INTRODUCTIONThe cholesteatoma of middle ear is one of the most fascinating topics and one of the greatest and most complex problems in otology, if it is studied and analyzed deeply in all its varied aspects.
Being relatively frequent in adults, it also occurs in children and may have serious consequences. As time goes by, it destroys middle ear, causing low audition or deafness in most affected patients and, occasionally, brings life risk.
Most otologic surgeons agree on the fact that cholesteatoma treatment is surgical. However, the kind of surgery varies considerably, and it is possible to find support in medical literature for almost all kinds of surgery.
There are different opinions concerning the selection of conservation technique of canal wall. Many doctors have been trying to perform intervention aiming at the reconstruction of the empty ear. In such process, three points are essential:
- perform an eardrum graft;
- reestablish a solid base for such graft;
- reconstruct the ossicle chain.
Such intervention has been used after the emptying of open tympanomastoidectomies, in which the tympanus cavity and the eardrum are partially or totally destroyed, in which just the stapes may exist, or the stape does not exist (or just the platen exists), or when the ossicle chain is not fixed in an irremovable sclerosis block.
The functional rehabilitation of the open tympanomastoidectomy cavity with allograft involves the anatomic rehabilitation of middle ear and of external auditory canal, which is essential for the functional result and, at the same time, allows patients to practice water sports.
At present, even when the tympanomastoidectomy is necessary, it will be followed by a further functional rehabilitation.
It has been many years that some otologists try to give solutions to the problem of open tympanomastoidectomy cavity1.
The use of tympanic-ossicle allograft has been contributing to the transformation of surgical prognosis2. Such technique brought the conditions of normal physiology of eardrum cavity, guaranteeing its aeration and drainage.
Total tympanic-ossicle allograft is considered the group of eardrum, malleus, incus and stapes. Different varieties of partial stapes may be described according to different techniques used.
As Marquet wrote, "homograft of complete tympanic-ossicle system seems to be the ideal solution for different problems posed by reconstructive surgery of middle ear"3.
The highest indication of total tympanic-ossicle allograft is in the functional rehabilitation of tympanic-mastoid cavities, but three conditions are necessary: two of them are common in all tympanoplasties - on one hand, the absence of any inflammation and/or infection and on the other hand, the functional state of Eustachian tube -, and the third condition is the situation of the tympanic-mastoidectomy cavities - the situation of the mucosa, which is frequently substituted by epidermis.
Such conditions are essential for a good functional result, preventing patients from recurrence of inflammations and infections and even from cholesteatoma.
Functional results presented by Marquet, reproduced by statistics of post-operative audiometric curves controlled by tympanometry may be considered excellent, next to 90%, higher than the ones obtained through other techniques4.
The total reconstruction of the tympanic-mastoidectomy cavity with tympanic-ossicle allograft offers a wide range of possibilities:
- it allows suspension and physiological movements of grafted ossicle chain5;
- it avoids false routes of embryonic epithelial migration6;
- it equally contributes to homeostasis of pressure in middle ear cavities7;
- it enables patients to practice water sports8.
There are several kinds of technical concepts for reconstruction of tympanic-mastoidectomy cavity9. The total reconstruction of posterior wall of the external auditory canal with a piece of autograft of fresh cortical bone or septum cartilage, together with partial or total tympanic-ossicle allograft, had our preference.
This study aims at showing the technique, the material used and the anatomic and functional results obtained with such technique.
MATERIAL AND METHODWe have selected 21 ears with dry open tympanic-mastoidectomy cavity for more than two years. 18 patients were adults and 3 were younger than 16 years old. The average age of patients operated with the described technique was 27.19 ± 13.99. All of them had already undergone previous surgery; some of them had been operated twice or three times, in order to solve inflammation.
All of them previously presented partial, total or subtotal tympanic perforation, and such perforation lasted from three to forty years.
We consider close technique (CT), in open tympanic-mastoidectomy, the reconstruction of the posterior wall of the external auditory canal, with cortical of mastoid or septum cartilage and closing of middle ear, with tympanic-ossicle allograft.
Reconstruction time was around 12 months after the first surgery.
We consider total perforation the total absence of tympanic membrane; partial perforation is considered the existence of part of tympanic membrane around the tympanic ring and sub-total perforation with just remains in pars flaccida region.
Surgical success meant no complications in the reconstructed tympano-mastoid cavity.
Patients of this research were operated between 1982 and 1988 at Hospital São Paulo (university hospital of UNIFESP). Some cases of our private clinic have also been included.
The surgeries have been performed by the author of this investigation or by the members of his working team under his supervision.
The surgeries were distributed in the following way:
- 18 (adult) ears underwent reconstruction of open tympanic-mastoidectomy with tympanic-ossicle allograft and reconstruction of the posterior wall of the external auditory canal, with cortical of mastoid.
- 3 (young) ears underwent reconstruction of open tympanic-mastoidectomy with tympanic-ossicle allograft and reconstruction of the posterior wall of the external auditory canal, with septum cartilage.
- total ears: 21
We just admitted patients who presented no other problem except such anatomical-functional ear problem. Consequently, the ones who presented general chronic diseases (diabetes, infections, ect) and neurossensorial hearing loss were excluded from this investigation.
The tympanic-ossicle allograft was obtained in the Decease Verification Service of Hospital São Paulo, emphasizing patient's identification in order to avoid any transmittable disease. All phases of material preparation for implant were performed within the highest standard of asepsis and with removal of allograft in aseptic environment.
We have followed the removal methods, conservations means and ways of placing the allograft previously described by AQUINO10.
In the reconstruction of tympanic-mastoidectomy cavities, we provided post-operative follow-up of around 4 years and a half (minimum of six months and maximum of five years and six months.
Patients were seen right after the surgery whenever possible and up to twice a week for at least four months. After such period care was less frequent, but we tried to do them at least twice a year. In each visit, we did ear analysis and, when necessary, aspiration under microscope. Audiological routine with vocal discrimination was performed every 60 days, for 4 months. After that, audiometric and CT exams were done less frequently. We had special attention with operated ear, after surgical cicatrisation. All patients previously agreed on having the proposed surgical technique with allograft use.
Fixation of tympanic-ossicle set was performed in the beginning of our surgeries with butyl-2-cyanoacrylate in some cases and, further, with fibrin glue or not.
We evaluated the surgical results of this investigation under the following aspects:
a) Anatomic results:
- In terms of tympanic membrane aspect (surgical success), evaluated with otoscope and surgical microscope;
- In terms of surgical failure: perforation and perforation with intermittent otorrhea; interruption of ossicle chain; reabsorption of reconstruction material.
b) Functional result:
It is evident that it is among valid anatomic results that good functional results are observed. However, with some exceptions, a small dry perforation of the new eardrum may occur with substantial auditory result, a result which may be assisted by a simple myringoplasty reconstruction.
Functional auditory results were evaluated 4 months or more after the operation, through the difference between bone way and air way before and after the surgery, calculated over the average frequencies in 500Hz-1 KHz-2 KHz before and after the surgery.
We considered auditory improvement the average variation after the surgery from 10 to 20 dB for better; unchanged, when there was no auditory gain, and changed between 10 to 20 dB to worse.
We used statistical data to evaluate anatomic and functional results the T paired test, mean, standard deviation, for samples gathered before and after the surgery.
In all cases the rejection level of nullity hypothesis was between 0.05 and 5% (α
< 0.05) and significant values were marked with an asterisk.
We showed the technique of mastoid cortical bone removal to reconstruct the external auditory canal with some modifications designed by us (11, 12, 13, 14, 15) according to pictures 1 and 2.
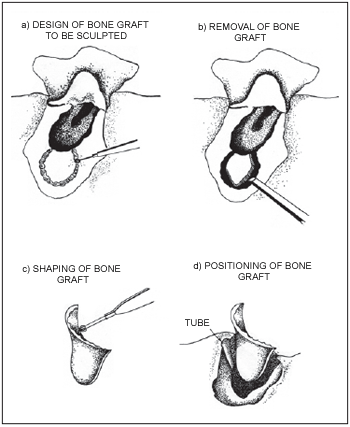
Picture 1. Reconstruction of canal wall with cortical bone of mastoid. Marquet Technique (1970).
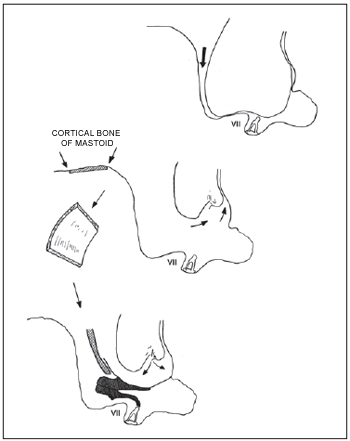
Picture 2. Rehabilitation of radical mastoidectomy cavity with tympanic-ossicle allograft
Operation Technique itself (closed technique)
We may classify the several techniques designed in two groups: open and closed techniques; both of them may imply an immediate functional reconstruction of middle ear. In the closed technique, surgical periods were performed like MARQUET stated9.
1) Incision is done with #15 surgical knives, circumscribed to the pavilion, 1 cm behind the pavilion. With the help of an electrocute, a skin flap is done. The anterior fold is represented by the retro auricular sulks and skin elevation is done together with it. The incision of the periosteum circumscribed within the skin incision is also done with electrocautery. The periosteum-muscle flap, in which the anterior fold is located in the posterior border of the open tympanic-mastoidectomy cavity, must be very wide; its traction in the end of intervention avoids a canal ptosis. The elevation of such flap is prepared with grinder, right in the posterior border of the tympanic-mastoidectomy cavity. After that, a careful hemostasia is performed and a retractor is placed without strong retraction, in order to avoid the rupture of periosteum flap. The elevation is done through microscope. Such surgical period is essential, and the graft of the posterior wall must be covered with skin, over all surfaces within the canal without continuity solution.
2) Cleaning of open tympanic-mastoid cavity - it is an essential surgical period in which the middle ear must be of the epithelium which covers the cavity:
- the tympanomastoidectomy cavity may be carefully polished with the help of a diamond drill;
- at the level of tympanic cavity, epithelium is carefully removed, as well as the one at window level (oval and round windows) and at Fallopian tube level, without drilling. The tympanic remains and the malleus are removed;
- at the level of the tube orifice, where fissures usually occur, careful cleaning must be performed.
If we find a cholesteatoma which invades the open tympanic-mastoid cavity, there is no contra-indication to practice the closed technique.
The matrix of the cholesteatoma will be carefully elevated.
- The tympanic-mastoid cavity and the attic are polished with diamond drill. At the level of the tympanic cavity, in the Fallopian tube, in the region of oval and round window at the level of eardrum sinus (cavity which is located between promontory and pyramidal eminence), and equally in the region of facial access, area where cholesteatoma recurred, the ablation of cholestatoma matrix must be as prudent as possible;
The cholesteatoma matrix must be carefully liberated, in which it is necessary to avoid facial nerve harm, at the level of its third position. The Fallopian tube may suffer suture opening at this level.
3) The removal of bone piece - using of fragment of external cortical of temporal bone - is processed like MARQUET technique13. The removal is performed behind the tympanomastoidectomy cavity.
In the bone, the shape of a small trapezium is designed and with the help of a cutting drill with four pads, such part of bone is removed with osteotomus and malleus; the bone dust gathered during the drilling will be further used to "cement" the graft of the posterior wall; the lateral sinus and the dura-mater may be cleared during such maneuver. It is enough to close the cleared part with bone wax in such cases.
The piece of temporal cortical removed will be worked with drill so that it will reproduce the canal format (format of a small trapezium). The big side corresponds to the bone part of the canal, and the small side corresponds to the external part of the attic.
Such piece of bone is carefully polished with diamond drill, under continuous irrigation, and will be sculpted according to the cavity which needs to be redone.
Two sulci are marked in the cavity: a superior one in the level of the anterior part of the junction between the attic and the atrium at the level of facial wall. Such sulci must allow the connection between the non-parallel sides of the trapezium. The bone fragment placed in saline solution will be ready for its positioning.
4) Positioning of tympanic-ossicle allograft - the manipulation of the chain must be careful. The grafted eardrum must not be traumatized, in order to reduce post-surgical perforation.
The selection of the tympanic-ossicle system depends on different surgical setbacks:
a) The stape is movable and intact: An allograft block which comprehends tympanus-malleus-incus is introduced. The tympanic border of the grafted eardrum in introduced in the receptor sulcus. The lenticular apophasis of the grafted incus may be exactly the same as the incus head of the receptor. Immunebilogical glue may be used to form such articulation(15).
b) the stapes is intact, but blocked by tympanosclerosis: in such case, allograft is performed (tympanus-malleus-incus), which allows middle ear to close if it is dry. If no infection sign appears, one year after the surgery, a platinectomy is performed with positioning in the place of prosthesis in piston or an inverted stapes over venous interposition3.
c) Accidental opening of oval wall: a system which is the same as the previous one is placed over venous intervention. Post-operative wide antibiotic therapy and therapeutic orientation are performed in order to avoid labyrinthization 3.
5) Placing of posterior wall - once the ossicle chain is placed, the piece of cortical bone is placed, shaped in the dimensions of the cavity which will be reconstructed. The dust of the recovered bone of both drilling periods will be used to cement the autograft of the posterior wall.
The chain should never touch the eardrum cavities after the positioning of posterior wall. The canal skin should cover the bone autograft, in order to avoid expulsion and decay. If the necessary skin is not big enough, a fragment of temporal aponeurosis is used, duplicating the external face of the autograft of the posterior wall. With the help of a surgical knife, skin is incised so that it is folded, in a way that the bone graft is totally recovered by the epithelium.
Intervention finished with suture under tension of the periosteum-muscle flap, and with a drain in the antral cavity which will provide an aeration way for the eardrum cavity.
Finally, skin is sutured in two plans. The drain will be removed 48 hours after the surgery.
6) Final wound healing - we call attention for special care which is necessary for the final wound healing of the allograft. A piece of silicon lamina (Silastic) folded like a cigarette is introduced in the external auditory canal, next to the eardrum, and pieces of synthetic foam soaked with ointment associated with antibiotics and corticosteroid placed inside with tweezers. Such wound healing will be there for at least seven days and the foam can be exchanged or removed, provided that the "silastic cigarette" is not touched.
Such care is taken under microscope and aspiration. Any skin maceration must be avoided and the wound healing may be removed so that the allograft is watched. Such local treatment is also associated to oral antibiotic covering, in addition to auricular drops.
RESULTSWe showed our surgical statistics between 1982 and 1988 (Table 1)
We evaluated the surgical results of this investigation under the following aspects:
- Anatomic Results:a) In terms of tympanic membrane aspect (surgical success), evaluated with otoscope and surgical microscope; (Table 2)
b) In terms of surgical failure: perforation and perforation with intermittent otorrhea; interruption of ossicle chain; reabsorption of reconstruction material. (Table 3, Chart 1)
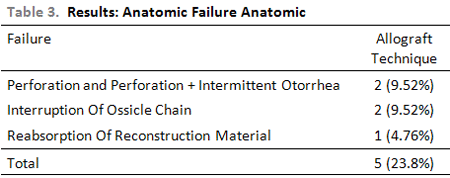
Chart 1. Anatomic surgical failure. Perf: Perforation I: interruption
There was no residual or recurrent cholesteatoma, or retraction bag in this study.
c) We did post-operative evaluation through CT scan of reconstructed cavity 12 months after the surgery.
- Functional result:Functional auditory results were evaluated 4 months or more after the operation and calculated over the average frequencies in the conservation areas obtained in audiometries performed before and after the surgery.
The average result (in absolute values) of airways of open cavities was around 48.9 dB, and bone way around 17.6 dB, and the data corresponding to conversation area was used as base (Table 4, Chart 2).
Concerning the auditory global functional result (Chart 4), out of the patients who had closing of tympanic membrane with allograft technique, 14 (66.6%) presented improved hearing level, 4 (19%) remained with the same hearing level and 3 (14.4%) presented worse hearing level.
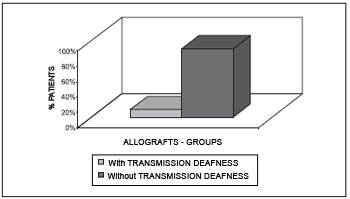
Chart 3. Functional surgical failure.
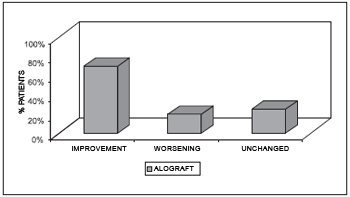
Chart 4. Global auditory functional result.
The audiometric results are presented on Charts 2, 3, 4 and 5.
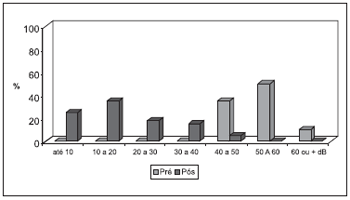
Chart 5. Auditory functional result at conservation area (allograft).
The percentage variation before and after the surgery (D %), concerning audiometric result, is presented on Table 4 and Chart 5.
DISCUSSIONBetween 1982 and 1988 we tried to rigorously select patients carrying patients with open tympanomastoidectomy cavities which would be reconstructed, taking into account the following criteria:
- severely dry ear;
- ear with excellent cochlear reserve;
- how possible it would be to perform patients post-operative follow-up;
- how possible it would be to convince patients to accept recovery in case of surgery failure;
- evaluation of the other ear.
The rigid criteria to select patients have been limited the quantity of interventions, once such patients usually come from distant parts of Brazil and from low social classes, what makes many of them not come back to our clinic, or come back months or years later.
The criteria which have been guiding us to choose a solution to preserve the temporal bone removed from the donator were created by MARQUET4. We used as routine 4% formol solution and pH 5.6, in which such temporal bones will be immersed from 10 to 15 days in 4º C refrigerator, before being dissected. Such permanence period is necessary so that such bactericide solution sterilizes the material, and to slightly harden the eardrum and to fix the incudomalear and incudostapedic articulations.
The chemical sterilization of this material, aiming at eliminating microorganisms which may transmit diseases to receptors, was very efficient, once culture for fungi and bacteria were always negative, even after one year in storage.
The objective of the sterilization of tympanic-ossicle allograft is to not transmit to the receptor microorganisms from the donator or from manipulation during preparation. It is ideal that the allograft which will substitute the tympanic membrane be free from microorganisms, mostly because nowadays it is essential to eliminate contamination risks with HIV and HBV.
Precaution of the use of formol solution in recommended concentrations and in the rigorous selection of our transplanted patients, overcomes, with large security margin, international recommendations adopted for inactivation of AIDS virus16.
Immunological reactions related to ossicle-tympanic allografts have been object of many scientific articles17, 18.
Despite all inconvenience, we wanted to try the technique created by MARQUET19, which consists of closing tympanic cavity with a complete tympanic-ossicle allograft, of reestablishing a columelar effect through the procedure which seems to be more suitable to present conditions and to reconstruction of external wall of the attic, with fragment of cortical of mastoid or septum cartilage (closed technique). Careful restauration of the wall of the external auditory canal (EAC), as well as the reduction of cavity size, are recommended for a good anatomic and functional result.
Studies performed by ARS20 showed that there is no correlation between the size of the allograft, age and sex of the patient. Eardrum size is particularly important when allograft is used in reconstructive surgery of middle ear. According to MARQUET4, it is essential that allograft have perfectly similar sizes.
Tympanic-ossicle allograft, since its removal until its surgical positioning, is, from our point of view, one more option which meets our otosurgical needs in the reconstruction of open tympanic-mastoid cavity and also in reconstruction of partial or total perforations of eardrum. Its removal requires certain surgical training, but it can be stored for one year at most, which provides dozens of surgical reconstructions, provided that there is an allograft "bank". The standard used allowed us to guide our attention to one part of the study of anatomic and functional results of such surgery, relating them to several degrees of pathological states of middle ear.
The reconstruction of open tympanic-mastoid cavity provides patient with hearing improvement, as well as with sea and pool baths, depending on the technique used8.
We used two stages in our surgeries: first, removal of disease and second, at least six months later, tympanic and ossicle plastic reconstruction.
We used the tympanic-ossicle allograft technique in 21 patients. Just one patient suffered filling of open cavity with bone and bone dust, and the canal wall with mastoid cortical (once it was a very big mastoid). Its stability was guaranteed thanks to the tube made in the anterior and posterior part, at canal level, in order to place its extremities. In order to improve such stability, we put bone dust in the tube (fibrin glue15 may also be used in its extremities).
In the reconstruction of the tympanic-mastoid cavity with allograft, we found stapes in 8 cases (38%), and it was absent in 13 cases (62%). Platine was movable in all cases, 21 (100%).
In terms of graft quality, we obtained 76.2% of anatomic success.
WAYOFF et al(21), when analyzing results by 233 otosurgeons from Canada, Europe and Africa, provided a more trustworthy standard to evaluate our results. They show that 82.6% of surgeons had anatomic-tympanic success in more than 75% of patients, when the whole evaluation of all techniques and materials used for eardrum reconstruction was considered. Some otosurgeons pointed anatomic success in more than 90% of patients, when they used temporal aponeurosis or autogenous tragal perichondrium. Concerning functional improvement, the percentages presented for both global tissue sample and individual temporal aponeurosis were in 60 to 70% of cases.
The comparison of our anatomical global results - 76.2% of success in closing partial or total perforations of tympanic membrane, with the percentages mentioned in the study by WAYOFF et al(21), register tympanic-ossicle allograft as a good option to solve such processes.
Concerning anatomic surgical failure, tympanic perforation, either associated or not to intermittent otorrhea, was one of the main reasons of our failures.
The incidence of otorrhea in literature is variable: MARQUET(22) found 5.5% in radical surgeries; PALVA, KARMA, PALVA 10.0%(23); BROWN 25.0% in adults and 33.0% in children(24); VAN BAARCE & HUYGREEN 10.0 to 15.0% in modified mastoidectomies 20.0 a 25.0% in classic mastoidectomies(25), and PECH et al 9.5% in classical mastoidectomies26).
There are many factors which contribute to post-operative perforation of a new eardrum: They include:
- the state of middle ear mucosa;
- severe hemorrhage during surgery, which may provide a proper environment to microorganism development;
- infection of high airways which would cause obstruction of Eustachian tube, thus blocking ventilation of the cavity with consequent middle otitis;
- defect of surgical technique when placing tympanic graft;
- recurrence of cholesteatoma with consequent perforation, most of the time.
In this study, most perforation percentage and perforation associated to intermittent otorrhea in surgeries were: 9.5% for tympanic-ossicle allograft technique and 4% in closed technique.
According to PORTMANN et al(14), in allograft cases, perforations appear usually two months after the surgery, appearing in 8.5% of their results. They are central and do not harm functional prognosis when they are small and when do not follow interruption of ossicle chain, which is frequent. According to MARQUET22 they may be originated from technical failure of allograft positioning, but they may also be related to an epithelization delay; it is necessary to point out the canal skin, in which vitality influences epithelization speed. Certain perforations may be closed with the help of aponeurosis, through further myringoplasty. In case of surgical failure, we are forced to remove the allograft and put another one. Perforations which are discovered later in otorrhea situation have a very different meaning. They show persistence of an infection and inflammation, sometimes related to cholesteatoma.
ROULLEAU et al(27) observed that perforations are more frequent in allograft (10,0%) than they are in temporal apneurosis (5,0%), what explains the fact that inflammations are frequently found in the level of open tympanic-mastoid cavities, and that allografts are more vulnerable than autografts.
CHARACHON, ROUX, EYRAUD(28) and CHARACHON, GRATACAP, ELBAZE(29), registered 8% of perforations in patients operated under closed technique.
After three-year follow-up, PECH et al(26) observed 13% of perforations.
We also had interruption of ossicle chain in our study, as a result of connection loss between receptor stapes and the grafted block.
The interruption of ossicle chain occurred in allograft technique in two cases (9.52%) through destruction of the long branch of the grafted incus. That was observed in cases which Histoacryl was used. It varied since 5.0% on study by MARQUET(22), to 20.0% on study by PORTMANN et al(14) and almost reached 10.0% on study by ROULLEAU et al(27). Authors admit that such fact must be related to secondary displacement through ossicle wear, through fixation of ossicle chain in the attic, or through platinum fixation.
Among the patients of this investigation, there was one case (4.76%) of reabsorption of the reconstruction material of the posterior wall of external auditory canal, when closed technique was performed. On MARQUET reconstructive surgeries, there was 4.0% of reabsorption. The case of out study started with cartilage decay and further reabsorption with otorrhea. Such complication became worse due to Histoacryl use as mean to fixate the cartilaginous autograft. The corticle bone, which is less flexible, but easier to be taken from mastoid cortical for reconstruction of posterior wall of external auditory canal has been used, in most of our surgeries, shaped to the drill and placed according to JUNICHI et al(30) technique.
Bone reconstruction is not indicated when it is not certain that total extirpation of lesion will occur or when there are severe surrounding complications.
Causes of functional surgical failure were observed in patients who underwent second intervention.
Transmission hypoacusia worsening was observed by MARQUET(22) in 6.0% of patients and by PORTMANN et al(14) and JUNICH et al (30) in 5.0%. . We had two cases (9.5%) in allograft technique.
Radical intervention usually worsens the auditory deficit before the surgery. It is common that deafness sequel be between 40 and 60 dB. Such deficit increases, also through chronic infections and degenerative labyrinth process.
We did not have severe complications in our study, any chophouses case (0%) and any labyrinth accidental opening (0%). Post-operative chophouses were observed five times by PORTMANN et al(14), once by WAYOFF et al(21), twice by ROULLEAU et al(27). They are related to platinum trauma in inflammation.
Auditory functional global results of this investigation point out 66.6% of auditory improvement for allograft (gain of 10dB to a 20dB in frequencies averages 500Hz, 1000Hz and 2000Hz); if pre- and post- operative phases are compared in partial, total and sub-total perforations, such results may be considered satisfactory. Results could be even better for such technique if there were more stapes present.
We believe we can improve our results by better selecting our patients who present tympanicmastoid cavities, improving techniques of canal reconstruction, maybe using new bio-materials in the future, such as ceramic (Hidroxiapatite) which has been widely used in Europe and performing functional intervention, which allows the absence of a retractions bag or residual cholesteatoma. Recently, (December 2006 to February 2007) we had the opportunity to review five out of such reconstructions which had stable audition and bone wall and dry tympanic-mastoid cavity without cholesteatoma recurrence and/or retraction bag.
Despite of extensive explanations over allograft use on reconstruction of open tympanic-mastoid cavities as well as of international recommendations adopted concerning HIV and HBV virus, our patients have been hesitating to undergo such kind of surgery, even after knowing about practice and results of such technique. However, we consider the allograft technique (closed technique) a choice method for the surgery of middle ear cholesteatoma.
CONCLUSIONSTo perform the closed technique it is necessary to create, manage and use a temporal bone bank, which are essential to tympanic-ossicle allograft surgery.
We presented how difficult it is to reconstruct the external auditory canal with the cortical bone of mastoid. We have currently abandoned cartilage use, due to its flexibility, inconstancy and mainly its reabsorption.
Long-term results show that the technique of reconstruction of the posterior wall of external auditory canal, together with transplant of tympanic-ossicle allograft, allows the reconstruction of open tympanic-mastoid cavities, which can even provide almost anatomically normal ear and good functional result.
This study is motivating and makes us think that this kind of intervention deserves being always considered by the ones who perform otologic surgery.
REFERENCES1. Aboulkehr P, Demaldent JE, Prache H. Essais de reabilitation fonctionelle des evidements totaux. Ann. Otolaryngol. (Paris), 1970, 87(suppl1/2):35-48.
2. Marquet JFE. Technique inedité de myringoplastie par homogreffe du tympan. Acta otorhinolaryngol. (Belg.) 1967, 21:127-32,
3. Marquet JFE. Les homogreffes tympano-ossiculaires. Paris, Arnette, 1978, 126p
4. Marquet JFE. Homografts in middle ear surgery: ten years of experience. Trans. Am. Acad. Ophtalmol. Otolaryngol., 1975, 80:30-6,
5. Ars B, Decraemer W, Ars-Piret N. Timpano-ossicular allograft: morphology and physiology. The American journal of Otology, 1987, vol 8(2):148-54.
6. Ars B. Organogenesis of the middle ear structures, The Journal of Laryngology and Otology, 1989, 103:16-21.
7. Ars B, & Ars-Piret N. Middle ear pressure balance under normal conditions. Specific role of the middle ear structures, Acta Belgica ORL,1994, 4:48-50.
8. Ekval L. Total middle ear reconstruction. Acta ORL (Stockh),1973, 75:279-81.
9. Marquet JFE. Homografts in tympanoplasty and other forms of middle ear surgery. In: Ballantyne, J.C., ed. Operative surgery. 3 ed. London, Butterworths, 1976, p.100-15.
10. Aquino JEP. Banco de osso temporal: da criação a utilização de um banco; etapas indispensáveis para a realização dos homoenxertos tímpano-ossiculares. São Paulo, 1989. (Tese-Mestrado-Escola Paulista de Medicina)
11. Wullstein HL. Technique et resultats de la tympanoplastie. Ann. Otolaryngol. (Paris), 1955, 72:764-81.
12. Portmann M, Guerrier Y, Guillein G, Lenoir J, Riemens V. Évidements petromastoidiens avec temps tympanoplastique. In: Traité de technique chirurgicale ORL et cervico-faciale. Paris, Masson, 1975, v.1, p.208-10
13. Marquet JFE. Les homograffes du tympan en chirurgie reconstructive de l'oreille moyenne. J. Fr. Otorhinolarynngol., 1970, 18:369-72.
14. Portmann M, Poncet E, Roulleau P, Lacher G. Les homogreffes tympano-ossiculaires. Paris, Arnette, 1978, 205p.
15. Seelich T. Tissucol (immuno, vienna): biochemistry and methods of application. J. Head Neck Pathol., 1982, 3:65-9.
16. Brasil, Ministério da Saúde. Secretaria Nacional de Programas Especiais da Saúde. Divisão de Dermatologia sanitária. Centro de referência para Aids-SIDA/AIDS: recomendações para hospitais, ambulatórios médicos, odontológicos e laboratórios. Brasília, Centro de Documentação do Ministério da Saúde, 1986, 16p. (normas e manuais técnicos, 34).
17. França GV. Transplantes de órgãos e tecidos. In: Direito médico, 3.ed. São Paulo, Byk Procieux, 1982, v.18, p257-9.
18. Veldman JE, Kuijpers W, Overbasch MC. Experimental models for reconstructive ear surgery: immunobiology, autoimmunity and transplantation in otolaryngology. Clin. Otolaryngology, 1978, 3:293-7.
19. Marquet JFE. Les homogreffes du tympan en chirugie reconstructive de l oreille moyenne. J. Fr. ORL, 1970, 18:369-72.
20. Ars B. La partic tympanale de l'os temporale. Cahiers D'ORL, 1983, 18:439-523.
21. Wayoff M, Chobaut JC, Deguine C, Desauty A, Dubreuil C, Fraisse B, Magnan J, Romanet P, Roulleau P, Simon C, Uziel A. Les greffes du tympan, Paris, Arnette, 1990, 273p.
22. Marquet JFE. Twelve years experience with homograft tympanoplasty Otolaryngol. Clin. North Am., 1977, 10:581-93.
23. Palva T, Karma P, Palva A. Cholesteatoma surgery: canal wall down and mastoid obliteration. In: Mc Cabe BF, Sadé J, Abramson M. Cholesteatoma, Birmingham, Aesculapius, 1977, p.363-7, Alabama.
24. Brown JS. A ten years statistical follow-up 1142 consecutive cases of cholesteatoma: the closed versus the open technique. Laryngoscope, 1982, 92:390-96.
25. Van Baarce PW, & Huygren PL. Findings in surgery for chronics otitis media: retrospective data analysis of 2255 cases followed for two years. Clin. Otolaryngol.,1983, 8:151-8.
26. Pech A, Thomassin JM, Canoni M, Zanaret M, Scavennec, C, Triglia JM. Cholesteatome de l'oreille: experience d'une attitude therapeutique écletique. Ann Otolaryngol (Paris), 1985, 102:575-80.
27. Roulleau P, François M, Receveur M, Candeau P. Rehabilitation des cavités d'évidement: bilan de 5 années. Ann Otolaryngol. (Paris), 1984, 101:53-61.
28. Charachon R, Roux O, Eyraud S. Le cholesteatome de l'oreille moyenne: choix des technique et resultats chez l'adulte et chez l enfant. Ann. Otolaryngol. (Paris), 1980, 97 (suppl. ½):65-78 29. Charachon R, Gratacap B, Elbaze D. Rehabilitation des évidements par la tympanoplastie in technique ouverte avec comblemente músculo-périosté. J. Fr. ORL, 1985, 34(suppl.9):421-28.
30. Junichi B, Watanabe N, Mogi G. Reconstruction of the external auditory canal after canal down tympanomastoidectomy for chronic otitis media with cholesteatoma: long term observation of hearing and canal expansion. Cholesteatoma and mastoid surgery, 1992, p.679- 82. Proceedings of IV Intern. Conference. Niigata, Japan, Kugler Publications, Amsterdam / New York.
1. Doctorate - UNIFESP - and Head professor II on Otorhinolaryngology at Faculdade de Medicina Santo Amaro - UNISA - SP.
2. Doctor's degree on Otorhinolaryngology by Faculdade de Medicina USP and doctor in charge of the Otology sector of the Hospital Beneficência Portuguesa - SP.
3. Senior Medicine student at Faculdade de Medicina de Nova Iguaçú - RJ.
This study was done at EPM-UNIFESP. Prof. Dr. Nelson Álvares Cruz's clinic.
Mail address:
Alameda Ribeirão Preto, 410, apto. 1106 - Bela Vista
Cep. 01331-000, São Paulo - SP.
Tel. (011) 3251-2096. E.mail: clinicaorlsp@uol.com.br
This article was submitted at SGP (Sistema de Gestão de Publicações) of R@IO on January 7, 2007. Code #206 and was approved on June 3, 2007.