INTRODUCTIONForeign Bodies (FBs) are common occurrences in emergency department affecting both children and adults. The introduction of the FBs is usually voluntary in children and patients with mental disorders, and it occurs accidentally in adults. In accidental cases, the FBs are usually animated (i.e. living creatures) (1).
Symptoms may vary according to type, localization, complications of the FBs as well as the time they remain in the human body. When in the nasal cavities, the symptoms are clearer by starting with mucopurulent rhinorrhea and unilateral fetidness; epistaxis and unilateral nasal obstruction might also occur. (2)
When the FBs arise in the ears, patients' condition may vary from asymptomatic to ear pain, otorrhea, hypoacusis and otorrhagia (3, 4).
When the FBs are found in the oropharynx and hypopharynx (usually fish bones or food), symptoms are varied, thus these FBs cause great discomfort, pain, dysphagia and sialorrhea (1).
The presence of the FBs or their manipulation in order to be removed might seem a simple issue; however, there is a complication risk, by both their presence and removal attempt (5).
Improper manipulation of ear FBs might trouble their removal, which can cause laceration, bleeding and oedema of the external acoustic meatus, and further, a possible lesion of the tympanic membrane and ossicular chain (3).
In nasal FBs, electrical batteries, by their simple presence, might cause septal perforation, synechias and epistaxis (6).
The main complications of nasal FBs are epistaxis, asthma and bronchopulmonary infections (1).
Yet, the complications of FBs in the oropharynx and hypopharynx are retropharyngeal abscess, craniofacial celulitis, mediastinitis, aspiration pneumopathy diseases and migration to neighboring organs (1).
Due to all these complications, the removal of the FBs must be performed by trained and skilled professionals, as well as proper tools.
OBJECTIVEThe target of this study is to evaluate cases of FBs in the ear, nose and oropharynx according to gender, age, localization and origin of the FBs; to observe the types of complications when removing a FB and its relation to previous manipulation; also, to warn emergency doctors as for FB severity in the otorhinolaryngology area.
MATERIAL AND METHODA cross-sectional study performed from July 2004 to August 2006 by the Otorhinolaryngology Service of the Hospital e Maternidade Celso Pierro da Faculdade de Medicina - PUC/Campinas. It was submitted to and approved by the Research Ethics Committee under the protocol 094/07.
346 patients with FB in the nose, ears and oropharynx were evaluated. The medical report consisted of identification; age; localization and type of the FB; symptoms; the need of anesthesia procedure; previous manipulation by other type of professionals and complications of the FB removal.
Inclusion criteria:1 - Any patients, both adults and children, who were sent to the emergency department of our service in the city of Campinas, with or without FB symptoms;
2 - FB findings at the physical exam in ENT ambulatory visiting.
The removal procedure was performed by resident doctors of the ENT service under the supervision of assistants from the same service. The material used consisted of bayonet and Hartmann tweezers; Itard probe; curettes and wash; sometimes, sedation and withdrawing from the surgery room were needed. Vaseline was used in order to immobilize the animated FBs (insects) in the first place, then, followed by wash and aspiration. In the cases of myiasis, oral Invermectina was previously used (6mg), and then followed by nose washes and the larva removal, in cases of nasal myiasis.
RESULTS346 foreign bodies were removed; 130 from (37.3%) female patients and 216 (62.6%) from males (Chart 1).
Chart 1 - Distribution of patients with FB in otorhinolaryngology area, according to gender.
Regarding age, 88 patients (25.4%) were over 12 years old and 258 (74.5%) of them were 12 years old or younger (Chart 2).
Chart 2 - Distribution of patients with FB in otorhinolaryngology area, according to age.
Patients considered in the pediatric age were divided into:
- 0 to 3 years old: 96 cases - 28% of material
- 4 to 6 years old: 90 cases - 26% of material
- 7 to 12 years old: 72 cases - 21% of material
Regarding localization of the FB, 267 (77%) were found in the ears, 72 (21%) in the nasal fossae (including one case where the FB was found in the nasal fossa and in the nasopharynx at the same time) and 7 (2%) in the oropharynx (Chart 3).
Chart 3 - Localization of the FBs in otorhinolaryngology sites.
When relating FB age and localization (Chart 4) in 0-3-year-old children, the nasal fossa prevailed, affecting 54 cases (56.2%); ears in 40 cases (41.6%) and 2 cases (2.08%) affecting the oropharynx. In 4-to-6-year-old children, the FBs in the ears accounted for 77 cases (85.5%); 12 cases (13.3%) in the nasal fossa and 1 case in the oropharynx (1.11%). In 7-to-12-year-old children, FBs in the ears also prevailed, accounting for 69 cases (95.8%); 2 cases (2.7%) of FB in the nasal fossa and 1 case (1.3%) in the oropharynx.
Chart 4 - Distribution relation of age and FB localization
When foreign bodies were present in adults, 81 cases (92%) were in the ears; 4 cases were in the nasal fossa (4.5%) and 3 cases were in the oropharynx (3.4%).
Regarding FB origin, 295 (85.2%) cases were inanimate and 51 (14.7%) were animate; 50 of these were ear FB, and 1 was a nasal and nasopharyngeal FB. Regarding inanimate ear FB, seeds prevailed in 17.9%, followed by plastic objects (14.2%) and cottons (13.1%) (Chart 5).
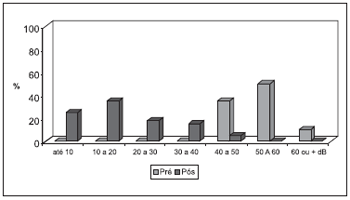
Chart 5 - Inanimate objects found in the ears
The most common FBs in the nasal fossae are seeds (26.3%) and foam (25%) (Chart 6).

Chart 6 - Inanimate objects found in the nasal fossae
Regarding symptoms, 215 patients (62.1%) presented no symptoms. Out of 131 patients who presented symptoms, 96 of them had FB in the ears (accounting for 35.9% of ear FB); 28 (38.8%) in the nasal fossa and 7 (100%) in the oropharynx (Chart 7).

Chart 7 - Distribution of FB localization regarding the presence or not of symptoms.
Ear pain (68.7% - 66 cases), tinnitus (21.8% - 21 cases), and hypoacusis and otorrhea (6.25% - 6 cases) were the symptoms reported from patients who presented ear FB.
In the 28 cases of nasal FB, the most common symptoms were: rhinorrhea (82.1% -23 cases); fetidness (35.7% -10 cases); nasal obstruction (7.1% -2 cases) and fever (3.5% -1 case).
Seven patients who had oropharyngeal FB reported discomfort in the throat and odynophagy. One patient reported excessive sialorrhea (14.2%), and another reported dysphagia (14.2%) and the third reported dyspnea (14.2%).
There had been previous manipulation in 147 cases (42.4%), and 29 of them (19.7%) presented complications; and 25 patients (12.5%) with no previous manipulation presented complications (Chart 8).
The most frequent previous manipulation attempts in ear FB were performed in 112 patients (76.1%); attempts in nasal fossa FB were performed in 34 patients (23.1%) and there was just one case of oropharyngeal FB (0.6%).
Regarding complications, 54 patients (15.6%) presented them at FB removal; 29 patients (53.7%) with ear FB presented laceration of the external acoustic meatus; 9 patients (16.6%) presented external acoustic meatus infection and 3 of them (5.5%) had tympanic membrane perforation. In nasal fossa FB, 8 cases (14.8%) had nose bleeding; 1 case (1.8%) had septal perforation; and in oropharyngeal FB, 1 case (1.8%) presented aspiration pneumonia.
Regarding the need of anesthesia, 13 patients (3.75%) were submitted to sedation or general anesthesia. Of these, 9 (69.5%) were younger than 12 years old; 2 adults (15.3%) were mentally retarded; 1 (7.6%) had rhinolith and 1 (7.6%) had extensive myiasis in the nasal fossa and nasopharynx.
Of the patients who were submitted to anesthesia procedure, 76.9% (10 cases) of them had ear FB; 15.3% (2 cases) had nasal and nasopharyngeal FB and 7.6% (1 case) presented hypophryngeal FB. Of those, 69.2% had previous manipulation history.
DISCUSSIONConcerning the gender of patients with FB, our study presented similar figures as others, in which males prevailed (5, 7, 8).
Most patients (75%) were in pediatric age (12 years or under). This finding agrees with Marques (8) who found 69% of occurrences of FB in patients aging 12 or under.
The ears are, in otorhinolaryngology terms, the main site for Foreign Bodies.
This study found 77% of ear FB, while others found an incidence of 48% and 38.27% (8, 7).
Bressler (4) states that ear FB is a common problem in emergency departments, its occurrence can vary from 1-to-219 patients up to 1-to-1792 ones.
BENTO (3) reports that 55% of the cases of ear FB occur in children not over 15 years.
Young children present a higher incidence rate of nasal FB regarding localization and age. This is interesting information displayed in Chart 4 and mentioned in other studies.
In a certain study (2) on 420 cases of nasal fossa FB, 91% affected children under 4 years.
Such a fact makes us look at an important detail: introducing FB in the nose can be totally unconscious for young children, which differs from the older ones who introduce FB voluntarily in the ear instead. However, as mentioned in this study and in Tiago's (7), the older the child the lesser the incidence of nasal FB.
Regarding the FB origin, most of them presented in this study were inanimate (85.2 %), both in the ears and nasal fossae. The more common ones are seeds (bean, corn, nuts); small objects, plastic items; cotton pieces (especially in the ears) and foam in the nasal fossa.
The literature (8) shows an agreement on the type of ear FB, seeds being the main one. However, in the same study, nasal FB prevails as plastic items, naphthalene and small jewels, which differs from our study.
Figueiredo (2), who only studies nasal FB, also reports similar results to ours, i.e. the predominance of foam, plastic items, beans and paper.
Concerning the FB origin, there were 5 cases of alkaline battery in nasal fossae, which represents otorhinolyngology emergency, by requiring an immediate removal (6), as the presence of this type of FB might cause expressive tissue lesions (9).
There was one case of oropharyngeal FB that was neither food nor fish bone; it was a plastic item that remained attached to the hypopharynx and was only identified on the 21st day of hospitalization, when an otorhinolaryngology evaluation was required.
Most patients with FB in this study did not present symptoms. Ikino et al (5) described that 35% of the ears and 66.6% of nasal FB were not suspected previously in other services due to the absence of symptoms.
In the literature (7), the most frequent symptom for oropharynx FB is odynophagy (90.91%) and unilateral rhinorrhea symptom for nasal FB (76.92%); this agrees with our study that also found odynophagy (100%) and unilateral rhinorrhea (82.1%) respectively.
That same study (7) referred hypoacusis as the main symptom for ear FB (28.07%), while in our study we found a great incidence of ear pain (68.7%).
Tiago (7) found 16.05% of previous manipulation on arrival at the ENT service. The complications by the FB presence or previous removal attempts were 16.05%.
In another study (5), involving children, the removal attempts of ear FB occurred in 60%; complications due to FB presence or removal attempts occurred in 22.5%. In nose FB, previous manipulation accounted for 52% with no complications.
In Marques' study (8), 58.9% of the FBs were manipulated either in other service or by other professionals. Bressler (4), who only studied ear FB, reported 53% of removal by non otorhinolaryngologist professionals.
We achieved a number of 42.4% of previous manipulation in this study, in which 19.7% of the cases had been previously manipulated and 12.5% had not. One should consider that complications regarding FB might be caused by several different factors; they are: origin, remaining time in the body and also previous manipulation. A likely explanation for the previous manipulation attempt in other services might be due to the fact that our hospital is tertiary level, which comprehends cases initially assisted by either basic health units or public hospitals that do not provide otorhinolaryngology service.
In our study, the main complication concerning ear FB was lacerations of the external acoustic meatus (53.7%), being similar to Bressler's study (4) that reports 29.5% of the same type of complication and to Ikino's (5) reporting 20% of it. In the studies (7 and 8) the main complication found was otitis externa (12.28% and 44.46% respectively); and in our study that percentage was 16.6%. In our study, bleeding was the main nasal complication found (14.8%), but it occurred in small amounts in just one case. There was a need of unilateral nose packing because of the rhinolith removal. The study (2) also refers epistaxis as the main complication (7.06%). In the studies (7 and 8), the main complication was rhinosinusitis, but epistaxes were mentioned from 7.69% to 37.93% respectively.
In our study, the need of sedation or general anesthesia was graded in 3.75%, which differs from the literature that refers from 8.6% to 30% (7).
CONCLUSIONThe conclusions of this study were:
1 - The FBs in the ears are very common in both adults and children;
2 - The smaller the children, the more care should be taken regarding FBs in the nasal fossa and oropharynx, where more severe complications occur, related to aspiration and pneumonias;
3 - Most FB is inanimate, which means, they can be avoided: foam, plastic pieces and seeds. Once they are within the reach of children, parents and teachers must be alert towards their behavior;
4 - The FBs in the oropharynx are extremely symptomatic;
5 - Previous manipulation by either non-trained professionals or use of improper tools can cause more complications when removing the foreign bodies;
6 - Early diagnosis also avoids complications when removing FBs.
REFERENCES 1. Meirelles RC: Corpo Estranho em Otorrinolaringologia. In Patrocínio, JA, Patrocínio, L G: Manual de Urgências em Otorrinolaringologia, 1a edição, Rio de Janeiro: Editora Revinter, 2004, pp 201-207.
2. Figueiredo RR, Azevedo AA, Kós AOA, Tomita S. Corpos estranhos de fossas nasais: descrição de tipos e complicações em 420 casos. Rev. Bras Otorrinolaringol 2006;72:13-23.
3. Bento RF: Corpos Estranhos de Orelha Externa. In: Bento RF et al: Condutas Práticas em Otologia, 1a edição, São Paulo: Fundação Otorrinolaringologia, 2002, pp 42-44. 4. Bressler K, Shelton C. Ear Foreign - Body Removal: A Review of 98 Consecutive case. Laryngoscope 1993;103:367-370.
5. Ikino, CMY, D" Antonio WEPA, Balbani APS, Sanchez TG, Butugan O. Análise dos atendimentos para retirada de corpos estranhos de ouvido e nariz em crianças. Rev. Bras Otorrinolaringol 1998;64:379-83.
6. Gomes C C, Sakano E, Melo R R G. Disco de bateria elétrica como corpo estranho de cavidades nasais. Aspectos peculiares. Rev. Bras Otorrinolaringol 1989;55:42-44.
7. Tiago RSL, Salgado DC, Côrrea JP, Pio MRB, Lambert EE. Corpo estranho de orelha, nariz e orofaringe: experiência de um hospital terciário. Rev. Bras Otorrinolaringol 2006;72:177-181.
8. Marques MPC, Sayuri MC, Nogueira MD, Nogueirol RB, Maestri VC. Tratamento dos corpos estranhos otorrinolaringológicos: um estudo prospectivo. Rev. Bras Otorrinolaringol 1998;64:42-7.
9. Gusmão, RG; Bueno M C; Murad, M P: Bateria Alcalina como Corpo Estranho de Ouvido: Relato de 3 casos. Rev. Bras Otorrinolaringol 1995;61:79-81.
1. Resident Doctor in the Otorhinolaryngology Service of the Hospital e Maternidade Celso Pierro - PUC/Campinas.
2. 6th year student of Medicine at Faculdade de Ciências Médicas - PUC/Campinas.
3. Titled teacher at the Faculdade de Ciências Médicas - PUC/Campinas.
Hospital e Maternidade Celso Pierro da Faculdade de Medicina da Pontifícia Universidade Católica de Campinas Otorhinolaryngology Service of the Hospital e Maternidade Celso Pierro - PUC/Campinas
Address: Av. John Boyd Dunlop, s/n, CEP: Jardim Ipaussurama Campinas - SP
Kátia Cristina Costa
Mail address:
R. Angela Signori Grigol, 643 Jardim Independência - Campinas - São Paulo - Cep: 13084-405 - Fax: (19) 3729 8518 - E-mail: k.cristinacosta@bol.com.br
This article was submitted to SGP (Sistema de Gestão de Publicações) of R@IO on November 17th, 2006 and approved on June 11th, 2007. Code # 193