INTRODUCTIONThe term myringoplasty was firstly used in 1953 by Horst Wullstein when reporting his reconstruction technique of the tympanossincular system in cases of middle chronic otitis. Regarding the technique, the main targets of surgery, according to Sheehy (1) are: the eradication of the pathological condition, if it exists, resulting dry middle ear; an untouchable tympanic membrane; preservation or reconstruction of the meddle/external ear and restoration of the mechanisms that transmit sounds. The tympanic membrane (TM) is made of three layers: one outer layer made of queratine scaly epithelium, one intermediate mesodermic fibrous layer and one inner endodermic mucosa layer.
When the tympanic membrane is in continuity solution, it regenerates starting from two known mechanisms of epithelial migration. One of them is the centrifugal movement from the TM umbilicus. The second mitotic standard, which is considered essential for the cicatrisation of continuity solutions, is the centripetal movement, which happens in all the tense parts of the TM, with higher activity around the tympanic ring. In the miringoplasties, the graft works as a substitute in the corneous extract on which epithelial migration waves flow, with the purpose of fixing perforation(2).
In the literature, several studies have discussed which conditions of the middle ear in the chronic ear may affect, in some way, the cicatrisation of TM and consequently the final anatomic result in the miringoplasties. The classical House study established that the presence of active infection and mucosa hyperplasia in the middle ear are factors which diminish the surgical success. Besides the condition of the mucosa of the middle ear, other studies consider re-operation, material used for the graft, technique of the graft position and size of tympanic perforation predictive factors(3,4,5).
This study evaluates if it is possible that intra-operatory findings influences the final anatomic results of miringoplasties performed by second year medic residents of Hospital das Clínicas da Universidade Federal de Pernambuco.
MATERIAL AND METHODThe picture of this study has been retrospective through the revision of medical histories in which 94 patients with diagnosis of chronic non-colesteatomatosis middle otitis who were undertaken to a kind 1 miringoplasty of Wüllstein have been analyzed between 2002-2003.
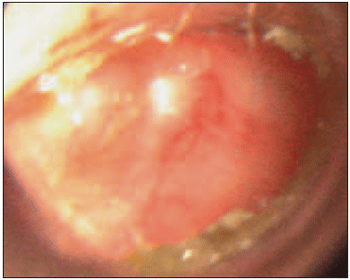
Picture 1. Post-operative of miringoplastia - Second month of postoperative miringoplastia of the left ear. There is the cable of the hammer and normal production of cerumen. There was Total healing of the tympanic membrane, prior to core drilling of 60%.
One record for the registration of information of each patient in their pre, trans and post-surgical phases has been used. In this record the patients' characteristics such as age, surgical access, kind and position of the graft have been reported. The presence of infection in the middle ear, the mucosa state, the presence or not of tympanosclerosis and the size of perforation have been analysed and compared with the final anatomic result - closing, or not, of the perforation. The surgery has been performed by medic-residents with their preceptors. This study has been approved by the Ethics Council of the Health Science Center/Hospital das Clínicas da Universidade Federal de Pernambuco. (Project number 0241.0.172.000-06/Record number 233-06 approved on November 1st, 2006).
RESULTS 97 ears in 94 patients have been undertaken to surgery, being 29 men and 68 women, with average age of 25.16 years old (between 10 and 52 years old). All surgeries have been performed under general anesthesia, and the most used surgical way was the retroauricular one. (n=91). Fascia has been used as graft according to the underlay technique in most of patients (n=94).
The variables study results which may influence in the TM cicatrisation have been statistically analysed and presented in the tables below. The surgical success is equivalent to the whole TM presence 6 months after the miringoplaty surgery.
Table 1 shows the study of TM according to the presence or absence of secretion in the middle ear during the surgery. This table show that most of the operated ears with complete cicatrisation of TM did not present secretion during the surgery. However, at 5.0% level, there has not been significant association between middle ear secretion and the TM condition according to the test Fisher test results (p>0.05).
Table 2 shows the study of TM according to the mucosa state in the middle ear during the surgery. This table shows that 11 cases of tympanic perforation which presented mucosa hyperplasia in the middle ear has surgical success. In the ears with healthy mucosa there has been 80% of surgical success. However, at 5.0% level, there has not been significant association between middle ear mucosa and the TM condition according to the test Fisher test results (p>0.05).
Table 3 shows the study of TM according to the presence or absence of tympanosclerosis. Such table shows that out of the 78 ears with whole TM after the surgery, 85.7% had significant association between the presence or absence of tympanosclerosis and the TM condition according to results of
Table 4 shows the study of TM according to the size of perforation. This table shows that out of the 56 cases with perforation higher than 50%, there has been 78.5% of surgical success. In the minor perforations the success of the graft was of 85.4%. In this relation there has not been significant association between the size of perforation and the TM condition after the surgery according to the X2 test results (p>0.05).
DISCUSSIONThe final anatomic objective in the miringoplaties is a dry middle ear through a whole tympanic membrane. In the literature, several studies have discussed which conditions of the middle ear in the chronic ear may affect, in some way, the cicatrisation of TM and consequently the final anatomic result in the miringoplasties.
This study presented a 80.4% success, considering the total closing of perforation. Compared to the literature, it is a satisfactory result. Sheehy(1) in a revision of 472 cases presented a rate of ear perforation TM closing of 97% and Kotecha(6), in his study, , presented a rate of 82.2%. If we evaluate the populations which are similar to the sample economically and socially, we can observe that the surgical success varied from 66,6%%(9) to 78% (7,8,9,10). The Fukuchi study performed with 37 patients which have been seen in the otorrinolaryngology clinic of Faculdade de Medicina do ABC obtained 51.4% of closing of perforation of TM in the first surgery and 65% considering the re-operations(11).
The presence or absence of intra-operatory otorrhea did not influence the final anatomic result. The intermittent otorrhea is one characteristic of simple chronic middle otitis. According to Sismanis, the chronic middle otitis agravation with purulent infection is a relative contra-indication for the miringoplasty(12) On the other hand, Sheehy previews a dry ear for a better surgical result (13) and Gersdodoff M emphasizes the ears which were operated and had otorrhea presented worse results than the dry ears (14). Whers R(15) comments that otorrhea may be present in the middle ear without being active infection, mainly if the secretion is serous, odorless and with negative bacteria culture. Such condition is commonly known as humid ear, which does not present surgical contra-indication because of otorrhea. The secretion culture is not part of our record, but the 9 ears which were operated with otorrhea presented serous and odorless secretion, with TM closing in 7 of them. Studies such as Mak D(7) and Black JH(8,9) did not find significant association between the serous secretion in the middle ear and the TM cicatrisation, which agrees with our results. This way, it is observed that the surgery can be performed if the ear is totally dry or not. Such information assumes higher importance on SUS patients, whose difficult access to health system, for many times, does not allow us to keep them in ideal conditions for surgery.
In the evaluation of mucosa state, it has been observed that it has not influenced the surgical results. The degree of affection of the mucosa of the middle ear indicates the magnitude of the disease for the mastoid, once its hyperplasia indicates important bad aeration. Shelton C(13) evaluated the mucosa of the middle ear as the main factor in the staging of the surgical approach in 400 cases in the House Ear Clinic. In the proposed staging, which evaluates otorrhea, ossicular chain, mucosa of middle ear, among other factors, 75% of the cases were indicated to mastoidectomy and 15% for miringoplastia. The surgical success with closing of air-bony GAP for less or equal to 20dB occurred in 68% of the ears with present stirrup. When Albu S(16) analyzed the prognosis factors which determine the post-operatory success of the otologic surgery he concluded that the mucosa situation is the most important predictive factor.. IN this study, the evaluation of the affection of the mucosa of middle ear has been performed by many different surgeons. We have not obtained uniform data, which may have influenced our results.
The tympanosclerosis is a hyaline degeneration of the submucosa layer of TM and it may be a risky factor for the miringoplasty failure. Ears with tympanosclerosis had worse results than the ones with normal TM, statistically significant. This way, we can observe that the presence of tympanosclerosis may harm the cicatrisation of the TM. Kageyama-Escobar(17), in his study, presented 82% of closing of tympanic perforation and observed that tympanosclerosis was among the risky factors for surgical failure, mainly when it diffusely involved TM. However, when Wielinga(18) evaluated the influence of tympanosclerosis in the miringoplasties, he studied 555 miringoplasties and concluded that there is no relation between that presence of absence of it in the final result, even if it is diffuse. When possible, we recommend the focus be removed in order to facilitate the epithelial migration and the closing of TM perforation.
The size of TM perforation, besides indicating a more difficult surgery for beginners residents, may indicate worse anatomic result(5,6,13,19) Albu S(16) observed that perforations smaller than 50% presented better anatomic and functional prognosis. Gonzáles FC(20) performed a retrospective study with 197 miringoplasties in which the only decisive factor for the surgical success was the place of the perforation, with better results in the posterior perforations and worse ones in the subtotal ones.. Halik JJ(21) demonstrated worse cicatrisation in children which were younger than 10 years old and in the anterior perforations. In the present study, in relation to the size of perforation, there was a tendency of better results in the perforations smaller than 50%, despite the lack od statistic co-relation.
CONCLUSIONThe anatomic final results of the miringoplasties may be influenced by several factors. When we analyze some of these factors we conclude that the patient, once he/she is operated through retroauricular access, using fascia as graft and through the underlay technique, will have better anatomic results with total closing of the perforation if the is absence of tympanosclerosis in the TM. The presence of otorrhea and alteration of the mucosa in the middle ear have not changed the final surgical result. Perforations which are smaller than 50% may present better results than total perforations. It is important to point out that despite these variables are analyzed separately, in the clinical practice all those factors are connected and concomitantly contribute for the TM cicatrisation.
REFERENCES1. Sheehy JL et Anderson RG. Myringoplasty. A review of 472 cases. Ann Otol Rhinol Laryngol. 1980, 89(4 Pt 1):331-4.
2. Costa S, Cruz OLM, Kluwe LHS, Smith MM. Timpanoplastias. Em: Cruz, OLM e Costa, S (eds). Otologia clínica e cirúrgica. 1ª ed. São Paulo: Editora Revinter; 1980, pp. 245-271.
3. Kartush JM, Michaelides EM, Becvarovski Z, LaRouere MJ. Over-under tympanoplasty. Laryngoscope 2002, 112(5):802-7.
4. Gerber MJ, Mason JC, Lambert PR. Hearing results after primary cartilage tympanoplasty. Laryngoscope 2000, 110(12):1994-9.
5. Desaulty A; Lansiaux V; Machiels S; Gael JF. Failures after tympanoplasty. Rev Laryngol Otol Rhinol 1996, 117(5):357-61.
6. Kotecha B, Fowler S, Topham J. Myringoplasty: a prospective audit study. Clin Otolaryngol 1999, 24(2):126-9.
7. Mak D, MacKendrik A, Bulsara M, Coates H, Lannigan F, Lehmann D, Leidwinger L, Weeks S. Outcomes of myringoplasty in Australian Aboriginal children and factors associated with success: a prospective case series. Clin Otolaryngol 2004, 29(6):606-11.
8. Black JH, Hickey SA, Wormald PJ. An analysis of the results of myringoplasty in children. Int. J. Pediatr Otorhinolaryngol 1995, 31(1):95-100.
9. Black JH, Wormald PJ. Myringoplasty-effects on hearing and contributing factors. S Afr Med J 1995, 85(1):41-3.
10. Ogisi FO, Adobamen P. Type 1 Tympanoplasty in Benin: a 10- year review. Niger Postgrad Med J 2004, 11(2):84-7.
11. Fukuchi I, Cechiari DP, Garcia E, Rezende CEB, Rapoport PB. Timpanoplastias: resultados cirúrgicos e análise dos fatores que podem interferir no seu sucesso. Rev.Bras Otorrinolaringol, 2006, Vol 72(2):261-6.
12. Sismanis A Tympanoplasty. Em: Galsscock-Shambaugh.Surgery of the Ear. 5ª edição. Hamilton. London. Editora: BC Decker Inc; 2003, pp.39-73.
13. Shelton C, Sheehy JL. Tympanoplasty: review of 400 staged cases. Laryngoscope 1990, 100(7):679-81.
14. Gersdorff M, Garin P, Decat M, Juantegui M. Myringoplasty: long-term results in adults and children. Am J Otol 1995, 16(4):532-5.
15. Wehrs RE. Hearing results in tympanoplasty. Laryngoscope 1985, 95(11):1301-6.
16. Albu S, Babighian G, Trabalzini F. Prognostic factors in tympanoplasty. Am J Otol 1998, 19(2):136-40.
17. Kageyama-Escobar AM, Rivera-Moreno MA, Rivera- Mendez A. Risk factors for myringoplasty failure. Gac Med Mex 2001, 137(3):209-20.
18. Wielinga EW, Derks AM, Cremers CW. Tympanosclerosis in the tympanic membrane: influence on outcome of myringoplasty. Am J Otol 1995, 16(6):811-4.
19. Onal K, Uguz MZ, Kazikdas KC, Gursoy ST, Gokce H. A multivariate analysis of otological, surgical and patientrelated factores in determing success in myringoplasty. Cin Otolaryngol 1995, 30(2):115-20.
20. Gonzales FC, Castro-Vilas C, Rodriguez Cabanas E, Elhendi W, Vaamonde L P. Caballero LT. Prognostic factors influencing anatomic and functional outcome in myringoplasty. Act Otorrinolaringol Esp 2002, 53(10):729-35.
21. Halik JJ, Smyth GD. Long-term results of tympanic membrane repair. Otolaryngol Head Neck Surg 1988, 98(2):162-9.
1. Resident doctor in ENT (Speech therapist)
2. PhD in ENT (Collaborator doctor at the service of residence at Hospital das Clínicas da UFPE)
3. Teacher of ENT (Adjunt teacher of residence program in ENT at Hospital das Clínicas da UFPE)
Hospital das Clínicas da UFP
Débora Bunzen Serviço de Otorrinolaringologia do Hospital das Clínicas - UFPE. 6º andar Av.Prof. Morais Rêgo, S/N. Cidade Universitária - Recife-PE - Phone (FAX)- 81-3217-4443/81- 3227-1513. e-mail: dbunzen@yahoo.com
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on July 2, 2006 and was approved on November 20, 2006 22:30:22.