INTRODUCTION The presence of foreign bodies (FB) in nasal fossas is one of the most common causes of emergency/urgency doctor visiting in ENT area, occurring from 9 to 15% of the total specialized services and more frequent regarding children specially unilateral ones (1,2).
The cases of nasal FB often cause symptoms such as sneezing, coryza and nasal blockage that develop to unilateral purulent and fetid rhinorrhea and are more excessive as longer as the permanence period in nasal fossas (1).
These FB can be introduced spontaneously or by accident, the former is more common in children or patients with psychiatric disorders, and the latter in adults (1,3). The FB can inanimate or not; in the second case, they are mainly insects. From these, the most associated ones to complications are myiasis that cause suppuration and ample destruction of the nasal mucosa, leading to turbinate and septal cartilage necrosis, extension to paranasal cavities, orbit and CNS (3,4).
The size and shape of the FB can determine the difficulty in its removal, what can cause epistaxis, more rarely septal perforation, rhinosinusitis and bronchoaspiration of it (5). The great potential for complications during the removal of these foreign bodies makes the performance of the ENT doctors important in this procedure. The success of the removal of FB depends on the cooperation of the patient, on the ability of the doctor in visualizing the FB, on the type of the FB, the previous manipulation and the available equipment (1).
In this way, it was made a revision of the cases at the urgency service of a hospital. It was observed some features as type of the FB, time of development, symptoms, attempt of removal by a not specialized team and other data that were considered important in order to make a global view of this type of attendance possible.
MATERIAL AND METHODS 54 patient's records of were retrospectively examined from January, 2003 to December, 2004.
These patients were assisted at the Emergency room of Faculdade de Medicine de Marília. They were suspected of foreign body in the nose. Such patients were submitted to ENT evaluation, performed through previous nasal rhinoscopy with nasal speculum and with no use of topical drugs. The initial clinical evaluation and the procedure of removing the FB were performed, when necessary, by the resident doctors under supervision of teachers of the ENT service of the institution.
When reviewing patient's record, it was filled in a form in which it was possible to know: age, gender, place and origin of the FB, associated symptoms, time of development, complications, attempt of removing the FB by other professionals, instrument used and place of the removal of the FB (clinic or ER).
Data were analyzed in descriptive manner and this study was approved by the Ethic Medical Committee of the institution under protocol n°228/06. Moreover, it was done a bibliography survey of the searched subject.
RESULTS 54 cases of foreign bodies in nasal fossa were studied. From those, 10 complaints occurred, in which no foreign bodies to the physical and specialized exam were found. The majority of these cases were revised using nasofibroscopy and in none of them the FB was found. The statistic data came from a total of 44 patients who had FB in nasal fossa.
When evaluating the distribution of the cases regarding age of patients, there was an absolute concentration on those less than five years, only one case of a seven-year-old patient. It had 21 cases of patients with age between 0 and 2 years (47.72%), 20 cases between 2 and 4 years (45.45%), 2 cases between 4 and 6 years (4.54%), and 1 case with more than six years (2.28%).
In 30 cases (68.18%) the removal of the foreign body was performed at the ER, and 14 patients (31.82%) in the clinic. The instrument used for removing it was the Itard's probing tube. It was not necessary sedation or anesthesia for the removal process in none of the patients.
21 cases (47.72%) presented foreign body in the right nasal fossa, 21 cases (47.72%) in the left nasal fossa and 1 case (2.28%) was bilateral and 1 was not specified.
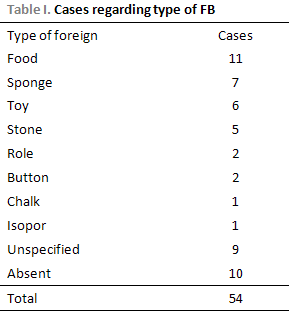
It was observed a great variety of foreign body. The most frequent ones were: foods (mainly grains) in 11 cases (25%), foam pieces in 7 cases (15.9%), and parts of toys in 6 cases (13.63%). In only 2 cases (4.54 %) fragments of paper were found (Table 1, Picture 1 and 2).
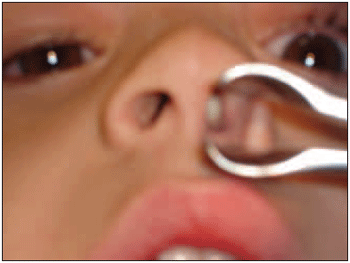
Picture 1. FB in the left nasal fossa nasal (corn grain).
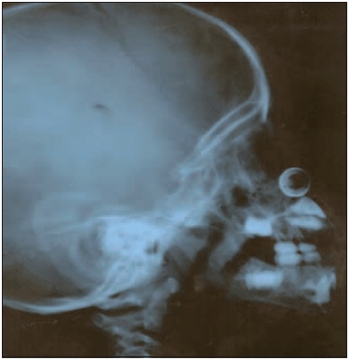
Picture 2. Side simple X-ray (metal object).
Regarding genders, it was observed a great number of occurrences in girls, 24 (54.55%), against 20 boys (45.45%).
According to development time, most of foreign bodies were removed on the first day, in 29 cases (65.9%). 2 cases (4.54%) had their removal on the second day, 1 was removed on the third day (2.28%), 2 on the fourth (4.54%), 1 on the fifth (2.28%), 3 on the seventh one (6.81%) and 2 were removed between the tenth and fourteenth days (4.54%).
It was necessary to perform antibiotic therapy in 8 patients (18.19%), and in 36 cases (81.81%) only the use of physiological serum at 0.9% of nasal topic was prescribed.
The main symptoms were: unilateral rhinorrhea in 20 patients (45.45%) and cacosmia in 6 cases (13.63%). Only in four cases (9.1%) attempts of removal of the foreign body in other not specialized services occurred. It was found epistaxis in 4 patients (9.1%) and rhinosinusitis in 8 patients (18.19%). The removal of no foreign body was not necessary through surgery.
DISCUSSION This study showed that the occurrence of foreign body in the nasal fossa is related with age, but disappearing as child goes older. Intense concentration was observed in the ages from 0 to 2 and 2 to 4 years, what it is confirmed in literature for several other studies (1,6) (Picture 3).
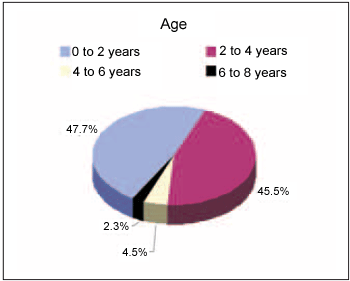
Picture 3. Incidence by age.
It was found in this study a greater prevalence of cases in women (54.55%) against 45.45% in men. These data differ a little from the majority of the found studies, in which the prevalence is greater among boys or there is a balance in the distribution between genders (1,2).
Regarding the side of presentation of the foreign body, predominance was not observed. There was only one case in which foreign bodies were found in the two nostrils.
It was observed great occurrence of foreign bodies from child's meal, or even from not cooked food such as beans and corn. This shows the need of evaluation of the child's environment inside house, though it suggests that the child might not be under proper watching, in dangerous places such as the kitchen. Ikino et al when studying 88 cases of FB in the ear and nose in children suggested that the prevention is the best approach in the cases of foreign bodies and orientation for the family of the possible complications of it (2).
It was also found a great frequency of foam among types of foreign body. In these cases, material is probably taken from pillows, mattresses and sofas. These are the most probable cases when parents do not observe the moment of the installation of the foreign body and also where the most symptomatic cases might appear due to the time of development (7).
From the obtained data, it was also possible to notice that the development time has great influence on symptom. The majority of cases whose symptom was only local pain, it is where there were few hours of development. In the cases of two or more days of development it was observed other symptoms such as fetid unilateral rhinorrhea. Picture 4.
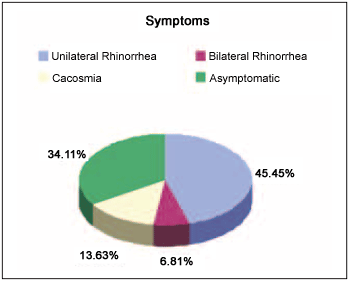
Picture 4. Symptoms.
Regarding complications, twelve cases (27.29%) were observed, 4 of them of epistaxis, equivalent to 9.10% of the total, and presence of rhinossinusitis in 8 patients (18.19%), what in the first cases, bleeding was always in small amount and controlled only with finger nasal compression, and in the last ones it was prescribed antibiotic and local care. These data agree with the ones by Marques et al. where 19.19% of complications during removal was found (6,8).
CONCLUSION In this study, the nose FB was found especially in patients aging from 0 to 2. The main associated symptom was unilateral rhinorrhea. The most found type of FB was food. It was not necessary anesthesia for removing FB in none of the evaluated patients.
The most of cases of nose FB is easily solved with no sequelae, but some can develop serious complications, mainly when there is an attempt of removal by professionals not properly qualified or a lack of suitable instrument. The most feared complication of nose FB, although rare, is the aspiration of it to the inferior air paths, what demonstrates the need of training for removing the nose FB, due to the severity of this occurrence.
REFERENCES1. Tiago RSL, Salgado DC, Corrêa JP, Pio MRB, Lambert EE. Corpo estranho de orelha, nariz e orofaringe: experiência de um hospital terciário. Rev Bras Otorrinolaringol. 2006; 72:177-81.
2. Ikino CMY, D'antonio WEPA, Balbani APS, Sanchez TG, Butugan O. Análise dos atendimentos para retirada de corpos estranhos de ouvido e nariz em crianças. Rev Bras Otorrinolaringol. 1998; 64:379-83.
3. Figueiredo RR, Azevedo AA, Kós AOA, Tomita S. Corpos estranhos de fossas nasais: descrição de tipos e complicações em 420 casos. Rev Bras Otorrinolaringol. 2006; 72:18-23.
4. Figueiredo RR, Dorf S, Couri MS, Azevedo AA, Mossumez F. Corpos estranhos animados em otorrinolaringologia. Rev Bras Otorrinolaringol. 2002; 68:722-9.
5. Sobrinho FPG, Jardim AMB, Sant'Ana IC, Lessa HA. Corpo estranho na nasofaringe: a propósito de um caso. Rev Bras Otorrinolaringol. 2004; 70:120-3.
6. Marques MPC, Sayuri MC, Nogueira MD, Nogueirol RB, Maestri VC. Tratamento de corpos estranhos otorrinolaringológicos: um estudo prospectivo. Rev Bras Otorrinolaringol. 1998; 64:42-7.
7. Endican S, Garap JP, Dubey SP. Ear, nose and throat foreign bodies in melanesian children: an analysis of 1037 cases. Int J Pediatr Otorhinolaryngol. In press 2006.
8. Mackle T, Conlon B. Foreign bodies of the nose and ears in children. Should these be managed in the accident and emergency setting? Int J Pediatr Otorhinolaryngol. 2006; 70:425-8.
1. Resident Doctor of ENT - FAMEMA (R3)
2. Doctor Professor in ENT by FMUSP (Head of ENT Discipline FAMEMA)
3. Master in ENT by FMUSPRP (Assistent Professor of ENT- FAMEMA)
4. Specialist in ENT (Assistant Teacher of ENTFAMEMA)
5. Resident Doctor of ENT - FAMEMA (R2)
6. Resident Doctor of ENT - FAMEMA (R1)
Faculdade de Medicina de Marília
Sávya Cybelle Milhomem Rocha
Address: Rua Hidekichi Nomura,175 Fragata Marília-SP CEP 17519-000 email: dra.savya@bol.com.br - phone: 14 3402 1744
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on June 24, 2006 and was approved on September 26, 2006 07:53:05.