INTRODUCTION Dizziness, which is generally considered one of the most frequent complaints on medical clinics, may cause difficulties on the subject daily life and even reduce their life quality.(1)
The study of the group of physical and emotional disturbances that concern the several kinds of dizzinesses may produce intense functional disturbances, which harms the professional, social and domestic activities of the patient, which makes the recover of their physical and psychological balance a great challenge (2). Speech doctors that work with evaluation and rehabilitation of body balance disturbances, should bare in mind that recognizing such disturbances may be an important step in the rehabilitation of their patients.
Anyway, it is correct that vestibular disorders of any kind produce several significant harms on the patients' abilities, in terms of managing their independence. They may require assistance for simple tasks that were previously performed normally in their lives (3). Those findings may be evaluated nowadays with the use of handicap inventories.
The handicap may be seen as the social consequences of incapacity, such as the difficulty to work due to the dependence to drive caused by dizziness (4).
Therefore, medical literature has shown that the handicap may be higher or lower according to the features of the vestibular lesion (5,6,7), to the duration and intensity of physical symptoms (3,8), as well as to the life style, expectations, motivations and psychological state of each subject.
The relation between dizziness and psychological disorders in adult and elderly subjects is very strong (9,10,11,12,13,14). There is a high proportion of otoneurological patients that demonstrate psychological disorders (15). Identifying those neurological problems on otoneurological patients start to be an important task, once the treatment given to the subject who has dizziness may be more influenced by the disease suffering and behavior than by the severity of the organic pathology (16).
Once dizziness may cause difficulty in daily life, many authors (8,11,17,18) developed questionnaires about handicap in patients with complaints related to the vestibular system during the last years.
Therefore, the objective of this project was to determine the handicap in subjects with dizziness symptoms, associated or not to tinnitus complaint, through the Brazilian DHI. The secondary objectives of this study were:
1. To establish the relation between the handicap and vestibular symptoms and signs.
2. To establish the relation between the handicap and vestibular exams result.
MATERIAL AND METHODOLOGY The study has been performed in an Otorhinolaryngology private clinic at the Otoneurology department and approved by the Research and Ethics Committee at Cefac - SP under the record number 167/06. A group of 27 subjects aging from 17 to 78 years old has been evaluated, which were distributed according to gender into 24 female subjects and 3 male subjects.
As an inclusion criteria on this study, the subjects should have undergone a complete audiologic evaluation, including vocal and tonal audiometry and impedanciometry; the subjects should have presented dizziness for more than 6 months and be older than 15 years older.
Any subject who presented evidences of a central vestibular dysfunction (18), severe hearing loss (19) and tympanometric curve of B kind that suggested presence of liquid in the medium ear would be excluded from the sample.
After having signed the informed consent term, all subjects underwent to an interview, with the purpose of verifying the fact, the time and intensity of hearing and vestibular signs and symptoms. The following vectoeletronistagmography tests have been performed: Investigation of dizziness and/or positional nystagmus, ocular movements calibration, spontaneous nystagmus with open and closed eyes (NE OA/OF), Semi-spontaneous Nystagmus (NSE) Horizontal Pendulum Tracing (RP), Optocynetic Nystagmus (NO), pre and post rotatory nystagmus in the Decreasing Pendular Rotatory Test, and pre and post caloric in the Caloric Test (PC), under the temperatures 30ºC and 44ºC with water.
The interpretation criteria of vestibular exam were followed according to the propositions by Mangabeira-Albernaz et al (1986) (18). The vectoeletronistagmography VN 116 BERGER has been used, with three register channels and the otocalorimeter OC 114 BERGER for the performance of the caloric tests.
After that, the Dizziness Handicap Inventory (DHI) has been applied, which has been developed by Jacobson and Newman (1990) (16) and translated to Portuguese by Castro (2003) (7). Such material is made of an auto perception questionnaire which evaluates the dizziness associated to the incapacities and handicap in the three areas of a patient's life: Physical, functional and emotional.
The answers have been scored as "0" for "no" (absence of symptoms/difficulties), 2 for "sometimes" (occasional presence of symptoms/difficulties) and 4 for "yes" (severe presence of symptoms/difficulties). Thus, the minimum punctuation would be 0 points (not representing handicap) and the maximum would be 100 (representing maximum handicap), being 28 points (7 items) for the physical aspect, 36 points (9 items) for each of the functional and emotional aspect.
As the Original Brazilian DHI does not present handicap interpretation in degrees, the punctuation of this project has been distributed into 4 degrees, for matters of analysis: 0 to 25 points (without handicap), 26 to 50 points (mild handicap), 51 to 75 points (moderate handicap) and 76 to 100 points (severe handicap). In order to establish a relationship between the punctuation of DHI and the several variables studied a descriptive and a statistics analysis have been performed.
For the application of the descriptive analysis, the correlation of Spearman and the level of significance of 5% (0.05) have been adopted, and for the statistics calculations, the program Statistical Package for Social Sciences (SPSS), version 10.0, has been adopted.
After the performance of otoneurologic exams and the punctuation obtained at the Brazilian DHI, the results have been compared, aiming at relating the vestibular signs and symptoms with the conclusion of the vestibulometry and the total handicap of the subjects.
RESULTS Of the 27 evaluated subjects, 24 (88.8%) were female and 3 (11.2%) were male. 48% of the evaluated subjects aged from 41 to 60 years old, followed by the subjects older than 61 years old (29%).
The general distribution of the Brazilian DHI in the evaluated sample may be observed on Graph 1.
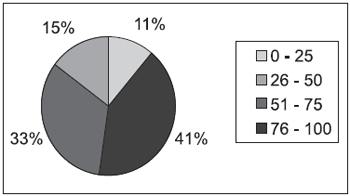
Graph 1. Score distribution of DHI on patients with vestibular complaints.
41% and 33% of the evaluated subjects can be mostly seen between 26-50 and 51-75 points respectively, that is, most of the subjects evaluated on this investigation may be seen at the mild and intermediate handicap, according to the analysis criteria suggestions of this project.
The distribution of the total Brazilian DHI with the functional, emotional and physical aspects and its respective averages, standard deviation, mode, median, minimum and maximum of each is demonstrated on Table 1.
The punctuation of the evaluated subjects has been significant with an average of 49.7 points, being the physical and functional aspects in equal proportions with an average of 18 points, followed by the emotional aspect, with an average of 12.8 points.
The scores of the Brazilian DHI have been related with age and gender variables and are not considered statistically significant (Tables 2 and 3).
Out of 27 subjects with dizziness complaint, 16 (59.2%) mentioned tinnitus, and 5 (18.5%) said that such symptom rarely occurs. Thus, the presence of tinnitus has been related with the total values of the Brazilian DHI as it can be observed on the following Table 4.
Among the subjects that presented tinnitus, the period of installation of such symptom has been taken into account (if it started in 1 year, in 1 year and a half or in 2 years.
The time of tinnitus has been close among those who had such symptom in 1 year (43.7%) and those who have had it for more than 2 years (50%).
Similarly to what happens with the tinnitus, the period of dizziness has also been taken into account and can mostly be seen in the subjects who have had it for 1 year (44.4%) and for more than 2 years (37.1%). The period of tinnitus has been statistically related the period of dizziness (p=0.007).
The intensity of dizziness has also been related with the Brazilian DHI values, which are mostly shown, at the intermediate degree, in 10 (37.1%) subjects and variably in 9 (33.3%), followed by the mild and intense degrees in 5 (18.5%) and 3 (11.1%) subjects, respectively.
The kind of dizziness, that is, if it is rotatory or not, or both, has been another variable analyzed. Out of the 27 subjects with dizziness complaint, 17 (63%) affirmed to be rotatory, 8 (29.6%) affirmed to be non-rotatory and 2 (7.4%) of both types.
The presence of nausea, sweating and paleness, which are considered neurovegetative symptoms were mentioned in 77.7% of the subjects.
The intensity of the dizziness (p=0.517), which has been evaluated isolatedly, as well as the kind of dizziness (p=0.544) and the presence of neurovegetative symptoms (p=0.302), have not been significantly related with the DHI Brazilian values, that is, they have not contributed with the determination of the handicap degree.
In the vestibulometry, all the evaluated subjects have presented regular calibration of ocular movements. The spontaneous nystagmus has been absent with open eyes, and with closed eyes it has been presented in 10 subjects, but its direction and velocity have been within the normal standards.
The results found on the NSE, RP and NO research have been within the adopted normal standards, as well as the symmetry of the directional preponderance of the nystagmus in the PRPD.
The evaluated subjects were different in the research concerning the positional and post caloric nystagmus, making an individual discussion of each performed test necessary.
Concerning the investigation of positional nystagmus, most of the subjects (81.4%) presented dizziness and/or nystagmus, some followed by neurovegetative symptoms. Five subjects (18.5%) presented absence of response.
In the PC it has been observed that 23 (92%) subjects presented normal responses, and 2 (8%) presented altered responses. One subject presented labyrintic preponderance > 33% and another presented hyperrflexy in total value on his left ear. It has not been possible to obtain the Jongkees Rate in two subjects due to the intensity of the neurovegetative symptoms presented in the warm tests, but its responses were found normal.
The conclusion of vestibulometry revealed 81.4% altered exams, and 77.7% indicated an Irritative Peripheral Vestibular Syndrome and 3.7% a Deficient Peripheral Vestibular Syndrome. Five subjects (18.5%) presented normal vestibular exams. Their values have been related with the Brazilian DHI according to the following table (Table 5).
DISCUSSION According to the sample, it can be observed that age must have been a factor that contributed for the increase of frequency of vestibular symptoms. The medical literature demonstrates that it is more frequent in female subjects and affects more adult and elderly people (21,22,23).
Despite of the higher number of women and of people between 42 and over 61 years old in the investigation, those variables are not related to the increase of handicap. The analyzed data are in accordance with the medical literature, which have not found any relation between sex and age with the incapacities severity (3,11,24,25,26).
Thus, we may consider that age, if analyzed as an isolated factor, does not contribute for the increase of handicap, because, for many times, the concomitance of dizziness with other symptoms or diseases for an elderly person will not bring great changes to his/her daily routine, once they have a less active life or are not acting professionally anymore.
The fact that the sample presents a higher punctuation in the physical and functional aspects of dizziness, followed by emotional aspect, corroborates with the medical literature, in which a higher modification in the physical aspects in the groups of benign paroxistic positional dizziness and in the physical and functional aspects in the groups with Ménière Disease (26) have been observed.
As the presence of tinnitus is analyzed, it can be observed that this has been a factor that called the attention for the contribution of the handicap for dizziness in those subjects, although it has not been significant. In a sample with a higher number of subjects, such result may be different.
It is important to pint out that the subjects that have been classified as holders of mild handicap, between 26 and 50 points, were distributed in a not even way among the ones who have tinnitus (n=6) and the ones who do not have it (n=2). On the other hand, the 3 subjects with Brazilian DHI with severe degree presented associated tinnitus and dizziness, while no subject under this handicap range holding tinnitus has been found.
Those data may make us think about the contribution of the union of two or more symptoms for the increase of incapacities, reflecting on the life quality of the subjects. A higher emotional suffering is common in patients with complaints of three or more symptoms.
The medical literature has demonstrated that the tinnitus itself brings handicap to the lives of the subjects (27,28). As the period of both symptoms have been closely related, this helps us to understand better the interference of tinnitus in the handicap for dizziness in those subjects.
In relation to fact that the intensity and kind of dizziness not being determinant in the handicap degree, the literature has controversies about it, once there are authors that state that the high frequency and severity of dizziness have been associated with the high negative impact in the life quality and in the limitation of daily activities (8,29), and others believe that the low levels of dizziness and unbalance many times may be enough to maintain a handicap and significant suffering.
We believe that the influence of other variables may have a higher weight in the determination of the incapacities, such as profession, personality and life style. Depending on what the subject does during their day-by-day, the functioning of the vestibular system needs to be harmonic between the years. This way, mild dizziness, flotation sensation or unbalance should be enough to refrain them from their professional duties.
This way, we can realize that the characteristics of the physical symptoms were not determinant for the incapacities profile of dizzy subjects.
Psychological conditions of depression and anxiety are important factors in order to determine the problem degree caused by the dizziness. The frequency distribution of patients with high impact on daily activities, on life quality and on fear of a coming dizziness, presented high rates in the patients' responses who were affected by psychological suffering (8).
Concerning the vestibulometry, the findings are different from other studies' findings (6.7), in which significant differences on the Brazilian DHI results have been observed concerning unilateral and bilateral harm of the vestibular system function. In one study, it has been observed that patients with DPVS presented higher harm on life quality in the functional aspects to the Brazilian DHI application, in relation to IPVS patients. (30).
No harm has been found on the life quality significantly associated with the vestibulometry findings. Although most of the evaluated subjects (81.4%) have shown altered vestibular exam with handicap varied proportions, there is still a small percentage of subjects (18.5%) with normal exams with a high important level of handicap, with an average of 45.6 points, reaching 68 points in one subject.
Thus, we believe that two or more people may have the same diagnosis and the same kind of dizziness, but be differently affected. This way, all the symptoms that follow dizziness, as well as the handicap profile and its incapacity analysis, will suffer some kind of interference according to their life style, to their expectations, motivations and psychological situation. That is why the description of a dizzy patient is very particular, once it gathers all those variables and even the role that the subject has at work, at home and in society.
Because of that, we realize the importance of handicap questionnaire in clinics practice, once the clinical exam and vestibulometry are not enough to investigate the functional and emotional parts of dizziness. Many times the harm degree on those areas influences in the patient's attendance to the doctor's office and makes us understand why there are some labyrintopathy patients that look for treatment and some that do not.
Maybe the agglutination of such procedures in the clinic routine provides more specific data which allow the definition of the best behavior and counseling with the dizzy patient.
The introduction of questionnaires in the clinical routine aids, among other things, the reduction of discrepancy found in the doctor's and patient's opinion. The psychological factors, which are difficult to be evaluated, contribute for the differences found in the evaluation between doctor and patient in the impact that dizziness causes in the subject's health (8).
The application of Brazilian DHI and of any other questionnaire could be useful in the clinical situation of the patient, once it helps the doctor with their treatment plan, as well as with the indication of psychological intervention, for example.
Besides, the questionnaires could also be one of the parameters to verify the possibility of the subjects to be candidates of Vestibular Rehabilitation therapy, having more acceptances to this treatment, after realizing their own difficulties during the questionnaire application.
For the professionals that work in the otoneurological area, the application of the self-perception questionnaire will be a valuable and useful clinical instrument and should be included in the clinical evaluation and also in the evolution monitoring of any patient with vestibular complaint.
Although the clinical experience shows that dizziness may bring psychosocial consequences, there are not many projects in the Brazilian literature that cover this issue with more details, like it happens with hearing loss, about which there are many investigations.
It would be interesting that new projects be developed, using the Brazilian DHI in more investigations, or even comparing different handicap questionnaires, trying to improve the life quality of patients with vestibular complaint.
CONCLUSION With the results found in the investigation in patients with vestibular complaint, we can conclude that:
- The handicap in subjects with dizziness has shown a higher number in the ranges between 26-50 and 51-75 points on the Brazilian DHI, that is, between the mild and intermediate ranges of the handicap, with a higher punctuation in the physical and functional aspects of dizziness, followed by the emotional aspect.
- The tinnitus symptom has been a factor that called attention for the contribution of handicap, being its period significantly related with the dizziness period.
- The gender and age variables have not been statistically significant in relation to the Brazilian DHI results, as well as the characteristics of physical symptoms such as duration, intensity and kind of dizziness and the presence of neurovegetative symptoms.
- The findings of the vestibular exams have not been significantly related with the Brazilian DHI results either.
- The functional and emotional investigation of dizziness, through the Brazilian DHI, has demonstrated to be a valuable and useful instrument in the clinical routine.
BIBLIOGRAPHY1. Enloe LJ, Shields RK. Evaluation of health-related quality of life in individuals with vestibular disease using diseasespecific and general outcome measures. Phys Ther 1997; 77(9):890-903.
2. Ganança FF. Tratamento da vertigem e de outras tonturas. São Paulo: Lemos Editorial; 2002.
3. Cohen H. Vestibular rehabilitation reduces functional disability. Otolaryngol Head Neck Surg 1992; 107(5):638-43.
4. World Health Organization International. Classification of Impairments, Disabilities and Handicaps. WHO, Geneva; 1980.
5. Bamiou DE, Davies RA, McKee M, Luxon LM. The effect of severity of unilateral vestibular dysfunction on symptoms, disabilities and handicap in vertiginous patiens. Clin Otolaryngol 1999; 24:31-8.
6. Jacobson GP. Calder JH. Self-perceived balance disability/handicap in the presence of bilateral peripheral vestibular system impairment. J Am Acad Audiol 2000; 11(2):76-83.
7. Castro AS. Dizziness Handicap Inventory: adaptação cultural para o português brasileiro: aplicação, reprodutibilidade e comparação com os resultados à vestibulometria [dissertação]. São Paulo: Universidade Bandeirante de São Paulo; 2003.
8. Honrubia V, Bell TS, Harris MR, Baloh RW, Fisher LM. Quantitative evaluation of dizziness characteristics and impact on quality of life. Am J Otol 1996; 17(4):595-602.
9. Yardley L, Owen N, Nazareth I, Luxon L. Prevalence and presentation of dizziness in a general practice community sample of working age people. Br J Gen Prac 1998; 48:1131-5.
10. Hallam RS, Stephens SDG. Vestibular disorder and emotional distress. J Psychossom Res 1985; 29(4):407-13.
11. Yardley L, Putman J. Quantitative analysis of factors contributing to handicap and distress in vertiginous patients: a questionnaire study. Clin Otolaryngol 1992; 17:231-6.
12. Yardley L, Luxon LM, Haacke NP. A longitudinal study of symptoms, anxiety and subjective well-being in patients with vertigo. Clin Otolaryngol 1994; 19:109-16.
13. Yardley L. Overview of psychologic effects of chronic dizziness and balance disorders. Otolaryngol Clin North Am 2000; 33(3):603-16.
14. Sloane PD, Hartman M, Mitchell CM. Psychological factors associated with chronic dizziness in patients aged 60 and older. J Am Geriatr Soc 1994; 42(8):847-52.
15. McKenna L, Hallam RS, Hinchcliffe R.The prevalence of psychological disturbance in neuro-otology outpatients. Clin Otolaryngol 1991; 16:452-6.
16. Jacobson GP, Newman CW. The development of the Dizziness Handicap Inventory. Arch Otolaryngol Head Neck Surg 1990; 116:424-7.
17. Cohen H, Kimball KT. Development of the vestibular disorders activities of daily living scale. Arch Otolaryngol Head Neck Surg 2000; 126:881-7.
18. Mangabeira-Albernaz PL, Ganança MM, Caovilla HH, Ito YL, Novo NF, Juliano Y. Aspectos clínicos e terapêuticos das vertigens. Acta Awho 1986; 2(5):49-109.
19. Davis H, Silvermann RS. Hearing and deafness. New York: Holt, Rinehart & Winston; 1970.
20. Jerger J. Clinical experience with impedance audiometry. Arch Otolaryng 1970; 92:311.
21. Ganança MM, Caovilla HH. Labirintopatias. Acta AWHO 1991; 10(1):4-16.
22. Ganança MM, Caovilla HH, Munhoz MSL, Munhoz ML, Ganança FF. Tratamento da vertigem na criança. Pediatr Mod 1997; 33:7-19.
23. Campos CAH. Principais quadros clínicos no adulto e no idoso. Em: Ganança MM, editor. Vertigem tem cura? São Paulo: Lemos Editorial; 1998. p.49-57.
24. Telian SA, Shepard NT, Smith-Wheelock M, Kemink JL. Habituation therapy for chronic vestibular dysfunction: preliminar results. Otolaryngol Head Neck Surg 1990; 103:89-105.
25. Bamiou DE, Davies RA, McKee M, Luxon LM. Symptoms, disability and handicap in unilateral peripheral vestibular disorders. Scand Audiol 2000; 29(4):238-44.
26. Handa PR, Kuhn AM, Cunha F, Schaffleln R, Ganança FF. Qualidade de vida em pacientes com vertigem posicional paroxística benigna e/ou doença de Ménière. Rev Bras Otorrinolaringol 2005; 71(6):776-83.
27. Baguley DM, Andersson G. Factor analysis of the Tinnitus Handicap Inventory. Am J Audiol 2003; 12(1):31-4.
28. Ribeiro PJ, Iório MCM, Fukuda Y. Tipos de zumbido e sua influência na vida do paciente: estudo em uma população ambulatorial. Acta Awho 2000; 19(3):125-35.
29. Yardley L, Masson E, Verschuur C, Haacke N, Luxon L. Symptoms, anxiety and handicap in dizzy patiens: development of the Vertigo Symptom Scale. J Psychossom Res 1992; 36:731-41.
30. Ganança FF, Castro AS, Branco FC, Natour J. Interferência da tontura na qualidade de vida de pacientes com síndrome vestibular periférica. Rev Bras Otorrinolaringol 2004; 70(1):94-101.
1. Specialist degree (Speech Doctor graduated at PUC-SP, specialist on Audiology graduated at IEAA responsible for the Otoneurology and Audiology department of the PROMUR Institute)
2. PhD (Assistant Professor at Faculdade de Fonoaudiologia da PUC-SP (Speech Therapy College) and professor at IEAA.
3. PhD (Doctor on Human Communication Disorders and titular professor at the Speech Therapy College of PUC-SP)
4. Medical Residence (Third Year Resident on Otorhinolaryngology at PROMUR Institute)
IEAA - Instituto de Estudos Avançados da Audição
Daniela Affonso Moreira
Address: Rua Aviador Gil Guilherme, 123 Santana São Paulo/SP cep 02012-130 tel/fax: (11) 6221-8524 Email daffmoreira@hotmail.com
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on June 6, 2006 and was approved on September 26, 2006 o7:25:35.