INTRODUCTION The tonsillectomy is one of the most performed surgical procedures in the whole world, reaching numbers of 500 thousand surgeries per year only in the EUA(1-2-3-4).
The first report of exeresis of palatine tonsils was performed by Cornelius Celsus, dated from 3 A.D. and it is until the current days, as the most common surgery performed by otorhinolaryngologists(1).
The indications of amygdalectomy are divided in absolute and relative. In the group of the absolute indications there is the amygdaline hypertrophy with blockage of superior aerial ways, syndrome of the obstructive sleep apnea, suspicion of malignity, hemorrhagic tonsillitis, and deficit of feeding, abnormalities of orofacial growth and of dental occlusion. In the relative indications there are the recurrent tonsillitis, the tonsillitis with systemic repercussion (rheumatic fever, anti-IgA), periamygdaline abscess and tonsillitis caseous.(1-8-9)
With the recent technological advances, every year new surgical, anesthetical and side therapies techniques appear which aim to diminish the surgical time, the bleeding and peri and postoperative pain, thus minimizing, the morbidity and mortality associated to tonsillectomies(3).
Many amygdalectomy techniques have already been described in literature as cold bistoury, guillotine, bipolar shears, electro cautery knife, laser Co
2, KTP laser (potassium-titanium-phosphate), cautery knife of suction modified by Armstrong,, bipolar forceps of argon coagulator, micro-needle, ultrasonic hook among others(3-4-5).
The harmonic scalpel appeared around 1992 and was used only in laparoscopic, gynecological and urological surgeries. Around 1999, this instrument started to be investigated and to be used by the otorhinolaryngologists. Ochi, in 2000, was the first author to describe the use of ultrasonic surgical knife in the performance of tonsillectomy(6).
The ultrasonic device is made of a generator, a part of hand (scaffolding and transducer) and a blade. It runs on vibratory mechanical energy (active frequency of 55.5 kHz). This mechanical energy generates an oscillation of the blade that promotes the superficial coagulation of the proteins, which when associated to the movements of the blades, produces the dissection of tissues(5).
The amount of energy supplied to tissues and its effect on them depend on different factors as the level of harnesses selected (1 the 5), on characteristic of the blade, on tissue tension, type of tissue, pathology and surgical technique, being that the bigger the power, the greater the vibration and consequently the bigger the area of cut(5) and the lower the coagulation effect.
In the studies previously published with the use of harmonic scalpel in the amygdalectomy performance, the blade used by the authors was of the "hook" type (Picture 1). Our study reports the experience with a new type of blade, the "Ultrasonic Blade" (Picture 2).

Picture 1 - "Hook" blade.

Picture 2 - "Curved Scissor" blade.
To evaluate this new surgical technique of amygdalectomy with harmonic scalpel comparing the surgical time, the intra-operatory bleeding, pain, the necessity of analgesic use and aspect of the amygdaline area in after the surgery with the technique of cold blade surgical knife.
CASUISTRY AND METHOD 100 sequential patients of both genders, with minimum age of 03 maximum of 10 years have been selected through anamneses, otorhinolaryngologic examination, nasofibrolaryngoscopy and in some cases polissonograhy, and who presented criteria of absolute indication for amygdalectomy associated to moderate hypertrophy (bigger that 50%) or serious (bigger that 75%) of pharyngeal tonsil. The patients who have history of periamygdaline abscess, chronic illnesses, coagulopathies and acute infection have been excluded. These children have been divided randomly in two groups: 50 patients (group 1) have been submitted the surgery of adenoamygdalectomy with the use of harmonic scalpel (ultrasonic blade) and 50 patients (group 2) submitted to the same surgical procedure however with cold blade and aspirating elevator. In both groups, the adenoidectomies have been performed in the same surgical time and with the use of curette for pharyngeal tonsil (Beckmann). The surgeries have all been performed by same surgeon and in the same place, during 2005 and 2006, after the research has been approved by the committee of medical ethics of the hospital (protocol: 2004-0020/5). All the tutors have received orientation in terms of the surgical method to be applied and have signed consent term approving it.
Before the beginning of the study, the surgeon underwent a period of specific practical training with the harmonic scalpel in which 10 surgeries have been performed in this hospital (learning curve) in addition to theoretical lessons on the functioning of the device given by the technician responsible for the manufacturer.
The device of harmonic scalpel (ultracision) is produced by Johnson & Johnson
® and was granted by the Ethicon Endo-Surgery
®. The hand part is sterile and disposable; having been, therefore, used one per patient. The blade was chosen as standard type "harmonic blade" in power "2". None of the authors have received any type of financing for this study; they have only received the donation of the ultrasonic blades and their maintenance.
All the patients have been submitted to the general anesthesia under orotracheal intubation by the same anesthesist and under same medications, varying only the dosage, proportionally to the weight of the patient. The surgical times have been rigorously followed in the two groups (adenoidectomy followed by left and later right tonsillectomy). The beginning of the time of each surgery was counted from the moment that the table was set, the fields set and the antisepsis done. The ending was considered at the moment that the hemostasis was considered satisfactory by the surgeon. The time of use of the surgical knife (harmonic or cold) initiated from the moment of the first incision and finished in total exeresis of lateral palatine tonsil.
The bleeding during the surgery was evaluated through the volume measured in the collector of the aspirator and registered in milliliters. The necessity of hemostasis with suture was also evaluated, which was performed with simple Catghut 3.0 suture when necessary. The presence of immediate postoperative bleeding (in the after-anesthetical recovery room - AAR), at the moment of the discharge and until the first outpatient return was also evaluated, 5 days after the surgery.
The evaluation of pain was performed at the moment of the hospital discharge and in the first outpatient return by the analogical scale and the number of analgesic doses. The analogical-visual scale was used (AVS) which was exhaustingly explained to the patients and tutors at the moment of the hospitalization. This scale consists of the drawing of 7 faces, placed in linear form and horizontally ordered with increasing expression of pain, from the right to the left (Picture 3). After the answer was obtained, the result was registered numerically, corresponding the face 1 of lesser pain (left) and 7 of bigger pain (right). All the parents or tutors have received the same analgesic prescription and the same orientation at the moment of hospital discharge: Paracetamol 1 drop/kg every 6 hours (maximum dose of 40 drops every 6 hours) if the child complained pain, cold and liquid feeding, to avoid the physical effort and the exposition to the heat. They have also received orientations to register the AVS daily, right after the patient woke up, before medicating him/her.
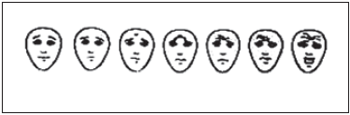
Picture 3 - Pain visual-analogical scale.
The criteria for hospital discharge have been: the permanence of the patient in the hospital for at least 8 hours after the surgery, present diuresis, and absence of vomit or of active bleeding.
The aspect of the amygdaline place was classified visually by the oroscopy in 4 categories: dry, presence of edema, presence of edema and fibrin and presence of coagulum. The evaluations have been made at the moment of the hospital discharge and in the first outpatient treatment. The evaluations performed during the surgery, AAR and moment of the discharge have been performed by the surgeon herself.
The evaluation of the first outpatient return, after 5 days, was performed by another researcher who was not aware of to which group the child belonged ("blind" examiner).
All the collected data have been registered in a specific protocol (Picture 4), considering that "the blind" examiner only had access to protocol "B".

Picture 4. Study protocol.
The surgical time, the amount of bleeding during the surgery, the necessity of hemostasia during the surgery, postoperative pain (AVS), the aspect of the amygdaline area (dry, edema, edema and fibrin or coagulum) and the number of doses of postoperative analgesic used have been compared between groups 1 and 2. The continuous variables with homoscedasticity and equality of variances (evaluated through the Levene Test) have been compared using test t by Student for independent samples. The continuous variables that did not meet these criteria and the ordinal variable have been submitted to test distribution free U Mann-Whitney. The categorical 0 variable has/have been compared by using the test of the qui-square and the accurate Fisher test. The adopted level of significance was of 5 % (p<0.05).
RESULTS 2 groups of 50 patients have been analyzed, being group 1 operated with harmonic scalpel and group 2 with bistoury of cold blade. Table 1 presents the demographic data and the characteristics of the tonsils and adenoids of groups 1 and 2. There was no statistical significant difference for age, gender and degree of amygdaline hypertrophy, however the children from group 1 presented severe hypertrophy of adenoid more frequently (p<0.01).
All the patients have appeared with tutor in the outpatient appointment 5 days after the surgery.
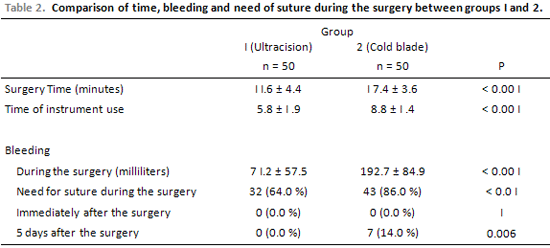
No patient showed bleeding during the surgery with intervention necessity after the adenoidectomy. In Table 2, the comparisons between groups 1 and 2 in terms of the surgical time, time of use of the surgical knife, bleeding and necessity of suture during the surgery, bleeding immediately after the surgery and on the first 5 days are presented. The surgical time and the time of use of the surgical knife have been significantly smaller in the group 1(p<0,001), taking around 2/3 of the time of group 2. In group 2, the total surgical time lasted around 3 minutes more than in group 1. The volume of bleeding and the ratio of patients who have also needed suture for hemostasis during the surgery have been significantly smaller in group 1 in relation to group 2 (p<0.001). No patient presented immediate postoperative bleeding and 7 patients (14.0 %), all of which from group 2 have reported some type of bleeding during the first 5 days after the surgery (p = 0.006).
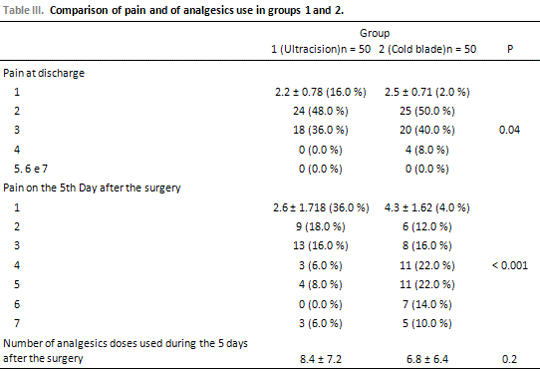
The comparison of the results of the evaluation of pain surveyed through the AVS after the surgery, as well as the number of doses of analgesics used between the groups are presented in Table 3. The former is also represented graphically in Graph 1. At the moment of the discharge, group 1 presented a score which was 0.3 lesser in relation to group 2 (p = 0,04), and in 5th postoperative day group 1 presented a score which was 1.7 lesser in relation to group 2 (p<0.001). Forty children (80.0 %) of group 1 reported their pain at that moment with scores 1, 2 or 3, against only 16 (32.0 %) of group 2. The average number of doses of analgesic used did not differ significantly between the groups (p = 0.2).
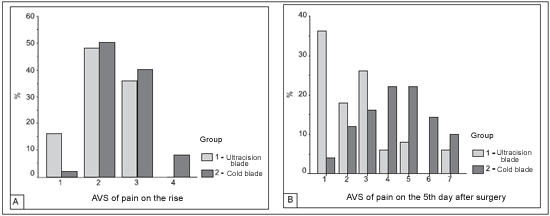
Graph 1. (A) - Percentage of patients in relation to pain (visual-analogical scale) at the moment of the hospital discharge(p<0.04)
(B) - Percentage of patients in relation to pain (visual-analogical scale) on the 5th day after the surgery(p<0.001)
There was no visualization of coagula or bleeds in the amygdaline areas in none of the patients examined in 5th after-surgical day. The comparison between groups 1 and 2 in relation to the aspect of the amygdaline area on that day is presented in Table 4.
There was no significant difference in the result of the incidence of edema and fibrin when the groups were compared.
DISCUSSION The harmonic scalpel (HS) appeared around 1992 and is indicated to cut soft tissues, complementing or substituting electrocautery knife(1). The basic system of the HS is composed of a generator, a handle of feeding, a stand and a pedal. The generator presents two connectors, electric and air, both for the hand part. The electric energy sent to the generator is converted into mechanical energy in the hand part that lodges the acoustic system and it does not vibrate when the system is activated(6). The blade longitudinally vibrates 55,500 times per second and the mechanical energy (ultrasonic) is transmitted for the extensor of plates that is settled by six silica rings in the points of zero amplitude. This energy is concentrated in the distal point of the blade transmitting maximum amplitude. The movement of the blade is connected to proteins of the tissue breaching the hydrogen linkings and disorganizing them. The vibrations of proteins produce a secondary heating forming one coagulum and sealing small vessels.
Sood et al(10). after the accomplishment of 158 amygdalectomies (59 with harmonic scalpel "hook") and Ramos1 after performing adenoamygdalectomies in 26 patients (13 with harmonic scalpel "hook") have already shown a significant difference in the surgical time between this technique and the conventional one. D'Avila(11), who performed a prospective study of 26 patients, in which he associated microsurgery to the HS, observed equivalence in the time of duration of the surgical act in comparison with the classic technique of dissection, with average of 14 minutes for each tonsil. Our study got a result in relation to the surgical time and to the time of use of the bistoury significantly lesser in group 1, taking around 2/3 of the time of group 2. In group 2, the total surgical time took around 3 minutes more than in group 1. Although the degree of adenoid hypertrophy presents a significant difference between the groups, we believe that this datum is not a bias of the results once the group that presented a degree of bigger hypertrophy (group 1) was the same that presented the lesser surgical time and bleeding.
In relation to the bleeding during the surgery, Sood(10) report that all the procedures performed with cold surgery knife have presented a volume of bigger bleeding besides making the necessity of hemostasis with surgical suture higher. On the other hand, out of the patients operated with HS by such author, only 15.4% have needed suture for hemostasis. D'Avila(11), with the help of the microscope, relates that he got an excellent control of the bleeding during the surgery and that 50% of the patients have only needed cauterization with the bipolar electric cautery of the thick vessels. This author also relates that he did not have any immediate and/or delayed postoperative hemorrhagic complication. According to Andréa(13), the microsurgery of tonsils provides lesser bleeding during the surgery as in the postoperative period, due to better preservation of the structures and more efficient vascular hemostasis. In our study, no patient presented bleeding in the immediate postoperative period (AAR). The volume of bleeding and the ratio of patients who have needed suture for hemostasis during the surgeries has been significantly lesser in group 1 in relation to group 2 (p<0.001). Our statistical study also found a reaction risk of children of group 2 to need suture for hemostasis during the surgery 2.0 times (1.1 to 4.0) higher than the risk of group 1 (p = 0.01). It was not possible to distinguish if the bleeding was amygdaline or adenoideane, even so, the risk of children of group 2 to report bleeding in first the 5 days of postoperative was 2.2 times (IC 95% 1.7 to 2.7) the risk of group 1. The coefficient of correlation of Pearson between the duration of the surgery and the amount of bleeding was of 0.23 for group 1 (p<0.1) and of 0.33 for group 2 (p<0.02) having significant correlation between the amount of bleeding during the surgery and the time of surgery in group 2.
A prospective study with 58 patients performed by Geraldo D. Sant Anna(12) quantified postoperative pain in adults and children with more than five years of age submitted to elective tonsillectomy and demonstrated a distinct standard in postoperative pain among individuals with more or less 10 years of age being the intensity of related pain, its decrease and its lesser disappearance for the group of 10 years or less, than the one in the patients of 11 years of age or more. He also concluded that the difference was kept in the direction of the lesser frequency of analgesic use and in the precocious return to a normal diet.
Some authors report absence of pain in the immediate postoperative period; however, pain in the subsequent days was not statistically different in relation to the cold bistoury and harmonic scalpe(2). Ramos(1) found greater pain in the immediate postoperative period in the group operated with HS (30.8% of the cases) than in the control group (7.7%). Andréa(13) concludes that the reduction of pain in the tonsillectomies made with cold surgical knife with the microscope use is due to the identification and preservation of peripheral nervous structures, mainly of branches of the glossopharyngeal nerve(1-2), as well as the most efficient hemostasis. Other authors compare the surgery of electrocoagulation with cold dissection and show that the cold technique causes less pain in the pos operative period; however the electrocoagulation presents less bleeding(1-2). Our study he did not find significant difference in relation to the immediate postoperative pain (AAR). Pain in this period can suffer action from the analgesic use during the surgery by the anesthetist.
However, in the late post-operative period, there was an important reduction of pain in the patients operated with the ultrasonic blade. The risk of a child submitted to amygdalectomy with the use of ultracision to present scores of
< 3 of pain (AVS) in 5th postoperative day was of 3.1 times (IC95% 1.8 to 5.6) the risk of the children submitted to the conventional surgery.
Electrophysiological studies demonstrate that harmful stimulation can induce, for activation of afferent C fibers, changes of long duration in the excitability of the neurons of dorsal horn. The supported hyperexcitability of the spinal marrow produced by nociceptive gross stimuli can contribute for pain after the surgery. The harmonic scalpel which causes minimum tissue injury and a reduced use of the electrocoagulation can result in diminished nociceptive stimuli and therefore, in diminished level of pain after surgery(3).
In the first postoperative period performed by Branches, 69.2% of the patients operated with cold surgery knife and 30.8% of the patients operated with HS have presented edema. All the patients of first group and 46.1% of the patients of the second group had fibrin in this period. Only one patient from group 1 (7.7%) related to bleeding and none did from group 2. A patient of each group presented coagula in the fossas. Our study shows, in first late postoperative period, performed five days after the surgery, of operated patients HS 98.0% (49) presented fibrin in amygdaline fossa, 50.0% (25) edema. Out of the operated ones with cold surgery knife, (50) have been found 100% (50) fibrin and 38% (19) of edema. However, there was no significant difference between the groups. None of the two groups presented coagulum or bleeding.
CONCLUSION The use of ultracision in the amygdalectomy was associated with the lesser surgical time, lesser bleeding during the surgery, minimum necessity of haemostatic suture and lesser punctuation in pain (AVS). The postoperative aspects of the amygdaline fossas have not presented significant difference. We therefore believe that the use of the ultrasonic blades is possible in the amygdalectomy performance.
REFERENCES 1. Ramos FA, Ferreira RDP, Silva RH, Prado EP. Estudo Comparativo entre duas técnicas de tonsilectomia: bisturi harmônico e dissecção tradicional com bisturi de lamina fria. Rev. Bras. Otorrinolaringol 2004;70:316-322.
2. Maddern BR. Electrosurgery for Tonsillectomy. Laryngoscope 2002;112 (8 part 2) supplement no 100.
3. Steward DL, Chung SJ. The role of adjuvant therapies and techniques in tonsillectomy. Curr opin otolaryngol. Head and neck surgery. 2000;8(3):186-192.
4. Rideout BMSIV, Shaw GY. Tonsillectomy using the Colorado microdissection needle: a prospective series and comparative technic review. South Med. 2004; 97(1):11-17.
5. Akural EI, Koivunen PT, Teppo H; Alahuhta SM; Löppönen HJ. Post-tonsillectomy pain: a prospective, randomized and double-blinded study to compare an ultrasonically activated scapel technic with the blunt dissection technic. Aneaesthesia. 2001; 56(11):1045-1050.
6. Ochi K, Ohashi T, Sugiura, N, Komatsuzaki Y, Okamoto, A. Tonsillectomy Using an Ultrasonically Activated Scapel. Laryngoscope. 2000; 110(7):1237-1238.
7. Friedman M, LoSavio P, Ibrahim H, Ramakrishnan V. Radiofrequency tonsil Reduction: Safety, Morbidity, and Efficacy. Laryngoscope. 2003; 113(5):882-887.
8. Kavanag TK, Beckford SN. Adenotonsillectomy in children: Indications and contraindications. Southern Medical Journal 1988; 81(4):507-11
9. Almeida ER, Campos VAR - In Campos CAH, Costa Hoo. Tratado de Otorrinolaringologia. 1 edição. São Paulo: Ed Rocca; vol 3:248-52, 2002.
10. Sood S, Corbridge R, Powles J, Bates G, Newbegin CJR. Effectiveness of the ultrasonic harmonic scalpel for tonsillectomy. ENT - Ear, nose & Throut Journal . 2001;514-8.
11. D´Avila JS, Neto JCT, Antunes A. Microcirurgia de tonsilas com bisturi ultracision. 2001;5(4):172-174.
12. Sant Anna GD, Mauri M, Silva DB. Dor pós-tonsilectomia: comparação entre pacientes com diferentes idades. Rev. Brás Otorrinolaringol 2000;60(2):15-17.
13. Andréa M. Microsurgical Bipolar Cautery Tonsilectomy. Laryngoscope. 1993;103:1177-8.
1. Otorhinolaryngologist Medical Doctor
2. Otorhinolaryngologist Resident at Hospital CEMA - São Paulo
3. Otorhinolaryngologist Medical Doctor and Preceptor of Medical Residence at Instituto CEMA - São Paulo
4. Otorhinolaryngologist Medical Doctor and Preceptor of Medical Residence at Instituto CEMA - São Paulo
5. Otorhinolaryngologist Medical Doctor, Master's and Doctor's degree by UNIFESP/EPM - São Paulo. (Coordinator of Medical Residence at Instituto CEMA - São Paulo)
Hospital CEMA - Contact: Raquel Salomone
Mail Address: Rua: Jaci, 164 - CEP:04140-080 - Phone: (11) 82119946 - Fax: (11) 50729254 - E-mail raquelsalomone@yahoo.com.br
This article was submitted at SGP (Sistema de Gestão de Publicações) (Publication Management System) of R@IO on October 13th, 2007 and approved on November 2nd, 2007, at 10:38:36.