INTRODUCTIONHearing loss followed by non-otologic surgical procedures is not often mentioned in the literature, it is associated to cardiopulmonary bypass and rachidian anesthesia most of time.
Perioperatory hearing alterations is a little reported process, though it seems to be more frequent from surgeon and anesthesiologist viewpoint. Some circunstances which involve surgical work can simulate those alterations or can be of no notice because of its subclinical nature if audiometry is not done. I was already decribed with almost all anaesthesic techniques from local anaesthesia to general one, discussing in each of the cases a series of self or associated mechanisms (1).
In the case of epidural anesthesia or lumbar puncture, hearing loss has been often reported (1-3). Therefore, we are not always aware that this might happen, and even more, if we have in mind that the specific presentation and the beginning of the defict can widely vary (4), and that does not have great audiometric studies about and we cannot have an accurate idea of their clinical or subclinical incidence. From all studies, it is estimated that from 10% to 50% of the patients who had espinal anaesthesia can undertake hearing deficit measured in audiometric way in low frequencies, though only one fourth of them presented clinical manifestations (1). In other cases of local anaesthesia as blocking of plexes (5) or odontological anaesthsia with the blocking of nerve (6) it was also reported hearing loss.
In relation to general anaesthesia, the revision shows us that a greater number of cases is associated to cardiopulmonary bypass surgery (1,7). Our revision lets us report a total of 40 cases of sudden sensorineural hypoacusis followed by general anaesthesia in surgeries neither cardiopulmonary nor otological (1,3,8-17) (Table 1), and only one of them is associated to laparoscopic surgery (18). Although the cause of hearing loss associated to general anaesthesia, it is not very discussed. There is, in this medical work, a series of probable etiologies, which include changes and/or vascular damages, variations on pressure of medium and internal ear, changes on pressure of cerebrospinal fluid, embolis, ototoxic drugs, etc.
The target of the current study is to report a case of irreversible bilateral profound sensorineural hypoacusis followed by general anesthesia laparoscopic colecistectomy, etc.
CASE REPORTMale patient at 63 years of age, smoker for about 20 years, with an average of 20 cigarretes a day, reduced to 5, 12 months ago, with previous diagnosis of chronic obstructive pulmonary disease (COPD) and treating it with salbutamol and beclometasone. He had an audiometry done two years ago with light sensorineural hearing loss in frequencies of 4000 and 8000 Hz (1).With normal and complete pre-surgery evaluation and surgical risk ASAII, he is submitted to laparoscopic colecistectomy by cholelithiasis, using sevoflurene as the only anesthesic gas under usual procedures of the service and without evidence of any alteration neither during anesthesic, surgical work nor during post-anesthesic recovery what it refers the service unit of hospitalization.
After anesthesia effect, about 10 hours later, he presents intense tinnitus, vertigo and bilateral hypoacusis. He is evaluated by Otorhinolaryngology, showing bilateral profound sensorineural hypoacusis (2). Biometry exams were normal and ear tomography, internal hearig conduct and posterior cavity did not present any alterations. The patient carried on his post-surgery treatment with cephalothin, ranitidine, tramadol, dimenhydrinate and prednisona, and was released from hospital on the fifth day without evidences of clinical or audiometric improvement. All treatment is dismissed and it is recommended hearing aids. Six months later it is done control audiometry (3) without any improvement.
DISCUSSIONSudden defness, defined as sensorineural hearing loss of 30 db or more in three consecutive frequencies ocurring less than 72 hours, has been associated to accidents, cranioencephalic trauma, infections, metabolic perturbations, etc., but only about in 10% is possible to determine especific etiology. In the remaining, it is not possible to identify it or consider it ideopathic (1,19).
Previous reports have assigned that some medical and surgical procedures can result in hearing damage of different intensity; so, lumbar punction can cause cerebrospinal fluid loss and soon after hearing alterations affecting both ears on intense sounds and usually in a transitory way (1,3) and it can be of no notice if specific research is not done.
Hearing loss is reported to be more frequent when associated to spinal anesthesia (3), therefore its incidence is unknown due to lack of studies with this purpose. It is known that 0.4% of the patients submitted to spinal anesthesia undertake some type of hearing perturbation (1). MICHAEL (20) has described sensorineural hypoacusis followed by mielography, lumbar punction and spinal anesthesia. Hearing deficts were regularly situated in low frequencies (125 - 1000Hz). From 10 to 50% of the patients who had epidural anesthesia undertook mesurable hearing defict in low frequencies, therefore less than one fourth is clinically known (1-3,20).
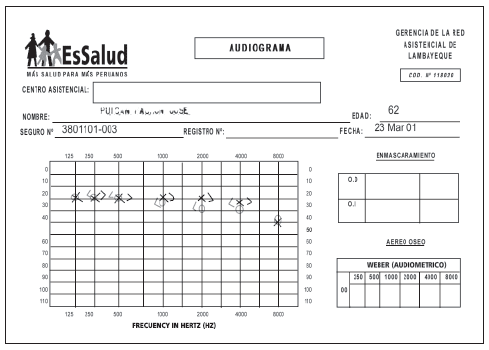 Picture 1.
Picture 1. Audiometry done two years before surgery.
 Picture 2.
Picture 2. Audiometry done soon after surgery.
From the cases of sudden sensorineural hypoacusis followed by non-otological surgery under general anesthesia, most of them refers to patients submitted to cardiopulmonary bypass syrgery (1,7). In the current report, we have presented hearing loss associated to general anesthesia to laparoscopic surgery. In the revised literature, we discussed about 40 documented cases of hearing loss followed by general anesthesia, only one of them in relation to laparoscopic surgery, and the second reported, the current one, in relation to general anesthesia and laparoscopic surgery and the first in which sevoflurane was the only anesthesia gas used.
During general anesthesia and laparoscopic colecistectomy there are changes on body pressures: arterial pressure, intrabdominal pressure and/or of cerebrospinal fluid which can be direct and indirectly conducted to ear structure causing its lesion (1,14,17). Hearing loss can occur by disarticulation of the ossicular chain and by perilynphatic fistula on oval window in relation to ventilation with oxygen mask, therefore, those pressure increasings do not necessarily ask for great efforts, thus, they can cause labyrinthic membrane with valsalva maneuver, sneezing or cough (1). Some anesthesic gases, such as nitrous oxide, because of its easy dissolution and penetration on tissues, changes the nitrogen in them, altering pressure on cavities as ears, for example, when anestesia is discontinued and opposite process quikcly occur, what it can cause rupture of the labyrinthic membrane and hearing alterations as consequence (1,14,15). In the current case it was done anesthesic induction and maintanance with sevoflurane, anesthesic over which we have not found reports that describe hypoacusis as adverse effect from its use.
Laparoscopic surgery to colecistectomy asks from pneumoperitoneum with CO2 which produce an increase of the intrabdominal pressure, if it matches with head upwards position to displace intestinal wing out of operation field, if it produces blood epistaxis on legs, reducing venous return, hypotension and tendencies to thrombosis what might lead to changes on cardiac, renal and hepatic physiologies of the patient, producing hypercapnia and acidosis, unusually air embolism and cardiac irritability; even though it stimulates hormone liberation related to renal-cardiac function and vaso-vagal stimulation which might cause circulatory collapse (21).
Those factors when alone or in combination make production of blood redistribution to other organs easy, deviating from internal ear, which is particularly susceptible as it lacks colateral circulation and its cells have high energy metabolism. Epithelial damage on internal ear microcirculation causes reduction of the potential of cochlear work (1,22). Evaluating this mechanism, the idea of damages produced on internal ear microcirculation during general anesthesia, lead to lack of oxygen of the cilliated cells and hearing loss.
If we compare the possibility of recovery from sudden sensorineural hypoacusis according to type of anesthesia and surgery (1), we see that almost all patients, with hearing loss followed by rachidian anesthesia, reach recovery. In patients submitted to general anesthesia, recovery is partial on the ones who underwent cardiopulmonary bypass surgery; in patients submitted to other types of non-otological or non-cadiovascular surgery, recovery is less probable.We have to keep in mind that when sudden hearing loss occurs, at greater grade of loss, the association to vertigo and age (above 60), the possibility of recovery is also minute.
CONCLUSIONSReportamos un caso de hipoacusia neurosensorial súbita bilateral persistente luego de colecistectomía laparoscópica, una complicación poco esperada y menos entendida, cuyos probables mecanismos fisiopatológicos son diversos y complejos lo cual limita nuestras actitudes preventivas y terapéuticas ante tan devastadora condición.
We have reported a case of persistent bilateral sudden sensorineural hypoacusis followed by laparoscopic colecistectomy, a type of complication little expected or understood, whose physiopathological mechanisms are diverse and complex, which limits our preventive and therapeutic attitude towards this condition.
REFERENCIA BIBLIOGRAFICAS1. Warltier D, Sprung J, Bourke D, Contreras M, Warner M, Findlay J. Perioperative hearing impairment. Anesthesiology, 2003, 98(1): 241-57.
2. Gultekin S, Ozcan S. Does hearing loss after spinal anesthesia differ between young and elderly patients. Anesth Analg, 2002, 94(5):13-18.
3. Schaffartzik W, Hirsch J, Frickmann F, Kuhly P, Ernst A. Hearing loss after spinal and general anesthesia: A comparative study. Anesth Analog., 2000, 91:1466-72.
4. Ok G, Tok D, Erbuyun K, Aslan A, Tekin I. Hearing loss does not occur in young patients undergoing spinal anesthesia. Reg Anesth Pain Med, 2004, 29(5):430-3.
5. Rosemberg P, Lamberg T, Tarkkila, Marttila T, Bjorkenheim J, Touminen M. Auditory disturbance associated with interscalene brachial plexus block. Br J Anaesth., 1995, 74(1):89-91.
6. Shenkman Z, Findler M, Lossos A, Barak S, Katz J. Permanent neurologic deficit after inferior alveolar nerve block: a case report. Int J Oral Maxilofac Surg, 1996, 25(5):381-2.
7. Walsted A, Andreassen K, Berthelsen P, Olesen A.Hearing loss after cardiopulmonary bypass surgery. Eur Arch Oto-Rhino-Laryngol, 2000, 257(3): 124-27.
8. Millen S, Toohill R, Lehman R. Sudden sensorineural hearing loss: operative complication in non-otologic surgery. Laryngoscope, 1982, 92(6 Pt1):613-7.
9. Girardi F, Cammisa F, Sangani PK, Parvataneni H, Khan S, Saltar N, et al: Sudden sensorineural hearing loss alter spinal surgery under general anesthesia. J Spinal Dis, 2001, 14(2):180-83.
10. Evan K, Tavill M, Goldberg A., Silverstein H. Sudden sensorineural hearing loss after general anesthesia for nonotologic surgery. Laryngoscope,1997, 107(6): 747-52.
11. Velazquez F. Hearing loss after general anesthesia for cecectomy and small bowel resection. AANA Journal, 1992, 60(6):553-5.
12. Cox AJ, Sargent E. Sudden sensorineural hearing loss following nonotologic, noncardiopulmonary bypass surgery. Arch Otolaryngol Head Neck Surg, 1997, 123(9):994-8.
13. Segal S, Man A, Winerman I. Labyrinthine membrane rupture caused by elevated intratympanic pressure during general anesthesia. Am J Otol, 1984, 5(4):308-10.
14. Hochermann M, Reimer A. Hearing loss after general anesthesia (a case report and review of literature). J Laryngol Otol, 1987, 101(10):1079-82.
15. Pau H, Selvadurai P, Murty G. Reversible sensorineural hearing loss after non-otological surgery under general anesthesia. Postgraduate Medical Journal , 2000, 76:304-306.
16. Nishida T, Nishihara L, Hanada R, Tsukahara E, Okada T, Gomyo I: Two cases of hearing disorder following general anesthesia. Masui, 1999, 48(5):518-22.
17. Peng T, Chen CH, Fang T, Chang Ch, Wu C. Sudden hearing loss after general anesthesia: a case report. Acta Anaesthesiol Taiwan, 2005 43(1):43-7.
18. Belan A, Rida A, Hamoud N, Riou B, Vergel M: Bilateral sensorineural hearing loss after general anesthesia. Ann Fr Anesth Reanim., 1994, 13(3):400-2.
19. Eisenman D, Arts A. Effectiveness of treatment for sudden sensorineural hearing loss. Arch Otolayngol Head Neck Surg, 2000, 126(9):1161-64.
20. Michel O, Brusis T, Loennecken I, Matthias R. Inner ear hearing loss following cerebrospinal fluid puncture: a too little appreciated complication? HNO, 1990, 38(2):71-6.
21. Preventza O, Habib F, Young S, Penney O, Oppat W, Mittal V. JSLS, 2005, 9(1):87-90.
22. Chao T. Sudden sensorineural hearing loss after rapid reduction of blood pressure in malignant hypertension. Ann Otol Rhinol Laryngol, 2004, 73-75.