INTRODUCTION The respiratory system is made of two basic components, the lungs and the thorax wall (1) besides being constituted by many organs which conduct air in and out of the pulmonary cavities. These organs are the nasal fossae, the mouth, pharynx, the larynx, the trachea, diaphragm, the bronchi, the bronchioles and the alveoli, the three last ones located in the longs. The passage of air through the nose is basic, once there is the preparation of air to reach the lungs in the best conditions for oxygen absorption.
The breathing process occurs thanks to the movements that increase and diminish the thorax making the air to be inspired to the lungs and then expired.
The movement of the thoracic cage is carried through by the muscular action together with the external and internal intercostal muscles and mainly of the diaphragm, which makes the diameter of the thorax increase vertically with its contraction(2). Other muscles also work during the forced breath, such as scalene and the sternocleidomastoid. The calm expiration is passive; however a forced expiration has the aid of the abdominal and inner intercostal muscles.
The thoracic movement only becomes possible when there is enough force to win the elastic retraction and the resistance to the air flow.(3)
The high airways are the greatest responsible for the increase of the resistance with the increase of the air flow, therefore factors that modify the diameter of the airways can modify the resistance. The blockage of the superior airways leads to a oral breathing, which harms the ventilation and the thoracic expansion, resulting later in disorders of the thoracic cage development among other face, dental and vertebra alterations(1).
The hyperplasia of tonsillas is one of the main factors for the superior airways blockage and for symptoms that usually are reversible after the adenoidectomy or tonsillectomy. Reports from the 1980s inform that children with adenoid and tonsil hypertrophy presented this pathology as a reversible cause of the lack of growth of children(4).
The pharyngeal tonsil is of lymphoid nature, which may be found in infants, however it is more frequent in children. A natural trend of involution exists after during and the puberty, whereas the hyperplasia of palatine tonsils, amygdales, is characterized by an irreversible increase, once the hyperplasia of the lymphoid elements occurs. Only at adult age, with physiological involution of lymphoid tissue, there is reduction of tonsils(5).
Cheng (1988) in its study with oral breathing children, proved that the younger the child, the less alterations due to the blockage of superior airways they present, which suggests that, with their growth these alterations will go increase(6).
When these organs involute, the bone development is advanced and suffered the action from the soft parts that work in association, as the theory of Functional Matrix by Moss explains, demonstrating that the bone growth occurs in response to the functional relations(6).
Other important alterations are results of the blockage of superior airways such as cough as consequence of inspiration of dry and cold air, pulmonary hypertension and cor pulmonale, diurnal sleepiness, unsynchronized sleep. Morning migraine, irritability, problems of learning, hyperactivity, aggressiveness and growth retardation can occur(7).
In the past there were controversies related to the fact of whether or not adenoamigdalectomies should be performed. Currently it is possible to define absolute indications for the performance of the surgery, among which is the blockage of nasopharynx through hyperplasia of palatine or pharyngeal tonsils which cause respiratory discomfort or frequent episodes of sleep apnea and cor pulmonale, and reasonable indications to carry out the surgery. The results are satisfactory in cor pulmonale cases and in precocious alterations of dentitions, as well as in children with recurrent respiratory and ear problems(8).
Based on the data above we considered a study for the evaluation of the thoracic perimeter in children with hyperplasia of pharyngeal and palatine tonsils.
Considering the importance of correct breathing, the increase of tonsil volume and the scarcity of objective data on its repercussion, the present study aimed at evaluating the thoracic perimeter in children with increase of tonsil volume.
MATERIAL AND METHODS The protocol was submitted and approved by the Comitê de Ética e Pesquisa da Disciplina de Otorrinolaringologia and by Hospital das Clínicas in 2002. The authorization of the patients or their tutors was gotten before carrying out the test, through the signature of the Term of Free and Clarified Consent.
73 children (aging 4 -13 years) were included in the evaluation, both male and female. There was not race distinction, so white, black, yellow or light brown children participated on this study, all of whom with diagnosis of blockage of superior airways due to increase of the volume of tonsils assisted in the clinic of Divisão de Otorrinolaringologia do Hospital das Clínicas/ Faculdade de Medicina da Universidade de São Paulo in the period between October, 2003 and May, 2005.
The research was characterized as quantitative, descriptive and experimental. The population studied was composed by the children evaluated in the group of children with surgical indication for adenoamigdalectomy in the otorhinolaryngology meeting. The studied sampling was sequential (not accidental probabilistic accidental, that is, at random). The observation of the sample was carried through in a systematic and individual way.
All the evaluated children agreed on undergoing the requested examinations and later the terms of the free and clarified assent have been signed and dated by the parents or tutors.
The gravity of the blockage of palatine tonsils was classified according to criteria described by BRODSKY (9) (Table 1), including the patients with blockage of degrees III and IV. The measure of the diameter of the thorax was carried out through the use of a conventional tape measure (Manufacturer: Fiber-Glass Japan Buttefly - graduation in millimeters 01-150cm). The measuring was carried through at the level of nipples after a calm expiration. The same patients have been evaluated in terms of the muscular force measured through a manovacuometer device that measures the inspiratory and expiratory pressure through an oral inspiration or expiration (Manufaturer Gear- resulted supplied in centimeters of water, variation of the values from 0 to 120 cm/ H2O). The pulmonary volume has also been evaluated through a pediatric incentive inspirometer (DHD 22-2000).
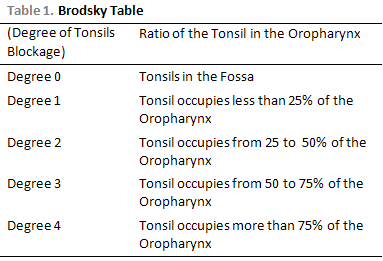
Seven children have been excluded, for presenting blockage lower than Degree 3 according to Brodsky table, twelve children have been excluded for being younger than 6 years old, once we do not have control group for this age and two obese children have also been excluded. The total of children for the study was of 52 children.
A control group was created in order to get a comparative thoracic perimeter number in relation to the group with increase of tonsils volume, once we did not find in literature value of normality in the studied age.
The children evaluated in the control group belonged to the Casa de Apoio Madre Clélia and have been evaluated under the authorization of the parents and institution. These children did not present increase of tonsils or other respiratory problems, and were as old as the studied group.
In the control group 57 children have been evaluated (of both genders) aging from 6 up to 13 years. Twelve children, for presenting throat infection or for having increase of the tonsils volume, and two obese children have been excluded. Total of children for the study was of 43.
Patients with asthma, children with neurological compromise, obese children, children who did not understand what was being requested or did not collaborated with the execution of the complementary examinations have been excluded from the study.
The statistical analysis was carried out through by the non-parametric method, Mann-Whitney Rank Sum Test. This test aims at verifying if the two samples come from the same distribution. The null hypothesis is that the two samples are extracted from only one population, and consequently that its distributions of the probability are equal.
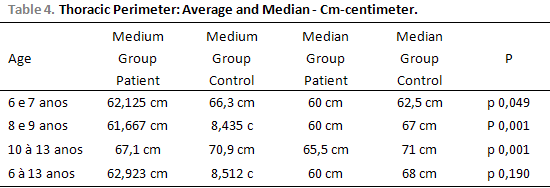
RESULTSThe thoracic perimeter which was obtained was significantly different comparing the two groups: 62.923 cm ± 7.715 (52-85) in the group of increase of tonsils volume (n=52) and 68.512 cm ±6.933 (57-88) in the control group (n=43). There is a statistical difference between the groups (P = <0.001). Figure 1.
When the groups were evaluated according to age, it has been verified: thoracic perimeter = 62.125 cm± 8.311(52 -85) in the group of increase of tonsils volume (n=24) and 66.300 cm ± 9.166 (57-88) in the control group (n =12) between 6 and seven years old, statistically significant difference (P = 0.049). Figure 2.
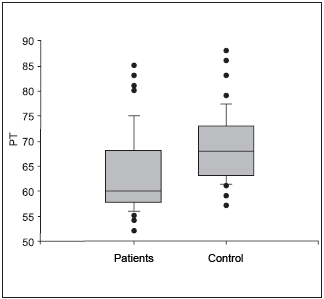
Figure 2. Thoracic perimeter in 6-to-7-year-old children of both genders. - PT- Thoracic Perimeter
The thoracic perimeter analyzed between 8 and 9 years old demonstrated the result 61.667 cm ± 6.490 (55-80) in the group of increase of tonsils volume (n =18), 68.435 cm ± 6.639 (59-86)? in the control group (n =23), thus producing a statistical significant difference between the groups (P = <0.001) Figure 3.
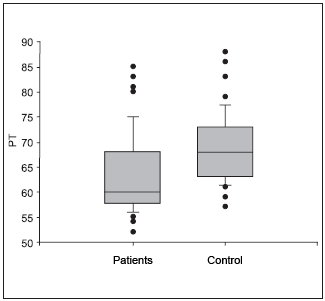
Figure 3. Thoracic perimeter in 8-to-9-year-old children of both genders. - PT- Thoracic Perimeter.
From 10 to 13 years old, the group of increase of tonsils volume presented thoracic perimeter of 67.100 cm ± 7.549 (57-81) (n = 10). The control group with thoracic perimeter of 70.900 cm ± 4.557 (64-79) (n =10). There is no statistically significant difference between the groups (P = 0.190). Figure 4
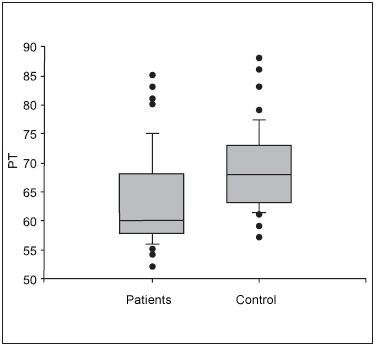
Figure 4.Thoracic perimeter in 10-to-13-year-old children of both genders. - PT- Thoracic Perimeter
The increase of tonsils volume is one of the main causes for respiratory problems during sleep. The oral breath and the snore are common symptoms in children (10). There are no reports on the measure of the thoracic perimeter in children with increase of tonsils volume. In the present study, children with increase of tonsils volume presented minor Thoracic Perimeter than the children of the control group. These children present mechanical difficulty to breathe through the superior airways, and in order to survive they search for an airway that presents minor resistance to air passage, thus carrying through oral breath.
The hyperplasia of tonsils leads to a relaxation of the face musculature as well as of all the body of the child, resulting in a out-of-alignment position. The corporal position has great influence in the respiratory capacity. Children with increase of tonsils present a relaxed facial musculature, kyphosis and slower growth (weight and height) than the children with normal tonsils (11). The respiratory capacity depends on a position of muscular balance, being also more efficient in spending energy. Kyphosis, kyphoscoliosis and pectus excavatum restrict respiration, leading to a reduction of the complacency of the thoracic wall. (12)
Bones are the second most solid substance of the human body. Despite this, when submitted to small forces for long periods it is extremely susceptible to deformations. The oral breath demands the use of a different musculature from the one used during a nasal breath (7). The consequence is a change in the muscular forces that act on the thorax. We understand, through 1980s' reports that the children with adenoamigdalian hypertrophy presented this pathology as a reversible cause of the lack of growth.(4)
The biggest period of growth of children occurs in their first years of life. Their weight doubles in the first five months as well as their height during the three first years. In the fourth year their craniofacial formation will have reached 60% of the adult characteristics.(7)
Some studies point out an increase of the growth (Weight and height) after adenotonsilectomy in children assisted during one year after the surgery. The increase of tonsils volume does not lead to retardation of the growth, however slower growth is associated to it. (13) (14) Such fact can be associated with the smaller thoracic perimeter.
By means of all the information above we conclude that, children with blockage of superior airways due to hyperplasia of tonsils carry through an oral breath, for they search for an airway of lesser resistance to the air passage once the superior airways are obstructed. This process leads to a lesser muscular effort since the resistance found for the oral breath is lesser than the one through the nasal breath. The result is a weaker respiratory musculature and a lesser thoracic expansibility and thus a lesser thoracic perimeter, as shown in the results gotten in the research described in the item 3, "Results". The data show a difference between the thoracic perimeters of children of the 04 to 13 years group without increase of palatine tonsils in relation to children with increase of tonsil volume. There are differences between the 6-7 years group and 8-9 years group. The group of 10-13 years did not demonstrate statistically significant difference.
These children need to be treated, once the increase of the tonsil volume leads the alterations of facial tonus, in the long run, craniofacial morphologic alterations and of occlusion, with reduction of the force of the respiratory musculature. Moreover, the quality of life of the child is harmed.
CONCLUSIONThe increase of volume of palatine and pharyngeal tonsils (degree 3 and 4 through Brodsky's table) was associated with a smaller Thoracic Perimeter resulted from a weaker respiratory musculature and a lesser thoracic expansibility and thus a lesser thoracic perimeter. The children with this diagnosis also present difficulties in the deglutition and ingestion of more solid foods which leads to a better acceptance of the pureed diet. Consequently, the inadequate diet results in less weight gain than the one which is expected for the age, thus contributing as one more factor for a lesser thoracic perimeter. The breath during sleep is irregular and is added to a deficient oxygenation, harming the release of the growth hormone as described in some works. We then conclude that the addition of all these factors influences a lesser thoracic perimeter in children with increase of the palatine tonsils volume.
BIBLIOGRAPHY 1. Zin W. Fisiologia do Sistema respiratório. In Bethem N. Pneumologia, São Paulo: Atheneu; 1995.39-53.
2. Shepherd B R. Fisioterapia em Pediatria, 3 edição editora Santos, São Paulo, 1995; 338-343.
3. Romaldine H. Fisiologia Respiratória.In Rozov T. Doenças Pulmonares em Pediatria-Diagnóstico e Tratamento, São Paulo: Atheneu; 1999. 19-31.
4. Deutsch E, Reilly J. Amigdalectomia e Adenoidectomia-Mudanças nas Indicações. In Sih T. Manual de Otorrinolaringologia Pediátrica do IAPO:1997.145-159.
5. Hungria H. Otorrinolaringologia. 8 edição Guanabara koogan Rj, 2000;167-170.
6. Di Francesco R. C. Crescimento e Desenvolvimento Craniofaciais Pós-Natais. A Influencia da Respiração. In Sborl Tratado de Otorrinolaringologia, São Paulo: Roca; 2003. 619- 625.
7. Saffer M. The Child that Breathes Through the Mouth. In Chinski A, Eavy R. II Manual Of Pediatric Otorhinolaryngology of IAPO, edição. Buenos Aires: Marino; 1999. p175-187.
8. Paradise J. L. Tonsillectomy and Adenoidectomy. In Chinski A, Eavy R. II Manual Of Pediatric Otorhinolaryngology of IAPO, edição. Buenos Aires: Marino; 1999. 129-134.
9. Brodsky L. Tonsillitis, tonsillectomy and adenoidectomy. In: Bailey, BJ, ed. Head and Neck Surgery-Otolaryngology, Philadelphia, Lippincott, 1993; 833-47.
10. Wandalsen NF. Rinite Alérgica. Pediat Moderna 1982; 17(4).
11. Perdigão, A B. Trabalhando com a Postura Corporal do Respirador Oral. In Krakauer L, Di Francesco R, Marchesan I. Respiração Oral, Pulso Editora; 2003.127-143.
12. Kendall F, Mc Creary, Provance P. Músculos - Provas e Funções. Editora Manole 4 Edição 1995; 324-330.
13. Ersoy B , Yuceturk AV, Taneli F, Uyanik BS. Changes in growth pattern, body composition and biochemical markers of growth after adenotonsilectomy in prepubertal children. Int. J. Pediatr. Otorhinolaryngol. 2005, 69(9):pp1175-81.
14. Selimoglu E, Selimoglu MA, Orbak Z. Does Aden tonsillectomy improve growth in children with obstructive adenotonsillar hypertrophy? J Int Med Res, 2003 Mar-Apr., 31(2) pp 84-87.
1. Specialization in Respiratory Physiotherapy (CRA Clinic Research Associated)
2. Doctor in Medicine by Universidade de São Paulo - University of São Paulo (Assistant Doctor at Hospital das Clínicas da Faculdade de Medicina USP.)
3. Doctor in Medicine by Faculdade de Medicina USP (Collaborating Professor of Otorhinolaryngology at Faculdade de Medicina USP)
4. Doctor in Pediatrics (Doctor of the Primary Immunodeficiency Clinic and Medical Researcher of the Medical Investigation Laboratory on Allergy and Immunology of the Dermatology Department, FMUSP)
Faculdade de Medicina USP
Institution: Faculty of Medicine - University of Sao Paulo (USP).
Mailing address: Melissa Guerato Pires - Rua Carlos Weber, 601 Apartment: 114 C - Lapa - Sao Paulo / SP - CEP: 05303-000 - Phone: (11) 3641-2941 -- Mobile: (11) 9215-4856 - Fax: (11) 3021-8892
This article was submitted in System Management Publications by R@IO on July 16, 2006. Cod. 138. Article accepted on April 13, 2007.