INTRODUCTIONDirectional Preponderance (DP) was firstly defined by Jongkess (1) as a tendency to a greater intensity of nystagmus to a certain direction in comparison to another. According to some researches, DP is more frequent noticed in patients who present spontaneous nystagmus in the same direction (3,4). Thus, patients present caloric responses resulting nystagmus in the same direction as the spontaneous one. On the other hand, they present low responses in the opposite direction to spontaneous nystagmus. The international consensus is that DP would be associated to the vestibular compensation process (4,6). Even after vestibular compensation occurs, some patients present latent nystagmus, which might remain in the opposite direction to the involved side (7).
Others believe that DP would be such pathology of both vestibular systems: central and peripheral ones. Actually, DP has been observed in restricted disorders at the end of vestibular system, ramifications of the 8th cranial nerve, brainstem and cortex (4,5,8,9).
It is also important to mention that DP has also been observed in normal subjects with no evidences of pathology in the vestibular system (3,4,6).
In Brazil, the presence of DP above 33% has been mainly associated to labyrinth disease or irritative syndrome (10), though, an established concept of the latter was not found in the literature.
The target of this study is to describe a case of deficient labyrinth disease whose patient was evaluated through vectoeletronystagmography up to one year after an acute crisis. Also, to discuss the evolution of vestibular compensation on unilateral loss of labyrinth function and the concept of directional preponderance associated to irritative peripheral labyrinth disease.
CASE REPORTA 46-male patient was examined due to a complaint of a sudden vertigo, lasting more than 24 hours, with no hearing complaint. On the clinical exam, it was observed spontaneous horizontal nystagmus to the right side and Romberg to the left.
Hearing test was in normal condition. The image and laboratory propaedeutic established diagnosis of left vestibular neuronitis (Picture 1).
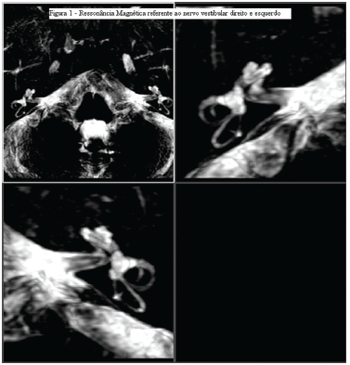
Picture 1. Magnetic resonance imaging of the right and left vestibular nerve.
One month later diagnosis had been done, the first vestibular test was performed. One test was repeated 6 months and one year after the crisis.
Vectoeletronystagmography was a method used to record eye movement. It was used Contronic do Brasil version 5.1, Copyright 1993-2000, - Contronic Sistemas Automáticos da Universidade Católica de Pelotas (Automatic systems of Catholic Universtity - Pelotas). Previously the vectoeletronystagmography exam, its skin was cleaned in order to place the electrodes, and the triangular disposition of those was used, commended by Pansini and Padovan (1969) (11). Vestibular test consisted of the following steps: eye movement calibration, research of spontaneous nystagmus with open eyes, research of spontaneous nystagmus with closed eyes, research of semispontaneous nystagmus, pendular tracking, research of optokinetic nystagmus and research of post-caloric nystagmus (caloric test in water at 44ºC e 33ºC). It was used methods of Jacobson et al to perform and interpret vectoeletronystagmography, considering as normal the values up to 20% and 27% regarding labyrinth and directional preponderance of nystagmus respectively.
When examining oculomotors movement, it was observed saccade with normal latency and speed, 2-kind tracing and symmetrical optokinetic nystagmus.
Regarding caloric test, the results were:
One month later acute crisis: left areflexia and right hyperreflexia, above 70º/sec in 30ºC and 44ºC.
Six months later: LE44ºC=06º/sec, LE30ºC=25º/sec, RE44ºC=24º/sec, RE30ºC=58º/sec, with LP to the right at 45% and DP to the right at 47%.
One year later: LE44ºC=06º/sec, LE30°C=10º/sec, RE44°C=16º/sec, RE30°C=22º/sec, with LP to the right at 41% and PD to the left at 4%.
Patient improvement can be seen on Picture 2 that stands for obtained values in each caloric stimulation and on Picture 3 the obtained values for LP and DP.
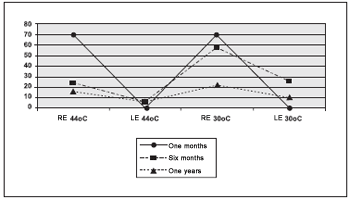
Picture 2. Sequence caloric test.
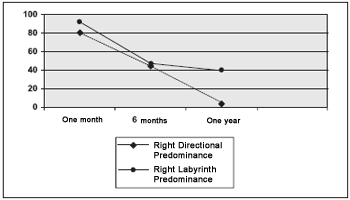
Picture 3. Values of labyrinth predominance and directional preponderance.
Fitzgerald and Hallpike(12) presented the DP phenomenon in their historical article which describe alternated binaural and bithermal caloric tests. The following formula allows calculating the Directional Preponderance:
PD = (OE 44º C + OD 30º C) (OD 44º C + OE 30º C) x 100 OE 44º C + OE 30º C+ OD 44º C + OD 30º C
The values of an expressive DP can vary from hospital to hospital depending on the internal standards. It is considered when there is a difference higher than 26% to 30% (2,10,13) between maximum intensity of Angle Shape Speed Of Slow Component of the nystagmus to the right (LE 44ºC + RE 30ºC) in relation to nystagmus to the left (RE 44ºC+ LE 30ºC) in the caloric test and vice-versa.
The case report describes a classic central compensation in patient who had already had vestibular neuronitis. Left areflexia, one month later the crisis, confirmed the diagnosis. In that moment, hyperreflexia to the right, camouflaging an irritative syndrome, was related to the release of response of the brainstem of the health labyrinth, which occurs at the beginning of vestibular compensation (14). The exam performed after six month present improvement of central compensation.
LP and DP to the right indicate that left labyrinth was under deficient function in relation to the right one and that central compensation was not already established, because there was a LP to the right. The test performed one year later the crisis presents a balanced patient (normal DP), with asymmetric labyrinth function, due to vestibular neuronitis, which led to a partial loss of the left labyrinth, though irreversible.
Thus, one might be sure that DP to the right after one year, under the amount of 81%, refers to liberation of the contralateral vestibular core. After some time, it is possible to observe a decrease of such value, due to a partial vestibular compensation that is completed after one year later the labyrinth crisis, which made the LP remain to the right, indicating a definite lesion on the left labyrinth with a decrease of the function on this side.
CONCLUSIONDP does not define if peripheral labyrinth disease is either irritative or deficient. That is why it is important to consider clinical history and a follow-up of the patient.
DP can be observed in peripheral vestibular lesions, central ones or even in normal patients.
REFERENCES1. Jongkees LB: Caloric test, general considerations. Acta Otorhinolaryngol Belg. 1950; 4(24):376-82.
2.Jacobson GP, Newman CW: Interpretation of caloric testing. In: Jacobson GP, Newman CW, Kartush JM. Handbook of balance function testing. Singular Publishing Group. San Diego. London. 1997.
3. Jongkess LBW: Value of caloric test of the labyrinth. Arch Otolaryngol 1948; 48:402-417.
4. Halmagyi GM; Cremer PD; Anderson J; Murofushi T; Curthoys IS: Isolated directional preponderance of caloric nystagmus: I. Clinical significance. Am J Otol 2000;21(4):559-67.
5 Halmagyi GM; Cremer PD; Anderson J; Murofushi T; Curthoys IS: Isolated directional preponderance of caloric nystagmus: II. A neural network model. Am J Otol. 2000;21(4):568-72.
6. Kazmierczak H: Directional preponderance of caloric nystagmus in vestibular neuronitis. Otolaryngol Pol. 1989;43(2):128-34
7. Okinaka Y, Sekitani T, Okazaki H, Miura M, Tahara T: Progress of caloric response of vestibular neuronitis. Acta Otolaryngol Suppl.1993;503:18-22.
8. Kazmierczak H: Study of directional preponderance in central disorders of the vestibular system Otolaryngol Pol. 1989;43(3):195-200.
9. Proctor LR: Results of serial vestibular testing in unilateral Ménières disease. Am J Otol 2000; 21(4):552-8.
10. Mor R, Fragoso M, Taguchi CK, Figueiredo JFFR: Vestibulometria e fonoaudiologia: como realizar e interpretar. Lovise. São Paulo. 2000.
11. Pansini M, Padovan I: Three derivations in electronystagmography. Acta OtoLaryng. Stockh., 1969; 67:303-309.
12. Fitzgerald G, Hallpike CS: Studies in human vestibular function I: Observations on the directional preponderance ("nystagmusbereitschaft") of caloric nystagmus resulting from cerebral lesions. Brain 1942; 62(part 2):115-137.
13. Ganança MM, Caovilla HH, Munhoz MSL, et al: Nistagmo póscalórico. In: Caovilla HH, Ganança MM, Munhoz MSL, Silva MLG. Equilibriometria Clínica. Atheneu. São Paulo, 1999. 75.
14. Imate Y, Sekitani T: Vestibular compensation in vestibular neuronitis. Long-term follow-up evaluation. Acta Otolaryngol. 1993;113(4):463-5
1. Master degree student in Health Science: Infectious Diseases and Tropical Medicine by UFMG (Speech Doctor ate Clinical Hospital - UFMG)
2. Master in Linguistic Studies by UFMG (Speech Doctor, Assistant Teacher in the courser of Speech Therapy - UFMG)
3. PhD student in Health Science: Infectious Diseases and Tropical Medicine (Adjunct Teacher in the Ophthalmology ok and Phonoaudiology Department at the Medical School - UFMG)
Federal University of Minas Gerais Medical School Course of Post-Graduate Health Sciences: Infectologia and Tropical Medicine.
Lilian Felipe
Address: Street Mars, 83 - Neighborhood Ana Lucia - Sabará/MG - Phone/Fax: (31) 3485-5110 - E-mail: lilianfelipe@hotmail.com
CAPES - Coordination of Improvement of Higher Education Personnel
This article was submitted in Management System Publications (SGP) in the R @ IO 10/8/2006 and approved in 3/10/2006 12:39:04.