INTRODUCTION Pleomorphic adenoma is the benign neoplasm more commonly found in greater salivary glands, mainly in parotid in 80% of the cases, and only 8% in lower salivary glands (1-4).
The cases that might affect nasal cavity are not very common. Nasal pleomorphic adenoma was first described by Denker and Kahler (1929), an then by Stevenson (1932) and Weidlen (1936) [5]. Since then few cases have been described in the literature.
The target of this study is to report a case of nasal pleomorphic adenoma causing facial deformity in a 16-year-old female patient, due to the uncommon clinical condition observed which needed surgical resection through degloving because of size.
CASE REPORTJ.M.B. 16-year-old female patient, white, went to Serviço de Otorrinolaringologia da Faculdade de Medicina da Universidade Federal de Uberlândia (Otorhinolaryngology Service of Federal Medical School - Minas Gerais, Brasil) complaining of unilateral nasal obstruction to the left and small quantity of epistaxis for about a year. Along months, patient developed facial asymmetry, and went back to ambulatory with an enlargement of the nasal pyramid and bulging on ipsilateral malar area.
Previous rhinoscopy presented a type of reddish, friable aspect mass occupying the whole left nasal fossa and septum deviation blocking all right nasal fossa. CT from paranasal sinus showed a polyp-like lesion with some soft parts in terms of density on left nasal fossa from nostril up to nasopharynx, remodeling and filling left maxillary sinus, with obstruction of ipsilateral ostiomeatal complex. There was erosion of nasal bone septum with deviation to the right (1).
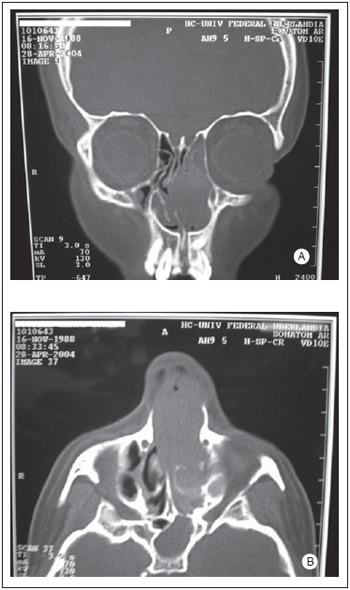
Figure 1. Computerized tomography of breasts paranasais in cuts coronal (A) and axial (B) demonstrating a lesion of aspect polipóide, with soft, located density of parts in left nasal sewage, from the nostril to nasofaringe, remodeling and filling out the maxillary breast to the left, with obstruction of the compound óstio-meatal ipsilateral, erosion of the nasal bone septo and deviation of this for the right.
Patient underwent surgical removal of tumor through degloving, with margin of safety of tumor-free mucosa (2). Its pedicle was in the nasal septum, next to cranium base. Pathological anatomy exam showed an expressive development with poligonal cells of eosinophils cytoplasm and round and oval nuclei disposed in acinus and trabeculae, over a myxoid matrix and diagnosed as pleomorphic adenoma (mixed benign tumor). Patient developed well in post-surgery period.
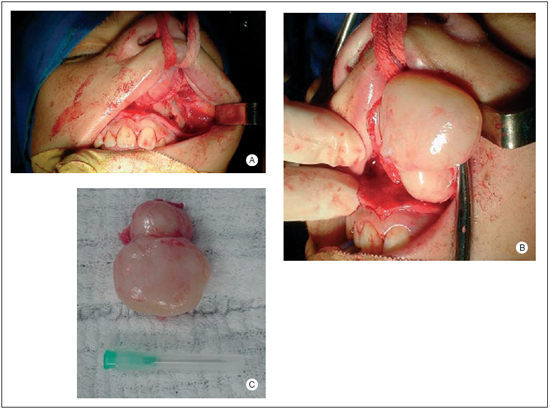
Figure 2. Pictures demonstrating the surgical times of the éxerese of the tumor through medium-facial degloving: (a) Incisions in the furrow gengivo-buccal superior and intercartilaginosa, descolamento subperiosteal of the jawbone and elevation of the scrap; (b) Exérese of the tumor; (c) he/she Asks surgical.
She has been under ambulatory follow-up for 12 months and does not show tumor recurrence, with no complaints or regression from facial deformity.
DISCUSSION Salivary gland tumors are not very common, corresponding about 0.3% from all neoplams, according to cancer records from England and Wales (6). In Brazil, in the period of 1981 and 1985, from the 530,910 reported cases of malignant tumors in all topographies, 1,504 of them presented salivary glands, corresponding to 0.28% (7). About 94% of the salivary gland tumor is epithelial, and parotid gland is its first place from 70 to 80% (4). In this gland, 80% of the tumors is benign, and pleomorphic adenoma prevails, with an incidence ranging from 60.6 a 76.2% (2,8).
According to Spirro and col (1973), 11.8% of the salivary gland tumors are benign and only 1% of tumors can be seen in the nasal cavity (1). The most common place for pleomorphic adenoma in nasal cavity is on four-square cartilage of nasal septum, followed by external nasal wall, mainly in nasal conchas (2). Compagno and Wong examined 40 cases of mixed benign nasal tumor and found that most of theses neoplasms come from mucosa of bone or cartilaginous septum (9). In Brazil, it was described only two cases of pleomorphic adenoma confirmed after histopathological analisis (5,10).
At the present moment, there are different theories for the origin of pleomorphic adenoma in the nasal septum: 1) Jacobson´s organ or vomeronasal organ, a duct with a 6mm-longitude-epithelial covering in the cartilaginous part of the septum, next to nasopalatine opening, which normally disappears in precocious way, therefore it can be permanent in adults (Stevenson, 1932); 2) a second hypothesis is it comes from aberrant cells in the covering epithelium of the nasal septum (Ersner and Saltzaman, 1944); 3) a third one is that it comes from ectopic salivary gland tissue (Evans and Cruicksbank, 1970) (5).
Tumor can arise in any age of life, but it is more frequent in people at their 60s, mainly in women no matter their race (9). Patients usually look for a doctor because of unilateral nasal obstruction and/or presence of painful mass in nasal fossa, less common than epistaxis.
Pleomorphic adenoma presents as a polyp-like, flat, lobed, firm and encapsulated mass. Two cellular types need to be present to the pathological anatomy of mixed tumor: one type is epithelial and myoepithelial cells; and the second is a fibroid, myxoid, chondroid, vascular or myxochondroid stroma (6). Image exams, especially CT, determine tumor extension and implication of neighboring structures, explaining the best intervention.
Differential diagnosis should be performed with epithelial papilloma, angioma, transitional cell carcinoma, adenocarcinoma, gliomas, meningiomas and olfactory neuroblastoma and others (10).
In the current case, patient presented repeated epistaxis, a reddish mass in nasal fossa, which seen from CT, endangered all nasal fossa since the sphenopalatine foramen area; this led to a supposition of nasophrynx angiofibroma (even being a female case). As we consider a possible hypothesis, we did not perform pre-surgery biopsy.
Ex-pleomorphic adenoma carcinoma is the most common malignant tumor from the mixed tumor of nasal septum. In that tumor, only the epithelial component changes into malignant and is able to perform metastasis (11).Benign pleomorphic adenoma, which is able to perform metastasis, is another type of malignant tumor. It is rarely found in recurrent tumors in which metastasis occurs with benign histological aspect, though it has such aspect (11). Only two cases in lower salivary glands were described. One by Wermuth et al. in nasal cavity and another by Freeman et al. in nasal septum.
The first treatment choice is surgical removal, which has large margin of safety with tumor-free mucosa. Surgery approach depends on lesion size. If tumor is small, transnasal endoscopy is recommended, though if it is large, it is recommended a resection by lateral rhinotomy or degloving complemented with nasal endoscopy (12). In the current case, we decided for performing degloving due to the large amount of mass, which caused sever facial deformity, and for previous diagnosis indefinition to surgery.
Some diagnoses hipotheses, besides being tumor salivary glands, were also: schwanoma, nasopharyngeal angiofibroma and inverted papilloma, and an ample access, with an ample tumoral resection and margin of safety, was needed. The use of freezing pathological anatomy analysis on perioperative period can be a useful option the best surgery method choice. In the current case, despite CT suggested benign tumor, we considered that freezing biopsy would be valid, though it was not available in our institution. That is why we enlarged the tumor resection margin.
Image exams, especially CT, detemine tumor extension and length of adjacent structure, indicating the best intervention.
Radiotherapy is not so useful for such patients, and it is only recommended in non-resection tumor and in cases of absolute surgical counterindication.
Pleomorphic adenoma reincidence occurs more often in such components in whose histological analysis, large amount of myxoid can be found, what it is rare in nasal localization, opposed to what ocurrs in main gland neoplasms (5). Tumor recurrence is estimated in about 5% of cases after primary removal and about 2 to 3% become malignant, especially in cases of tumoral recurrence.
FINAL CONSIDERATIONSDifferential diagnosis of lesions on nasal fossa and paranasal sinus is not so easy to be done. Definite diagnosis is only achieved after pathological anatomy exam of surgical specimen. Although pleomorphic adenoma in nasal cavity is rare, it is a type of neoplasm which should be part of differential diagnosis of nasal tumors associated to epistaxis and nasal obstruction. An ample surgical access such as degloving to large mass is essential to therapeutical success.
BIBLIOGRAPHY1. Spiro R, Koss L, Hadju S, Strong EW. Tumors of minor salivary origin. A clinicopathologic study of 492 cases. Cancer, 1973, 31:117-29.
2. Eneroth CM. Salivary gland tumors in the parotid gland, submandibular gland and the palate region. Cancer, 1975, 27:1415-1418.
3. Eveson JW, Cawson RA. Salivary gland tumors. A review of 2,410 cases with particular reference to histological types, site, age and sex distribution. J Pathol, 1985, 146:51-58.
4. Spiro RH. Salivary neoplasms: Overview of a 35-year experience with 2,807 patients. Head Neck Surg, 1986, 8:177-184.
5. Felix J, Tonon S, Saddy J, Meirelles R, Felix F. Adenoma pleomórfico do septo nasal: relato de caso e revisão de literatura. Rev Bras Otorrinolaringol, 2000, 66:276-9.
6. Eveson JW. Pathology of salivary gland tumors. In: Malignant tumors of the mouth, jaws and salivary glands: Edward Arnold, 1995.
7. Registro Nacional de patologia tumoral. Diagnósticos de Câncer. Brasil - 1981/1985. Ministério da saúde. Instituto Nacional do Câncer. Coordenação de Programas de Controle de Câncer (Pró-Onco).
8. Rapoport A, Kanda JL, Kowalski LP, Sobrinho JA, Carvalho MB, Fava AS. Tumores benignos da glândula parótida. Estudo de 90 casos. Rev Bras Cir Cab Pesc, 1983, 7:205-227.
9. Compagno J, Wong RT. Intranasal mixed tumors. Am J Clin Pathol, 1977, 68.213-18.
10. Rocha MP, Campagnolo AM, Macedo VS, Scarton FB, Rocha HP, Kuhl G. Adenoma pleomórfico de septo nasal: relato de caso. Rev Bras Otorrinolaringol, 2004, 70(3):416-418.
11. Freeman SB, Kennedy KS, Parker GS, Tatum AS. Metastasizing pleomorphic adenoma of the nasal septum. Arch Otolaryngol Head Neck Surg, 1990, 116:1331-1333.
12. Berenholz L, Kessler A, Segal S. Massive pleomorphic adenoma of the maxillary sinus. Int J Oral Maxillofac Surg, 1998, 27:372-373.
1. Graduation student from Medical School - PUCCAMPINAS.
2. Titled Professor - Head of Otorhinolaryngology Service of Faculdade de Medicina da Universidade Federal de Uberlândia (Federal Medical School).
3. Resident Doctor of Otorhinolaryngology Service of Faculdade de Medicina da Universidade Federal de Uberlândia (Federal Medical School).
Serviço de Otorrinolaringologia da Faculdade de Medicina da Universidade Federal de Uberlândia, Uberlândia, Minas Gerais, Brasil (Otorhinolaryngology Service of Federal Medical School).
Lucas Gomes Patrocínio Rua XV de Novembro, 327 / 1600 Uberlândia - MG.
CEP: 38.400-214 Phone / Fax: (34) 3215-1143.
E-mail: lucaspatrocinio@triang.com.br
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on September 29, 2005 and was approved on January 18, 2006 22:30:22.