INTRODUCTIONProblems from vestibular diseases are responsible for about 50% of body balance disorders (8), which is one of the most frequent complaints from patients. In this way, we can understand the concern of evaluating labyrinth function through different tests, with the purpose of identifying possible vestibular lesions responsible for such disorder.
Only some patients who suffer from dizziness do not need a quantity vestibular evaluation. A well-performed clinical history is able to provide important quality data, which can route diagnosis and a follow-up of the patients (5). According to American Academy of Neurology Technology Assessment, caloric tests are still a proper technique. It is well accepted and useful in detecting vestibular disorders, especially on unilateral involvement (1). Once decreasing pendular rotatory test is considered a gold standard method when reporting bilateral vestibular loss (6).
The tests evaluate the vestibulo-ocular reflex (VOR), which originates from the semicircular canal. Therefore, although VOR is fundamental for the body angular displacement, the vestibulospinal reflex (VSR) performs an essential role on posture maintenance and, only VOR evaluation become insufficient to observe vestibular function as a whole. Another important fact is that visual and somatosensory information, as well as the correct sensorial integration from brainstem take part on the body balance maintenance. This makes clear the importance of a diagnostic method that evaluates such information in a individual way.
Dynamic Computerized Posturography (DCP) complements the classical tests for vestibular involvement diagnosis which were redundant when investigating VOR (3). DCP is useful to check dizziness as a complementary exam for those patients who present complaints related to body balance which are not diagnosed by the conventional test. Its clinical importance is to diagnose the presence of body disorder and, then, if that is a result from a sensorial integration or afference to an inefficient motor response or even a combination of both. When DCP is compared to other vestibular tests, it provides diagnosis data in about 40% of the patients who present electronystagmography in normal condition (2). That happens as DCP evaluates vestibulospinal pathway which is not analyzed by the conventional tests. On the other hand, even patients who present DCP under normal conditions can present electronystagmography alterations. Therefore, DCP does not replace conventional vestibular tests, but it complements their findings and it is recommended for specific situations in which investigations of VSR and sensorial analysis of balance disorder are important.
What is a DCP?DCP is a computerized system which allows us to isolate and quantify vestibular, visual and somatosensory information, as well as its sensorial integration on body balance maintenance. DCP perform two types of test: Sensory Organization Test (SOT), which tell us about sensorial organization and Motor Control Test (MCT), which allow us to evaluate the intensity and coordination of motor response to the stimuli received on orthostatic posture (3).
The equipment consists of a surface of reference where patient remains standing up. This is composed by pressure sensors, which will be activated due to patient´s weigh´s displacement over their sole of the foot in response to body displacement. The surface of reference is surrounded by a movable visual field that goes through anterior-posterior displacement, changing visual information (Picture 1).
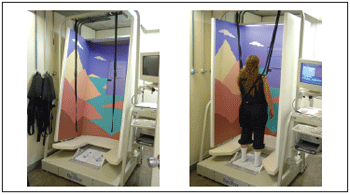
Picture 1. Dynamic Computerized Posturography
The used models to evaluate the components of sensorial and motor integration are:
- Quantifying visual, vestibular and somatosensory information.
- Quantifying mechanisms of central integration which select the best way to use received information.
- Quantifying responses to different sensorial stimuli.
- Quantifying motor response resulting from received stimuli.
SOT is the only available test that provides quantity information regards the three systems which give information on body balance. This step of the exam involves six different situations/conditions, which lead patients to different sensorial information making them use different strategies to body balance maintenance (Picture 2).
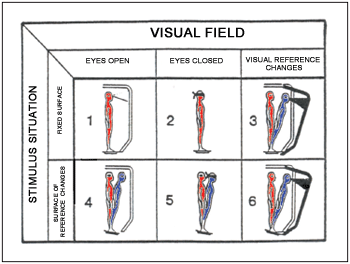
Picture 2. Different conditions of possible sensorial stimulus on DCP.
Condition 1: patient is placed standing, feet apart over sensors of the surface of reference;
Condition 2: same position with eyes closed;
Condition 3: patient keeps eyes open but visual field suffers anterior-posterior displacement;
Conditions 4, 5 and 6: steps 1, 2 and 3 are repeated respectively, but surface of reference changes at see-saw-like movements.
MCT measures involuntary movements that patients present in response to sudden anterior or posterior movements of the plaque of reference. This test provides objective information towards response speed, power and symmetry of the inferior members regarding received displacements. The prolongation of latencies informs us about lesions on nervous paths, either peripherical or central.
In any moment, DCP provides the etiology of dysfunction only by numbering systems which are involved in the process.
When is DCP recommended?Patients, who suffer from dizziness, ataxia and body unbalance and do not suit clinical criteria established to a certain diagnosis, are inclined to DCP (3). One might indicate the following (2):
- Tests of complementation of conventional vestibular exams.
- DCP is useful to isolate sensorial or motor system responsible by body balance disorder and to recommend proper therapy.
- Peripheral vestibular diseases
- For its specification and sensitiveness it is able to identify vestibular disorders in a precise and quick way.
- Neurological diseases
- It is useful on diagnosing and investigating neurological diseases such as Parkinson, multiple sclerosis, polineuropathies and peripheral neuropathy.
- Control of clinical therapy or rehabilitation
- It is an excellent exam to monitor functional and motor recovery during and after clinical treatment.
- Visual Vertigo
Late studies have been shown that the vestibule is used as a sensorial source especially in situation of conflict between visual and somatosensorial information (7). DCP is able to identify patients who use visual information instead of vestibular one, even if it is not the proper one.
In the elderlyBody unbalance and falls result from cumulative effect of peculiar degenerative diseases or phenomena towards aging. Isolating such factors makes dizziness approach proper.
Compensation and CapacityDCP can surely inform the final compensation state of body balance. Even after lesion of one of the systems, patient can try other sources of information and keep their posture properly.
SimulationsDCP holds specific physiological patterns. Non physiological patterns during the exam expresses favorably on deliberate simulation and oscillation.
CONCLUSIONDCP can improve the diagnosis rate of patients who suffer from complex body balance disorder (9,4). It is able to find previously the system responsible for the disorder with good sensitiveness and specification. It complements conventional tests of vestibular diagnosis, which are redundant on the analysis of VOR, and presents valuable clinical approach, documentation and monitoring of treatment of body balance disorder.
REFERENCES1. Assessment: Electronystagmography. Report of the Therapeutics and Technology Assessment Subcommittee. Neurology, 1996, 46(6):1763-1766.
2. Black FO. Clinical status of computadorized dynamic posturography in neurotology. Curr Opin Otolaryngol Head Neck Surg, 2001, 9(5):314-8.
3. Black FO. What can posturography tell us about vestibular function. Ann N Y Sci,, 2001, 940:446-64.
4. Black FO, Angel SC, Pesznecker SC, Gianna C. Outcome analisys of individualized vestibular rehabilitation protocols. Am J Otol,2000, 21:543-51.
5. Fife TD, Tusa RJ, Furman JM, Zee DS, Frohman E, Baloh RW, Hain T, Goebel J, Demer J, Eviatra L. Assessment: vestibular testing techniques in adults and children: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology, 2000, 55(10):1431-41.
6. Goebel JA, Hanson JM, Langhofer LR, Fishel DG. Headshake vestibulo-ocular reflex testing: comparison of results with rotational chair testing. Otolaryngol Head Neck Surg., 1995, 112:203-209.
7. Kaufman GD, Wood SJ, Gianna CC. Spatial orientation and balance control changes induced by altered gravitoinertial force vectors. Exp. Brain Res., 2001, 137(3-4):397-410.
8. Kroenke K, Hoffman RM, Einstadter D. How common are various causes of dizziness? A critical review. South Med J, 2000, 93(2):160-7.
9. Lipp M, Longridge NS. Computadorized dynamic posturography: its place in the evaluation of patients with dizziness and imbalance. J Otolaryngol, 1994, 23:177-83.
Doctor of Medicine (Medical assistant to the Division of Otoneurology HFMUSP)
Roseli Saraiva Moreira Bittar
Discipline of ENT Clinic (HCFMUSP)
Address: R. Dr. Enéas de Carvalho Aguiar, 255 - 6º andar - sala 6021 - São Paulo/SP- CEP: 05403-000 - Fone/Fax: 3069.6288 - E-mail: otoneuro@hcnet.usp.br
This article was submitted in Management System Publications (SGP) R@IO in the August 16, 2007. Cod. 298. Article accepted on August 16, 2007.