INTRODUCTIONThe etiology of oroantral fistulas is very varied, among which we may point out pathologies which affect the maxillas, sequels of surgeries for tumor or cystic lesion removal and, the most frequent one, surgery for maxillary teeth extraction (pre-molar and molar). Several methods for the closing of such fistulas have been reported in the Medical literature, such as Killey & Key's in 1967, who demonstrated the slide-in flap technique through vestibular or palatine areas. However, this method is not always efficient in the treatment of such communications.
An oroantral fistula which is smaller than 2 mm frequently closes spontaneously. However, when the defect is bigger or when there is inflammation, maxillary sinus or periodontal region infection, such fistula demands surgical treatment for its complete closing (1).
The anatomy and vascularization of the buccal fat pad were investigated by Tideman et al. in 1986, and were classically described as holder of four extents: buccal, pterygoid, and superficial temporal and deep temporal. Its body is the area with most facial surgical access.
Egyedi, in 1977, was the first one to report the use of buccal fat pad in a pedicellate way. And in 1983, Neder referred to the use of the buccal fat pad as free graft in 2 patients in the construction of oral defects which had artificially been created. A study presented by Tideman et al in 1986 about the use of pedicellate graft with the buccal fat pad to correct buccal and maxillary defects concluded that such grafts present good results.
Consequently, we aim at reporting a clinical case of secondary closing of oroantral fistula through the technique of buccal fat pad as pedicellate graft associated to mucous graft.
CASE REPORT47-year-old male leukodermatous patient, referred to the oral and maxillofacial attention at the multiple-specialty clinic in Blumenau-SC complaining of pain on the left hemiface and of persistence of non-healed orifice due to a superior tooth extraction six months before. At the clinical examination, a fistula in alveolar border of left maxilla was observed, with communication with the maxillary sinus and pus drainage after orifice pumping with a curette. The X-ray revealed left maxillary sinus veiling with fault in its floor (Pictures 1 and 2), leading it to the chronic sinusitis diagnosis.
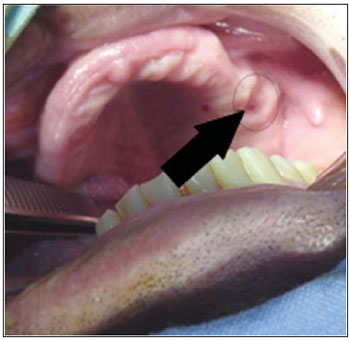
Picture 1. Buccalsinusal communication.
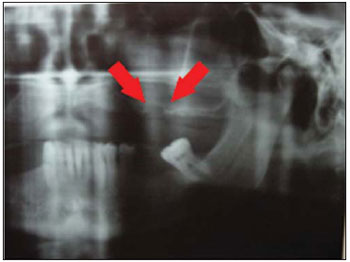
Picture 2. Panoramic X-ray which shows bone defect.
Antibiotics and anti-inflammatory medication have been used to control the infection and to a further closing surgery through the use of buccal fat pad technique. After 7 days using the medication, the patient underwent a new evaluation, when he presented no symptoms and no pus drainage in the fistula.
The closing surgery happened under general anesthesia through nasal-tracheal intubation. The approach has been started with infiltration of vasoconstrictor solution (adrenaline 1/90,000) in and area adjacent to the perforation and at the bottom of the left maxillary groove. The borders of the fistula were subperiostally incised in wedge with superior extension in vestibular floor up to the inserted mucosa. The posterior-superior elevation was done with a Freer elevator, close to the maxillary wall until the buccal fat pad was found. At this moment, a mild suction was started with aspirator beak, which enables the fat elevation up to the oral cavity. The buccal fat pad was gently stuck by tweezers and gripped up to the fault (Picture 3 and 4)
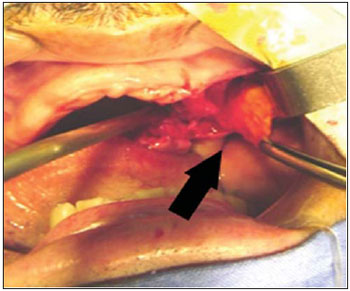
Picture 3. Buccal fat pad gripping.
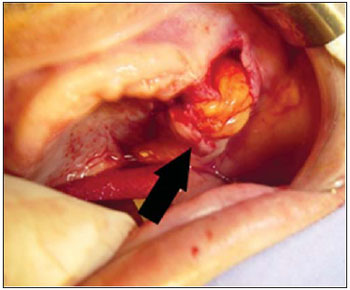
Picture 4. Buccal fat pad exposition.
After the complete covering of the bone defect, the fat was stitched to the adjacent mucosa with plain catgut 3.0 suture. At this moment, a supra-periostal longitudinal incision aiming at the hard palate was done, elevated and rotated to cover the buccal fat pad, and then stitched to the alveolar mucosa vestibular to the defect (plain catgut 3.0). After the surgery, the patient was medicated and guided to not do intra-oral negative pressure and to cease using his denture for thirty days. The post-surgical phase has no complications, and a mild loss of vestibular groove depth was observed, but did not prevent him from using his denture (Picture 5 and 6).
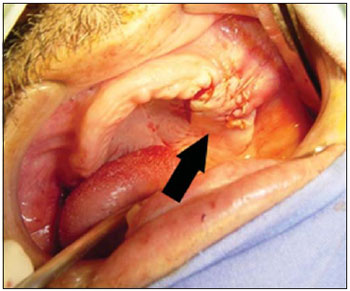
Picture 5. Final aspect of the fistula closing.
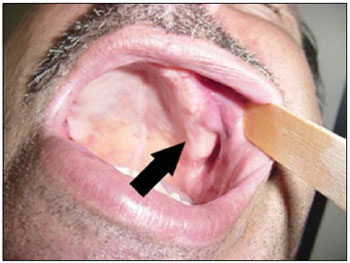
Picture 6. Image after 30 days.
The primary closing of oro-antral fistulas in 48 hours presents a 90 to 95% success rate, and such rate falls to 67% when the closing is secondary (5,6). The latter is still a problem with difficult solution. It is essential that the sinusitis is treated first. Several authors demonstrated that a three-day exposure of the maxillary sinus presents a pathology through radiographic evidence (7,8).
The buccal fat pad may be used to close oro-antral communications once its success has been proved in the medical literature and because it does not interfere the vestibular groove depth. Due to its anatomical position, it has beneficial characteristics to be used as pedicellate graft to reconstruct intra-oral defects, specially in the posterior region of the maxilla.
CONCLUSIONThe treatment of oro-antral communications through the use of buccal fat pad is a simple and complete method, which enables several uses in most of the cases. The blood supply of the buccal fat pad is not affected due to its displacement, once it is gripped and replaced between the flap and the maxillary wall. The operated case had no complications and the chronic sinusitis was cured.
BIBLIOGRAPHIC REFERENCE1. Hanazawa Y, Itoh K, Mabashi T, Sato K. Closure of oro-antral communications usig a pedicled buccal fat pad graft. J oral Maxillof Surg. 1995, 53:771-775.
2. Tideman H, Bosanquet A, Scott J. Use of the buccal fat pad as a pedicled graft. J oral Maxillofac Surg. 1986, 44:435-440.
3. Egyedi P. Utilization of the buccal fat pad for closure of orao-antral and/or oro-nasal communications. J Maxillofac Surg. 1977, 5:241.
4. Neder A. Use of buccal fat pad for grafts. Oral Surg. 1983, 55:349.
5. Eppley B, Scfaroff A. Oro-nasal fistula secondary to maxillary argumentation. Int Oral Surg. 1984, 13:535.
6. Stajcic Z. The buccal fat pad in the closure of oro-antral communications - A study of 56 cases. J Craniomaxillofac Surg. 1992, 20:193.
7. Ericson S, Finne K, Persson G. A clinical - radiographic review of treated oro-antral communications. Int J Oral Surj. 1973, 2:185.
8. Haanaes H R, Pedersen K N. Treatment of oroantral communication. Int J Oral Surg. 1974, 3:124.
1. Oral and Maxillofacial Surgeon at Hospital Santa Catarina and Santo Antônio de Blumenau - SC. Medicine Student at Universidade Regional de Blumenau- FURB.
2. Medicine Student at Universidade Regional de Blumenau- FURB.
Institution: Universidade Regional de Blumenau - FURBBlumenal / SC - Brazil.
Mail address:
José Carlos Martins Junior
Armando Odebrech 70, Sl. 1006 - Garcia
Blumenau / SC - Brazil - Zipcode: 89020-400
Telephone: (+55 47) 3322 4389
E-mail: j.c.martinsjr@bol.com.br
Article received on June 06, 2007.
Article approved on October 12, 2007.