INTRODUCTIONThe multiple sclerosis is an inflammatory and demyelinating disease of the central nervous system. It is admitted that the T cells, when activated by non determined autotigenous, on subjects with immunogenetic polygenic predisposition, transfer from the periphery to the SNC through the hematoencephalic barrier, an event which is considered essential in the pathogenesis of the demyelination. In addition to the genetic predisposition, there are non identified environmental factors which are associated to the MS (1,2).
The clinical forms of the MS may be divided into: a) benign; b) relapsing-remitting; c) transitional; d) secondarily progressive and; e) primarily progressive (3).
This disease mainly affects individuals between the second and the fourth decade of life, and mostly female (1,4)
The diagnosis is performed through a detailed anamnesis in addition to the results of computer tomography, encephalon magnetic resonance and cephalonrraquidinianus liquid analysis, which are important exams for the anatomic localization of the lesion and for the therapeutic procedures to be performed (3,5,6).
Its etiology is unknown, but there is a hypothesis to be caused by one or more viral agents, contracted during childhood, with late production of the clinical condition of the disease in patients with such predisposition (1,4).
Until the beginning of last decade, the treatment was performed with corticoid and other immunosuppressive agents with little efficient results and without interfering the disease's progression (3). In 1993, FDA approved and authorized the use of beta-interferon in the SM treatment in patients suffering from relapsing-remitting form. The interferons are proteins which are produced by all the vertebrate cells and work on the cell function and on the immunoregulation, used on the disseminated erythematous lupus, on the rheumatoid arthritis, on lynphangioma, and, more recently, on the MS (3). The authors also observed a tendency to reduce the number of outbreaks in a significant number of patients, a slower progression of the disease and that the interferons produced transitory side effects which were well tolerated by the patients.
The lesions of such disease are diffusely distributed through all the white substance with some predominance areas in the brain (periventricular and callous body). Clinical symptoms and signs due to the encephalic trunk tract, spinal medulla and optic nerves, in which mild morphophysiological changes may produce severe clinical manifestations (1,7,8). Such manifestations may present exacerbation periods intercalary periods of remission. (5,7,8).
Vertigo, unbalance and nystagmus are frequently mentioned as preliminary manifestations that occur before the verification of the disease's diagnosis (1,9).
The body balance depends on the integrity of the vestibular system (labyrinth, vestibulocochlear nerve, nucleus, ducts and inter-relations in the central nervous system), of the somathosensorial system (sensorial receptors which are located in tendons, muscles and articulations) and of vision (10,11). The labyrinth is responsible for the balance and the position of the body in space. Dizziness and/or unbalance appear when something interferes in the normal functioning of the body balance system, and it may be of peripheral or central origin (11).
The VENG is of great help in the precocious and differential diagnosis of the MS due to its sensitiveness and to its very close relation among its predominance locations (encephalic areas of skull posterior fossa) and structures that contribute to the maintenance of body balance (1,12).
Concerning audition, the authors (8,13) have observed audiometric characteristics of neurosensorial hearing loss with gradual decrease of high frequencies.
Sometimes MS is an otoneurological disease because some patients presented the first signs of such affection in the hearing and body balance sphere (12). Because of that, the objective of this study is to follow the behavior of the hearing and vestibular systems in relapsing-remitting SM patients within 1 year with continuous use of beta-interferon.
MATERIAL AND METHODOLOGYThis study has been approved by the Institutional Ethics Comittee record number 084/2003 and authorized by patients through the signature of the Term of Clear and Free Consent.
Eight patients have been evaluated, four of them being male and four being female aging from 27 to 59 years old (average age of 46 years old), with relapsing-remitting SM diagnosis according to McDonald et al criteria. (13), forwarded by the Instituto de Neurologia de Curitiba e da Associação Paranaense de Esclerose Múltipla (APAREM) to the Otoneurology Laboratory of Universidade Tuiuti do Paraná.
The casuistry is reduced due to the fact that some patients started using a wheelchair, which made the access to the evaluation department impossible, that some died and that some live in different cities. We point out the difficulty to gather all the patients of this research one year later to the first evaluation. Due to the reasons mentioned above and in order to give this study a proper continuation, we spread our association with the Neurology Department of Universidade Federal do Paraná.
The patients have being evaluated not taking into account the previous treatment period and (re) evaluated after one year of use of beta-interferon. We point out that the alterations observed in the present study when comparing the first and the second evaluation, once the evaluated patients had already been under treatment and kept it during the evaluation period. He patients have been submitted to the following procedures:
Neurological EvaluationThe patient used to be clinically evaluated (general and neurological) and laboratorially evaluated (screening for infectious and auto-immune diseases, complete liquor exam, protein immunoelectrophoresis and VDRL and HTLV-1 serology), visual evocated potential, skull and cervical medulla magnetic resonance with punctuation according to the Kurtzke scale (EDSS) (14).
AnamnesisA questionnaire has been applied which emphasized the otoneurological signs and symptoms, and the family and personal background.
Otorhinolaryngological EvaluationIt has been performed with the objective of excluding any alterations that could interfere the exam.
Conventional Hearing EvaluationThe frequencies 0.25 to 8 kHz through air have been investigated. The speech recognition threshold (SRT) and the speech recognition percentage rate have also been investigated. He equipment used was the interacoustic audiometer AC-40 model and TDH-39P models with threshold expressed in dBNA.
The Davis and Silvermann (15) and Silman and Silvermann classifications have been applied in order to characterize the kind and degree of hearing loss.
Measure of Acoustic ImmitanceThis procedure has been performed in order to evaluate the integrity of the tympanus-ossicular system through the tympanometric curve and through the acoustic reflexion investigation. The equipment that has been used was the interacoustic impedanciometer AZ-26 and earphones 39P. For the result interpretation, the Jerger criteria (17) have been applied.
Vestibular EvaluationThe patients have been submitted to the following tests that make the vestibular exam.
Without records- The nystagmus and positional vertigo have been investigated through the Bradt & Darrof maneuver(18).
- The spontaneous and semi-spontaneous nystagmus with open eyes, with front sight and at 30-drgree deviation to the left, to the right, up and down, have been investigated
With recordsTo perform vectoelectronistagmography, it was used a Berger thermosensitive device, VN316 model, with three record channels. After cleaning skin of periorbitary areas using alcohol, an active electrode is attached with electrolytic paste to the lateral angle of each eye and frontal medium line, forming an isosceles triangle, which made the identification of oblique, vertical and horizontal eye movements possible. This type of VENG has enabled in obtaining more accurate measurement of slow component speed (vestibular correction) of nystagmus.
It was also used a Ferrante adjustable height pendular swivel chair, a Neurograff visual stimulator, EV VEC model, and a Neurograff air otothermometer, NGR 05 model.
The following eye and labyrinth tests at VENG were performed according to PADOVAN AND PANSINI´S and MANGABEIRA-ALBERNAZ´S et al. criteria.
- Eye movement calibration;
- Spontaneous (open and closed eyes) and semi-spontaneous (open eyes) nystagmus research;
- Pendular Tracking research;
- Optokinectic nystgamus research;
- Pre- and post-rotatory nystagmus research at descending pendular rotatory test, stimulating lateral, anterior and posterior semicircular ducts;
- Research of pre and post-caloric nystagmus, performed on patients positioned with head and trunk leaned backwards at 60º, in order to properly stimulate lateral semicircular ducts. The air irrigation time in each ear at 42 degrees Celsius, at 20 degrees Celsius and at 10 degrees Celsius lasted 80 seconds for each temperature and the responses have been recorded with open eyes and then with closed eyes in order to observe the inhibiting effect of eye fixation. In this evaluation, direction, the absolute values of angle speed of slow component and the relation calculation of directional predominance and of labyrinthic predominance of post-caloric nystgamus have been observed.
Statistic MethodologyFor the statistic study, a descriptive analysis of anamnesis data has been performed. For the data analysis of the vestibular, immitaciometric and audiologic evaluations, the Proportion Difference Test has been applied and the significance level of 0,05 or 5% has been adopted for the rejection of nullity hypothesis.
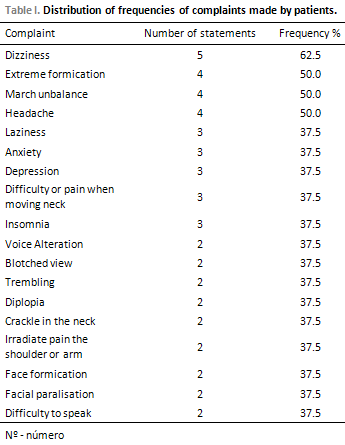
RESULTSConcerning the complaints which were mentioned in the anamnesis, predominance of dizziness (62.5%), of extremity formication (50.0%), of march unbalance (50.0%) and of headache (50.0%) have been observed, as displayed on Table 1.
Concerning the conventional hearing test that included the research of tonal threshold in the frequencies from 0.25 to 8 kHz, the research of SRT and of IPRF comparing the first and the second evaluation, alteration in the tonal threshold have been found in three patients (37.5%). The patient number 2 presented alteration in both ears. In the first evaluation, the exam had normal results and in the second evaluation a decreasing audiometric curve from the 4 kHz frequency with auditive threshold in 50 dB in the 6 and 8 kHz frequencies in the right ear and in 45 dB in the same frequencies in the left ear have become evident The patient number 3 presented alteration only in the left ear. In the first evaluation, a decreasing audiometric curve from the 4 kHz frequency has been observed and in the second evaluation a decreasing audiometric curve from the 3 kHz frequency with hearing threshold in 45 dB in the 4 kHz frequencies, in 55 dB in the 6 kHZ frequency and in 70 dB in the 8 kHz has also been observed. Lastly, the patient number 7 presented normal results in the first evaluation of his right ear and in the second evaluation a decreasing audiometric curve from the 6 kHz frequency on the same ear with hearing threshold in 55 dB in the 8 kHz frequencies, as displayed on Table 2.
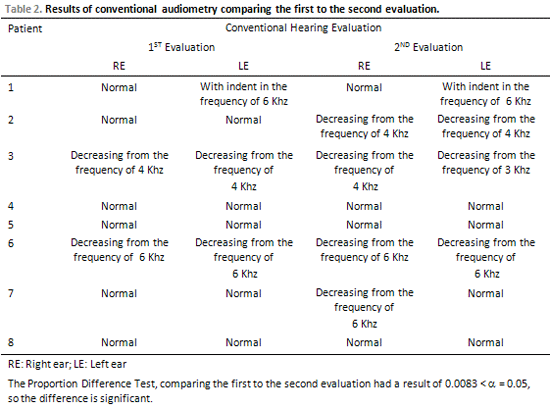
In the Proportion Differences Test application comparing the first and the second evaluation, it has been verified that there is a significant difference in the proportion of ears that suffered some kind of alteration.
Regarding the SRT and the IPRF, they did not present any kind of alteration, that is, they have been compatible with the tonal threshold.
In the immitanciometric evaluation, comparing the first and the second evaluation, alteration in three patients (37,5%) has become evident. The patient number 2 presented on the first evaluation a presence of acoustic reflex in the left year, and on the second evaluation of the same ear, an absence of acoustic reflex on the 3 and 4 kHz frequencies has been observed. The patient number 3 presented on the first evaluation an absence of acoustic reflex in the left ear in the 3 kHz frequency, and on the second evaluation of the same ear, an absence of acoustic reflex on the 3 and 4 kHz frequencies has been observed. The patient number 4 presented on the first evaluation an absence of acoustic reflex in both ears in the 3 kHz frequency, and on the second evaluation of the same ear, an absence of acoustic reflex on the 3 and 4 kHz frequencies has been observed. The tympanometric curve has been normal, that is, of "A" kind in all evaluated cases, as displays Table 3.
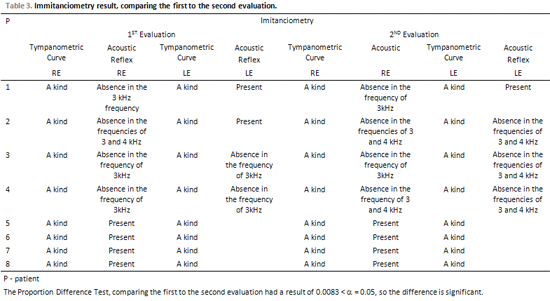
On the application of the Proportion Differences test, comparing the first to the second evaluation, it has been verified that there is significant difference in the proportion of ears that suffered alteration.
In the evaluation of the vestibular function, the investigation of positional, spontaneous and semi-spontaneous nystagmus without registration, eye movement calibration, spontaneous and semi-spontaneous nystagmus with registration, pendular tracking, pre and post rotatory optokinetic nystagmus, had no alterations.
The alteration in the exam has been predominant in the peripheral vestibular system and in the caloric test. Comparing the first to the second evaluation, alteration in three patients (37,5%) has been observed. The patient number 2 presented in the first evaluation an irritative peripheral vestibular syndrome to the left and in the second evaluation an irritative peripheral vestibular syndrome to both sides has become evident. The patient number 3 presented in the first evaluation a deficient peripheral vestibular syndrome to the left and in the second evaluation a deficient peripheral vestibular syndrome to both sides has been observed. The patient number 4 presented in the first evaluation an irritative peripheral vestibular syndrome to both sides and in the second evaluation a deficient peripheral vestibular syndrome to the right has become evident, as displays Table 4.
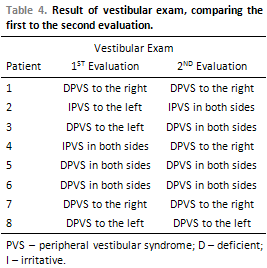
On the application of the Proportion Differences test, comparing the first to the second evaluation, it has been verified that there is no significant difference in the proportion of patients that suffered alteration.
DISCUSSIONIn the anamnesis analysis, psychological, vestibular, sensorial and motor symptoms have been observed, being dizziness, extremity formication, march unbalance and headache, the ones that have been mentioned the most. Several authors (4,9,20-23) mention, besides the symptoms described above, concomitant or isolated motor sensorial disorder in several degrees, laziness, depression and anxiety. According to several studies (24,25), one of the most frequent symptoms which are produced by the oculomotor vestibular system is the unbalance. It occurs because the demyelinating focuses are frequently located on encephalic areas of the skull posterior fossa.
Here is a great number of possible causes for the dizzinesses and they are described on around 300 otoneurological clinical condition with different clinical manifestations. Such variety may be explained through the labyrinth structure and physiology themselves, both in vestibular and hearing parts, which is very sensitive to physiological alterations that occur in other organs at distance and are frequently ethiologic agents of vestibular dysfunctions (26-27).
Absence of hearing symptoms has been observed in our study. We point out that the manifestations vary from patient to patient and may develop in periods of exacerbation and remittance of the disease as years go by.
Regarding the conventional hearing evaluation, comparing the first to the second evaluation in our study, significant alteration in the proportion of altered ears has been verified. A drop of the hearing sensitiveness in high frequencies has become evident. Some authors (12) have observed audiometric profiles initially demonstrating hearing loss in the high frequencies with normal tonal sensitiveness in the low and medium frequencies in a significant number of ears. Tu and Young (8) and Munhoz et al. (28) related, on their studies, sensorineural hearing loss. Colletti (29) states that only 4% of the evaluated patients present some kind of measurable change in the conventional audiometry, not mentioning the affected frequencies.
Some studies reveal that one potential consequence of desmyelination of hearing pathway cause interruption in the perception of some frequencies. The desmyelination may harm a great quantity of fibers of the nerve that conducts the stimulation, harming the transmission of high frequency signs but not the low frequency ones. (12)
In the acoustic immittance measurement it has been verified in our study a normal tympanometric curve of "A" kind in all studied cases and significant alteration in the proportion of altered ears in the research of acoustic reflex, when the first and the second evaluation were compared. Alterations in the research of acoustic reflex have also become evident in the Colletti studies (29), in which the percentage of alterations varied from 8% to 90% of the cases.
In the vestibular exam there has been alteration in the caloric test. Comparing the first to the second evaluation, the evident alteration has not been significant in the proportion of altered patients. The alterations were predominantly found in the peripheral vestibular system. Such finding may have happened due to the disease of the patient, which little affects vestibular structures regarding the central nervous system at the moment. Some studies (9) state peripheral and/or central otoneurological manifestations, isolated or combined. They also state that the vestibular signs are determined by the desmyelination boards in the areas of vestibular nucleus in the 4th ventricle ground.
N our results, we point out irritative and deficient peripheral vestibular syndromes, in one or both ears. Such findings are suitable to several researches (4,8) which also pointed out such alterations. Mangabeira-Albernaz et al. (4) also observed absence of EIFO.
Some authors (1) state that the most common electronystagmographic findings in the MS are alterations of inducted eye movements in the saccadic movements, in the pendular tracking research, in the optokinetic nystagmus research and mainly in the post-caloric nystagmus research.
Several studies state that the loss of ciliated cells of the ampullar crests and of maculae, the decrease in the number of nerve cells of the Scarpa's ganglion, the otoconium degeneration, the reduction of the labyrinthic blood flow, the progressive depression of the neural stability, reduction in the capacity of compensation of ocular-vestibule reflex (which is responsible for keeping the sight stable during head movement) and spinal-vestibule reflex (which is responsible for body stability) all contribute for the speed reduction of following movements and for the caloric and rotational hyporeactitivty of the vestibular system both at central and peripheral level (30).
We point out that there is not a pathognomic picture of the MS in the evaluation of hearing and vestibular systems. Because the disease is diffuse, it has a great variety of clinical manifestations which, most of the times, affect the patient in acute or subaccute episodes of recurrence with variable remittance, which mat affect several structures of the vestibular system both in central and in peripheral level.
CONCLUSIONAlterations in the exams performed after one year of treatment have become evident, when the first and the second evaluation were compared.
In Brazil, there are few epidemiological studies about the SM. Studies on eye alterations are also rare, mainly in Latin-American countries.
We point out the importance of the functional study of the vestibulocochlear system in this kind of population, as well as the inclusion of vestibular exam as clinical routine.
REFERENCES1. Aantaa E, Riekkinen PJ, Frey HJ. Electronystagmographic findings in multiple sclerosis. Acta Otolaryngol., 1973, 75(1):1-5.
2. Compston A, Coles A. Multiple sclerosis. Lancet, 2002, 359:1221-31.
3. Tilbery CP, Felipe E, Moreira M, Mendes MF, França AS. Interferon Beta-1 A na esclerose múltipla. Arq. Neuropsiquiatr.,2000, 58(2B):452-59.
4. Mangabeira-Albernaz PL, Ganança MM, Mangabeira- Albernaz PM, Settanni FAP, Caovilla HH, Falsetti HDC e 'et al.'. Aspectos otoneurológicos na esclerose múltipla. Acta Awho, 1983, 2(2):35-42.
5. Arruda WO, Scola RH, Teive HA,Werneck LC. Multiple sclerosis: report on 200 cases from Curitiba, Southern Brazil and comparison with other Brazilian series. Arq. Neuropsiquiatr.,2001, 59(2A):165-70.
6. Poser CM, Brinar VV. Diagnostic criteria for multiple sclerosis. Clin Neurol Neurosurg., 2001, 103:1-11.
7. Sibinelli MAMF, Cohen R, Ramalho AM, Tilbery CP, Lake JC. Manifestações oculares em pacientes com esclerose múltipla em São Paulo. Arq.Bras.Oftal., 2000, 63(4):287-91.
8. Tu CE, Young YH. Audiovestibular evolution in a patient with multiple sclerosis. Ann Otol Rhinol Laryngol., 2004, 113(9):726-29.
9. Ganança MM, Caovilla HH, Munhoz MSL, Silva MLG, Settanni FAP. Tumores e doenças desmielinizantes da fossa posterior. In: Silva MLG, Munhoz MSL, Ganança MM, Caovilla HH. Quadros otoneurológicos mais comuns. São Paulo: Atheneu: 2000. p.131-43.
10. Mangabeira-Albernaz PL, Ganança MM, Pontes PAL. Modelo operacional do aparelho vestibular. In: Mangabeira- Albernaz PL, Ganança MM. Vertigem. 2.ed, São Paulo: Moderna: 1976. p.29-36.
11. Jurkiewicz AL, Zeigelboim BS, Mangabeira-Albernaz PL. Alterações vestibulares em processos infecciosos do sistema nervoso central. Distúrb. Comum., 2002, 14(1):27-48.
12. Tomaz A, Borges FN, Ganança CF, Campos CAH, Tilbery CP. Sinais e sintomas associados a alterações otoneurológicas diagnosticadas ao exame vestibular computadorizado em pacientes com esclerose múltipla. Arq. Neuropsiquiatr., 2005, 63(3B):837-42.
13. Bentzen O, Jelnes K, Thygesen P. Acoustic and vestibular function in multiple sclerosis. Acta Neurol Scand., 1951, 26:265-95.
14. McDonald WI, Compston A, Edan G, Goodkin D, Hartung HP, Lublin FD e 'et al'. Recommended diagnostic criteria for multiple sclerosis: guidelines from the international panel on the diagnosis of multiple sclerosis. Ann Neurol., 2001, 50(1):121-27.
15. Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology, 1983, 33(11):1444-52.
16. Davis H, Silverman RS. Hearing and deafness. 3ª ed. New York: Holt, Rinehart & Wilson: 1970. p.253-79.
17. Silman S, Silverman CA. Auditory diagnosis, principles and applications. London: Singular Publishing Group: 1991. p.215-32.
18. Jerger J. Clinical experience with impedance audiometry. Arch Otolaryngol., 1970, 92:311-24.
19. Brandt T, Daroff RB. Physical therapy for benign paroxysmal positioning vertigo. Arch Otolaryngol., 1980, 106:484-5.
20. Padovan I, Pansini M. New possibilities of analysis in electronystagmography. Acta Otolaryngol., 1972, 73:121-5.
21. Ganança CF, Ganança FF, Ganança MM, Caovilla HH, Munhoz MSL, Silva MLG. Vertigem posicional paroxística benigna e esclerose múltipla. In: Munhoz MSL, Ganança MM, Caovilla HH, Silva MLG. Casos clínicos otoneurológicos típicos e atípicos. São Paulo: Atheneu: 2001. p.207-08.
22. Murbach V. Schwannoma vestibular e síndromes vestibulares centrais. In: Munhoz MSL, Ganança MM, Caovilla HH, Silva MLG. Casos clínicos otoneurlógicos típicos e atípicos. São Paulo: Aheneu: 2001. p.107-15.
23. Mendes MF, Tilbery CP, Balsimelli S, Moreira MA, Barão-Cruz AM. Depressão na esclerose múltipla forma remitenterecorrente. Arq. Neuropsiquiatr., 2003, 61:591-95.
24. Alpini D, Caputo D, Pugnetti L, Giuliano DA, Cesarani A. Vertigo and múltiple sclerosis: aspects of differential diagnosis. Neurol Sci., 2001, 22(2):584-87.
25. Maudonnet O, Maudonnet E. Causas centrais da vertigem. In: Campos CAH, Costa HOO. Tratado de Otorrinolaringologia. 2.ed, São Paulo: Roca: 2002.
26. Silva MLG, Munhoz MSL, Ganança MM, Caovilla HH. Quadros clínicos otoneurológicos mais comuns. São Paulo:Atheneu: 2000.
27. Ganança MM, Caovilla HH, Ganança C.F. Vertigem e sintomas correlacionados, avaliação funcional do sistema vestibular. In: Ganança MM. (coord) Vertigem: abordagens diagnósticas e terapêuticas. Fascículo I. São Paulo: Lemos: 2002.
28. Munhoz MSL, Silva MLG, Ganança MM, Caovilla HH, Frazza MM. Labirintopatias auto-imunes. In: Silva MLG, Munhoz MSL, Ganança MM, Caovilla HH. Quadros otoneurológicos mais comuns. São Paulo: Atheneu: 2000. p.131-43.
29. Colletti V. Stapedius reflex abnormalities in multiple sclerosis. Audiology. 1975, 14(1):63-71.
30. Hain TC, Ramaswamy TS, Hillman MA. Anatomia e fisiologia do sistema vestibular normal. In: Herdman SJ. Reabilitação vestibular.2ª.ed. São Paulo: Manole: 2002. p.3-24.
1. Medical Doctor (Coordinator of PhD and Mastering Program in Speech Disorders of Universidade Tuiuti - Paraná)
2. Master (Assistant Professor of the Neurology Department of Universidade Federal - Paraná)
3. Professor (Professor of Speech therapy Department of UNIFESP/Escola Paulista de Medicina)
4. PhD (Professor of PhD and Mastering Program in Communication Disorders of Universidade Tuiuti - Paraná)
5. Master
Setor de Otoneurologia da Universidade Tuiuti do Paraná (UTP).
Bianca Simone Zeigelboim - Rua: Gutemberg, 99 - 9º andar-CEP 80420-030 -Curitiba/Pr - Phone/Fax(41)3331-7807 - E-mail: bianca.zeigelboim@utp.br.
Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq).
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on August 7, 2006 and was approved on September 27, 2006 22:30:22.