hermann Schwartze to standardize the procedures and indications for mastoidectomy.
Simple mastoidectomyIn 1873, Hermann Schwartze and Adolf Eysell (31) published an article describing the procedure for mastoidectomy. It was the first systematic description of how and under what conditions the procedure should be performed.
The article explained that curettage of the interior wound might cure the mastoid in patients who presented with destruction of the mastoid cortex. Schwartze also reported a case of a patient who presented with mastoid suppuration with a cortex soft enough to be easily penetrated with a probe. However, he suggested although the cortex was more often hard, the firm bone could be penetrated with trocars. Schwartze defined the concept of a standard surgical procedure for mastoidectomy, recommending the use of a chisel and hammer to remove the bone in such a way that the antrum could be properly inspected and efficiently drained.
Schwartze also stated clear indications for the procedure:
1. to treat purulent secretion through the attic, without consideration for the hearing capacity and removing the malleus and incus
2. to treat chronic purulent otorrhea of the tympanic cavity with positive signs of erosion of the incus and malleus as well as to treat cholesteatoma of the tympanic cavity
3. to improve hearing and treat subjective noise when the malleus is fixed and incurable obstruction of the Eustachian tube is observed as well as to treat sclerosis of the tympanic cavity with no signs of death of the auditory nerve.
After the publication of Schwartze's findings, a professor at the renowned Halle Clinic sought to reintroduce mastoidectomy (30-31).
Schwartze mastoidectomy, as it was known at the time, was used to establish a direct connection between the mastoid process and the tympanic cavity to enable irrigation with antiseptic solution. While initially performed in patients suffering from acute mastoiditis, Schwartze mastoidectomy was later used to treat exacerbations of chronic infections in which the fistula was found to pass through the bone and, finally, to treat patients suffering from persistent suppurative otitis media.
Hermann Hugo Rudolf Schwartze was born in Neuhof, Germany, in 1837.
Schwartze studied in Berlin and Wurzburg and then received his medical degree from the University of Berlin in 1853. He studied under the tutelage of Anton von Troltsch and served as an assistant at the Anatomopathological Institute of the University of Wurzburg. He became Professor and Director of the Otologic Clinic at the University of Halle in 1859. In 1863, Schwartze, with von Troltsch (1829-1890) and Adam Politzer (1835-1920), founded the Journal Archiv fur Ohrenheilkunde, the first journal dedicated exclusively to the pathology and treatment of the ear.
Schwartze then founded his own clinic to treat patients suffering from ear diseases (32). During the Franco-Prussian War, he served as a doctor at a field hospital and received the medal of the Iron Cross, Second Class. In 1903, he was the first ear surgeon in Germany to receive the title of Full Professor for this discipline. He was a member of several scientific societies, including the American Otological Society. The University of Halle established the Hermann-Schwartze medal, to be awarded for scientific contributions.
Near the end of his life, Schwartze suffered from restlessness, vertigo, and mental confusion (33-34). Curiously, his mentor Von Troltsch experienced the same problems; his obituary reported that, "recently, an insidious neurosis removed all his energy and finally left him in total need of help."
Radical mastoidectomyA simple mastoidectomy or antrostomy was observed to be sufficient in cases of acute mastoiditis. Radical mastoidectomy, a major procedure, was developed for treatment of chronic otitis or acute cases presenting with intracranial complications. Ernst Kuster and Ernst von Bergmann, both general surgeons, were credited with developing the radical surgery, which was known for some time as Kuster-Bergmann surgery. They advocated combining the dissection of several spaces of the attic, antrum, and middle ear, transforming these into a single large cavity, into one surgical procedure.
Ernst Kuster, a German general surgeon, suggested that the Schwartze surgery could be extended. In 1888, Kuster presented this idea to the German Medical Society; he later published a study reporting that according to his knowledge, abscesses that developed in hard bone at any depth should be completely exposed by dissecting the entire source of the infection. In contrast to the dissection of the antrum suggested by Schwartze, this procedure should open the bone surrounding the antrum as well as the posterior wall of the meatus. He suggested that in principle, all infectious bone disease should be opened and fully exposed, thus enabling removal of all of the affected tissue and extirpation of the source of suppuration. The release of purulent secretions should not be prevented. Only this level of dissection represents true adherence to the surgical principles suggested by Kuster.
In particular, if "the tympanic cavity was filled with granulations and the membrane as well as the ossicles were partially or totally destroyed, I try to go deeper. Then, guided by my eye, I could remove all the disease with the aid of a sharp spoon" (36).
In 1889, von Bergmann reported in a seminar that "between the upper wall of the external auditory canal and the lower and lateral side of the middle cranial fossa, a thick layer of bone might be observed. A sizel might penetrate up to the bone of the tympanic membrane without opening the cranial cavity." After a detailed description of how to reach the posterior wall with the aid of a sizel, von Bergmann suggested that upon removal of the wall of the meatus, a single funnel cavity might be created and a finger introduced up to the tympanic cavity to remove the remaining ossicles, granulations, and purulent material with a sharp spoon (37-38). Von Bergmann also recommended caution with regard to the depth of the insertion of the sizel in the posterior wall because of the possibility of facial nerve injury.
Dr. Arthur Hartmann from Berlin (39) reported the commentary of an American otologist on visiting Berlin in 1895: "I was in Berlin for only 2 days and saw 3 cases of facial paralysis after a mastoid surgery performed using a chisel, whereas in America I never assisted in any."
Emanual Zaufal (40) further improved radical surgery by dissecting from the antrum to the attic. In 1890, he modified the Schwartze procedure by suggesting removal of the posterior wall.
He revealed his findings at the Association of German Doctors in April 1890 and later at the 20th Convention of Swiss and Southern German Otologists, which was held in Prague in May 1890. He explained that this procedure was to be performed using a gouge, or a chisel and a hammer, with the aim of passing through the mastoid and reaching the eardrum. Zaufal performed the operation with a forceps-like clamp, placing one scalpel in the channel and the other in the antrostomy. He then removed the entire wall of the channel with one movement, exposing the entire cavity and the incudomalleolar joint. "Now," he wrote, "we have the important mission of removing [the] malleus, incus as well as the remaining tissue and bone using a sharp spoon or forceps." (39-40)
Zaufal opted to close the retroauricular wound rather than leaving a drain in place.
In 1890, Ludwig Stacke, a German otologist, introduced the idea of opening through the external auditory canal to seek the source of the infection (as in subcortical procedures). This allowed him to remove layers with the option of leaving a skin flap to promote better epithelialization.
In 1893, Sir William MacEwan (42) established the concept of the suprameatal triangle, also called the MacEwan triangle. Dissection of the mastoid antrum could be safely performed within this triangle, which is formed by the posterior root of the zygomatic process in front, the superoposterior segment of the external acoustic meatus bone at the bottom, and an imaginary perpendicular line joining these 2 areas and extending from the posterior meatus bone to the root of the zygomatic process at the back.
Modified radical mastoidectomySuddenly, traditional procedures regained popularity due to their ability to preserve hearing and middle ear function.
The declaration of Turmarkin reflects the feelings of those who condemned traditional surgery: "Radical mastoidectomy is one of the surgeries with the higher number of unsatisfactory results. Before surgery, the patient is quite deaf and presents otorrhea. After surgery, the hearing worsens when the patient is not completely deaf, whereas the otorrhea often continues. The patient may require a clarification about the reasons to perform this serious surgery."
Gustave Bondy (Figure 6) was credited with improving the procedure that was the precursor of the modified radical mastoidectomy in 1910 (44-49).
In order to release the purulent secretions confined within the antrum and the attic, Bondy removed the bone up to the external wall of the attic. He intended to preserve the tense part of the tympanic membrane and, if possible, the ossicles. A meatal skin flap was used to seal the defect between the epitympanum and mesotympanum; alternatively, when the ossicles were preserved, the flaps could be used to cover the exposed bodies (49-51).
Gustave Bondy was born in Austria in 1870 (Fig 5) and received his medical degree at the University of Vienna in 1894. In 1897, he began working at the Department of Otology of the General Polyclinic, where he remained an assistant until 1907, the year he became the first assistant of Professor Victor Urbantschitsch.
Bondy became famous for his work, published in 1907, on the comparative anatomy of auditory organs: Beitrage zur Vergleichenden Anatomie des Gohorogans (53). With expertise in otologic surgery and the treatment of intracranial otologic complications, he became famous for developing criteria for the modified radical mastoidectomy.
Bondy described the use of curettes and gouges in surgery. Moreover, he developed his criteria based on the evaluation of postoperative results assessed by his associate Erich Ruttin, who performed 1000 radical mastoidectomies in 1910. Bondy noted that although many of the patients had presented with a normal tympanic membrane, intact ossicles, and relatively normal preoperative hearing associated with attic cholesteatomas that affected only the pars flaccida of the tympanic membrane, their hearing worsened after surgery.
Before the Second World War, Bondy moved from Vienna to Australia, where he lived for the rest of his life.
Since the 1930s, mastoidectomy has evolved into a procedure that is now accepted as a standard otologic technique.
The discovery of penicillin by Alexander Fleming changed the natural course of potentially fatal otologic infections that had previously required surgery despite the risks for complications. Moreover, the number of interventions diminished. Access to preventive medical treatments and the greater possibility for antibiotic therapy allowed Armstrong to treat secretory otitis with a ventilator in 1970. The incidence of complications of chronic otitis media has recently decreased significantly in developed countries, although it remains high in poor regions.
Concern about regaining functional capacity and apprehension regarding reconstruction increased significantly with the introduction of other options. Concomitantly, mastoidectomy was increasingly used for other purposes, including labyrinthectomy, access to the internal auditory canal, and removal of glomus tumors. In recent years, the advent of implantable hearing prostheses (cochlear implants and other prostheses) has increased the importance of the otologic surgeon's knowledge of mastoidectomy.
Wullstein of Würsburg, Germany, introduced the surgical microscope after working with Zeiss to adapt a microscope developed for colposcopy and in situ diagnosis of uterine cervical cancer. Wullstein was the founder of ossicular reconstruction. Attention was redirected to the functional aspect of mastoid surgery in the early 1950s.
The present article mainly describes the origins and development of mastoidectomy for the treatment of chronic otitis media and its complications. However, we cannot fail to mention a major, if not the greatest, otologist of the 20th century, Dr. William House (Figure 7) from Los Angeles, California, United States. He began his career as a dental surgeon, following in the steps of his father, who was a famous dentist in California in the 1930s and 40s. He then joined the faculty of medicine and initially worked as a maxillofacial surgeon. William House was born in 1923. He was an innovator who introduced new procedures for the reduction of jaw fractures.
As he wrote in his memoir (2011), the advent of penicillin and decreased rates of infection significantly diminished interest in otorhinolaryngology, and residency positions in this field were left vacant (53).
William House fell in love with otology during his medical residency, when he encountered cases of deafness in children for which nothing could be done.
He introduced access to the facial nerve recess (posterior tympanotomy), which led to tympano-ossicular reconstructions with mastoidectomy (the so-called closed-cavity mastoidectomy or tympanomastoidectomy) as well as the use of traditional mastoidectomy for the treatment of chronic suppurative and cholesteatomatous otitis, now practiced worldwide. He introduced other innovative techniques in otology, but we have highlighted posterior tympanotomy because of its importance in mastoidectomy.
Throughout its history, mastoidectomy has shown a tendency to preserve or restore hearing. Currently, mastoidectomy is performed with the aim of preserving the anatomy of the ear, which may require several reoperations because of the tendency of cholesteatomas to recur.
The first mastoidectomy performed in Brazil was carried out in 1893 by Henrique Guedes de Melo in Rio de Janeiro.
Access through the mastoid was not abandoned. It was re-introduced by House with the aim of reaching the internal acoustic meatus and the posterior fossa through the translabyrinthic tract.
In 1972, Pulec and Hitzelberger used the mastoid to access the retrolabyrinthic tract to perform neurectomy initially of the trigeminal nerve and later of the vestibular nerve (54).
In 1995, Bento and colleagues presented the possibility of removing acoustic neuromas via the transmastoid and retrolabyrinthine approaches and thereby preserving the cochlear nerve (55,56).
Mastoidectomy has significantly evolved since the time of Ambroise Paré. Its improvement has relied on the introduction of more elaborate surgical procedures and particularly on advancements in surgical equipment made during the last century.
Mastoidectomy continues to be a life-saving surgical procedure.
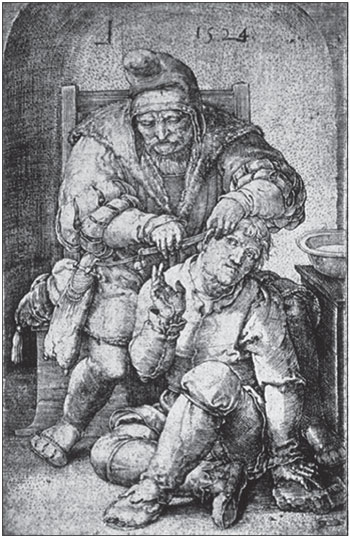
Figure 1. Early mastoid surgery as performed by a barber surgeon. Incision to drain abscesses has been practiced since ancient times. Lucas van Leyden, 1494-1533; The Surgeon, 1524.

Figure 2. "Mastoid Club"-Picture from the time of the first World War illustrating how frequently mastoidectomies were performed. (Sander and colleagues, 2006).

Figure 3. Jean Louis Petit (1674-1750). French surgeon who was the first to formally describe opening the mastoid, in a text published posthumously in 1774.
Figure 4. Wilde's incision. Wilde used the retroauricular incision only to drain purulent secretions rather than to enter the mastoid cavity. (Portmann G. A treatise on the surgical technique of otorhinolaryngology; Baltimore: William Wood; 1939).

Figure 5. Irish surgeon who popularized the retroauricular incision.

Figure 6. Gustave Bondy (1870-1954), Austrian surgeon (University of Vienna), popularized the modified radical mastoidectomy in which some or all of the middle ear structures were preserved in order to attempt to preserve hearing.
Figure 7. William House. American surgeon who introduced modern techniques of mastoidectomy and the use of mastoid access in otoneurosurgery.
1. Sunder S, Jackler RK, Blevins NH. Virtuosity with the mallet and goug: the brilliant triumph of " the modern" mastoid operation. Otolaryngol Clin North Am. 2006 Dec;39(6):1191-210.
2. Politzer A. Geschichte des ohrenheilkunde. Stuttgart (Germany): Verlag von Ferdinand Enke; 1913.
3. Lustig L, Jackler R. The history of otology through Eponyms II: the clinical examination. Am J Otol. 1999;20:535-50.
4. Duckworth WLH. Galen on anatomical procedures: the later books. Cambridge (MA): University Press; 1962.
5. Galen C. Galen: on the usefulness of the parts of the body, vol. 1. Ithaca (NY): Cornell University Press; 1968.
6. Galen C. Galen: on the usefulness of the parts of the body, vol. 2. Ithaca (NY): Cornell University Press; 1968.
7. Siegel RE. Galen on sense perception. Basel (Switzerland): S. Karger; 1970.
8. Millstein S. The history of mastoid surgery. Am J Otol. 1980;1(3):174-8.
9. Cawthorne T. The surgery of the temporal bone. J Laryngol Otol. 1953;67:377-91.
10. Mudry A. Contribution of Ambroise Pare´ (1510-1590) to otology. Otol Neurotol. 1999;20:809-13.
11. Liston SL. Ambroise Paré and the King's Mastoiditis. Am J Surg. 1994 Apr;167(4):440-2.
12. Singer DW. Selections from the works of Ambroise Pare. London: John Bale, Sons & Danielsson, Ltd; 1924.
13. Pare A. The apologie and treatise of Ambroise Pare. New York: Dover Publications; 1968.
14.- Sonnenschein R. A brief consideration of the history of the development of the mastoidectomy. Ann Med Hist. 1935;8:500-10.
15. Riolan J. A sure guide, or, The best and nearest way to physick and chyrurgery [Encheiridium anatomicum et pathologicum]. London: John Streater; 1671.
16. Riolan J. Anthropographia et Osteologia. Paris: Moreau; 1626.
17. Louis A. Extraits de l'eloge de Jean-Louis Petit lus dans la seance publique de l'Academie royale de chirurgie du 26 mai 1750 par A. Louis. Chirurgie 2001;126:475-81.
18. Ballance B. Essays on the surgery of the temporal bone, vol. 1. London: MacMillan & Co, Ltd.; 1919.
19. Petit, J-L. Traite´ des maladies chirurgicales, et des operations qui leur conviennent. Nouve´edition. Paris: 1790.
20. Schmucker, JS. Vermischte Chirurgische Schriften, vol. 3. Berlin; 1782.
21. von Tro¨ ltsch AF. Treatise on the diseases of the ear, including the anatomy of the organ. New York: William Wood, Co.; 1869.
22. Dezeimeris JE. De la perforation de L'apophyse mastoide. Dans diverses affections de ses cellules, et dans quelques cas de surdite´. L'Experience. Jounral de Medecine et de Chirurgie. 1838;33:497-501.
23. Dezeimeris JE. De la perforation de L'apophyse mastoide. Dans diverses affections de ses cellules, et dans quelques cas de surdite´. L'Experience. Jounral de Medecine et de Chirurgie.1838;33:513-20.
24. Wilson TG. Historical vignette - Sir William Wilde. Arch Otol. 1965;81:626-9.
25. Wilson T. Victorian doctor: being the life of Sir William Wilde. New York: Fischer; 1946.
26. Robins AH, Sellars SL. Oscar Wilde's terminal illness: reappraisal after a century. Lancet. 2000;356:1841-3.
27. Wilde WR. Practical observations on aural surgery and the nature and treatment of diseases of the ear. Philadelphia: Blanchard & Lea; 1853.
28. Kramer W. An exposure of "Wilde's Aural Surgery.". Lancet. 1853;62(1575):446-7.
29. Toynbee J. Diseases of the ear. London: J. Churchill; 1860.
30. Mawson SR. Surgery of the mastoid: the first centenary. Proc R Soc Med. 1975;68(6):391-5.
31. Schwartze H, Eysell C. Uber die kunstliche eroffnung des warzenfortsatzes. Arch Ohrenheilkd. 1873;7:157-62.
32. Pappas DG. Hermann Hugo Rudolf Schwartze (1837-1910). Ear Nose Throat J 1996;75(11):708-9.
33. Ohlroggen M, Lustig L. Atranslation of: The scientific progress of otology in the past decennium (until late 1862) by Hermann Schwartze: pathology and therapy of the external ear. Otol Neurotol. 2003;24(6):952-7.
34. Pappas D. Hermann Hugo Rudolf Schwartze (1837-1910). Reintroduction of paracentesis and mastoid surgery. Ear Nose Throat J. 1996;75:708-9.
35. Obituary. Lancet. 1890;135(3467):328-9.
36. Küster E. Uber die Grundsa¨ tze der Behandlung von Eiterungen in starrwandigen Höhlen. Deutsch med Wochenschr 1889;13:254-7.
37. Von Bergmann E. Berl klin Wchnschr 1888;36:1054.
38. Von Bergmann E. Die chirurgische Behandlung von Hirnkrankheiten. Berlin; 1889.
39. Hartmann A. Historical remarks upon the operation for exposing the tympanic cupola-space (attic) and the mastoid antrum. In: Knapp H, Moos S, Pritchard U, editors. Archives of otology. New York: GP Putnam's Sons; 1895. p. 1-11.
40. Zaufal E. Technik der Trepanation des Proc. Mastoid. Nach Kuster'schen Grundsatzen. Arch Ohrenheilkd. 1890;30:291.
41. Stacke L. Indicationen betreffend de Excision von Hammer und Amboss. Arch Ohrenheilkd. 1890;31:201-15.
42. MacEwenW. Pyogenic and infective diseases of the brain and spinal cord. Glasgow: MacLehose & Sons; 1893.
43. Tumarkin A. Mastoid surgery - old and new. Lancet. 1948;251(6506):708-11.
44. Heath C. The restoration of hearing after removal of the drum and ossicles by a modification of the radical mastoid operation for suppurative ear disease. Lancet. 1904;164:1767-9.
45. Heath C. A short paper (founded upon an experience of 400 operations) on the restoration of hearing after removal of the drum and ossicles by a modification of the radical mastoid operation for suppurative ear disease. In: Horne J, editor. Transactions of the Otological Society of the United Kingdom. London: J & A Churchill; 1905.
46. Heath CJ. Diagnosis and treatment in cases of otitis media (mastoid disease). London: Baillière, Tindall and Cox; 1919.
47. Heath CJ. The conservative mastoid operation. Lancet. 1928;211(5450):279-81.
48. Bryant WS. The radical mastoid operation modified to allow the preservation of normal hearing. Trans Am Otol Soc. 1906;9:292-5.
49. Richards GL. The so-called conservative mastoid operation, with a description of the technic of Heath, Bondy, and Siebenmann. Ann Otol Rhinol Laryngol. 1911;20:578-94.
50. Bondy G. Totalaufmeisselung mit Erhaltung von Trommelfell und Gehorknochelchen. Monatsschr Ohrenheilk. 1910. p. 15-23.
51. Pappas DG. Bondy's modified radical mastoidectomy revisited. Ear Nose Throat J. 1994;73(1):15-8.
52. Bondy G. Beitra¨ ge zur Vergleichenden Anatomiedes Goroha Gohorogans. Anat Hette; 1907.
53. House WF. The Struggles of a Medical Innovator: Cochlear Implants and Other Ear Surgeries. [place unknown]: CreateSpace; 2011. 208 p.
54. Hitselberger, WE; Pulec, JL- Trigeminal nerve (posterior root) retrolabyrintine selective section-operative procedure for intractable pain. Arch. Otolaryng. 1972;96:412-5.
55. Bogar P, Miniti A, Bento RF. The transmastoid, retrolabyrintine and presigmoid approach and hearing preservation. In: 2nd International Conference on Acoustic Neuroma Surgery and 2nd European Skull Base Society Congress, Paris, França, Final Program; 1995, p. 104.
56. Bento RF, Brito Neto RV, Sanchez TG, Miniti A. The transmastoid retrolabyrinthine approach in vestibular schwannoma surgery. Otolaryngology-Head Neck Surgery. 2002:127(5):437-41.
1) Professor. Chairman, Department of Otolaryngology, University of São Paulo, School of Medicine, São Paulo, Brazil.
2) Otology Fellow. ENT Specialist. Physician, Otology Group, Department of Otolaryngology, University of São Paulo, School of Medicine, São Paulo, Brazil.
Institution: Department of Ophthalmology and Otolaryngology, University of São Paulo, School of Medicine. São Paulo / SP - Brazil. Mailing address: Ricardo Ferreira Bento, MD, PhD. - Department of Ophthalmology and Otolaryngology - University of São Paulo - School of Medicine - Av. Dr. Enéas de Carvalho Aguiar, 255 - Sala 6167 - São Paulo / SP - Brazil - Zip code: 05403-900 - E-mail: rbento@gmail.com
Article received on October 20, 2012. Article accepted on December 9, 2012.