INTRODUCTION The technique of aspiratory puncture with fine needle (APFN) was initially used to investigate injuries in salivary glands around 1920(1,2) with improvement and development between 1950 and 1960 and popularization in the seventies(3,4). It is a minimally invasive diagnostic examination and of low cost(5,6) used in the differentiation between neoplasia and non-neoplasia injuries and being able to differentiate between a benign or malign neoplasia injury(7).
The APFN presents considerable advantages in the diagnosis in relation to the radiological findings and of physic examination (8,9) as well as in relation the surgical conventional biopsies(10) being that this procedure not always can be discharged(11).
Hemorrhages, hematomas, neoplasia dissemination and injury of the face nerve are some possible complications(12,13).
Being injuries of the parotid region a diagnostic challenge and considering the APFN an excellent procedure for the diagnosis of the tumoral injuries of the parotid region, we investigate its capacity in promoting a correct diagnosis of these injuries comparing the cytological and histological findings of submitted patients with the parotidectomia with previous puncture.
MATERIAL AND METHOD Retrospective analysis of the data of 156 patients submitted to the resection of injuries in parotid region in our hospital between January 2001 and January 2005. 58 patients with injury in topography of parotid gland were selected, who submitted to the pre-surgical APFN with positive cytological results.
All the patients had been guided and had assented in terms of the accomplishment of the APFN and the surgical treatment. The APFN was carried through by an only pathologist doctor of our hospital, with experience in the method, who also prepared the material and interpreted the findings. The puncture was carried through with needle 0.70 X 30/22G 1 ¼ with cytoaspirator connected to the syringe of 20 ml and guided by ultrasonography (US). A smear of the material obtained was done in 6 microscopy blades, half of which were imbibed in 96% alcohol and the remains sent to laboratory dry. The material was stained by the method of Papanicolau or eventually by the method of Giemsa.
The patients were submitted to surgical treatment that varied according to the necessity of each case being carried through since partial parotidectomies with preservation of the face nerve until total parotidectomies. Twenty and eight patients were male and thirty female with average age varying between 61.2 ± 18.5 years and 69.3 ± 15.6 years, respectively. The findings of the cytology were divided in two groups: neoplasia and non-neoplasia injuries. The injuries of the first group had been classified in adenolymphoma, pleomorphic adenoma, mucoepidermoid carcinoma and squamous cell carcinoma. The second group injuries were classified in sialoadenitis, cyst and lymphoid hyperplasia. These findings were compared with the histological findings of the material in paraffin and the agreement among them evaluated by calculating the sensitivity, specificity, positive predictive value, negative predictive value and accuracy. These same calculations were carried through in the independent evaluation of the diagnosis of adenolymphoma and pleomorphic adenoma. Study registered in the committee of ethics of the institution (protocol 049/06).
RESULTSThe cytological findings of the APFN were divided in neoplasia and non-neoplasia injuries (Table 1). It had positive correlation between the cytological and histological results in 44 cases (75.86%) and negative correlation in 14 cases (24.14%) (Table 2).
Considering the capacity of the APFN in diagnosing neoplasia, independent of the histological type, it had a positive correlation in 49 cases (84,48%) and a negative correlation in 9 cases (15,52%) (Table 3). Sensitivity (s) was of 82.4%, specificity (e) of 100%, positive predictive value (PPV) of 100%, negative predictive value (NPV) of 43.8% and accuracy of 84.4% (Table 4).


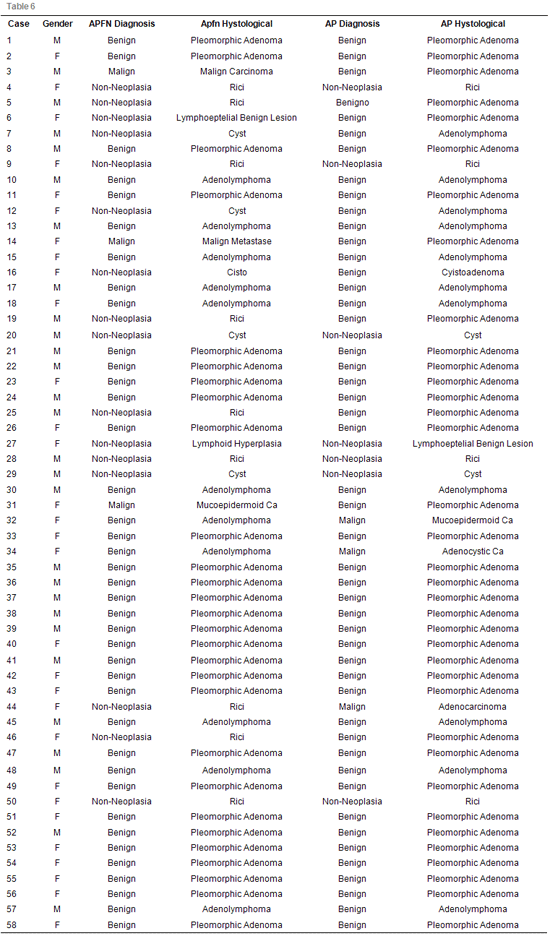
The relation of the divergent diagnostic between cytology and histology is shown in Table 5. In relation to these divergent diagnostic in 9 punctures classified as non-neoplasia the histological result showed to be neoplasia and benign injuries. In the 5 punctures with diagnosis of neoplasia, being 2 malignant and 3 benign, the histology showed that the 2 benign neoplasias in the cytology were malignant in the histology and the 3 malignant neoplasias of the cytology were benign in the histology. The classifications of all the injuries with their respective cytological and histological diagnostics are shown in Table 6.

All the punctures with cytology of pleomorfic adenoma (28) had confirmation in the histology although in others 8 cases with varied punctures (goal CEC, sialoadenitis, lymphoid hyperplasia, mucoepidermoid carcinoma) the histology revealed to be pleomorfic adenoma. The calculations for this diagnosis showed a sensitivity of 77.7%, specificity of 100%, PPV of 100%, NPV of 61.1% and accuracy of 86.2% (Table 7).
In relation to the diagnosis adenolymphoma, in 2 cases the histology did not confirm the diagnosis that were compatible with malignant neoplasia being 1 cystic adenoid and 1 mucoepidermoid. In 1 case with puncture of cyst the histology showed to be about one adenolymphoma. We have thus a sensitivity of 86.2%, specificity of 95.8%, PPV of 81.8%, NVP of 97.8% and accuracy of 94.8% (Table 8).
Hematomas, infection, implantation of neoplasia cells, damages to the face nerve or other complications in the accomplishment of the APFN were not observed.
DISCUSSION Our study showed that in 44 cases (75.86%) there was a positive correlation between the cytological findings and the histological results found after the surgery of patients with injuries in parotid gland. When we consider the capacity of the APFN in diagnosing neoplasia injuries we observe a little bigger positive correlation, occurring in 49 cases (84.48%) and with a accuracy of 84.4%, concordant with literature(7,14).
Among the 9 cases (15.51%) in which there wasn't a positive correlation between the cytology and the histology we observe that the histological diagnosis was of malignant neoplasia in all the cases. We know that there is a great difficulty in the diagnosis of malignant neoplasias with a trend to underestimating the findings thus classifying the finding as benign neoplasia(15,16) being what occurred in relation to our disagreeing diagnostic where the cytology showed a diagnosis of adenolymphoma and the histology confirmed a diagnosis of mucoepidermoid carcinoma in a case and a carcinoma cystic adenoid in another one.
In relation to the disagreeing diagnostics with puncture of malignant neoplasia it was about a mucoepidermoid carcinoma with histology of pleomorphic adenoma and two metastases of squamous cell carcinoma with histology of pleomorphic adenoma demonstrating habitual diagnostic confusion in relation to the pleomorphic adenoma and the malign injuries(8,17,18,19).
We do not observe false positives in the correlation of the cytological findings and histological as for the neoplasia diagnosis thus justifying the high value of the specificity and agreeing to the literature that presents a variation between 0% and 6% (8,15,20,21,22).
In relation to the false negatives we observe that in 5 injuries classified as sialoadenitis they were in fact about 4 benign neoplasia injuries (pleomorphic adenoma) and a malignant neoplasia injury (adenocarcinoma). We know that for the diagnosis of a neoplasia injury the identification of distinct cellular types is necessary and that the malignity diagnosis is based on the finding of signals as invasion and destruction of fabric to salivar normal, anaplasia, pleomorphism and atypical mitosis(14). In these cases, we believe that the material has been collected in inadequate place or specifically in the malignity case the material has been insufficient for a correct diagnosis. In relation to the cytology of lymphoid hyperplasia with histology of pleomorphic adenoma we believe that even with the orientation of the ultrasonography the punctured place did not correspond to the place of the injury. The cystic injuries present a great percentage of false diagnostics(3,6,19), being that in 3 of our cases the histológico examination revealed to be about benign neoplasia injuries: 2 adenolymphomas and 1 cystoadenoma.
All the cytological diagnostisis of pleomorphic adenoma were confirmed in the histology leading to a specificity of 100% and sensitivity of 77.7% while sensitivity for the diagnosis of adenolymphoma was of 86.2% what goes against the findings of Atula and col that shows a bigger sensitivity in relation to the diagnosis of pleomorphic adenoma between the benign neoplasia injuries. Perhaps this difference can be justified by our reduced sample.
Even with an accuracy above 80% in the differentiation between the neoplasia and non-neoplasia injuries, we come across with the false negative results that can consequently lead to an incorrect diagnosis and to an improper treatment(14,20). We thus realize the importance of the medical follow-up for the patients whose puncture result presented non-neoplasia injury and that were not submitted to the surgery. We point out that the decision of surgical approach in the cases of puncture with non-neoplasic diagnosisis related to the clinical suspicion of the surgeon in being a neoplasia injury, based on clinical history, physical examination and radiological examinations which also increases the sensitivity of the APFN(23,24). The surgical treatment exactly with the negative APFN is considered many times the best therapeutic option(11).
We know that our casuistry is small, mainly in relation to the diagnostic of malignant neoplasias, but we consider the study opportune for the classification and better understanding of the data in our environment.
The APFN is a safe diagnostic procedure and of easy accomplishment that causes little discomfort to the patient with improvement of its accuracy when guided by US(25,26). The main objective of the cytological diagnosis is the differentiation between neoplasia and non-neoplasia injuries and if possible the differentiation of the neoplasia injuries in benign or malignant, being that the histological definition of the tumor will be carried through, in the majority of the times, in definitive in the histological study. However, the main point to be considered is the capacity of the examination in supplying to a cytological trustworthy pre-operatory diagnosis that is of great value for the therapeutical planning mainly in patients with important comorbities in which the surgical risk is high. Therefore, the APFN is a widely used examination for the diagnosis and surgical planning of the neoplasias of salivary glands allowing to one better interaction between the doctor and the patient, providing a discussion on the therapeutical options and promoting a more conscientious decision on the considered treatment. However, all professionals that use the APFN in practical clinic must be aware of the limitations of the method.
CONCLUSIONThe aspiratory puncture with fine needle of injuries in parotid gland reveals to be an adequate method of evaluation and therapeutical planning providing to better conditions for the discussion of the case between the doctor and his/her patient.
We thank the clinic of Pathological Anatomy and Dr. Karla N. Dantas for the contribution with the service of Otorhinolaryngology and ENT Surgery.
BIBLIOGRAPHY1. Martin HE, Ellis EB. Biopsy by needle puncture and aspiration. Ann Surg 1930; 62:169-181.
2. Dudgeon LS, Patrick CV. A new method for rapid microscopical diagnosis of tumors. Br J Surg 1927; 15:250-261.
3. Mavec P, Eneroth CM, Franzen S, Moberger G, Zajicek J.Aspiration biopsy of salivary gland tumors. Acta Otolaryngol (Stockh) 1964; 58:471-484.
4. Bonneau H, Sommer D. L'orientation du diagnostic des tumeurs salivaires par la ponction à l'aiguille fine. Pathol Biol 1959; 7:786-791.
5. Frable MA, Frable WJ. Fine needle aspiration biopsy of salivary glands. Laryngoscope 1991; 101(3):245-9.
6. Layfield LJ, Glasgow BJ. Diagnosis of salivary gland tumors by fine needle aspiration cytology: a review of clinical utility and pitfalls. Diag Cytopathol 1991; 7(3):267-72
7. Atula T, Grenman R, Laippala P, Klemi P. Fine-needle aspiration biopsy in the diagnosis of parotid gland lesions: evaluation of 438 biopsies. Diagnostic Cytopathology 1996; 15:185-190.
8. Zurrida S, Alasio L, Tradati N, Bartoli C, Pilotti S. Fineneedle aspiration of parotid masses. Cancer 1993; 72:2306- 2311.
9. Owen E E R T C, Banerjee A K, Prichard A J N, Kark A E. Role of fine-needle aspiration cytology and computed tomography in the diagnosis of parotid swellings. Br J Surg 1989; 76:1273-1274.
10. Biaforetti G, Giannoni M, Ranieri A, Leocata P. Fine needle aspiration cytologic diagnosis of swellings in the parotid and submandibular regions. Cytologic-histologic correlations in 49 cases. Minerva Stomatol 1996; 45(1-2):9-16
11. Batsakis J G, Sueige N, el Nagar A K. Fine-needle aspiration of salivary glands:its utility and tissue effects. Ann Otol Rhinol Laryngol 1992; 101:185-188.
12. Cramer h, Layfield L, Lampe H. Fine-needle aspiration of salivary glands: its utility and tissue effects. Ann Otol Rhinol Laryngol 1993; 102(6):483-5.
13. Deans G T, Briggs K, Spence R A. An audit of surgery of the parotid gland. Ann R Coll Surg Engl. 1995;77: 188-92
14. Costas A, Castro P, Martin-Granizo R, Monje F, Marron C, Amigo A. Fine-needle aspiration biopsy for lesions of salivary glands. B J Oral Maxillofacial Sur 2000; 38:539-542.
15. Weinberg M S, Rosberg WW, Meurer W T, Robbins K T. Fine-needle aspiration of parotid gland lesions. Head Neck 1992; 14:483-7
16. Ariyan S. Cancer of the head and neck. St Louis. MI: CV Mosby, 1987:603-605
17. Heller KS, Dubner S, Chess Q. Value of fine needle aspiration biopsy of salivary gland masses in clinical decision make. Am J Surg 1992; 164:667-670.
18. Kumar N, Kapila k, Verna K. Fine needle aspiration cytology of mucoepidermoid carcinoma: a diagnostic problem. Acta Cytol 1991; 7:267-272.
19. Macleod C B, Frable W J. Fine needle aspiration biopsy of salivary gland: problem cases. Diag Cytopathol 1993; 9:216-225.
20. Cristallini E G, Ascani S, Farabi R, Liberati F, Bolis G. Fine needle aspiration biopsy of salivary gland, 1985-1995. Acta Cytologica 1997; 41:1421-1425.
21. Qizilbash A H, Siamos J, Young J E M, Archibald S D. Fine needle aspiration biopsy cytology of major salivary glands. Acta Cytol. 1985; 29:503-512.
22. O'Dwyer P, Farrar W B, James A G. Needle aspiration biopsy of major salivary gland tumors. Cancer 1986; 57:554-557.
23. Van der Brekel M W M, Stel H V, Castelijns J A, Snow G B. Lymph node staging in patients with clinically negative neck examinations by ultrasound and ultrasound-guided aspiration cytology. Am J Surg 1991; 162:362-6.
24. Boccato P, Altavilla G, Blandamura S. Fine needle aspiration biopsy of salivary gland lesions. A reappraisal of pitfalls and problems. Acta Cytol 1998; 42:888-98.
25. Sack M, Weber R, Weintein G. Image guided fine needle aspiration biopsy of the head and neck Arch Otolaryngol Head Neck Surg 1998; 124:155-1161.
26. Malinsky R, Dall'Igna D, Smith M, da Costa S S. Punção aspirativa por agulha fina em tumores cervicais. Rev Bras Otorrinolaringologia 2002; 68:394-398.
1. Specialist on Otorrhinolaryngology and ENT Surgery; PhD student on Otorrhinolaryngology at Faculdade de Medicina da Universidade de São Paulo (Assitant Medical Doctor of the Otorrhinolaryngology and ENT Surgery Clinic at Hospital do Servidor Público Estadual de São Paulo)
2. Medical Residence (Otorrhinolaryngology and ENT Surgery Clinic at Hospital do Servidor Público Estadual de São Paulo)
3. PhD (In charge of the ENT Surgery Sector of the Otorrhinolaryngology and ENT Surgery Clinic at Hospital do Servidor Público Estadual de São Paulo)
Hospital do Servidor Público Estadual de São Paulo (Public Civil Servant São Paulo State Hospital) - Serviço de Otorrinolaringologia e Cirurgia de Cabeça e Pescoço (ENT Surgery and Otorrhinolaryngology Clinic)
Rogerio Borghi Buhler
Rua Aliança Liberal, 1015 - Ap 101 - Alto da Lapa - São Paulo/SP - CEP: 05088000. Fone/Fax: 5088 8406 - E-mail: rbbuhler@uol.com.br
This article was submitted to SGP (Publishing Management System) of R@io on June 14, 2007 and approved on August 5, 2007 at 11:54:44.