INTRODUCTIONPeritonsillar abscess is the most common deep suppurative infection of the parapharyngeal space. Patients complain about intense odynophagia, fever and trismus. It always occur as a consequence of a nearby infection, especially from oropharynx or teeth, and rarely from naso-sinusal or even otological processes. The physical exam was done in a patient with apparent toxemy and the pharyngoscopy demonstrates unilateral oedema of the peritonsillar area with contralateral deviation of the uvula and postero-lateral area bulging of the soft palate, with no difficulty of diagnosing. We will introduce a case of a male patient, 42, with complaints about intense odynophagia with no fever. Traditional ENT exam and videolaryngoscopy presented normal results. The use of non-steroid anti-inflammatory did not improve any condition, so neck and pharyngeal area computed tomography scan was requested. The result showed well-defined nodular structure, with hypodense center and ring-like impregnation with iodine contrast, placed on the right anterior tonsil pillar, suggesting a little abscess in such area. After the diagnosis, the clinical treatment with levofloxacin caused improvement of symptoms and CT presented normal condition three weeks later.
LITERATURE REVISIONAlthough clinical diagnosis is not easily done most of times, in the current case, only CT could clear the patient's complaints. When revising literature, CT is recommended in order to confirm diagnosis. Ultrasonography is also recommended in order to confirm diagnosis and its development when it is possible to evaluate if process is still peritonsillar cellulitis or if purulent collection already exists, what is useful to decide on clinical or surgical treatment (3,4). CT has been also used to evaluate surgical treatment risks, considering that the contrast finds the internal artery carotid track that goes into the medium peripharyngeal space.
According to literature the germs which cause such supuration are the ones found on infections of superior aerodigestive passages, both aerobic and anaerobic types, and the main cause of this complication would be microbian selection due to a either badly prescribed or baldy used antibiotic therapy. The most found aerobic germs are: beta and alpha-hemolytic Streptococcus pyogenes belonging to group A and Staphylococcus aureus and more rarely Streptococcus pneumoniae, Haemophilus influenzae, Klebsiella pneumoniae and Escherichia coli. And from the anaerobic germs, the most frequent ones are: Bacteroides sp, Peptococcus sp, Peptostreptococcus sp and Actinomycosis sp (6,7).
Antibiotic therapy should be aggressive, and considering the flora one of the most common found, the choices are: penicillin G, third generation cephalosporin, imidazolin and quinolon. In clinical routine the bacteriological study is essential, but it should be recommended for patients with resistant microorganism such as diabetic ones, immunocompromised patients and for those with recurrent peri-tonsillar abscess (7). Clinical treatment is used during cellulitis stage and surgical treatment when purulent collection occurs. Yet on adults drainage with local anesthesia should be done, inserting lidocaine on the mucosa from anterior pillar belonging to tonsillar fossa, blocking tonsillar branch of the glossopharyngeal nerve. Then a thick needle punction is done in order to find purulent collection, and soon after that, an incision on anterior pillar. The opening is separeted and enlarged and the exudate is aspirated. In this stage, antibiotic therapy can be through oral passage up to infection is extinguished. Although tonsillectomy is recommended after total process resolution, some authors do it during abscess drainage. When doing abscess drainage in children, general anesthesia should be done (8-11).
As severe implications are rare and tonsillectomy is requested, either during abscess drainage or after acute stage healing, because recurrences are frequent and even worse predisposing to implications. There are reports on necrotizing fasciitis of the conjunctive and adjacent muscle tissues with high rate of mortality especially on weak or immunocompromised patients (12,13).
CLINICAL CASE INTRODUCTIONA male patient, 42, with intense odynophagia complaint, with no fever and traditional ENT exam and videolaryngoscopy presented normal results. The use of non-steroid anti-inflammatory did not improve any condition, so neck and pharyngeal area computed tomography scan was requested. The result showed well-defined nodular structure, with hypodense center and ring-like impregnation with iodine contrast, measuring 1.8 x 1.5cm in its larger transversed diameters, placed on the right anterior tonsil pillar, suggesting a little abscess in such area (Picture 1). After the diagnosis, the clinical treatment with levofloxacin caused improvement of symptoms and the CT presented in normal condition two weeks later (Picture 2). Although clinical diagnosis is not easily done most of times, only CT could clear the patient's complaints.
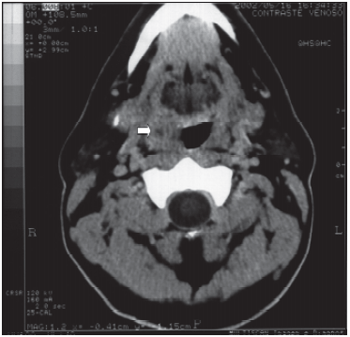
Picture 1: Pharynx CT and cervical area showing well-defined nodular structure, with hypdense center and ring-like impregnation with iodine contrast, measuring 1.8 x 1.5cm in its larger transversed diameters, placed on the right anterior tonsil pillar.
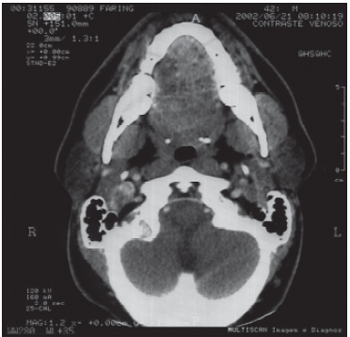
Picture 2: Pharynx CT and cervical area in normal condition three weeks after treatment with levofloxacin.
Diagnosising peritonsillar abscess is easy to be done most of times, and treatment should start soon after its result in order to avoid local and systemic implication, and also to ease patient suffering. Surgical treatment of abscess drainage is done most of time either in advance or delayed because of the uncertainty of an existence or not of a purulent collection on peritonsillar infection, what it is only cellulitis, as complaints about both conditions are the same as well as physical exam. The certain diagnosis is also done with aspiration using thick needle and abscess drainage, and it is followed by antibiotic therapy if found. The current case was only diagnosed through CT and although treatment was exclusively clinical it certainty came because of antibiotic therapy response. Scott et al. (1999) in prospective study on 14 patients with peritonsillar infection concluded that clinical impression had 78% of sensitivity and 50% of specificity to peritonsillar abscess (4). CT presented 100% of sensitivity and 75% of specificity and ultrasound presented 89% of specificity and 100% of sensitivity, and the latter was suggested as an important exam on differential diagnosis between peritonsillar abscess and peritonsillar cellulitis. Miziara et al. (2001) recommend ultrasonography as a good method for differential diagnosis between both, having found 92.3% of sensitivity and 62.3% of specificity (3). Ishii et al. (2002) recommend CT with contrast to inquire into anatomical relations between abscess and parapharyngeal space in order to determine more suitable surgical places for drainage, considering anatomical conditions of the abscess with carotid artery, internal jugular vein and nerves that are placed on parapharyngeal space (5). The differential diagnosis should be also done with tumors of palatine tonsils and with infectious mononucleosis.
Tonsilectomy is recommended for peritonsillar abscess cases, therefor patient refused to undergo to proposed surgery. Up to the moment, 5 years after condition installation and treatment, patient has no symptoms and no peritonsillar infection recurrence or other acute tonsilites.
The moment when to do tonsilectomy in cases of peritonsillar abscess is questionable. Some authors do it and the abscess drainage at the same time; others do drainage first, suggesting tonsilectomy after healing acute condition. Raut and Yung (2000) did a study over their own patients and a poll with many ENT doctors from England and they concluded that tonsilectomy on peritonsillar abscess should be done as a definite treatment for those patients who have acute tonsillitis history and only clinical history would indicate radical treatment for both children and adults (10). Most of these patients who were in hospital and did not undergo tonsillectomy had no symptoms during 2 to 8 years after clinical treatment or drainage. Tonsilectomy should be recommended for few cases when traditional treatment has no effect.
FINAL COMMENTSAuthor presented CT as an important component, as a complementary exam of the acute infectious processes of oropharynx, especially those that are difficult to be identified and diagnosed. Treatment of suppurative infections of the paraphryngeal spaces should be done as earlier as possible avoiding implications of process spread to all local topography.
BIBLIOGRAPHY1. Steyer TE. Peritonsillar abscess: diagnosis and treatment. Am Fam Physician, 2002, 65(1):93-6.
2. Abu el-Naaj I, Krausz A, Ardekian L, Peled M. Parapharyngeal and peritonsillar infection following mandibular third molar extrsaction. Refuat Hapeh Vehashinayim, 2001, 18(3-4):35-9, 109-10.
3. Miziara ID, Koishi HU, Zonato AI, Valentini M, Miniti A, Menezes MR. The use of ultrasound evaluation in the diagnosis of peritonsillar abscess. Rev Laryngol Otol Rhinol (Bord), 2001, 122(3):201-3.
4. Scott PM, Loftus WK, Kew J, Ahuja A, Yue V, van Hasselt CA. Diagnosis of peritonsillar infections: a prospective study of ultrasound, computerized tomography and clinical diagnosis. J Laryngol Otol, 1999, 113(3):229-32.
5. Ishii K, Aramaki , Arai Y, Uchimura K, Okabe K, Nishida M, Yoda K. Evaluation of safe surgical treatment of peritonsillar abscess using computed tomography. Nippon Jibiinkoka Gakkai Kaiho, 2002, 105(3):249-56.
6. Fujiyoshi T, Inaba T, Udaka T, Tanabe T, Yoshida M, Kakishima K. Clinical significance of the Streptococcus milleri group in peritonsillar abscesses. Nippon Jibiinkoka Gakkai Kaiho, 2001, 104(9):866-71.
7. Cherukuri S, Benninger MS. Use of bacteriologic studies in th outpatient management of peritonsillar abscess. Laryngoscope, 2002, 112(1):18-20.
8. Kieff DA, Bhasttacharyya N, Siegel NS, Salman SD. Selection of antibiotics after incision and drainage of peritonsillar abscesses. Otolaryngol Head and Neck Surg1, 1999, 120(1):57-6.
9. Windfuhr JP, Chen YS. Immediate abscess tonsillectomy - a safe procedure? Auris Nasus Larynx, 2001, 28(4):323-7.
10. Raut VV, Yung MW. Peritonsillar abscess: the rationale for interval tonsillectomy. Ear Nose Throat J., 2000, 79(3):206-9.
11. Luhmann JD, Kennedy RM, McAllister JD, Jaffe DM. Sedation for peritonsillar abscess drainage in the pediatric emergency department. Pediatr Emerg Care, 2002, 18(1):1-3.
12. Goldenberg D, Golz A, Netzer A, Flax-Goldenberg R, Joachims HZ. Synergistic necrotizing cellulitis as a complication of peritonsilar abscesss. Am J Otolaryngol, 2001, 22(6):415-9.
13. Safak MA, Haberal I, Kiliç D, Göçmen H. Necrotizing fascitis secondary to peritonsillar abscess: a new case and review of eight earlier cases. Ear Nose Throat J, 2001, 80(11):824-30, 833.
1. PhD Professor in Otorhinolaryngology and Head of ENT Service of Hospital Universitário da UFES (University Hospital)
2. PhD in Otorhinolaryngology by Unifesp.
3. Medical School student at Universidade Federal do Espírito Santo (Federal University - ES)
4. Medical School student from Escola Superior de Ciências da Santa Casa de Misericórdia de Vitória.
Study done at Otorhinolaryngology Service of Hospital Universitário "Cassiano Antônio Morais" - UFES - Vitória - ES (University Hospital) and presented at XLIII Congresso Médico Estadual da AMES (State Medical Congress), from October 16 to 19, 2002.
Mail Address: Sergio Ramos - Avenida Saturnino de Brito, 256 - Enseada do Suá - Vitória - ES - CEP 29050-385 - Phone (27) 33451600 - Fax (27) 33450195 - e-mail sramos@tropical.com.br.
Article received on May 19, 2005 and accepted with its corrections on October 05, 2005.