INTRODUCTIONEctodermal Dysplasia represents a complex group of pathologies containing over 170 clinical features (1,2), with an incidence of 7 out of 10,000 born-alive children (1). Genetic transmission can vary among the different characteristics of the disease. It can be autossomic and X-linked - dominant or recessive and of sporadic transmission (1,2). Ectodermal Dysplasia holds clinical alteration which affects structures coming especially from ectoderm, such as skin and its appendages and also affects other non-ectodermal structures (4). The most common clinical evidences are problems in the skin, hair, teeth, nails and sweat glands.
Atrophic Rhinitis is one the situations related to Ectodermal Dysplasia (3,5-12). It mainly affects individuals at late childhood age (3,6) and young adults (4). Atrophic Rhinitis is a chronic inflammatory disease of the nose, producing crusts (6) due to imperfect movement of the nose hair. Besides being related to Ectodermal Dysplasia, it can be found at granulomatous diseases such as Tuberculosis and Hansen´s disease (5)
TARGETTo first report a case of a child who developed Atrophic Rhinitis symptoms at one month year old and also to demonstrate the association of such pathology with Genetic Syndrome of Ectodermal Dysplasia. Besides, to highlight the importance of Atrophic Rhinitis therapy by ENT doctors due to related complications.
CASE REPORTWe reported a case of a male patient at the age of 7 when he visited the doctor complaining of nasal obstruction and presence of crusts, mucopurulent rhinorrhea, nasal fetidness and breathing difficulties since his first month of life.
During pregnancy, his mother reports having had threatened abortion at the third and sixth months. The first prenatal ultrasonography was performed at the seventh month, when hydrocephaly was diagnosed. She had a premature labor by Caeserian (32 to 33 weeks old), and the baby was kept in neonatal ICU for 22 days.
During first week after being delivered from hospital, mother noticed nasal obstruction followed by breathing difficulties with crusts formation, progressive bad smell and mucopurulent rhinorrhea. Such symptoms remain up to now, and he had suffered 2 episodes of epistaxis so far.
From 6 month years old, patient started with constant episodes of fever, which became worse when heat exposure, and had a fever convulsion at 8 month of age. He underwent several antibioticotherapies for having been thought recurrent infections. Symptoms became eased when the child had cold bath or when was laid over cold floor. At the age of 3 he was diagnosed as Anhidrotic or Hypohidrotic Ectodermal Dysplasia.
Patient presents history of upper air pathway infections and recurrent othitis since he was 2 month years old. When he was four, myopia was diagnosed, presenting hypoacusis, occasional dysphonia, photophobia and a delay on psychomotor development.
In the physical exam, presence of crusts and mucopurulent rhinorrhea with nasal obstruction at rhinoscopy were observed. Yet, in the otoscopy there is presence of central perforation on the right tympanic membrane and retraction on the left one. Skin becomes thin, dry and scaled with hypotrichosis and nipple absence. Hair becomes thin, dry and hypochromic. There is presence of hypodontia and nails are hyperconvexed. Nose is sadlled-shape and face presents maxillary hypoplasia, inferior lip protusion, prominent front, periorbitary hyperpigmentation and low implanted ears.
The audiometric exam showed bilateral conductive hearing loss and nasofibroscopy showed severe pereustachian tube area edema and ample nasal fossa with plentiful formation of crusts.
Physical features pointed on the physical exam description can be seen on Pictures 1, 2 and 3
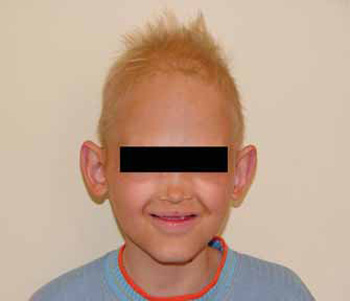
Picture 1 - Occurrence of periorbitary hyperpigmentation and Partial Baldness, as well as presence of low implantation of pointed ears and saddled nose.
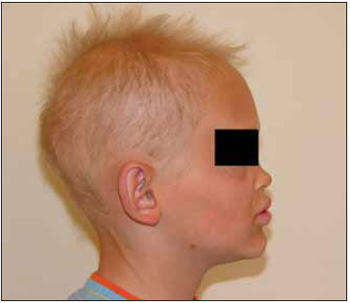
Picture 2 - Image showing Lip, and thin Hair Protrusion.
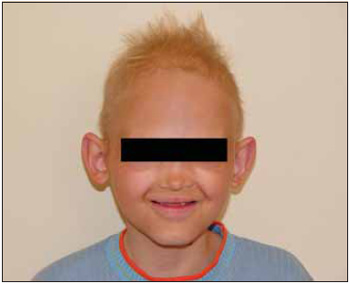
Picture 3 - Presence of hypodontia and prominent front.
Among the 30 types of Ectodermal Dysplasia in which their clinical alteration, Genetic and molecular causes (1,4) are known, the most common one is Hypohidrotic, also called as Anhidrotic Ectodermal Dysplasia or Christ-Siemens-Touraine`s syndrome (6). This one is related to alterations on X-linked recessive genes, or rarely to alteration on autossomal recessive and dominant genes (1, 2, 13). That is the reason why only men express their features in a comprehensive way.
Around 94% of the cases is due to alterations on ED1 gene (2), on Xq12-q13.1 (13), which was isolate by Kere et al. in 1996 (1,14). About 53 different alterations on ED1 gene has been described so far (13). Such gene is responsible for coding 2 isoforms of ectodysplasin, a transmembrane protein of collagen which is similar to proteins that join Tumor Necrosis Factor. The alteration on homologous domain to the TNF ligand ones shows that this protein area is fundamental to its functioning (1).
The two isoforms of Ectodysplasin are ED1-A1 and EDA-A2, which are respectively connected to the EDAR and XEDAR receptors. When such connections occur, the cascades of nuclear factor (NF)kB and JNK/c-fos/c-jun are activated. Both are responsible for the activation of signs to Epidermal Growth Factor job, which differ epiderm from its appendages (1,2,13). So, one might conclude that Ectodysplasin works on cell surviving, communication and growth (1).
Another alteration, besides this one, is the DL gene one, which is responsible for EDAR receptor. This causes recessive or dominant autossomic Ectodermal Dysplasia (1).
The most common manifestation of Hypohidrotic Ectodermal Dysplasia is the reduction or complete absence of eccrine, sweat and lacrimal glands. However, apocrine glands are in normal condition (1-3,6,13).
One of the consequences of gland alteration is the impossibility to sweat, what happens due to body temperature, hyperthermia crisis and fever convulsions (3,13). Skin, when usually hypopigmentated (2), becomes thin and dehidrated, scaled (6), and it can suffer from atopic dermatitis, xerodermia and liquenification (3).
The alteration on the lacrimal glands causes secretion in small amount and dacryocystitis of repetition (3,6).
Regarding dental formation, hypodontia and adontia are found. Teeth are small and conical shaped (1-3,6,13).
Hypotrichosis is frequent and it can many times be associated with baldness. Hair is thin, dry and hypochromic as well as the other hair of the body (1-3,6).
Among nail abnormalities, it can be found hyperconvexed, hypertrophic dystrophic, keratinized nails and even the absence of them.
Facial abnormalities show tipical appearances, such as saddled nose prominent front, low implanted pointed ears, inferior lip protrusion periorbitary hyperpigmentation.
The other alterations found are hypoplasia of mammary glands, visual disfunction, premature birth and mental retardation.
Most of ENT manifestations are due to secretion alterations from mucosal glands, which might lead to recurrent infections. It is constant the occurrence of infections of superior air pathways and repetition otitis - medium, external and eczematous one - many times followed by sensorineural hypoacusis. Patient can present chronic conditions such as pharyngitis, laryngitis, dysphonia and odinophagy as well as atrophic rhinitis followed by epistaxis and catarrh (3).
The occurrence of Atrophic Rhinitis is related to secretion disorder of mucosal gland, and also to inherited association with Ectodermal Dysplasia (4,5,7). Together with drainage and deficient ciliary movement, there is secretion retention with late development of crusts and fetid smell. Mucosa is bleeding and ulcer-like (4).
Atrophic Rhinitis is a type of disease that normally develops during late childhood (3,6) or young adult age (4), as mentioned in the literature (3,15). However, in the current case, its clinical condition appeared soon after birth, and it was diagnosed when patient was 7 years old.
Saddled nose is related to improper blood supply during nasal and septal bone growth. This occurs due to severe inflammatory reaction in Atrophic Rhinitis (6).
After describing signs and symptoms found in Ectodermal Dysplasia, it is possible to observe that the current patient has many of them, what characterizes a peculiar case as the disease appears in different ways in different people (2).
The used therapy is symptomatic. Humidification and often nose washing are used in order to prevent smell and crusts formation (3).
CONCLUSIONAtrophic Rhinitis is a type of disease associated with Genetic and molecular alterations of Ectodermal Dysplasia. Although it does not exist in all cases of Ectodermal Dysplasia, it is considered as a predominant complaint from patient. For this reason, it should be followed up and treated carefully by ENT doctors as it is related to different cases of infectious complications.
REFERENCES1. J. Lamartine. Toward a new classification of ectodermal dysplasias. Clinical and Experimental Dermatology 2003;28:351-355.
2. Priolo M, Silengo M, Lerone M, Ravazzolo R. Ectodermal Dysplasias: Not only a 'skin' deep. Clin Genet 2000;58:415-430.
3. J.Gonzáles Garcia, H. Galera Ruiz, F. Muñoz Borge. Manifestaciones ORL de la displasia ectodérmica hipohidrótica. Acta Otorrinolaringol Esp 2005;55:176-178.
4. Shehata M. Atrophic Rhinitis. American Journal of Otolaryngology 1996;17(2):81-86.
5. Wiesmiller K, Keck T, Lindemann J. Atrophic rhinitis in a patient with anhidrotic ectodermal dysplasia. Rhinology 2005;43(3):233-5.
6. Sinha V, Sinha S, Anhidrotic Ectodermal Dysplasia Presenting as Atrophic Rhinitis and Maggots. Indian Pediatrics 2003;40:1105-1106.
7. Sachidananda R, Nagadi A, Dass AA, Praveen Kmar BY. Anhidrotic ectodermal dysplasia presenting as atrophic rhinitis. J Laryngol Otol 2004;118(7):556-7.
8. Chistiakova VR, Toropchina LV, Chumicheva IV. The development of ozena in a child suffering from anhydrotic ectodermal dysplasia. Vestn Otorrinolaringol; (1):48-9,200.
9. Ibañes Cárcamo E. Anhidrotic ectodermal dysplasia: congenital ozena. Acta Otorrinolaringol Esp 1990;41(2):107-9.
10. Baer ST, Coulson IH, Elliman D. Anhidrotic ectodermal dysplasia: an ENT presentation in infancy. J Laryngol Otol 1988;102(5):458-9.
11. Martini A, Magnan G, Peserico A. Ozena as presenting symptom of a rare and severe genetic disease: hypohidrotic ectodermal dysplasia. Int J Pediatr Otorhinolaryngol 1984;8(1):97-103.
12. Gil-Carcedo LM. The nose in anhidrotic ectodermal dysplasia. Rhinology; 20(4):231-5, 1982.
13. Gun Yoen Na, Do Won Kim, Seok Jong Lee, Sang Lip Chung, Dong Jae Park, Jung Chul Kim, Moon Kyu Kim. Mutation in the ED1 Gene, Ala349Thr, in a Korean Patient with X-linked Hypohidrotic Ectodermal Dysplasia Developing de novo. Pediatric Dermatology 2004;21(5):568-572.
14. ECTODERMAL DYSPLASIA 1, ANHIDROTIC, ED1. OMIM (Online Mendelian Inheritance in Man) available at http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=OMIM
15. Rafiq M.A, Faiyaz-ul-Haque M, Amin ud Din M, Malik S, Sohail M, Anwar M, Haque S, Paterson A, Tsui L, Ahmad W. A Novel Locus of Ectodermal Dysplasia Maps to Chromosome 10q24.32-q25.1. J Invest Dermatol 2005;124:338-342.
1. Fifth-year-student at the Medical school from Universidade Federal do Paraná.
2. Doctor at the ENT Department from Universidade Federal do Paraná.
3. Titular Professor of the ENT Department from Universidade Federal do Paraná.
4. Resident doctor at the ENT Department from Universidade Federal do Paraná.
5. Resident doctor at the ENT Department from Universidade Federal do Paraná.
6. Titular Professor of the ENT Department from Universidade Federal do Paraná.
7. Titular Professor of the ENT Department from Universidade Federal do Paraná.
8. Resident doctor at the ENT Department from Universidade Federal do Paraná.
Universidade Federal do Paraná
Heloisa Nardi Koerner
address: Rua Buenos Aires, 600, apto 1901 Cep 80250-070 Curitiba-Paraná-Brasil helo_nk@hotmail.com
Phone: (41)3223-8117
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on February 16, 2006 and was approved on July 2, 2006 10:15:39.