INTRODUCTIONBody spatial orientation is the result from stimuli integration of vestibular system, sight and through central nervous system (SNC). In this way, any involvement of this complex integration system can cause body imbalance.
The association of vertigo and cervical spine pain is common on otoneurologic patient, however dizziness of proprioceptive cervical origin and its therapy are questionable.
Dizziness of proprioceptive cervical origin would make part of cervical syndromes, which are defined as syndromes that cause head pain signs and symptoms arising from cervical area(1).
The hypotheses which relate alterations of cervical spine with dizziness start are based on potentialization of sensitive afferences of cervical area, on cervical sympathetic nervous system involvement or even on vascular compression(1,2). Those alterations can be caused by inflammatory process, traumas, bad posture and cervical arthrosis. Cervical spine traumas, mainly the ones related to sudden head movement and neck sprains (whiplash injury), can cause, besides cervical injuries, functional and/or morphological alterations of the CNS, especially on the cerebral stem(3).
Injuries on profound sub occipital muscles and on articulations related to neck movement can produce more sensitiveness of the local receivers, involving body balance, causing ataxia and nystagmus(4). According to Jongkees, alterations of the cervical cervical proprioception can cause nystagmus followed by vertigo, ear pain, cervical pain which gets worsen by the movements, muscle tension. These symptoms might or might not be followed by acute tinnitus and fluctuation in hearing threshold5. Brandt viewpoint is that dizziness features starting from cervical segment would be ataxia, instability and imbalance when walking(6). He also discusses the use of nystagmus caused by cervical torsion as a standard of diagnosis, as it can affect individuals in normal condition and also because the cervico-ocular reflex is notable in individuals with absent vestibular function(7).
Proprioceptive cervical sensitiveness is from articulated capsules of the first cervical vertebra and from sub occipital muscles. Its information passes through the spinal vestibular pathways, which lead themselves to the inferior vestibular nucleus and to the cerebellar vermis, together with eye afferences. Excessive muscle tension involves a good performance of the cervical proprioceptors, by resulting conflicting information on balance condition(8). Manipulation therapy, aiming to soothe cervical muscle tension, could also ease proprioceptive cervical sensitiveness and then, remedy local afferences that reach CNS.
The literature describes a good response of cervical-origin body balance to manipulation therapy(4,7,8). An aspect that should be taken into care when manipulating cervical area is vascular accident probability. It is a rare situation, which accounts for 1 in 400,000 or 1,300,000 cases, by considering all techniques. 18% of the cases lead to death(9-12).
Computerized dynamic posturography (CDP) is a test performed on the follow-up of different balance-related pathologies. Alund and cols. made use of such evaluation method when following up cervical vertigo situations(13).
OBJECTIVEThe target of this study is to evaluate possible interferences of manipulation therapy on vertigo of cervical origin.
METHODPaper approved by Research Ethics Committee under # 932/05 on June 29th, 2006.
Retrospective study of 3 male and 7 female patients (average age: 56.3 years and standard deviation: 8.13). They were from Ambulatório de Otoneurologia do Departamento de Otorrinolaringologia da FMUSP (Otoneurology Ambulatory of ENT Department).
In order to clinically diagnose vertigo of cervical origin, it was considered: complaint of dizziness, pain and/or cervical muscle spasm, absence of any other condition that could be associated to the complaint.
All patients were submitted to a conventional otoneurological evaluation which covered clinical history; ENT exam; cranial pair exam; cerebellar testing; electronystagmography (ENG) with water stimulus, according to Fitzgerald and Halpike(14); radiology exam of cervical spine on frontal and side occurrences. In 6 patients CDP was performed before and after manipulation therapy.
The inclusion criteria were: aging over 18; dizziness; cervical pain; ENG; cervical spine x-ray with signs of cervical osteoarthrosis, or cervical lordosis correction. The exclusion criteria were: simultaneous diseases which could be related to the presented symptoms and cervical trauma history.
Complaints of dizziness, tinnitus, cervical pain and hearing loss were evaluated according to analogical visual scale (AVS), in which symptoms were graded from 0 (absent symptom) to 10 (maximum discomfort).
Manipulation therapy was managed from the diagnosis of vertigo of cervical origin. The period from diagnosing to therapy beginning was from 3 to 6 months, in which no medication acting on vestibular system was used.
AVS results were considered as variables of study.
Manipulation therapy followed the protocols:
- exteroceptive stimulation.
- classical massage.
- cervical pompage.
- global pompage.
The target of the procedures was cervical muscle relaxation by moving head as least as possible, reducing vestibular stimulus at its most and its consequent behavior.
After manipulation therapy, patient was submitted to a new otoneurological clinical evaluation and then a new grading of symptoms through AVS was carried out. On patients who had CDP done, the exam was repeated.
The statistical analysis of the averages was performed through the Student´s-t test. The significance level was p<0.005 according to standards used for biological studies.
RESULTSFrom the 10 evaluated patients, 7 (70%) of them presented dizziness progress, and form these, 6 (60%) presented absent symptoms. The 3 (30%) remaining patients did not report improvements following the program (Chart I).
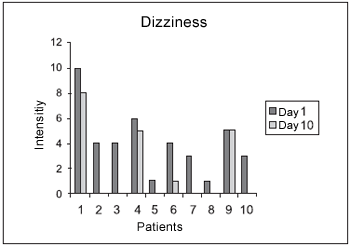
Chart 1. Development of dizziness before and after therapy.
Cervical pain was improved in 8 (80%) patients and 6 (60%) of them had it absent. Two patients did not report improvement on pain symptom or dizziness. (Chart II)
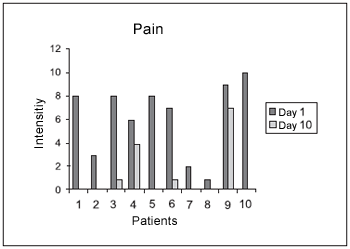
Chart 2. Development of pain before and after therapy
The obtained averages, both before and after therapy for dizziness symptoms on patients who reported improvement, were: 2.85 +/- 1.34 and 0.14 +/- 0.38 (t=5.72, p<0.05) and on patients who reported pain improvement, they were: 5.87 +/- 3.35 e 0.25 +/- 0.46 (t= 4.89, p<00.5).
In the current sample we found only one patient with bilateral continuous and acute tinnitus complaint, who presented with improvement after manipulation therapy.
The most constant findings on electronystagmography exam were: positional nystagmus in 2 (20%) patients. Nystagmus was from cervical torsion in 5 (50%) patients. Caloric tests showed hyperreflexia in 50% of the patients. Directional preponderance or labyrinth predominance were observed in only 3 (30%) of the patients.
From the 6 (60%) patients who underwent CDP before manipulation therapy, 4 of them presented normal results as regard their age and height and did not had any alteration after therapy. For 2 patients, CDP presented alterations on the first evaluation. After intervention, one of them presented with improvement and the other presented with normal response after the tenth therapy session.
Signs of cervical osteoarthrosis were the radiological diagnosis of all patients. 6 patients (60%) presented with cervical lordosis correction.
DISCUSSIONA good clinical background is the key to correct procedures on cases of body imbalance. A well done diagnosis provides proper therapy.
Besides cervical alteration is considered the primary cause of vertigo it can also be secondary when arisen from other vestibular pathology. In this situation, patient, through cervical muscle spasm, tries to keep head still avoiding labyrinth stimuli that cause dizziness by, this time, a proprioceptive stimulus even after vestibular problem, which started it, is healed.
We agreed on the statements by Brandt(6). We have no found any alteration which could isolatedly confirmed vertigo of cervical origin at the objective studies. We believe that both vestibular diseases and exam data should be considered together with clinical exam and background. According to our findings, clinical background of dizziness and cervical pain, when associated to muscle spasm or pain when touched; positional nystagmus; nystagmus of cervical torsion and hyperreflexia to caloric test during ENG, suggests diagnosis of cervical vertigo.
Manipulation therapy was positive in 70% of the patients, what agrees with Hulse and Holzl(8), who report expressive improvement on dizziness symptoms after cervical manipulation therapy on their patients. It is, however, important a good care when manipulating, by especially avoiding harsh movements and traction on cervical spine what can cause vertebral artery involvement(9-12).
Cervical manipulation can improve dizziness symptoms through reduction of excitability of cervical proprioceptive receivers, through muscle stretching, reduction of muscle twitch and posture correction, what would reduce information conflict of the CNS.
It was carried a new otoneurological evaluation on the 3 patients who did not present dizziness improvement in order to find another possible etiology. In one of them, who presented total relief on cervical pain but not on dizziness, it was observed heart arrhythmia (cardiogenic vertigo), and then patient was sent to heart doctor. In this case, cervical spasm was possibly from posture alterations, and not from origins of dizziness. The other two patients, who remained with cervical pain and dizziness, were diagnosed of anxiety disorder.
Although CDP, in the current study, is not considered as a useful tool for diagnosing vertigo of cervical origin, it is considered to be useful for following the effectiveness of manipulation therapy on patients who present CDP alteration at the initial evaluation. However, the material from the 6 patients does not allow any interference, thus another sample would change results.
Improvement on both pain and on dizziness is connected to muscle relaxation from muscle stretching and correct cervical posture, provided by proprioceptive stimulation, which helps patient to be more aware of their bodies.
On the last case in which patient presented with tinnitus at the beginning of manipulation therapy, the same patient denied dizziness, tinnitus and pain by the end of therapy. Tinnitus improvement could be justified by modulation of auditory signs through corticofugal path, as tinnitus can arise from somatosensory nucleus of the brain stem that receives afferences from cervical paths and from spinal tract of the trigeminal nerve(15).
CONCLUISIONBy considering dizziness and pain improvement reported by patients besides none of them have reported discomfort or opposite effect, the current study should be continued in order to search a better understanding of pathology and suggested therapy by aiming to improve quality of life of patients with cervical vertigo.
REFERENCES1. Bottino, MA. Doenças do ouvido interno in Bento RF, Miniti A, Marone SAM-Tratado de Otologia, EDUSP, 1988.
2. De Jong PTVM, de Jong JMBV, Cohen B, et al. Ataxia and nystagmus induced by injection of local anesthetics in the neck. Ann Neurol 1977;1:240-6.
3. Hinoki M. Vertigo due to Wiplash injury: a neurootological Approach. Acta Otolaryngol (Stockh.) 1985:Suppl.419:9-29.
4. Bittar RSM, Pedalini MEB, Hanitzch ES, Bottino MA, Formigoni LG. Síndrome cervivical proprioceptiva: considerações a respeito de um caso. Arquivos da Fundação Otorrinolaringologia 1998;2(4):153-6.
5. Jonkees LBW. Cervical vertigo. Laryngoscope 79(8):1473-84, 1969.
6. Brandt T. Cervical vertigo: reality or fiction? Audiol Neurootol. 1996;1:187-96.
7. Brant. T, Bronstein A.M. Cervical vertigo J Neurosurg Psychiatry 2001;71:8-12.
8. Hulse M, Holzl M. Vestibulospinale Reaktionen bei der zervikogenen Gleichgewiechtsstörung: Die zervikogene Unsicherheit. H.N.O. 2000;48:295-01.
9. Rothwell DM, Bondy SJ, Willians JI. Chiropratic manipulation and stroke: A population-based case-control study. Stroke 2001;32:1054-60.
10. Young YH, Chen CH. Acute vertigo following cervical manipulation. Laryngoscope 2003;113(4):659-62.
11. Menendez MG, Garcia C, Suarez E, Fernandez DD, Blazquez BM. Síndrome de Wallemberg secundário a disección de la arteria vertebral por manipulación quiroprática. Rev Neurol. 2003;37(9):837-9.
12. Refshauge KM, Parry S, Shirley D, Larsen D, Rivett DA, Boland R. Professional responsability in relation to cervical spine manipulation. Aust J. Physiother 2002;48:171-85.
13. Ålund M, Larson SE, Ledin T, Ödkvist L, Möller C. Dynamic posturography in cervical vertigo. Acta Otolaryngol (Stockh) 1991, suppl.481:601-2.
14. Proud GO, Barber HO. Pruebas de la función vestibular. In: Paparella MM, Shumrick DA. Otorrinolaringologia.2ª ed, Panamericana, vol II, p.1152-7. 1988.
15. Baner CA, Mechanisms of tinnitus generation. Curr Opin. Otolaryngol Head Neck Surg 2004, 12:413-7.
1. ENT Post-Graduation Student at Ophthalmology and ENT Department at FMUSP
2. PhD in Medical School (Doctor at Otoneurology Department of the ENT discipline at FMUSP)
3. PhD in Medicine (Head of Otoneurology Department of ENT discipline at FMUSP)
4. Physiotherapist (observer physiotherapist at Otoneuology department of ENT Discipline at FMUSP)
Hospital das Clínicas da Faculdade de Medicina da FMUSP - Medical School Hospital of University of São Paulo.
Mail address: Av Dr Eneas de Carvalho Aguiar nº 255, 6º andar - ICHC, São Paulo/SP - CEP:05403-000 - E-mail: megorl@hotmail.com
This article was submitted to SGP (Sistema de Gestão de Publicações - Publication Management system) of R@IO on August 17th, 2007 and approved on October 21st, 2007 at 20:37:24.