INTRODUCTIONAdvanced endonasal approaches (AEA) for treating lesions of skull base have been quickly developed (1). The main factors for such development are: better understanding of the endoscopic anatomy of skull base, proper tools production and the development of vascularized flaps for endoscopic reconstruction of skull base after such approaches (2).
Besides proper exposition and lesion resection, the endoscopic reconstruction of skull base defects is essential to achieve a good outcome. The targets of endonasal reconstruction and the targets of reconstruction after craniofacial approaches are the same, i.e. isolation of cranial cavity in order to prevent intracranial infections, liquoric fistula and and Pneumocephalus (3). The extension and localization of residual defect; previous endonasal surgery history or radiotherapy; age and patient's health condition as well as surgery team experience are important factor which might influence when choosing the reconstruction approach (4,5).
Endoscopic reconstruction of small fistula can be performed with graft of different types of tissues such as fat, fascia lata, medium turbinate mucosa, among others, presenting high level of success (6). Due to the expansion of endoscopic access to greater lesions on the skull base, the resulting fistula becomes massive to be reconstructed only with grafts. In this manner, the endoscopic reconstruction of such approaches has become a challenge for professionals. The rate of liquoric fistula in the post-operative period of advanced endonasal approach was high when using only grafts for reconstruction.
The use of a posterior pedicle nasoseptal flaps has been recently described for endoscopic reconstruction of the skull base, Hadad-Bassagasteguy flap (3). Since then, fistula rate on post-operative period of endoscopic approach to skull base was considerably reduced and has become similar to cranial-facial approaches rate. Special attention has been given to reconstruction with pedicle flaps and, only in the beginning of this year, two new flaps which can be used were described. The present study aims to review the present knowledge state concerning endoscopic reconstructive techniques for skull base after AEA. Two endoscopic reconstruction techniques are described, in which posterior nasal-septal flap and inferior turbinate posterior flap are used.
SURGERY APPROACHES
Nasal-septal posterior flapThis technique was described in 2006 by HADAD-BASSAGASTEGuy and consists of the use of a septal-nasal flap of mucoperiosteum and mucoperichondrium based on the posterior septal artery that is the posterior branch of the sphenopalatine artery (3).
Initially a vasoconstriction of the nasal cavity with oxymetazoline 0.05% is performed and the nasal septum is infiltrated with 0.5% to 1% Lidocaine with adrenalin 1/100,000 to 1/200.000. Usually the right medium concha is removed so that the skull base approach is performed, which makes the ipsilateral visibility of vascular pedicle and the rise of the septal flap easy. The flap is drawn according to the size and the form of the expected defect, however it is better to overestimate the size and, later, to remove the excesses of the flap if necessary. Two parallel incisions are performed in the septal-nasal mucosa through right nasal fossa. The first incision (inferior) must be parallelly made to the nasal fossa floor from posterior to anterior between septum and the floor. The second incision (superior) must be parallelly carried through to the first incision respecting 1 to 2 cm of distance of the nasal fossa ceiling for the preservation of the olfactory neuroepithelium. The two horizontal incisions must previously be joined by a vertical incision. These incisions can be modified in accordance with the specific area to be reconstructed. The two incisions are posteriorly extended in direction to rostrum sphenoidale. The inferior incision is continued with a vertical incision in the posterior free edge of nasal septum and, after that, laterally in the superior edge of the choana in a level which is a little below the sphenoid sinus floor. The superior incision follows with an incision which is immediately inferior to the sphenoid sinus ostium in direction to the sidewall of the nose. In this way, a narrow posterior pedicle is drawn containing the posterior septal artery. The rise of the flap of mucoperichondrium and mucoperiosteum is initiated anteriorly with a Cottle elevator or another similar instrument. The elevation of the sphenoid anterior wall flap is carried through with the posterior-lateral preservation of vascular pedicle. Multiple variations are possible in terms of the size and form of the flap. In the case of bigger defects, the inferior incision can be extended laterally in the nasal fossa floor, or bilateral flaps can be confectioned (Figure 1). Once it is elevated from the septum, the flap can be placed in nasopharynx until the surgical phase of approach and removal of the tumor have been concluded. In these endoscopic approaches to the skull base, the posterior portion of nasal septum is removed after the confection of the flap. During the surgery one must be careful with the bone removal in the lateral region to the pterygoid canal, since there can be injury of vascular pedicle of the flap in this region. According literature the average area of this flap is approximately 25 cm2 (7).
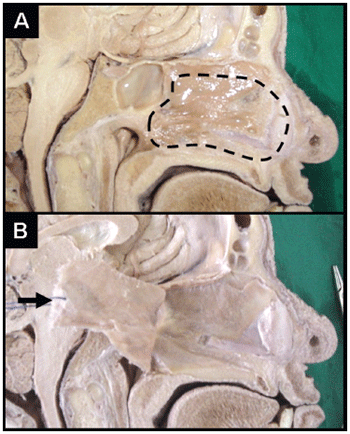
Figure 1. Nasal-septal posterior flap (sagittal incision, corpse dissection). (a) In prominence, septal area to be elevated for the confection of the flap. (b) Demonstration of the flap after the elevation (arrow). Attention: The visibility of flap pedicle in the images is not possible.
The reconstruction with the use of multiple layers is in general the most accepted one. A collagen matrix is placed in the subdural space (in lay). After that, one fascia or free fat graft is located on the dura-máter (on lay). The fat is preferred in the cases in which the obliteration of spaces such as in the defects of clivus, for example, is necessary. The nasal-posterior flap is, then, placed on the dura or the fat. Fibrin glue is used to help in the stabilization of the flap in the proper position. A Foley catheter (number 12 or 14), in general, is insufflated with saline solution inside the nasal cavity to perform a compression of the flap on the dural defect. The insufflation must be monitored under endoscopic visibility, since the hyper-insufflation can result into compression of intra-craniaal structures, harm the flap vascular pedicle, or dislocate the tissues used for the reconstruction. The probe must be kept for 4 to 7 days depending on the difficulty of the reconstruction and the liquoric risk on fistula. Splints of silicon are used to recover and to protect the naked remaining portion of nasal septum, being left there for 10 to 14 days.
Inferior turbinate posterior flapThis flap was described in July 2007 by Fortes-Carrau. The pedicle of this flap is based on the artery of inferior turbinate that is the terminal branch of the lateral nasal artery which is branch of the sphenoplatine artery (8).
Initially a vasoconstriction of the nasal cavity is made with 0.05% oxymetazoline and nasal septum is infiltrated with 0.5% to 1% lidocaine with adrenalin 1/100,000 to 1/200.000. After the accomplishment of the approach endoscopic and exeresis of the injury of skull base, the flap is confectioned as much as possible in the same side of the defect. Bilateral flaps of inferior turbinate can be made, in case they are necessary. Initially inferior turbinate is placed in the middle to display the meatus surface of inferior turbinate and to allow the visibility of the mucosa of the inferior meatus. The flap can be elevated according to the size of the defect in the skull base. However, is preferable to elevate the entire inferior turbinate to assure a complete covering of the defect.
Initially, the sphenopalatine artery is identified in the sphenopalatine foramen following it distally until finding the lateral nasal artery. The vascular pedicle of the flap is based on the artery of inferior turbinate that is branch of the lateral nasal artery. Under endoscopic visibility, two parallel incisions are made following the sagittal plan of inferior turbinate. The superior incision must immediately be made above inferior turbinate (maxillary sinus fontanel) and the inferior incision must be made in the caudal edge of inferior turbinate. A vertical anterior incision is carried through in the head of turbinate to join the two parallel incisions previously described. These incisions can be made with endonasal shears or, preferentially, with a tip of electrocautery. After that, the mucoperiosteum is elevated initially by the anterior aspect of turbinate. A variable amount of bone can be elevated together with the mucoperiosteum. Care must be taken to prevent the injury of vascular pedicle, since the artery enters the inferior turbinate about 1 to 1.5 cm anteriorly to the posterior extremity of turbinate, in its superior and lateral aspect. Special attention must be given to the lateral nasal artery, since the injury of this artery will harm the viability of the flap. The lateral nasal artery goes down vertically on the ascending process of the palatal bone. Its passage is anterior to the posterior wall of the maxillary sinus, consequently, care must be taken during the posterior extension of the maxillary antrostomy to maxillary in the attempt of localize the sphenoplatine artery, for example. Once it is completely elevated, the flap is located to cover the defect of the skull base (Figure 2). The approach area of the posterior flap of inferior turbinate is about 4.97 cm
2 (9).
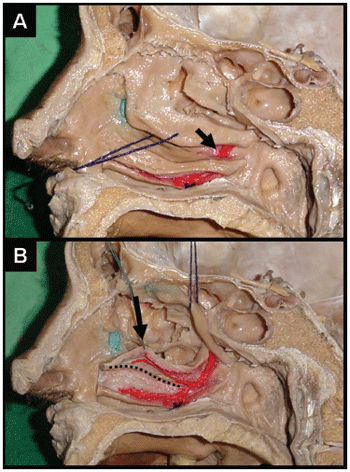
Figure 2. Inferior turbinate posterior flap (sagittal incision, corpse dissection). (a) After the vascular pedicle dissection the lateral nasal artery can be noticed entering in inferior turbinate (arrow). Please observe that the incision in the caudal edge of the turbinate has already been carried through. (b) The medial face of inferior turbinate will serve for the flap and is struck (arrow). Please observe the branch for inferior turbinater of the lateral nasal artery that is the base of flap nutrition. The hatched line shows where the superior incision of the flap must be carried through.
The flap can be applied directly over the dura-mater or naked bone, or can be used re-covering fat graft. It is mandatory, however, that the flap is in direct contact with edges of the defect and that all non-vascularized tissue present between the flap and edges of the defect is removed. Ibrine glue is used to help in the stabilization of the flap in the adequate position. A Foley catheter (number 12 or 14), in general, is insufflated with saline solution inside of the nasal cavity to exert a compression of the flap on the dural defect. The insufflation must be monitored under endoscopic visibility, since the hyper-insufflation can result in compression of intra-cranial structures, harm the vascular pedicle of the flap, or dislocate the tissues used for the reconstruction. The probe must be kept for 4 to 7 days depending on the difficulty of the reconstruction and on liquoric fistula risk. Splints of silicon are used to re-cover and to protect the sidewall of the naked nose, being left for 10 to 14 days.
DISCUSSIONSmall defects in the skull base are repaired successfully through a variety of techniques (6,10). Resultant defects of advanced endoscopic approaches (AEA) to the skull base present a series of challenges that increase the liquoric risk of fistula in the postoperative period (11). Despite the success of approximately 95% in the endoscopic treatment of traumatic liquoric fístula, the risk of fistula in the postoperative period of AEA to the skull base was of about 20 to 30% with the use of grafts and collagen matrix (11). Rates considered unacceptable for these approaches (8).
The advantages of the use of flaps for the reconstruction of the skull base after skull-face traditional approaches are well established. They promote a complete and fast cicatrization, speed up the postoperative recovery and prevent liquoric fistula and ascending meningitis (8). These advantages are important especially in the cases of great defects and patients that had been submitted to daily post-operative radiotherapy.
Based on the concept of the use of flaps for the reconstruction of the defects of the skull base, the nasal-septal posterior flap (HADAD-BASSAGASTEGUY) was developed. With the use of this flap the fistula rate in the postoperative AEA period presented a significant reduction being compared with the fistula rate of the traditional cranial-facial approaches(3).
The posterior nasal-septal flap is versatile, presents a good area of surface and a good arc of rotation (7). The formation of new mucosa on the donator area occurs in some weeks, and no case of previous septal perforation has been reported. However, some disadvantages of this flap can be observed: it must be elevated before the surgeon has the real dimension of the defect in the skull base and it cannot be used in patients who were submitted to posterior septectomy or ample sphenoidoctomies. These procedures interrupt the sanguine flow for the flap, making its use impracticable (3, 8). In these cases, the inferior turbinate posterior flap can be used, which is based on the artery of the inferior turbinate, which is branch of the lateral nasal artery that, in turn, is branch of sphenopalatine artery (8). This flap presents good arc of rotation that reaches most of the ventral-caudal defects of the skull base and is elevated after the complete removal of the injury of the skull base. However, the area of surface of this flap is not so ample as the one of the posterior nasoseptal flap. According to the literature, the average area of the inferior turbinate posterior flap is about 4.97 cm
2 (9), while the area of the posterior nasoseptal flap is approximately 25 cm2 (7). Inferior turbinate bilateral flap can be used in the cases of defects which are bigger than the surface of a flap.
Another disadvantage of the inferior turbinate posterior flap is the formation of crusts on the turbinate donator area. The formation of new mucosa on the donator area occurs in about 3 or 4 weeks. Patients with previous turbinectomy or atrophic rhinitis can present an insufficient area of flap surface. These cases are considered a relative contra-indication for this type of flap.
Recently, a new technique of use of the flap of temporal-parietal fascia for the endoscopic reconstruction of the skull base has been described. This flap is already well-established for the reconstruction after traditional skull-face approaches and is based on the superficial temporal artery. FORTS et al [2007] described this new technique for the transposition of this flap for the interior of the nasal cavity so that this can after be used in endoscopic AEA reconstruction. Through the confection of a tunnel temporal-infratemporal and an endonasal transpterigoid approach, the transposition of the flap for the interior of the nasal cavity is possible. The endonasal transpterigoid approach is carried through through the removal of the posterior wall of the maxillary sinus, dissection of pterigopalatine fossa and partial removal of the medial and lateral pterigoids processes. These maneuvers are carried through with intention to open a bone window so that the flap can pass from the temporal region, infrasecular fossa, pterigopalatina fossa and nasal cavity. The passage of the flap by soft tissues is opened in the use of percutaneous dilatators of tracheostomy. This flap presents a bigger morbidity when compared to the inferior turbinate flap and the nasoseptal flap. However it must be considered in cases in which the accomplishment of the two last flaps is not possible (12)
CONCLUSIONSThe defects in the skull after advanced endonasal approaches can be reconstructed with pedicle flaps. These flaps must be considered mainly for the reconstruction of great defects. Initial studies have demonstrated that the use of flaps is associated with a lesser liquoric fistula rate when compared to the use of free grafts. The nasal-septal posterior flap of Hadad-Bassagasteguy seems to be the first option of endoscopic reconstruction with flaps. However, in cases of posterior septectomy or any another condition that makes its use impracticable, the inferior turbinate posterior flap can be an excellent option.
REFERENCES1. Kassam A, Carrau RL, Snyderman CH, Gardner P, Mintz A. Evolution of reconstructive techniques following endoscopic expanded endonasal approaches. Neurosurg Focus 2005, 19(1):E8.
2. Nameki H, Kato T, Nameki I, Ajimi Y. Selective reconstructive options for the anterior skull base. Int J Clin Oncol 2005, 10:223-28.
3. Hadad G, Bassagasteguy L, Carrau RL, Mataza JC, Kassam A, Snyderman CH, Mintz A. A novel reconstructive technique after endoscopic expanded endonasal approaches: vascular pedicle nasoseptal flap. Laryngoscope 2006, 116:1882-86.
4. Carrau RL, Snyderman CH, Kassam AB. The management of CSF leaks in patients at risk for high-pressure hydrocephalus. Laryngoscope 2005, 115:205-12.
5. Goel A, Muzumdar DP. Recontruction of the sellar floor using vascularized pedicle mucosal flap. Br J Neurosurg 2003, 17(6):553-55.
6. Hegazy HM, Carrau RL, Snyderman CH, Kassam A, Zweig J. Transnasal endoscopic repair of cerebrospinal fluid rhinorrhea: a meta-analysis. Laryngoscope 2000, 110:1166-72.
7. Pinheiro-Neto CD, Prevedello DM, Carrau RL, Snyderman CH, Mintz A, Gardner P, Kassam A.Improving the Design of the Pedicle Nasoseptal Flap for Skull Base Reconstruction: A Radioanatomic Study. Laryngoscope 2007, Jun 27; [Epub ahead of print].
8. Fortes FS, Carrau RL, Snyderman CH, Prevedello D, Vescan A, Mintz A, Gardner P, Kassam AB.The Posterior Pedicle Inferior Turbinate Flap: A New Vascularized Flap for Skull Base Reconstruction. Laryngoscope 2007, Jun 27; [Epub ahead of print].
9. Murakami CS, Kriet D, Ierokomos A. Nasal reconstruction using the inferior turbinate mucosal flap. Arch Facial Plast Surg 1999, 1:97-00.
10. Zweig JL, Carrau RL, Celin SE, Schaitkin BM, Pollice PA, Snyderman CH, Kassam A, Hegazy H.Endoscopic repair of cerebrospinal fluid leaks to the sinonasal tract: predictors of success. Otolaryngol Head Neck Surg 2000, 123(3):195-01.
11. Snyderman CH, Kassam AB, Carrau R, Mintz A. Endoscopic Reconstruction of Cranial Base Defects following Endonasal Skull Base Surgery. Skull Base 2007, 17(1):73-8.
12. Fortes FS, Carrau RL, Snyderman CH, Kassam A, Prevedello D, Vescan A, Mintz A, Gardner P.Transpterygoid transposition of a temporoparietal fascia flap: a new method for skull base reconstruction after endoscopic expanded endonasal approaches. Laryngoscope 2007, 117(6):970-6.
1 Otorhinolaryngologist. Medical.
2 Head of the Department of Otolaryngology at University Hospital of the Federal University of Ceara. Professor of Otorhinolaryngology of the Federal University of
Ceara.
Institution: Federal University of Ceara.
Prof. Sebastiao Pinheiro Diógenes
Address correspondence to: Federal University of Ceara Discipline of Otolaryngology - Rua Alexandre Baraúna, 949 - Rodolfo Teófilo CEP 60430-160 - Fortress / EC - Brazil - Fax: (85) 3262-7297 - Email: sediogenes@yahoo.com
This article was submitted in System Management Publications by R@IO in August 1, 2007. Cod. 291. Article accepted on September 21, 2007.