INTRODUCTION Cholesteatoma is a type of inflammatory epidermic pseudo-tumor that penetrates cavities of medium ear and presents double potential of descamation on the surface and bone lysis on depth.
It represents 30% of surgery recommendation in children to chronic medium otitis. This number can grow according to age and to the increase of mucosal otitis, pouches of invagination, hyperkeratosis, external hearing canal (1).
Cholesteatoma is more aggressive in children than in adults; its growth is fast and it becomes worse by superinfection, which is often due to the importance of tubal factor, (2).
The different techniques to perform cholesteatoma surgery are based on conservation or not of the posterior wall of external hearing canal, raising or not the communication between mastoid cavity and exterior, through meatoplasty. There are more conservative techniques, though there is a need of a revision or second look, not always possible to be done, because restrictions of economical and social terms become difficult to perform a second routine surgery. For this study we followed the surgical procedures below:
- Removal of posterior canal wall (radical mastoidectomy) and partial removal canal wall (radical modified mastoidectomy BONDY).
- Tympano-mastoidectomy with or without posterior tympanotomy.
- Reconstruction of the radical mastoidectomy cavity using tympanoplasty and columellar effect of "small cavity" of PORTMANN (3).
We studied the concepts of the following results of compared variables.
-
Suppuration - it is the ear that suppurates continuously even being free from cholesteatoma, free from other factors (adenoid vegetation, allergies, sinusitis, etc.) and even under local treatment with antibiotics and aspirations.
-
Cavity Instability - we consider instable the cavity which goes through a period of drought and of suppuration, though with no cholesteatoma.
-
Recurrence - it is the cholesteatoma reappereance.
Terms such as recurrent recidivous and residual cholesteatoma were introduced by SHEEHY (4).
-
Drought of Cavity - We consider an ear is dry with no cholesteatoma or supporation in a period from six months to one year. If any secretion occurs, it is easily eliminated by remedy.
-
Surgery Revision - it is performed six months, at least, after first operation, either clinically or through evaluation by computed tomography, on closed technique where there is indication of recurrence of cholesteatoma.
The target of this study is to show surgery results from 200 children who underwent cholesteatoma opperation in different techniques and to compare results between open and closed technique to erradicate both residual and recidivous cholesteatoma.
PATIENTS AND METHODSOur record is composed by 200 children with cholesteatoma (COMC), assisted by Dr. Professor Nelson A. Cruz at São Paulo Hospital of Escola Paulista de Medicina and some cases from our private clinic between 1962 and 1990. We examined patients aging up to 15 years.
In the studied group, 128 (64.0%) of them were male and 72 (36.0%) were female.
The average age ranged from 4 to 15 years.
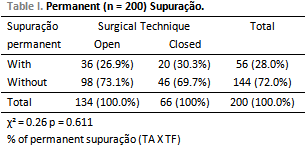
The surgery techniques performed in this study are displayed on Table 1.
Patients presented in their records: exam history from ears from otoscopy and/or microscopy of the nose and throat; culture and antibiogram from ear secretion; audiological and radiological evaluation.Hearing tests were done by phonoaudiologists before and after surgery, through preliminary tonal audiometry with distinguishion of the word. Each patient had radiological study as simple X-Ray from temporal bone in conventional postions, multidirectional and computed tomographies in special cases. We focused on nose and paranasal sinus for diagnosis and treatment of nasal obstruction, allergy and sinusistis when needed. We only ccepted patients with problems related to anatomy-functional area of ear. The method used was retrospective observation of clinical history. Data were written in a protocol especially done, where we registered data regarding at pre-surgery period, type of surgical intervention and post-surgery period. The responsible people for the children who would undergo surgery had to sign a term of consent.
COMC treatment is a surgical type when effectiveness does not depend only on type of used technique or quality of its performance. This effectiveness depends on a severe feature of erradication of cholesteatoma.
The used techniques were the following:
-
Radical Mastoidectomy - Open technique. The surgeon consumes intentionally by fire the posterior wall of the external hearing canal removing the tympanic membrane remainings, malleus and incus and it is associated to meatoplasty.
-
Posterior Tympanotomy - Performed on closed technique with the purpose of creating room in the posterior wall of external hearing canal, ahead of facial nerve, in order to observe and remove cholesteatoma and sick mucosa placed next to stapes and round window.
-
Mastoidectomy With Tympanoplasty - At the same time and when there was no doubt of comprehensive excision of cholesteatoma (closed technique) through posterior tympanoplasty, nearly compulsory.
-
Radical Cavity Reconstruction - ("small cavity" technique). Radical Mastoidectomy is performed with simple reconstruction of middle ear, using temporal fascia and interposition of incus between tympanum and platinum when there is no stapes.
-
Modified Radical Mastoidectomy - It consists of a partial removal of external wall of the attic and posterior canal wall which exposures and makes cholesteatoma external preserving hearing system.
-
Surgery Revision (second look) - It is recommended as a prevention in order to eliminate any residual or recurrent cholesteatoma.
RESULTS It is easy to analyze surgery results on COMC in children. The disagreement between open and closed technique is still present.
In most of our patients, cholesteatoma was found in the ATTIC (42.1%), ATTIC and ANTRUM (40.0%) extending to MASTOID in 18.0%. In this series we did not find any case of primary cholesteatoma.
All presented imperfection on ossicular chain, where incus was the first bone to be damaged.
Perforation of tympanic membrane on attic area (59.7%) was more frequent followed by marginal perforation (13.9%).
Although we preferred open technique (67.0%) we also performed the closed one (33.0%). - Frame 1
Residual cholesteatoma occured more often on ATTIC (42.0%), MESOTYMPANUM and HYPOTYMPANUM (36.0) and in other places of MASTOID (22.0%).
We also found problems such as facial palsy (1 case) that after decompression surgery and graft surgeries of the facial nerve recovered 85% of motricity, and facial paresis (1 case) that totally receded after surgery. Perichondritis with sequelae in 2 cases, hearing loss in 1 case and cochlear implication in 2 cases.
Temporal fascia was used to tympanic reconstruction; to ossicular chain. We used homologous ossicle from bank. Prothesis of biocompatible and alloplastic materials were not used.
Natomic And Functional Results (Closed Technique)1)
Simple mastoidectomy with tympanoplasty (at the same time or not) - closed technique (n=39).
Anatomic and functional results were examined from six months to five years after operation.
We obtained anatomic success - 91.2% (52/57) - when using graft of temporal fascia on mastoidectomy with tympanoplasty. Hearing functional results were calculated by the difference between post-surgery air pathway (POST AP) and pre-surgery bone pathway (PRE BP), calculated over frequency average (0.5 KHz- 1KHz-2KHz) at communication area:
- Preserved superstructure of the stapes: 31/57 (POST) AP - (PRE) BP:
< 20db=54.3%
- Destroyed superstructure of the stapes: 26/57 (POST) AP -(PRE) BP:
< 20db=45.7% (only platinum)
Hearing loss after surgery arose in our record in one case and cochlear implication (20% of loss or more in frequencies (4 and 8 KHZ)) arose in 2 cases.
2)
Tympanoplasty in radical cavity ("small cavity" technique).
We used the technique recommended by PORTMANN (2) where graft of temporal fascia, collumelar effect and cartilage of septum compiled in the attic.
We performed four interpositions of incus over stapes and another three of moulded incus over platinum. We had two surgery revisions in this technique.
We obtained anatomic success in 78.0% (7/9) using graft of temporal fascia.
Hearing functional results were calculated by the difference between post-surgery air pathway (POST AP) and and pre-surgery bone pathway (PRE BP), calculated over frequency average (0.5 KHz-1KHz-2KHz) at communication area:
- Preserved superstructure of the stapes: 6/9 (POST) AP - (PRE) BP:
< 20db=66.6%
- Absent superstructure of the stapes: 3/9 (POST) AP - (PRE) BP:
< 20db=33.3% (only platinum)
3)
Radical mastoidectomy: Open technique (n=134)
The main purpose of this technique is to control infection and cholesteatoma, with lesser prevention with hearing.
We controlled cholesteatoma and infection in 73.1% and there was recurrence of cholesteatoma in 19.4%, what is not a problem for being an open cavity we could remove it by aspiration.
In relation to hearing results, we had: Unmodified hearing - 131 cases and worse hearing in three cases. Two cases with worsening on bone pathway (4 e 8 KHZ) and one case of anacusis during post-surgery period.
We found the following results from compared variables. (Table 1, 2, 3, 5)
DISCUSSIONAccording to results regarding infection healing, OT and CT were different: 73.1% of cavity control for OT and 69.70% for CT (Table 4). It was not found any statistically expressive associations between drought of cavity and surgery technique used (p = 0.207). The percentage of patients submitted to open technique presenting drought in cavity was 73.1%, and the percentage of patients submitted to closed technique was 69.7%, with no expressive difference between them.
TOS & TORBEN (5) found 74.0% of drought in their cavities of radical mastoidectomy. This finding make us to consider that, in most of cases, we always should perform OT to large cholesteatoma, what provides positive results to infection process. This agrees on the findings by CRUZ, O.L. et al (6).
We found persistence of infection (constant suppuration - Table 1) in 30.3% in CT. This result should be meticulously analyzed when we recommend CT in children. These findings agree with STARK et al (2), PHIL & PADGHAN (7) e SCHURING et al (8), and JAHN (9).
We conclude that at OT the recurrence control and development of cholesteatoma is greater, reducing possible complications. It was not found statistically expressive associations between presence of constant suppuration and surgery technique (p = 0.611). The percentage of patients submitted to open technique presenting constant suppuration was 26.9%, and the percentage of patients submitted to closed technique was 30.3%, with no expressive difference between them.
When a proper post-surgery follow-up is possible, we can decide for either CT or OT if post-surgery development is not suitable as STERKERS & STERKERS(10), WAYOFF et al (11) and FISCH(12), ARRIAGA(13), GERSDORFF & VILAIN(14) recommend.
Regarding to residual cholesteatoma, we should, whenever possible, perform surgery revision in a period from 6 to 12 months at least. This period is ideal to identify any remains from squamous epithelium large enough to be distinguished, though this growth can be slow and if surgery is quite fast, there is a risk of not finding it. We should follow patient both clinically and through tomography. This can done one year after surgery and interfere when there is a trace of cholesteatoma recurrence.
Nevertheless, recurrence was a little higher in patients submitted to CT surgery (27.3% - Table 3).
In our study, recurrence was considered as a residual and recidivous cholesteatoma and retraction pocket. SHEEHY (15) found in CT in 51.0% of occurrence and CHARACHON & GRATACAP (16) reported that this recurrence occurs twice more on CT than on OT, TAKAHASHI et al (17), ROSBORG & DOMERBY (18), NISHIZAKI et al (19) MURATA et al (20), PEDERSEN (21), PFLEIDERER et al (22), BABIGHIAN(23), STANGERUP et al(24) found similar results, what coincides with our results. It was not found statistically expressive associations between recurrence and surgery technique (p = 0.207). The percentage of patients submitted to open technique presenting recurrence was 19.4%, and the percentage of patients submitted to closed technique was 27.3%, with no expressive difference between them.
Percentage of instability of surgical cavity is varies for different authors. To PALVA (25) instability is 10.0%; to SADE et al (26) is 30.0%; to BROWN (27) 33.0%; to WAYOFF et al (28) is 35.0% for both OT and CT.
We obtained 28.5% of instability for the two studied techniques (Table 2). It was found statistically expressive associations between instability and surgery technique (p = 0.001). The percentage of patients submitted to open technique presenting instability was 20.1%, and the percentage of patients submitted to closed technique was 45.5%. While on OT the worry about hearing is lesser, on CT, the target is its improvement.
Perhaps more satisfactory functional results are the ones from reconstruction of ossicular chain, when performed in te middle ear with healthy mucosa and stable tympanum. Such qualities are difficult to be achieved when we are before cholesteatoma after a second surgery during post-surgery period.
In the cases of reconstruction of our cavities, we firstly chose for removing infection and then, six months later at least, reconstruction by tympanoplasty.
We perform technique of "small cavity" of PORTMANN et al (3) whenever possible for three reasons: it avoids epidermization of the middle ear: it reduces the risk of tubal otorrhea and it can improve hearing.
CONCLUSION1) The open technique was the method chosen for handling cholesteatoma due to the following reasons:
a) Most of our patients come from far and cannot easily return, what makes frequent post-surgery follow-up impossible.
b) Lack of beds or surgical vacancies in public hospitals. Systematic surgery revision would grow the waits.
c) Resistence from patients to surgeries when knowing that they will be submitted to two or more surgeries.
d) Controlling recurrences and cholesteatoma development is greater, reducing possible complications.
2) It seems that cholesteatoma surgery with conservation of posterior wall should be set apart to some especial cases only and either classical or modified radical mastoidectomy should be the options on cholesteatoma eradication.
3)"Small cavity" technique allows comprehensive removal of cholesteatoma and makes hearing improvement possible.
BIBLIOGRAPHY1. Magnan J. Le cholestéatome: son histoire naturelle. Les Cahiers dORL. T.XXVIII - Nº 10 - 1993 pp.399-401.
2. Stark TH, Dazert S, Sudhoff H. Fibrocartilaginous Eustaquian tube and cholesteatoma. Middle ear cleft, 2003, pp.125-32. edited by B. ARS, Kugler Publications. The Hague, The Netherlands
3. Portmann M, Crovetto MA, Valles J, Aguayo F. Résultats anatomiques et fonctionnels de la "petite caisse" dans les évidements petro-mastoidiens pour cholestéatome. Rev. Laryngol, 1987, 108(2):161-64.
4. Sheehy JL & Jerald VR. Revision tympanoplasty: residual and recurrent cholesteatoma. A report on 272 intact - wall revisions. Cholesteatoma and mastoid surgery. Proceedings Ind International Conference, Tel Aviv, 1982, pp.443-48. Kugler Publications. Amsterdam.
5. Tos M, Torben L. Cholesteatoma in children. Long term results. Cholesteatoma and mastoid surgery. Proceedings of the third International Conference on Cholesteatoma, 1988, pp.677-83. Kugler & Ghedini Publications, Amsterdam, Berkeley, Milano.
6. Cruz OLM, Miniti A, Mello Jr J, Ayres JO, Ming Yen. Surgical treatment of cholesteatoma. Experience with 198 patients. Cholesteatoma and mastoid surgery. Proceedings of the thirt International Conference on Cholesteatoma, 1988, pp.925-29.
7. Phil, RPM & Padghan VD. Management of childhood cholesteatoma. The Journal of Laryngol and Otol.; 1991, 105:343-45.
8. Shuring AG, Rizer RM, Lippy WH, Shuring LT. Staging for cholesteatoma in the child, adolescent and adult. Ann. Otol. Rhinol. Laryngol., 1990, 99:256-60.
9. Jahn AF. Chrorinic otitis média: diagnosis and treatment. Clin. North. Am., 1991, 75(6):1277-91.
10. Sterkers JM & Sterkers O. Open and closed techniques in intra-temporal cholesteatoma surgery. Cholesteatoma and Mastoid surgery. Proceedings of the third International conference on Cholesteatoma, 1988, pp.1089-90. Kugler & Ghedini Publications, Amsterdam, Berkeley, Milano.
11. Wayoff M, Charachon R, Roulleau P, Lacher G, Deguine CH. Le traitement chirurgical du cholestéatome de loreille moyenne. Societé Française DORL et Pathologie cervicofaciale, Arnette, 1982, 229 p.
12. Fisch U. Timpanoplasty and Stapedectomy. A manual of techniques 1994, 284p. Georg Thieme Verlag, Stuttgard, New York.
13. Arriaga MA. Cholesteatoma in children. Otolaryngol. Clin. North. Am., 1994, 27(3):573-91.
14. Gersdorff M, Vilain J. Long-term results of various surgical treatments for cholesteatoma. Act. Orl. Belg. 1990, 44(4):393-98.
15. Sheehy JL. Intact canal wall. Tympanoplasty with mastoidectomy. Controversy in Otolaryngology. Ed. Snow, 1980, pp.213-22.
16. Charachon R. & Gratacap B. The surgical treatment of cholesteatoma in children. Clin. Otolaryngol; 1985, 10:177-84.
17. Takahashi S, Uruno M, Nakano Y. Outcome of congenital and acquired cholesteatoma after closed surgery in children. Cholesteatoma and Mastoid Surgery, 1992, 8-12, pp.509-13. Kugler publications, Amsterdam, N. York.
18. Rosborg J, Dommerby H. Results of cholesteatoma surgery in children. Cholesteatoma and Mastoid Surgery, 1992, 8-12, pp. 515-19. Kugler publications, Amsterdam, N. York.
19. Nishizaki K, Sugihara H, Kobayashi K, Masuda Y. Surgery for middle year cholesteatoma in children. Cholesteatoma and Mastoid Surgery, 1992, 8-12, pp. 521-524. Kugler publications, Amsterdam, N. York.
20. Murata K, Takeyama Y, Tanaka H, Tamaki K. Surgical management of cholesteatoma in children. Cholesteatoma and Mastoid Surgery, 1992, 8-12, pp. 525-528. Kugler publications, Amsterdam, N.York.
21. Pedersen C. Surgical treatment of cholesteatoma in children: Long-term results. Cholesteatoma and Mastoid Surgery, 1992, 8-12, pp. 529-34, Kugler publications, Amsterdam, N.York.
22. Pfleiderer AG, Ghosh S, Kairinos N, Chaudhri F. A study of recurrence of retraction pockts after various methods of primary reconstruction of attic and mesotynpanic defects in combined approach tympanoplasty. Clin. Otolaringol Allied Sci. 2003, 28(6):548-51.
23. Babighian G. Posterior and attic wall osteoplasty: hearing results and recurrece rates in cholesteatoma. Otol. Neurotol., 2002, 23(1):14-27.
24. Stangerup SE, Drozdziewicz D, Tos M, Hougaard-Gensen A. Recurrence of attic cholesteatoma: different methods of stimating recurrence rates. Otolaryngol, Head Neck Surgery, 2000, 123(3):283-87.
25. Palva T. Surgical treatment of cholesteatomatous ear disease. J. Laryngol. Otol., 1985, 99(6):539-44.
26. Sadé J, Berco E, Brown M. Results of mastoids operations in various chronic ear diseases. Am. Journal of Otol., 1981, 3:11-20.
27. Brown JS. A ten year statistical follow-up of 1142 consecutive cases of cholesteatoma. The closed versus the open technique. Laryngoscope, 1982, 92:960-66.
1. Doctorate - UNIFESP ( Titled Professor II Universidade Santo Amaro - UNISA-SP ENT).
2. PhD in ENT by medical school USP; responsible for Otology Department of Beneficencia Portuguesa Hospital - SP.
3. 5th year student of Medical School - Nova Iguaçu (Doctorate).
EPM-UNIFESP and private clinic
Address: Alameda Ribeirão Preto, 410/1106. Bela Vista cep: 01331-000 São Paulo-SP. CEP:01331-000.
Phone/Fax: (11) 3051-3059. E-mail: clinicaorlsp@uol.com.br
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) - RAIO on February 1, 2006 and approved on March 6, 2006 22:54:55.