INTRODUCTIONReconstruction methods are essential for functional rehabilitation and treatment of traumatic bone loss or atrophic changes of the upper and lower jaws. Autogenous bone graft is considered the gold standard (17,20), however, autografting is limited by the amount of bone that can be retrieved, morbidity and risk of infection (17,22).
Biomaterials can be used for replacing autografts (22) and organic bovine bone matrix, an osteoconductive biomaterial (17) is used for these purposes (8), showing good results in orthognatic (17) and trauma surgeries (4). During processing, the biomaterial is washed to eliminate blood, fat and any impurities in order to reduce the infection risks and immunogenic host response (9). Then, it is decalcified and dehydrated by the lyophilization process, which prevents denaturation of the proteins while keeping the component active, including bone morphogenetic protein (BMP) (4). Therefore, the biomaterial retains the trabecular collagenous framework of the original tissue and can serve as a biologic osteoconductive scaffold with osteoinductive proteins despite the loss of structural strength (9). In vivo, studies have demonstrated the feasibility of using xenogenic bone in orthognatic (17) and trauma surgeries (4), but the results remain controversial, with different outcomes according to the type of defect (33) and variable reabsorption rate (24).
The association of biomaterials with repair promoters, like platelet-rich plasma (PRP), is promising (14) because it accelerates deposition and incorporation of new bones along the graft material, thereby reducing the time necessary to achieve ideal results. The PRP effect is attributed to local growth factors contained in the platelet. Additional advantages include their adhesive nature (13,18), hemostasis and lack of immune reaction (13). Studies have shown an increase in osteoblast activity and bone formation when mineralized (35,36) and demineralized bone matrices (17) are used in association with growth factors (21). However, some studies did not observe any increase in bone healing when using PRP (1,11,27). Therefore, the purpose of this study was to histologically evaluate bone repair in rabbit calvaria bone defects, after using bovine organic bone matrix, associated or not with PRP.
METHODMaterial
The tested material was bovine organic bone (BOB) (GenOx-organic®, Baumer SA, Mogi Mirim, SP, Brazil).
PRP preparation
PRP was prepared by following aseptic processing procedures according to Sonnleitner modified method (11). Blood was obtained several minutes before the administration of anesthesia. Five milliliters of blood were drawn from each rabbit from auricular vein using one 5ml vacutainer tubes containing anticoagulant (sodium citrate). A first centrifugation was performed during 20 minutes at 1000 rpm (160g) to separate the cell from blood plasma. The supernatant and 2 mm below the dividing line between the phases was pipetted and transferred to a tube without anticoagulant. A second centrifugation was performed for 15 minutes at the speed of 1600 rpm (400g). The PRP was separated from platelet poor plasma (PPP). For each 0.5 mL of PRP, 25 microliters of 10% calcium chloride was added as an activator.
Surgery procedure
Twelve healthy mature female New Zealand white rabbits weighing between 2,5 and 3,5kg were used as experimental animals. The experiment procedures were executed in conformity with the ethical principles of Brazilian College of Animal Experimentation. The animals were anesthetized intramuscularly with ketamine (25 mg/kg)/xylazine (10 mg/kg)/acepran (0.2 mg/kg)/midazolan (0.2 mg/kg) and local anesthesia with 0.9 mL of mepivacaine with epinephrine. A single prophylactic dose of antibiotic therapy with cephalosporin (30 mg/kg) was administered intravenously. With the rabbits in ventral position, trichotomy and antisepsis were performed in the calvaria region with a solution of topical povidine. This region received a middle line incision, which extended from the frontal to the occipital bone. The parietal bone was exposed by detaching the muscle and periosteum. Using an 8mm diameter trephine drill, under abundant irrigation with physiological solution, two defects were created in the right and left parietal bone. The defects were filled with coagulum (group I), BOB (group II) and BOB with PRP (group III). The animals received a normal diet consisting of granular food and water ad libitum. Four weeks after surgery, they were anesthetized with thiopental 2.5% and euthanatized with potassium chloride at 19.1%.
Sample evaluation
The bone pieces with the defects and the attached soft tissue were removed and immediately fixed in 10% phosphate buffered formaldehyde solution during 48h. Thereafter, the tissue blocks were decalcified in EDTA 4,13% during four weeks, dehydrated with graded alcohols and embedded in paraffin. The histological semi-serial sections of 5µm thickness obtained were stained with Hematoxillin-Eosine and Mallory Trichrome. Histological analysis of bone filling in the defective area, presence of giant cells and graft particles in the defective area, new bone formation associated with the graft particles, was performed under light microscope at X10 and X40 magnification in 3 sections for each paraffin block. The analysis using scores was conducted according to the following criteria (Table 1).
The results obtained were submitted to normality test, Kruskall-Wallis (Dunns post test) and Mann-Whitney tests. Differences were considered statistically significant at p<0.05.
RESULTSDuring the experiment, all the animals remained in good health and did not show any complications. The histological analysis of the defective area showed normal healing process. No inflammatory signs or adverse tissue was observed irrespective of the evaluated groups.
In Group I (coagulum) the defective area showed a dense connective tissue (Figure 1A) with bundles of collagen fibers and little bone in-growth from the periphery of the defect. The presence giant cells were not observed. In Groups II (organic) and III (PRP-included organic), we observed a little new bone formation mainly from the edges of the defect (Figures 1B and 1C), similarly with Group I. The defect was completely filled with a connective tissue along with the periosteum. Particles of the implanted graft or new formation associated with them were rarely seen. In all groups, calvaria thickness was reduced in the defective area, with a loss of the original architecture.
Histological results revealed no statistically significant differences in defective bone filling between all studied groups (p=0.83). There was no significant difference in the number of giant cells (p=0.49), graft particles (p=0.73) and new bone formation around graft particles (p not calculated) between the grafted materials separately or jointly with PRP (Table 2).
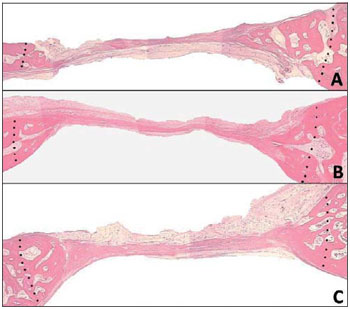
Figure 1. Defective area showed a dense connective tissue (Figure 1A) with bundles of collagen fibers and little bone in-growth from the periphery of the defect, in Groups II (organic) and III (PRP-included organic) a little new bone formation mainly from the edges of the defect (Figures 1B and 1C).
Rabbits are used as biological models to evaluate bone repair due to physiological and metabolic similarities to humans (25), in addition to offering a sufficient blood volume to prepare platelet concentrates (13). Furthermore, platelets of humans and other mammalians have a similar structure and constituents.
Bone regeneration in calvaria defects has some particularities due to the local tissue environment (10). In this study, care was taken to avoid damages in the underlying dura and also the periosteum, contributing to graft revascularization and integrity (19). It provides blood supply for bone and osteprogenitor cells, essencial for bone regeneration (2).
Large bone defects cannot heal spontaneously, preventing the natural repair of the damaged bone. Therefore, a precise comparison of different graft materials becomes possible (31). Autogenous graft is the pattern for reconstruction (16,17). However, researchers continuously try to improve the current bone grafting techniques and bone regeneration (3,5,30) to reduce the necessity of donor areas. Various bone substitutes and growth factors have recently become important in reconstructive surgeries (3,5).
The performance of organic bone replacements is not very clear, but some studies in orthognatic (17) and trauma surgeries (4) demonstrated good results, what didn't occur in the current study. The bone defects didn't show a new bone formation in the center of the defect in all experimental groups. Clearly, in the present study, the biomaterial was not able to maintain the original calvarial bone volume and, consequently, it didn't work as a scaffold. Bovine organic bone was rapidly absorbed and the histological analysis showed that the new bone was formed at peripheral areas, indicating a doubtful osteoconductive and osteoinductive (28) ability of the material, which didn't differ from coagulum.
Because the biomaterial reabsorption must occur just before the material can be replaced by the newly formed bone, a delicate balance between the two concurrent processes must be maintained for the graft to be replaced by the host bone without an appreciable loss of volume (15). As such, the reabsorption rate and the time elapsed for the material reabsorption appears to be related to the amount of new bone formation (24). When the graft particles are slowly absorbed, they act like a scaffold during the healing period, conducting the new bone formation within the defects. Therefore, the accelerated reabsorption rate of organic bone matrices observed may be the main disadvantage of this material. As a result, demineralized bone could be indicated in procedures where variable reabsorption may be acceptable (7) like the repair of small defects.
The material processing certainly decreases the risk of infection and immunogenic host response, nevertheless the possibility of transmitting diseases is not eradicated (9). Apparently, the material may elicit an antigenic stimulus sufficient to amount an antibody immune response in the host, resulting in accelerated incorporation and also, rapid graft reabsorption as observed in the present study. The biomaterial may be, for the host, an antigenic deposit which is continuously exposed to the immune system (23). As long as the graft reabsorption progress, the previously inaccessible incorporated proteins and, probably residual toxic agents derived from scaffold processing are released, affecting host cell viability and functions, including differentiation of surrounding osteogenic cells.
This material is formerly known as an alternative graft formed by placing the harvested bovine bone in acid bath, resulting in an osteoconductive collagen matrix with BMP, which impart the osteoinductive properties of this graft (7). Despite the expected positive effect of the biomaterial, some studies claimed that the material processing can reduce the concentration of matrix incorporated factors or even result in their inactivation, thereby accounting for the observed lack of osteoinductivity. This phenomenon may also be compounded by the presence of soluble osteogenic inhibitory factors, which can also be found in these kind of materials.
Platelets are a natural source of growth factors that play an important role in the wound-healing process (34). Increasing the concentration of platelets in a bone defect may lead to improved bone formation. However, the association of PRP to biomaterials stays controversial (27). Some in vivo studies demonstrated the effectiveness of PRP associated with bone substitutes for treating periodontal defects or for sinus floor augmentation (26). On the other hand, other studies have failed to show the favorable effect of PRP combined with various biomaterials on bone regeneration (32). The present study failed to identify a markedly increase in bone formation when adding PRP. The potency of growth factors liberated by PRP seems to be too weak to induce bone formation in defects with low regenerative capacity (29) like the ones of our study.
Platelets are known to be effective during the initial stage of bone graft healing (12), because the life span of a platelet in a wound and the period of direct influence of its growth factors are less than five days (6). Therefore, a major effect of PRP supposedly occurs during the early stages of bone regeneration (12) and couldn't be seen in long-term evaluations like in this study. Additionally, new bone formation along with the biomaterial particles didn't occur due to its fast reabsorption, which could have influenced the effectiveness of PRP.
CONCLUSIONIn this study, bovine bone material failed to perform the new bone formation within defects. In accordance with the results, the matrix of bovine organic bones neither separately nor jointly with PRP improves the bone repair.
REFERENCES BIBLIOGRAPHCS1. Aghaloo TL, Moy PK, Freymiller EG. Evaluation of platelet-rich plasma in combination with freeze-dried bone in the rabbit cranium. A pilot study. Clin Oral Implants Res. 2005, 16(2):250-7.
2. lberius P, Isaksson S, Klinge B, Sjögren S, Jönsson J. Regeneration of cranial suture and bone plate lesions in rabbits. Implications for positioning of osteotomies. J Craniomaxillofac Surg. 1990, 18(6):271-9.
3. Barone FC. Endogenous brain protection: models, gene expression, and mechanisms. Methods Mol Med. 2005, 104:105-84.
4. Bostrom MP, Seigerman DA. The clinical use of allografts, demineralized bone matrices, synthetic bone graft substitutes and osteoinductive growth factors: a survey study. HSS J. 2005, 1(1):9-18.
5. Butz SJ, Huys LW. Long-term success of sinus augmentation using a synthetic alloplast: a 20 patients, 7 years clinical report. Implant Dent. 2005, 14(1):36-42.
6. Choi BH, Im CJ, Huh JY, Suh JJ, Lee SH. Effect of platelet-rich plasma on bone regeneration in autogenous bone graft. Int J Oral Maxillofac Surg. 2004, 33(1):56-9.
7. Constantino PD, Facs S, Hiltzik D, Govindaraj S, Moche J. Bone Healing and Bone Substitutes. Fac. Plastic Surg. 2002, 18(1):25-34.
8. Eppley BL, Pietrzak WS, Blanton MW. Allograft and alloplastic bone substitutes: a review of science and technology for the craniomaxillofacial surgeon. J Craniofac Surg. 2005, 16(6):981-9.
9. Giannoudis PV, Al-Lami MK, Tzioupis C, Zavras D, Grotz MR. Tricortical bone graft for primary reconstruction of comminuted distal humerus fractures. J Orthop Trauma. 2005, 19(10):741-3.
10. Gosain AK, Santoro TD, Song LS, Capel CC, Sudhakar PV, Matloub HS. Osteogenesis in calvarial defects: contribution of the dura, the pericranium, and the surrounding bone in adult versus infant animals. Plast Reconstr Surg. 2003, 112(2):515-27.
11. Hatakeyama M, Beletti ME, Zanetta-Barbosa D, Dechichi P. Radiographic and histomorphometric analysis of bone healing using autogenous graft associated with platelet-rich plasma obtained by 2 different methods. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008, 105(1):13-8.
12. Kanno T, Takahashi T, Tsujisawa T, Ariyoshi W, Nishihara T. Platelet-rich plasma enhances human osteoblas-like cell proliferation and differentiation. J Oral Maxillofac Surg. 2005, 63(3):362-69.
13. Kim E, Park E, Choung P. Platelet concentrates and its effect on bone formation in calvarial deffects: an experimental study in rabbits. J Prosth. Den. 2001, 86:428-33.
14. Kim SG, Kim WK, Park JC, Kim HJ. A comparative study of osseointegration of Avana implants in a demineralized freeze-dried bone alone or with platelet-rich plasma. J Oral Maxillofac Surg. 2002, 60(9):1018-25.
15. Lewandrowski KU, Rebmann V, Pässler M, Schollmeier G, Ekkernkamp A, Grosse-Wilde H, Tomford WW. Immune response to perforated and partially demineralized bone allografts. J Orthop Sci. 2001, 6(6):545-55.
16. Lohmann H, Grass G, Rangger C, Mathiak G. Economic impact of cancellous bone grafting in trauma surgery. Arch Orthop Trauma Surg. 2007, 127(5):345-8.
17. Lye KW, Deatherage JR, Waite PD. The use of demineralized bone matrix for grafting during Le Fort I and chin osteotomies: techniques and complications. J Oral Maxillofac Surg. 2008, 66(8):1580-5.
18. Lysiak-Drwal K, Dominiak M, Solski L, Zywicka B, Pielka S, Konopka T, Gerber H. Early histological evaluation of bone defect healing with and without guided bone regeneration techniques: experimental animal studies. Postepy Hig Med Dosw (Online). 2008, 11(62):282-8.
19. Manson PN. Facial bone healing and bone grafts. A review of clinical physiology. Clin Plast Surg. 1994, 21(3):331-48.
20. Maus U, Andereya S, Gravius S, Siebert CH, Ohnsorge JA, Niedhart C. Lack of effect on bone healing of injectable BMP-2 augmented hyaluronic acid. Arch Orthop Trauma Surg. 2008, 128(12):1461-6.
21. Mott DA, Mailhot J, Cuenin MF, Sharawy M, Borke J. Enhancement of osteoblast proliferation in vitro by selective enrichment of demineralized freeze-dried bone allograft with specific growth factors. J Oral Implantol. 2002, 28(2):57-66.
22. Nacamuli RP, Longaker MT. Bone induction in craniofacial defects. Orthod Craniofac Res. 2005, 8(4):259-66.
23. Nordström E, Ohgushi H, Yoshikawa T, Yokobori AT Jr, Yokobori T. Osteogenic differentiation of cultured marrow stromal stem cells on surface of microporous hydroxyapatite based mica composite and macroporous synthetic hydroxyapatite. Biomed Mater Eng. 1999, 9(1):21-6.
24. Norton MR, Odell EW, Thompson ID, Cook RJ. Efficacy of bovine bone mineral for alveolar augmentation: a human histologic study. Clin Oral Implants Res. 2003, 14(6):775-83.
25. Nunamaker DM. Experimental models of fracture repair. Clin Orthop Relat Res. 1998, 355(Suppl):56-65.
26. Okuda K, Tai H, Tanabe K, Suzuki H, Sato T, Kawase T, Saito Y, Wolff LF, Yoshiex H. Platelet-rich plasma combined with a porous hydroxyapatite graft for the treatment of intrabony periodontal defects in humans: a comparative controlled clinical study. Periodontol. 2005, 76(6):890-8.
27. Plachokova AS, van den Dolder J, Stoelinga PJ, Jansen JA. Early effect of platelet-rich plasma on bone healing in combination with an osteoconductive material in rat cranial defects. Clin Oral Implants Res. 2007, 18(2):244-51.
28. Sanada JT, Rodrigues JGR, Canova GC, Cestari TM, Taga EM, Taga R et al. Análise histológica, radiográfica e do perfil de imunoglobulinas após implantação de enxerto de osso esponjoso bovino desmineralizado em bloco em músculo de ratos. J. Appl. Oral Sci. 2003, 11(3): 209-215.
29. Sarkar MR, Augat P, Shefelbine SJ, Schorlemmer S, Huber-Lang M, Claes L, Kinzl L, Ignatius A. Bone formation in a long bone defect model using a platelet-rich plasma-loaded collagen scaffold. Biomaterials. 2006, 27(9):1817-23.
30. Schizas C, Triantafyllopoulos D, Kosmopoulos V, Tzinieris N, Stafylas K. Posterolateral lumbar spine fusion using a novel demineralized bone matrix: a controlled case pilot study. Arch Orthop Trauma Surg. 2008, 128(6):621-5.
31. Schmitz JP, Hollinger JO. The critical size defect as an experimental model for craniomandibulofacial nonunions. Clin Orthop Relat Res. 1986, 205:299-308.
32. Tsay RC, Vo J, Burke A, Eisig SB, Lu HH, Landesberg R. Differential growth factor retention by platelet-rich plasma composites. J Oral Maxillofac Surg. 2005, 63(4):521-8.
33. Torricelli P, Fini M, Giavaresi G, Rimondini L, Giardino R. Characterization of bone defect repair in young and aged rat femur induced by xenogenic demineralized bone matrix. J Periodontol. 2002, 73(9): 1003-9.
34. Weibrich G, Kleis WK, Hafner G, Hitzler WE, Wagner W. Comparison of platelet, leukocyte, and growth factor levels in point-of-care platelet-enriched plasma, prepared using a modified Curasan kit, with preparations received from a local blood bank. Clin Oral Implants Res. 2003, 14(3):357-62.
35. Zambuzzi WF, Oliveira RC, Alanis D, Menezes R, Letra A, Cestari, TM, Taga R, Granjeiro JM. Microscopic analisys of porous microgranular bovine anorganic bone implanted in rat subcutaneous tissue. Journal of Applied Oral Science. 2005, 13(4):382-86.
36. Zambuzzi WF, Oliveira RC, Pereira FL, Cestari TM, Taga R, Granjeiro JM. Rat subcutaneous tissue response to macrogranular porous anorganic bovine bone graft. Braz Dent J. 2006, 17(4):274-8.
1 Master. Professor of Oral and Maxillofacial Surgery and Traumatology.
2 Master. Attending Doctorate Degree in Stomatopathology.
3 Doctor. Professor of Oral and Maxillofacial Surgery and Traumatology.
4 Doctor. Professor of Oral Histology.
Institution: Federal University of Uberlandia's Dentistry School. Uberlândia / MG - Brazil. Mailing address: Flaviana Soares Rocha - Avenida Pará s/nº - Campus Umuarama - Bloco 4T - Department of Oral and Maxillofacial Surgery and Traumatology - Bairro Umuarama - Uberlândia / MG - Brazil - ZIP Code: 38400-902 - Telephone: (+55 34) 3218-2636 / 3238-6095 - Email: flavianasoares.rocha@gmail.com
FAPEMIG
Article received on November 18, 2010 . Article approved on March 09, 2011.