INTRODUCTIONAlthough adenotonsillectomy is the most frequent surgery method performed by ENT doctors, its frequency has not been often used in the last decades1. It's a type of surgery in which patient develops with no severe variations, and is released from hospital less than 24 hours after it. Due to development of anesthesia and surgical techniques, complications have been reduced, though there are potentially fatal risk(1,2).
The most frequent complications are self-limited and disappear during cicatrisation process, such as odynophagia, dry cough, nauseas, vomiting, otalgia (by gloss pharyngeal nerve), low fever and other(3). There are also more severe complications such as post-surgery bleeding, infection or pulmonary oedema(4).
Cervical emphysema is a rare complication, but it can occur after tonsillectomy surgery(1,5). The complication described affected profound spaces in the neck of a healthy adult submitted to tonsillectomy surgery due to peritonsillar abscess and recurrent infection, discussing aspects related to physiopathology, diagnosis and procedure.
CASE REPORT A 20-year-old healthy patient with no medication use was hospitalized in order to be submitted to tonsillectomy due to repetition peritonsillar abscess to the right (2 episodes), and peritonsillar abscess to the left (1 epidose). Around 1 month before surgery, patient presented peritonsillar abscess to the left, treated with punction (with no purulent secretion) and antibiotic therapy using gatifloxacin. Patient improved slowly, and had tonsillitis episode after antibiotic therapy interruption, then was treated with amoxacilin with clavulanate and after 7 days was submitted to surgery.
Patient denied bleeding after dental procedures or accidents. S/he presented preoperative hemogram exam and coagulogram with no alteration. At physical exam, patient presented moderate tonsillar hypertrophy (grade II), and cervical palpation with no alterations.
Patient was submitted to tonsillectomy under general anesthesia with orotracheal intubation, performed through dissection of the tonsillar surface with difficulty due to fibrosis and adherence to more profound layers which, if associated with bleeding, make procedure difficult. Hemostasis was performed through bipolar scalpel and arterial ligation of a higher calibration vessel with haemostatic point to the right, side that bleeding occurs in greater amount. Patient condition developed well, and was released from hospital after 8 hours of development.
Around 24 hours after procedure, s/he presented flaccid, painless and non-creptant progressive cervical bulging to the right in submandibular area. S/he complained of adinophagy, but no dyspnea. Oroscopy did not presented bleeding on the surgical surface, but presented oedema and palate bulging and tonsillar pillar to the right. Nasoendoscopic exam presented medianization on the pharynx lateral wall to the right.
CT from the neck was performed in order to clarify and extend the process which showed presence of air in parapharyngeal and right submandibular spaces (Pictures 1,2,3,4). Presence of fluid or soft areas thickening from the neck was not observed. Besides, emphysema did not present extension to infrahyoid spaces.
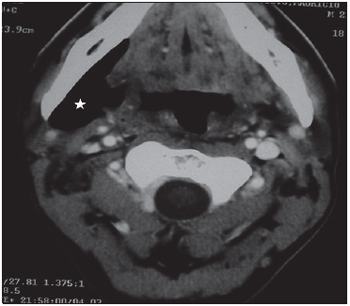
Picture 1. CT, axial cut, highlighting involvement of the right submandibular space by cervical emphysema.
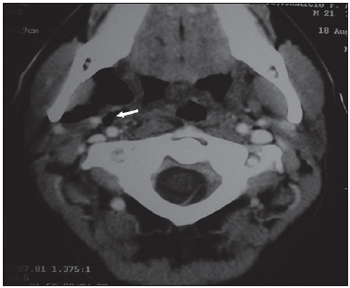
Picture 2. CT, axial cut, showing emphysema extension to parapharyngeal, adjacent to carotid spaces.
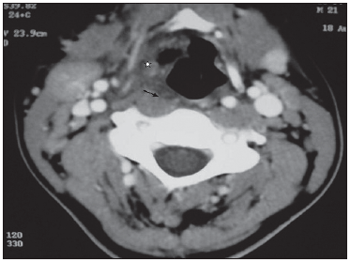
Picture 3. CT, axial cut, showing involvement of paraglotic space (star) and right retropharyngeal thickening (arrow).
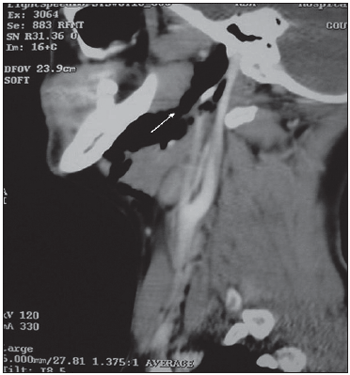
Picture 4. CT, sagital cut, showing cervical emphysema extension to the cranium base.
Patient remained under observation, diet, prophylactic antibiotic therapy with amoxacilin and clavulanic acid for 10 days. S/he developed with no fever, no variations with spontaneous reduction of bulging after 72 hours.
DISCUSSIONTonsillectomy is one of the most frequent performed surgeries and it usually develops with severe variations(1). Death rate is around 1 in each 35,000 of the cases, and it is normally related to anesthesic complications(3). Other types of potentially fatal complication are pulmonary oedema, which usually occurs during surgery process or soon after it, and post-operative bleeding(2,6). Bleeding usually occurs in the 24 first hours after procedure in 2 to 5% of the cases(3). Fatal bleeding is rare (less than 0.0002%6 of cases)(6).
Cervical emphysema is a type of complication that can occur in any surgical procedure in oral cavity and oropharynx, in which there is loss of mucosa integrity. There are reported cases of cervical emphysema that occur after teeth extraction and bucal, maxillary and facial procedures. Cervical emphysema as tonsillectomy complication is rare(5). The occurrence of pneumomediastimum is even more rare (less than 5 cases after 1955(6)). But there are other factors involved in its physiopathology besides loss of mucosa integrity5.
Cervical emphysema is caused by air from high aero digestive pathways. In these cases it is of secondary consideration to procedures of high digestive endoscopy or foreign body trauma(6). The process through which air release occurs can be by a primary imperfection on the mucosa from aero digestive pathway or by pressure increase leading to an alveolar rupture(5). The result of continuous mucosa can be a consequence of surgical trauma or complication of a traumatic intubation what led to a hypopharynx, larynx or trachea lesion(7). In this way, air is released and it dissects through fascial planes to mediastimum inferiorly, or in superiorly towards oropharynx and rinopharynx(6).
The increase of alveolar pressure and air pathways can be caused by a positive high pressure in the mouth or excessive manual ventilation. There are physiological mechanisms that also increase pressure on air pathways such as excessive coughing, sneezing, nausea, vomiting and even nose blowing(8). There is, in the literature, cases of pneumomediastimum and post-tonsillectomy cervical emphysema whose first symptom was rhinolalia¸ beginning soon after a nose blowing, what spreads emphysema to rhinopharynx and hiponasal voice(6).
In the post-tonsillectomy cervical emphysema, it is believed that the air penetrates the surgical surface through mucosal lesion or through a porous surface caused by profound dissection facilitated by the increase of intrapharyngeal pressure caused by cough, vomit or manual ventilation after extubation(8). Air goes through superior constrictor muscle dissecting through cervical fascial planes in order to achieve parapharyngeal space. And it can achieve retropharyngeal space and mediastimum(2). When pneumomediastimum occurs with no sign of subcutaneous emphysema, air can be penetrated through cervical vascular space or through retropharyngeal spaces in superior manner. From mediastimum, emphysema spreads to peritoneal cavity through diaphragmatic opening, especially esophagus and aortic ones.
There are authors who suggest that more profound peritonsillar infiltration of the surgical surface can favor air entrance, making cervical emphysema occurrence easier(2). Besides, there are cases of profound cervical abscess and vocal folds palsy after local anesthesic peritonsillar infiltration in tonsillectomy(10).
In the reported case, peritonsillar infiltration did not occur. Fibrosis caused by chronic infection process associated with excessive bleeding during procedure made dissection of tonsil surgical bed difficult, favoring superior constrictor muscle lesion. Solution of continuity might have been raised with parapharyngeal space that accelerated air accumulation by a valve process, probably after an increase of intra-pharyngeal pressure. The process achieved submandibular space. At the physical examination, it was observed bulging on pharynx lateral wall, causing involvement only of profound spaces of the neck.
There are also cases of cervical emphysema after tonsillectomy with the use of "Argom Beam Coagulator", instrument used in order to help on hemostasis, but it causes air flow(11). It is believed that it could predispose to emphysema increasing intra-pharyngeal pressure. The differential diagnosis of early cervical bulging is essential after surgery with other pathologies that might lead to oedema such as hemorrhage, allergic reaction and angioneurotic oedema(2,10).
In these cases, bulging features, occasional creptation and findings of image clear the diagnosis. The abscess of parapharyngeal space can also be tonsillectomy complication as a consequence of a breakage of the protection barrier of the mucosa, causing cervical bulging. It usually occurs later (from 24-28 hours), it presents progressive development with hardening and phlogistic signs on the neck, odinophagy, dysphagia, prostration and fever.
It affects more often patients with infection on surgical surface and immune depressed ones, and it can be eased with local anesthesia. Diagnosis is important in patients with progressive dysphagia and odinophagy after surgery, even in those who presents normal oropharynx appearance at the physical exam(1). In the reported case, good condition of the patient, bulging softened at palpation and quick development might help. Another condition that leads to cervical lemphysema is the necrotizing fasciitis(8). It is an extremely aggressive infection, with quick diffusion through fascial planes. The process takes gangrene to subcutaneous tissue and cervical fascials, quickly involving muscles, skin and adjacent tissues. It is usually related to odontogenic infections or trauma, though it can occur after tonsillectomy(4). Immunocompromised patients are more sensitive, especially when submitted to surgery under infection situation1. Though, in patients with immunological shortage, the breakage of the protection barrier of the mucosa causes bacteria diffusion especially the comensal ones from oropharynx (mixed flora of aerobic and anaerobic), even in the absence of infection conditon(3). At the physical exam, it can be observed creptation of subcutaneous tissue together with cervical bulging and phlogistic signs, in patients with sign of septicemia, opposing the reported case. In the radiology exams, besides cervical emphysema, it can observed oedema with soft parts, with occasional collection. It is compulsory the early diagnosis and aggressive surgical treatment in all cases due to high rate of mortality(3).
Although development of cervical emphysema is usually benign and self-limited, heart and respiratory complications might occur(3,6). In children, tracheal rings are less resistant and massive emphysema might lead to compression and obstruction of the trachea-bronchial tree. When associated pneumomediastimum occurs, heart compression with debt reduction and pneumothorax can affect ventilatory function, causing hypoxia.
Procedure is expectant in most cases(8). It is compulsory observing ventilatory and heart function, and clinically evaluating emphysema development. Patients should be advised to avoid situation which might cause intra-pharyngeal pressure such as cough, vomit, and physical effort(5). In more severe cases, with extensive emphysema or pneumomediastimum, patients should remain in hospital under monitoring of cardiac function and saturation. Thoracic drainage is rarely necessary to pneumothorax treatment. Antibiotic therapy with coverage to germs from oral cavity (Anaerobic gram-positive) in order to prevent infection is recommended, as there is breakage of oral mucosa barrier diffusing bacteria(2). In the reported case, patient developed with emphysema regression after 72 hours with no complications and to prophylaxis s/he made use of amoxacilin with clavulanate acid.
FINAL CONSIDERATIONS Cervical emphysema is a rare complication which might occur as tonsillectomy. Differential diagnosis, with conditions which lead to quick cervical bulging, especially infectious and hemorrhagic ones, is essential. CT is helpful to differential diagnosis and evaluation of the process extension. Although its development is benign, it is important to follow up and to observe patients up to their resolution.
REFERENCES1. McEwan JA, Dhingra J, Rowe-Jones J, Bleach NR. Parapharyngeal abscess: a rare complication of elective tonsillectomy. J Laryngol Otol 1997; 111:578-9.
2. Marioni G, Filipis C, Tregnaghi A, Gaio E, Staffieri A. Cervical enphysema and pneumomediastimum after tonsillectmy: it can happen. Otolaryngol Head Neck Surg 2003; 128:298300.
3. Sonne JE, Kim SB, Frank DK. Cervical necrotizing fasciitis as a complication of tonsillectomy. Otolaryngol Head Neck Surg 2001; 125:670-2.
4. Tami G, Parker G, Taylor R. Post-tonsillectomy bleeding: an evaluation of risk factors.Laryngoscope 1987; 97:1307-11.
5. Hampton SM, Cinnamond MJ. Subcutaneous emphysema as a complication of tonsillectomy. J Laryngol Otol 1997; 111:1077-8.
6. Baverman I, Rosenmann E, Elidan J. Closed rhinolalia as a symptom of pneumomediastinum after tonsillectomy: a case report and literature review. Otolaryngol Head Neck Surg 1997; 116:551-3.
7. Levine PA. Hypopharyngeal perforation: an untoward complication of endotracheal intubation. Archives of Otolaryngology 1980; 106:178-180.
8. Smelt GJC. Subcutaneous emphysema: pathological and anaesthetic, but not surgical. J Laryngol Otol 1984; 98:647-54.
9. Vos GD, Marres EH, Heineman E, Janssens M. Tension pneumoperitoneum as an early complication after adenotonsillectomy. J Laryngol Otol 1995; 109:440.
10. Fradis M, Goldsher M, David JB, et al. Life-threatening deep cervical abscess after infiltration of the tonsillar bed for tonsillectomy. Ear Nose Throat J 1998; 77:418-21.
11. Fechner FP, Kieff D. Letter to the editor. Laryngoscope 2003; 113:920-1.
1. Former resident physician and preceptor, HCFMUSP (Medical Employee of the Division of Clinical Otorhinolaryngology, HCFMUSP).
2. Professor Free-Teacher (Associate Professor of Discipline of Otorhinolaryngology, HCFMUSP. Bucofaringolaringologia Director of the Office of the HCFMUSP).
3. Scholar FMUSP (Scholar of the sixth year of the Faculty of Medicine, USP).
4. Doctor of Otolaryngology by FMUSP (Medical Assistant of the Division of Clinical Otorhinolaryngology, HCFMUSP).
5. Professor Free-Teacher (Head of the Group of Voice of HCFMUSP).
Division of Clinical Otorhinolaryngology, HCFMUSP.
Felipe Sartor Guimaraes Strong
Correspondence: Fernando Cardim Street, 161 - Apart. 154 - Jd. Paulista - Sao Paulo / SP - Brazil - CEP: 01403-020 -- Fax: (12) 3922-4422 - E-mail: fsgfortes@yahoo.com.br
This article was submitted in Management System Publications in the R@io 17/6/2006 and approved on 23/8/2006 00:31:57.