INTRODUCTIONTinnitus is an endogenous sonorous sensation, or rather, it is any sound perceived by the individual without the existence of an external acoustic stimulation (1,2). Its estimated prevalence ranges from 10% to 17% of the world-wide population (3,4) and attacks about one third of North Americans older than 55 (2). In Brazil, one believes that more than 28 million individuals are patients with tinnitus, which makes it a public health problem.
Despite the recent advances in specific literature, the physiopathology of tinnitus has not been completely elucidated, which makes it a great challenge for the scientific community. However, even with such difficulties, it is of utmost importance to understand the generation, detention and perception cascade of events of tinnitus better, aiming at investigating and controlling the specific causes found in each patient.
The causes of tinnitus are not always eminently otological. In fact, its genesis can be influenced by neurological, metabolic, pharmacologic, vascular, muscular, odontologic and even psychic factors (6-8). Moreover, it is not rare to find the manifestation of one of the causes in the same individual (7).
The myofascial trigger-points (MTPS) are small located hypersensitive areas in palpable tense muscular flanks in the muscle-skeletal that, spontaneously or under mechanical stimulation, initiate local and referred pain in distant or adjacent areas (9).
The MTPS are considered active when their stimulation generates referred pain that reproduces the preexisting painful complaint of the patient (9,10). They are often found in the postural muscles of the cervical region, in the scapular waist, pelvic and masticatory musculature where they cause spontaneous pain or to the movement (9,11). On the other hand, the latent MTPS are located in symptomless areas and they only cause referred and local pain when stimulated (9,11). However, they are less painful to palpation and much more frequently found in the population in general (11).
MTPS are detected in patients with painful myofascial syndrome who usually complain of tinnitus. Our previous experience with patients diagnosed with myofascial pain in parts of the head and neck have given us some reasons to suspect of a possible interaction between the MTPS and tinnitus: the palpation of MTPS caused temporary modulation of tinnitus in some patients and during deactivation treatment of these points there was a reduction and even the disappearance of tinnitus.
So far, literature is quite deficient in relation to the possible influence of the MTPS in the generation or perpetuation of tinnitus. Thus, innumerable questionings still need to be answered.
The objectives of this study were to investigate a possible association between:
1) tinnitus and the presence of MTP;
2) the ear with worse tinnitus and the side of the body searched with larger number of MTPS;
3) the presence of MTP and its capacity to modulate tinnitus.
MATERIAL AND METHODS This study was approved by the Commission for Analysis of Research Projects of Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (CAPPesq), under the protocol number 774/02, and delineated as a case-control study.
1. Group of cases (G1) There was the inclusion of 94 patients with complaint of constant tinnitus (uni or bilateral), for at least three months, of any gender, race or age range and who had been consecutively taken care by the Research Group on Tinnitus of the Division of ENT Clinic of the HCFMUSP. The data collection of the sample happened between the months of August of 2002 and August of 2004 and the exclusion criteria involved patients with (1) complaint of pain having involved three or more quadrants of the body, regardless of the cause; (2) infiltration with local anesthetic and/or specific deactivation treatment of the MTPS in the last 6 months; (3) medicine use for the treatment of pain; (4) Impossibility to understand the supplied orientations and/or to give information on the effect of the MTPS palpation in tinnitus; (5) Absence of tinnitus perception at the moment of the evaluation and (6) pulsatile or myoclonic tinnitus.
The selected individuals were submitted to a specific evaluation, by the same researcher, in a quiet environment in order to facilitate the perception of the modulation of tinnitus. Initially patients were questioned about localization of tinnitus (investigating the worse side in the bilateral cases) and the time of complaint.
The evaluation of tinnitus intensity was investigated before and only during the examination of palpation of the MTPS when there was a modulation of the symptom, by means of a numerical scale of which variation ranged from 0 (tinnitus absence) to 10 (the worst imaginable tinnitus). One considered as modulation the increase or immediate decrease of at least one point in the scale and/or change in the type of sound of tinnitus. During evaluation one investigated the presence or not of frequent regional pain for at least three months (chronic pain) in parts of the head, neck and scapular waist, as well as the symptom time, of which localization was registered in a corporal diagram by the individual him/herself.
The diagnosis criteria for the active and latent MTPS were: presence of a flunk of palpable muscular tension with hypersensitive point to palpation along this flunk, as well as a sensitive abnormality or referred pain at distance by the examined and standardized MTP for each muscle. For the active MTPS, this referred pain must correspond to the complaint of preexisting pain of the individual. The hypersensitivity of the MTPS was confirmed by the jump sign demonstrated by the patient, which can be revealed by facial expressions, as grimaces, verbal answers which signal pain or by movement of corporal escape. In this research, the located contracted reply (twitch response) of the MTPS it was not necessary condition for the outcome of the diagnosis. This visible muscular contraction is observed, mainly, during the stimulation with needle in the MTPS (9).
Initially transverse palpation to muscular fibers was performed, in search of the tense band and the hypersensitive nodule. The palpation of the MTPS was performed only once in each muscle, in the same portion, through distal part of the indicating finger or in "clamp" (indicating and thumb). A pressure supported in the MTPS was kept by up to 10 seconds. Nine muscles were researched in bilateral manner in the areas of head, neck scapular waist, in accordance with the described criteria by Travell & Simons (9): infra-spinal (in the two third medial of nasal cavity infra-spinal of the scapula), elevator muscle of scapula (above of the superior angle), superior trapezius, splenius of the head (region of the mastoid process), medium scalene, sternal division of the sternocleidomastoid, posterior digastric, superficial and temporal masseter.
During the digital pressure of the MTPS in each muscle, the following questionings were performed after being detected the palpable muscular tense band and the hypersensitive point: (a) "Do you notice any different sensation in another area of the body beyond the place I am pressuring?" If the answer was "not", the next muscle would be touched. If answer was affirmative and the individual did not present pain complaint, the MTPS would be considered latent. In the cases of presence of pain complaint, the following questions were asked: (b) "Is this sensation accurately the pain complaint you had before?" If answer was "yes", the MTPS was considered active. Finally, for patients who answered "yes" for the questions "A", the examiner would ask the following: (c) "Does tinnitus you feel changed intensity or type of sound?" If the answer was affirmative, the numerical scale from 0 to 10 would be applied for the new intensity and/or the new type of sound would be registered.
2. Group has controlled (G2) It had been enclosed 94 citizens without tinnitus, paired in gender and age with the group of the cases. The exclusion criteria had been the same ones adopted previously for the other group, except the ones of number 5 and 6. In the initial evaluation they had only been enclosed questions to about the complaints of chronic pain, in the same areas questioned for the previous group. During the examination of palpation of the MTPS, only question "C" was not carried through.
3. Analysis statisticsIn the statistical analysis for each parameter had been used the tests of Qui-square, Qui-square of McNemar, Student´s t-test, the Kappa value and the calculation of the reason of odds (RE) with its respective reliable interval (IC 95%). It was admitted level of significance statistics p> 0.05, as recommended for biological tests.
RESULTS From the 94 citizens evaluated in each group, 55 (58%) were female and 39 (41%) were male (p = 1,00, Qui-square test). In the G1, ages had varied from 29 to 84 years (average = 53 years) and from 29 to 80 years (average = 52,6 years) in the G2 (p = 0,82, Student´s t-test). The time of tinnitus in the G1 varied from 3 months to 40 years (average = 6.0 years) and half of the patients presented the symptom for three years.
The discomfort of tinnitus reported by patients, at the moment of the evaluation, by means of the numerical scale varied from 0 to 10 (right ear: average = 6.7; left ear: average = 7.0) and 49 (52%) patients had presented bilateral tinnitus. From these, 21 (42%) reported feeling greater discomfort to the left. Thirty-one patients with tinnitus (33%) presented chronic complaint of pain in the evaluated areas, with from 6 months to 30 years (average = 4.6 years).
1. Association between tinnitus and MTPSThe MTPS had been detected in at least one muscle in 68 (72.3%) patients from G1 and in only 34 (36.2%) ones from G2. Thus, patients with tinnitus complaint presented greater risk of MTPS (RE = 4.87; CR 95%: from 2.50 to 9.53; p< 0.001 corresponding QUI-squared test).
2. Association between the ear with tinnitus (or ear with worse tinnitus) and the side of the body researched with larger number of MTPSIn G1 it was observed an agreement of laterality of 56.5% (Kappa = 0.29; p< 0.001) between affected ear by tinnitus (or ear with worse tinnitus on bilateral cases) and side of the body evaluated with greater presence of MTPS (Table 1).
3. Modulation of tinnitus by means of compression of MTPSThe modulation of tinnitus during the digital compression of the MTPS occurred in 38 (55.9%) out of 68 from G1. From these, it was observed that a total of 136 MTPS presented capacity of modulate symptom. 30 of them (22.1%) were active and 106 (77.9%) were latent.
The change in the intensity of tinnitus was what more represented the modulation of the symptom by patients. However, the alteration in type of sound also was reported in some cases (Picture 1).
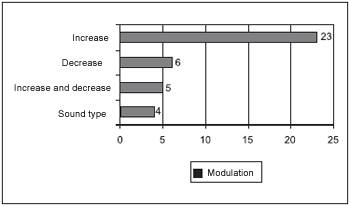
Picture 1 - Distribution of patients from G1 regarding modulation of the intensity and the type of tinnitus sound during the digital compression of the MTPS (n = 38).
The modulation of tinnitus was observed in all the muscles researched during digital pressure of MTPS. However, the main muscle with MTPS that modulated tinnitus was the masseter one, followed by splenius of the head, the sternocleidomastoid and the temporal one (Picture 2).
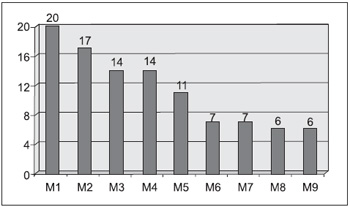
Picture 2 - Distribution of patients with modulation of tinnitus regarding the localization of the examined MTPS (n = 38). - M1- masseter, M2- splenius of head, M3- sternocleidomastoid, M4- temporal, M5- trapezius, M6- digastric, M7- scalene, M8- elevator muscle of scapula, M9- infra-spinal.
Amongst the 38 patients who modulated tinnitus, 25 (65.7%) were female and 22 (58%) presented bilateral tinnitus. It was also observed that 21 (55.3%) of them complained of pain in the evaluated areas. The age of these patients varied from 34 to 78 (average = 52.2) years and period of tinnitus of these patients varied from 3 months to 33 years (average = 4.9)
Comparing the 38 patients from G1 with MTPS that modulated tinnitus and the 30 patients who did not modulate it, there was no statistical significant difference regarding gender, age or localization of tinnitus. Yet, pain complaint was presented as a strong condition to modular patient. Tinnitus during the palpation supported in MTPS (p = 0.008, Qui-square test).
3.3. Modulation of the ipsilateral and contralateral tinnitus to the examined TPsFrom the 136 MTPS that caused modulation of tinnitus, 77.9% was ipsilateral to the ear with tinnitus that modulated and 22.1% were contralateral. But a MTPs located in the sternocleidomastoid muscle modulated a bilateral tinnitus at the same time.
Considering each muscle regarding the agreement between MTPS and tinnitus that modulated, the results show that the six out of nine muscles presented statistical significant responses regarding ipsilaterally (Table 2).
DISCUSSIONThere are evidences that the active MTPS and latent associates to the myofascial painful syndrome are common condition in diverse clinical specialties (12,13). The research that was developed in the Group of Research in Tinnitus showed that this ENT symptom also presents one strong association with the presence of MTPS in the areas of head, neck and scapular waist. The surprising prevalence of MTPS in 72.3% from 94 patients with tinnitus became even more considerable when it was observed the possibility of a patient with tinnitus presenting MTPS is almost five times greater than one a symptomless individual, in accordance with the calculation of odds ratio. Eriksson et al. (14) also also report statistical significant difference in relation to the presence of MTPS when comparing individuals with and without tinnitus. Fricton et al. (15) observed that 42.1% of patients with painful myofascial syndrome in the areas of head and neck also complain of tinnitus. This association is also verified in publications that use deactivation of the MTPS, through infiltration with anesthesic, for tinnitus therapy and its consequent improvement (16,17).
An important contribution for the understanding of the physiopathological mechanisms of tinnitus appears with the publication of the neurophysiological model by Pawel Jastreboff in 1990 (18). According to this author, some neuronal systems are involved in the perception of tinnitus clinically important, including peripheral and central hearing pathways and central, with expressive participation of the limbic and independent nervous systems. In other words, the perception of tinnitus can be activated in greater or lesser degree depending on the participation of other structures of the central nervous system not belonging to the hearing pathway.
One of the features of the MTPS is the presence of autonomic reactions related to distance of its place of origin (19), what stresses the similarity with tinnitus by neurophysiological model. According to Estola-Partanen (20), it is possible that tinnitus that improves with the infiltration of the MTPS is also mediated by the independent nervous system, justifying its improvement or annulment when the influence of this system in the hearing pathway is changed. This author also says that the improvement of tinnitus after infiltrations of the MTPS can be justified by the blockade of the pathways that lead tinnitus of the ear up to the hearing cortex, where it is perceived, although infiltration does not to act in the origin of tinnitus.
Another finding which would support the hypothesis of the influence of the MTPS as an etiological or coadjuvant factor of tinnitus is the correlation of laterality of 56.5% (p< 0.001) between the ear with tinnitus (or the ear with worse tinnitus) and the side of the body with more MTPs, especially in symptomless individuals of intensity between the two ears, followed by pain complaint.
In Estola-Partanen (20) it is also possible to observe a statistical significant result (p< 0.0001) regarding the side of body with more muscle tension - related with the presence of MTPS in the cervical muscles and the scapular waist - that is in ipsilateral manner besides tinnitus complaint. Bjorne (21), in 1993, evaluates 39 individuals with tinnitus, from which 29 with unilateral complaint present hypersensitive points in the lateral pterigoyd muscle, what coincides with the side of the ear with tinnitus. Travell (16) and Wyant (17) also report that the MTPS related with tinnitus are located ipsilaterally to the symptom. Hülse (22), in 1994, reports the existence of a connection between the proprioceptive and nociceptive afferents of the cervical area and the cochlear nucleus, what could justify, in the cases of muscular tension, the ipsilateral correlation with tinnitus. Levine (23), in 1999, suggests that somatic stimuli can encourage the ipsilateral cochlear nucleus, generating an exciting neuronal activity in the hearing path ways that result in tinnitus. According to Wright and Ryugo (24), the dorsal medular nucleus, formed by cuneiform and gracile nucleus, occupies a position in the somatosensory system similar to the one of the cochlear nucleus in the hearing system, receiving information straight from the dorsal root that receives information from the proprioceptive, touchable and vibratory receptors of the corporal surface. Thus, the lateral cuneiform nucleus is the arriving point of afferent fibers of the neck, the ear and the suboccipital muscles, that supply information on the position of head and external hearing necessary to the processing of acoustic information (24).
One of the most interesting findings of this research was the development of the modulation of tinnitus in 55.9% of the asymptomatic patients, occurring more frequently in ipsilateral manner in six out of nine evaluated muscles. This phenomenon of tinnitus modulation is mentioned by Levine (23) and Sanchez et al. (25), who used another type of methodology, where patients with and without tinnitus are submitted to isometric contraction maneuvers of muscles of head, neck and member area. In other studies, the modulation of tinnitus also is observed through electric stimulation of the medium nerve and voluntary movements of the ocular deviation (26,27).
Amongst the patients who presented modulation of tinnitus, 65% reported temporary worsening, while others affirmed that there was a reduction or change in the type of sound. These results are also observed by Levine (23) and Sanchez et al. (25). The increase of tinnitus can be explained by the experimental description of a great projection of the cuneiform nucleus over cochlear nucleus, with numerous rich terminations in glutamate, an exciting neurotransmitter (24). In this way, the aberrant neuronal activity in the hearing pathways of the patients with tinnitus can become aggravated by the exciting stimulation of the gracile and cuneiform nucleus over the dorsal cochlear nucleus, what justifies the increase of tinnitus as the most common effect in the patients who present some type of modulation (24).
The presence of chronic pain complaint in the examined areas was the only observed significant feature when compared the group with tinnitus modulation and the group without it. When analyzing the similarities between tinnitus and chronic pain, we observe that both are subjective sensations, they present diverse causes, they can be influenced by the central nervous system and suffer modulation in its intensity or its features along time. Its adequate control depends on a multiprofessional and individualized therapeutical approach. The psychological component that follows it supports the hypothesis that other cerebral areas are not directly responsible for the sensorial perception (limbic and independent systems) also are involved (28). Moreover, the anatomical localization of the neural structures that generate chronic pain and tinnitus differs from the structures to where these symptoms are related (29). Another similarity is that the hearing and somatosensory systems present an efferent fiber net well developed that seems to exercise some type of control over the afferent activity (28). Agreeing with these similarities, Isaacson et al. (30), in 2003, observe that 54.2% of 72 patients with chronic pain also present tinnitus.
The MTPS capable to produce modulation of tinnitus had been identified as active or latent to serve as a guide in clinic exercise and as tool for future therapeutical strategies. Initially it was believed that only the active MTPS would be able to modulate tinnitus due to its degree of activity and its capacity to reproduce previous painful sensation of patient when touched. However, the latent MTPS also modulated tinnitus, suggesting that they are able to cause an excitement and expressive sensitization of the involved structures in the detention and processing of the muscular nociceptive stimulaton; what would produce, during palpation, a zone of reference with intensity and extension enough to modulate tinnitus. Perhaps this occurs especially in the cases in which latent MTPS remain in the individual during lengthening period of time. The works by Travell and Simons (9) and Eriksson et al. (14) do not describe the type of TP that produces tinnitus in an asymptomatic individual or that it modulates tinnitus of a patient from the compression of a MTPS in the sternocleidomastoid muscle, what makes comparison of current study findings difficult.
The muscular localization of the MTPS that modulated tinnitus more frequently is similar to affirmation by Travell (16) and Travell and Simons (9), who relate tinnitus with the presence of MTPS in the masseter muscle, although these authors did not study the phenomenon of modulation. The MTPS located in the muscles of the head and neck produced more modulation of tinnitus than those present in the area of scapular waist, what remind the findings by Levine (23) and Sanchez et al. (25), in which contraction maneuvers of the muscles of head and neck produce more modulation of tinnitus than those performed by the superior and inferior members. These results can be explained by means of the neuroanatomy, where connections between the somatic and hearing pathways in the cephalic level are much richer.
Finally, considering that tinnitus can present more than one cause in a single patient, the possible function that the MTPS and the somatosensory system could develop in the origin or persistence of the tinnitus perception can not be left apart.
CONCLUSIONSThe MTPS were surprisingly common in patients with tinnitus, when compared with a control group, and caused a high rate of temporary modulation of the symptom during its digital palpation. The high agreement of laterality between tinnitus the ear with worse tinnitus and the side of the body examined with larger presence of MTPS fortifies the hypothesis that the somatosensory system can influence the hearing pathway. Future clinical assays that analyze the effect of the treatment of deactivation of the MTPS on tinnitus will be able to strengthen these findings, as well as clarifying if its presence in patients with tinnitus is an etiological and/or coadjuvant factor the symptom.
REFERENCES1. Jastreboff PJ, Sasaki CT. An animal model of tinnitus: a decade of development. Am J Otol 1994, 15:9-11.
2. Lockwood AH, Salvi RJ, Burkard RF, Galantowicz PJ, Coad ML, Wack DS. Neuroanatomy of tinnitus. Scand Audiol 1999, 28:47-52.
3. McKee GJ, Stephens SDG. An investigation of normally hearing subjects with tinnitus. Audiology 1992, 31:313-17.
4. Attias J, Urbach D, Gold S, Shemesh Z. Auditory event related potencials in chronic tinnitus patients with noise induced hearing loss. Hear Res 1993, 73:106-13.
5. Sanchez TG, Knobel KA, Ferrari GMS, Batezati SC, Bento RF. Grupo de apoio a pessoas com zumbido (GAPZ): metodologia, resultados e propostas futuras. Arq Otorrinolaring 2002, 6:278-84.
6. Moller AR. Pathophysiology of tinnitus. Ann Otol Rhinol Laryngol 1984, 93:39-44.
7. Sanchez TG, Levy CPD, Medeiros IRT, Ramalho JRO, Bento, RF. Zumbido em pacientes com audiometria normal: caracterização clínica e repercussões. Rev Bras de Otorrinolaringol 2005, 71:427-31.
8. Camparis CM, Formigoni G, Teixeira MJ, De Siqueira JTT. Clinical evaluation of tinnitus in patients with sleep bruxism: prevalence and characteristics. J Oral Rehabil 2005, 32:808-14.
9. Travell J, Simons DG. Myofascial pain and dysfunction: The trigger point manual, upper half of body. ed 2. Baltimore: Williams & Wilkins; 1999.
10. Aronoff GM. Myofascial pain syndrome and fibromyalgia: a critical assessment and alternate view. Clin J Pain 1998, 14:74-8.
11. Bonica JJ. Management of myofascial pain syndrome in general practice. JAMA 1957, 164:732-38.
12. Nielsen AJ. Case study: myofascial pain of the posterior shoulder relieved by spray and stretc. J Orthop Sports Phys Ther 1981, 3:21-6.
13. Rubin D. Myofascial trigger point syndromes: an approach to management. Arch Phys Med Rehabil 1981, 62:107-14.
14. Eriksson M, Gustafsson S, Axelsson A. Tinnitus and trigger points: a randomized cross-over study. In: Reich GE, Vernon JA (eds): Proceedings of the Fifth International Tinnitus Seminar. Portland; 1995, pp.81-3.
15. Fricton JR, Kroening R, Haley D, Siegert R. Myofascial pain syndrome of the head and neck: a review of clinical characteristics of 164 patients. Oral Surg 1985, 60:615-23.
16. Travell J. Temporomandibular joint pain referred from muscle of the head and neck. J Prosthet Dent 1960, 10:745-63.
17. Wyant GM. Chronic pain syndrome and their treatment II. Trigger points. Canad Anaesth Soc J 1979, 26:216-19.
18. Jastreboff PJ. Phantom auditory perception (tinnitus): mechanisms of generation and perception. Neurosci Res 1990, 8:221-54.
19. Travell J, Bigelow NH. Referred somatic pain does not follow a simple "segmental" pattern. Fed Proc 1946, 5:106.
20. Estola-Partanen M. Muscular tension and tinnitus: an experimental trial of trigger point injections on tinnitus. Tampere, 2000 (Dissertation - University of Tampere).
21. Bjorne A. Tinnitus aereum as an effect of increased tension in the lateral pterygoid muscle. Otolaryngol Head and Neck Surg 1993, 109:969.
22. Hülse M. Cervicogenic hearing loss. HNO 1994, 42:604-13.
23. Levine RA. Somatic modulation appears to be fundamental attribute of tinnitus. In: Hazell JPW (ed.): Proceedings of the Sixth International Tinnitus Seminar. Cambridge; 1999, pp.193-6.
24. Wright DD, Ryugo DK. Mossy fiber projections from the cuneate nucleus to the cochlear nucleus in the rat. J Comp Neurol 1996, 365:159-72.
25. Sanchez TG, Guerra GCY, Lorenzi MC, Brandão AL, Bento RF. The influence of voluntary muscle contractions upon the onset and modulation of tinnitus. Audiol Neurootol 2002, 7:370-5.
26. Moller AR, Moller MB, Yokota M. Some forms of tinnitus may involve the extralemniscal auditory pathway. Laryngolscope 1992, 102:1165-71.
27. Cacace AT. Expanding the biological basis of tinnitus: crossmodal origins and the role of neuroplasticity. Hear Res 2003, 175:112-32.
28. Moller AR. Similarities between chronic pain and tinnitus. Am J Otol 1997, 18:577-85.
29. Moller AR. Similarities between severe tinnitus and chronic pain. J Am Acad Audiol 2000, 11:115-25.
30. Isaacson JE, Moyer MT, Schuler HG, Blackall GF. Clinical associations between tinnitus and chronic pain. Otolaryngol Head Neck Surg 2003, 128:706-10.
1. Master (researcher Physiotherapist of the ENT and dentistry department of HCFMUSP)
2. Teacher (Associated teacher of ENT Discipline at FMUSP)
3. PhD (Buco-maxillary-facial surgeon at HCFMUSP)
Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo.
Address: Rua Capote Valente, 439 / cj. 34, Pinheiros, São Paulo - SP, 05409-001 Phone.: (11) 3442-5103 E-mail: carinafisiohc@hotmail.com
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on August 29, 2006 and was approved on September 2, 2006 10:14:43.