INTRODUCTIONA correct pre-surgical analysis of the patient is essential for a satisfactory result in rhinoplasties(1,2,3). The pre-surgical photographic documentation has become essential in all aesthetic(4) surgeries. Many abnormalities are more evident in good photographs than during the clinical examination. The images allow that the surgeon studies some perspectives simultaneously to define the deformities better. During the surgery, some deformities which had not been perceived before can become evident and also be perceived in pre-surgical photographs. Moreover, the necessity of legal documentation must also be taken in consideration.
The modification of images is a useful form of communication between patient and surgeon; in daily practices, the cases in which the patient presents unreal expectations in relation to the postoperative result are frequent, and in many cases, the potential result of the surgery is limited by individual factors(3,7,8). With the recent use of computer programs capable of modifying images, it became easier to simulate the surgical planning of the patient. According to Sullivan et al, this method still has reluctance in its use due to the cost of the program, the extra time of consultation and the learning of its use(5).
This study aims at evaluating the use of specific computerized program of image for rhinoplasty, through the comparison of the results planned with the program and reached with the surgery, and to correlate with the patient's satisfaction with the surgery.
MATERIALS AND METHODS Between January 2005 and June 2006, all patients (72 cases) submitted to rhinoplasties by the senior author in his private practice were also submitted to the computerized photographic study before the surgery through Alterimage
® (Seattle Design Software, version 3.1). Absence of photographic study, a postoperative assistance smaller than 6 months and previous rhinoplasties (secondary surgery) were exclusion criteria. A total of 46 patients met the criteria of the study. The research was approved by the ethics committee of the institution (number 036/2004) and the patients signed free and clarified consent term before the surgery.
The surgical technique used was individualized for each case. The approaches used were "closed" or "delivery", with or without the use of graft. The "open" technique was not used.
The pre-surgical photographs were taken in 4 incidences: frontal, right and left profile, and basal, according to the norms established by Staffel and Sullivan4,5. The photos were captured by high resolution digital camera. The modifications of the images were made with the interaction of the patient and the final aspect was in common agreement with the surgical possibility, experience of the surgeon and the expectation of the patient. New photographs were taken at least 4 months after the surgery for comparison reasons.
The photos which were modified through the AlterImage® were compared with the post-surgical photos and evaluated by a team of doctors made of 9 members with experience on nasal plastic surgery. Each postoperative result was classified by each evaluator, in relation to the projection of the computerized study before the surgery, into: identical, without comparison, better and worse. The cases in which the photograph did not provide, in the opinion of the evaluator, criteria to make comparative evaluation between two photographs, were considered without comparison. The data were compiled in data bank and analyzed by frequencies according to answers of each evaluator and each patient. The patients were asked on their satisfaction with the postoperative result.
RESULTSAmong the 46 patients, 15 were male and 31 female. The age varied from 17 to 50 years. After obtaining average of the results granted by the 9 examiners, the patients were classified. In 35 cases, the final result was better that the image projected before the surgery (Figure 1). In 10 patients the final result was worse than the projected image. And one case was considered identical. In relation to the total of answers by the evaluator, there were 240 evaluations as better, 95 as worse, 59 as identical and 20 as without comparison.
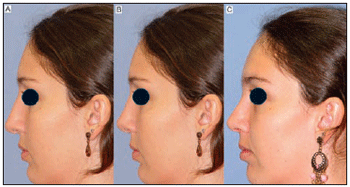
Figure 1. Left profile photographs demonstrating pre-operatory(A), computer photography with planned surgical result (B) one year after the rhinoplasty (C).
The 10 patients had worse results in the postoperative phase in relation to the planning had been submitted to the individual analysis with the presence of the same examiners. In 9 cases, it was considered that the result would have to be reevaluated in 6 or 12 months due to thickness of the skin.
In the subjective evaluation of the satisfaction of the patient, all the patients seemed to be satisfied with the result of the surgery 6 months after it.
DISCUSSIONThe same surgeon performed all the rhinoplasties, and the postoperative results were mostly better than the planning due the experience of the surgeon, considering that according to Fomon and Bells, the surgical imperfections are indirectly proportional to the ability and the knowledge of techniques and anatomy(6).
The program, despite the cost, is easy to use, mainly when the photos are modified in profile, not justifying this characteristic as reason for which many surgeons still do not use this or other similar(9) programs . However, there is a bigger attention time between the doctor and the patient when the modification of the image is carried through, in relation to attentions in which such modification is not carried out(7).
Out of the patients who presented worse results(9), patients could present photos with better results if they had been evaluated later, after complete cicatrization of tissues, for being patients with skin in which edemas take more time to disappear. New photographs will be taken one year after the surgery for a better analysis and comparison.
All patients preferred the postoperative results in relation to the modified images and were considered satisfied with the surgery. This can be explained by the fact that the medical board is more critical and, therefore, the projection, rotation and definition of the tip, and the nose proportion in face(2,6) were better evaluated. Moreover, before the new visual, the patient ends up not accurately observing the previously modified image(7).
According to the senior author's experience, the program was very useful in terms of giving more assurance to the patient, once he/she can more specifically explain his/her expectations and desires to the surgeon, who in turn can demonstrate what could be done according to the patient's expectation, individual anatomy, skin characteristic, age and sex. Other authors reiterate the benefit for both the surgeon and the patient in the use of the computer pre-surgical planning(3,5,9). Certainly, this interaction between patient and surgeon in front of the computer screen makes it easy to understand the patient's expectations in terms of what he/she really wants to have modified in his/her nose(7,8).
In spite of all the advantages, it is evident that no software can substitute the "eye" of the surgeon or his/her technical abilities in recognizing and producing an aesthetic result.
CONCLUSIONAll the patients and most of the doctor team considered the final result better than the planned one. The use of the image modification program is sufficiently useful for both the surgeon and the patient for the surgical programming, fact which is proved by the high subjective satisfaction of the patient.
BIBIOGRAPHY1. Anderson JR, Willet M. On planning before rhinoplasty. Laryngoscope 1984; 94(8): 1115-1116.
2. Colton JJ, Beekhuis BJ. Presurgical analysis for rhinoplasty. Facial Plast Surg 1988;5(2):97-107.
3. Mühlbauer W, Holm C. Computer imaging and surgical reality in aesthetic rhinoplasty. Plast Reconstruct Surg 2005;115(7):2098-104.
4. Staffel JG. Photo documentation in rhinoplasty. Facial Plast Surg 1997;13(4):317-32.
5. Sullivan MJ. Rhinoplasty: planning photo documentation and imaging. Aesthet Plast Surg 2002;26:17.
6. Fomon S, Bell J. Rhinoplasty: New Concepts. Evaluation and Application. Springfield: Charles C. Thomas; 1970.
7. Sharp, HR, Tingay RS, Coman S, Mills V, Roberts DN. Computer imaging and patient satisfaction in rhinoplasty surgery. J Laryngol Otol 2002;116(12):1009-13.
8. Smelt GJ. Dimensional analysis: its role in our preoperative surgical planning of rhinoplasty. Clin Otolaryngol 2005;30(4):379.
9. Tebbets JB. Rinoplastia Primária. A Nova Abordagem Lógica das Técnicas. São Paulo: Di Livros; 2002. p. 585-615.
1. Otorhinolaryngologist (Medical doctor at Faculdade de Medicina da Universidade Federal de Uberlândia)
2. Doctor (Resident at Faculdade de Medicina da Universidade Federal de Uberlândia)
3. Head Professor (Chief otorhinolaryngologist at Faculdade de Medicina da Universidade Federal de Uberlândia)
Otorhinolaryngology Department, Hospital Santa Genoveva, Uberlândia, Minas Gerais, Brasil.
Lucas Gomes Patrocínio - Rua XV de Novembro, 327 / aptº. 1600 - Bairro Centro Uberlândia - MG CEP: 38.400-214 Telephone/Fax: (55) 34 - 215-1143 E-mail: lucaspatrocinio@triang.com.br
This article was submitted to SGP (Sistema de Gestão de Publicações) of R@IO on November 13, 2006 and approved on March 29, 2007 at 03:26:36.