INTRODUCTIONLaryngeal Cancer is not very frequent. It represents from 1 to 2% of malignant tumors in men. Its importance is related to the changes in the vocal organ, for its presence as much as for surgical procedures, either changing or suppressing speech language. In some patients such changes lead to psychosocial alterations endangering their quality of life.
Such tumor can be healed when early diagnosed through surgical methods, irradiation, or this one combined with surgery and chemotherapy, originating good results as for patients' life and preservation of their speech language.
METHODSWe analyzed 1055 patients with laryngeal cancer, submitted to surgery for 35 years (1955 - 1990). Patients are from Clinica de Endoscopia Per-Oral (Peroral Endoscopy Clinic) and Head and Nech Surgery - Bonsucesso Hospital - Health Department - Rio de Janeiro State and patients from private clinics owned by one of the authors.
We will describe the used techniques, surgery and post-surgery implications followed by the result analysis. This type of tumor occurs in men with more frequency: 968 patients were male (91.7%) and 87 were female (8.2%). From the 1055 studied patients, 140 did not have a follow-up, 915 were reviewed for more than 5 years, 86% was white, 7.5% was brown and 5.6% was black, aging from 20 and 84 years.
We will follow the TNM Classification (tumor, nodes, metastasis) for being the best way of defining the level of lesions.
RESULTS AND DISCUSSIONLaryngeal cancer has its own features according to its location. Three areas compose larynx: supraglottic, glottic and subglottic. Supraglottic area arises from 3rd and 4th pharyngeal arches (facial bucal segment of the embryo), the other two areas arises from the 5th and 8th pharyngeal arches (pulmonary segment of the embryo) (1). Beyond these anatomic and embryological distinguishions, there is a division on blood and lymphatic irrigations. Supraglottic area is irrigated by superior laryngeal artery, carotid branch. Glottic and subglottic areas are irrigated by inferior thyroid artery, subclavian branch. The big amount of lymph nodes on supraglottic area drains through thyrohyoid membrane to medium and superior lymph nodes of the jugular chain. The lymph nodes from vocal fold, which are scarcer, drain through cricothyroid to medium and profound lymph nodes of the jugular chain.The anterior glottic area posses a lymphatic net that drains through superior part of cricothyroid membrane to pre-laryngeal or Delphian lymphonode. This lymph node is placed on anterior part of the cricothyroid membrane, above isthmus of thyroid gland. The contamination of pre0laryngeal lymph node is compared to contralateral lymph node metastasis (TUCKER, 2).
Histology from the 1055 patients showed: 1) epidermal carcinoma in 1050 cases; 2) carcinoma of fusiform cells (carcino-sarcoma) in 2 cases and, 3) one case of warty carcinoma, and 2 cases of papilliferous adenocarcinoma of thyroid gland penetrating larynx.
Supraglottic TumorsSupraglottic lesions are more often in women. From the 87 female patients, 18 of them (20.6%) had supraglottic tumors; from the 968 male patients, 57 of them (5.8%) had supraglottic lesions. Tumors on supraglottic area hardly spread to the glottic one, although there is no evidence of an anatomic barrier to explain such fact. The different embryologic origin of this area and separation of blood and lynphatic irrigations are possibly the reasons why such tumors rarely overpass Morgagni´s ventricle. Based on such findings, Alonso (3) created a surgery technique known as horizontal or supraglottic laryngectomy, and it is used by most of authors with excellent results. These tumors can infiltrate epiglottis cartilage and infect preepiglottic space. The tumors which infiltrate such space can also expand to the valecula and then to the base of tongue, spreading to aryepiglottic ligament and, in some cases, to medium surface of the pyriform sinus. 75 patients with supraglottic lesions underwent surgery by horizontal laryngectomy technique, with small changes, according to its extension. We did not withdraw the hyoid bone in the tumors in the laryngeal surface of the epiglottis because its presence makes the healing of surgery wound easier. In some cases we opened the bone in its medium part, separating the two halves and suturing at the end. In the cases in which we realized infiltration of pre-epigottic space during surgery, the hyoid bone was removed together with the surgical specimen and closing was performed with the base of tongue.
The critical point of this surgery is the delay to re-establish deglutition. For this reason, in the patients over 60, it was also performed, together with pre-surgery routinely exams, a clinical study of the respiratory function, though the elderly has more difficulty for deglutition. If respiratory function showed expressive changes, we would decide for comprehensive laryngectomy.
33 patients had lesion type T1AN0M0 (26 men and 7 women), 28 patients had lesions type T1BN0M0 (20 men and 8 women). In 7 patients, the lesion was a more extensive type, T4N0M0 (6 men and 1 woman). 7 patients presented metastasis in cervical lymph nodes: T1AN1M0, T1BN1M0, T4N1M0 (5 men and 2 women). 7 patients from this series did not have any follow-up and were taken out of the analysis. 68 patients had a follow-up, 50 men and 18 women. From these, 40 (58.8%) are alive.
11 patients had local recurrence, 4 underwent laryngectomy and 2 are alive. The others, although had been treated through irradiation or chemotherapy, died. 6 patients came back with distant cervical lymph node metastasis. In 3 patients a radical lymph node emptying was performed; 2 of them are alive and the others, with fixed or ulcerous lesions, died. 6 patients had distant metastasis: 5 patients with pulmonary metastasis and 1 with hepatic metastasis died. 2 patients died in the post-surgery period: one had a cerebral vascular accident and the other had hemorrhage on the lingual artery. 2 patients died two years after surgery: (acute myocardial infarction) and the other had lung abcess by aspiration. 1 patient died during surgery of cardiac-respiratory paralysis.
Tumors of ariepiglottic ligament Still on supraglottic area, 5 male patients underwent surgery with tumor on aryepiglottic ligament, 2 at the right side and 3 at the left one. In one patient the tumor was removed by endoscopy and its base was cauterized. The others underwent surgery through lateral pharyngotomy, with resection of lesion and suture of mucosa. One patient did not come back and 3 are alive and in good condition (75%). One patient presented recurrence and was submitted to a comprehensive laryngectomy and died of recurrence in the pharynx after ten years.
Glottic Tumors Tumors on glotal area occur more often in malignant lesions, arising from squamous epithelium of vocal fold mucosa. Their development occurs slowly; they have late metastasis and their main symptom is precocious dysphonia. They usually come after histological lesions of the epithlium, named pre-malignant, such as epithelial hyperplasia, which might present keratosis in its superficial layer, an in more profound ones (dyskeratosis). These alterations are in most cases responses to external inhaling, such as smoking. Dysplasia might occur in more advance stages, and they can be either mild, moderate or intense. Dysplasias are not described only by alteration on cell disposition, but also by nuclear changes (atypia), with hypercolored nucleus and increased nucleus, in relation to cytoplasm and appearing of mitosis. The next step is the intraepithelial carcinoma, where the epithelial layer is disorganized with a great number of mitosis, characterizing a malignant lesion.
Auerbach and col. (6) studied, through autopsy, subjects who had died of different causes, and separating them in three groups: smokers, non-smokers and former smokers for more than five years. The larynx exam showed cell atypia in 99% of the cases in the smoker group; in16% it was diagnosed carcinoma-in-situ. In the other two groups, no it intraepithelial carcinoma was found, and only 25% of the cases had cell atypia. The great number of lesion found on smokers and the large reduction of these lesions in patients who had quit smoking make us think, as AUERBACH and col. did, about the possibility of regression of these lesions with dismissal of aggressive agent.
Intraepithlial CarcinomaThis type tumor was described by BRODERS (7) in 1932. calling it as carcinoma-in-situ. ALTMANN (8) published a series of detailed cases in his histological structure in 1952. This is a malignant lesion in epithelial layer of the mucosa. However, when small epithelial bud from basal invades submucosa, it is named carcinoma-in-situ with microinvasion. Through laryngoscopy of suspension, LYNCH (9) performed operation in the first cases in 1920. Only in 1968, together with the works by KLEINSSASER (10) on endoscopy resection by microlaryngoscopy, this surgical method started being used and become known. APRIGLIANO FILHO (11), in his work on carcinoma-in-situ, also demonstrates the advantages of surgical treatment.
We operated 54 of cases of intraepithelial or microinvasive lesions of vocal fold. The average male age (46 patients) was 56 years and female age (8 patients) was 53. In 49 of the cases, lesion was unilateral and in 5 cases it was bilateral. From all cases, 30 of them were of carcinoma-in-situ, 19 were carcinoma-in-situ with microinvasion and 5 presented small invasive lesions limited to the third medium of folds. 4 cases presented recurrence, one did not come back, and 1 patient was submitted to a comprehensive frontal lateral laryngectomy, and is alive. Another one died of pulmonary metastasis. None patient died of laryngeal cancer.
Surgery by microlaryngoscopy is well known. Exposition of vocal folds should be complete from the anterior up to the posterior suture, using a larger suspension laryngoscope to the patient. Mucosa, fixed with micro nippers, is removed with a scalpel or curved scissors, up to the exposition of conical ligament. If in doubt, part of vocal muscle can be removed, for cicatrisation and vocal recovery being easy.
In the cases of bilateral lesions or second operation situation, the minimum break between procedures should be 4 weeks. This surgery should be performed with the aid of a pathologist, who will examine, through congelation, the limits of resection. These patients should be seen every 2 months during the first year, with a progressive increase of these breaks, and after 5 years the examination will occur once a year.
Invasive glottic tumorsThese tumors spread more easily to the subglottis, and it can also penetrate the Morgagni´s ventricle and paraglottic space, determining the palsy of the wounded vocal fold. The tumors of medium wall and anterior angle of the pyriform sinus can also determine vocal fold palsy by paraglottic space invasion, with no apparent lesion of it.
The glottic tumors that overpass Morgagni´s ventricle and invade the false fold were named transglottic (MAC-GRAVAN, 12). The first tumors from subglottis are rare. KLEINSSASER (13) does not believe they are from the area. According to him, subglottic area is part of the glottic one and such tumors would be subglottic extensions from glottic tumors. In our cases, we observed only one patient whose lesion was taken as primitive from subglottis (0.1%).
266 patients were submitted to partial laryngectomy.
21 of them with cordectomy and 245 with partial frontal lateral laryngectomy of LEROUX ROBERT type (14).
The 21 patients submitted to cordectomy were the first of our series and results were inferior if compared to other types of partial surgeries performed. 14 patients (66.6%) survived more than 5 years. One patient presented dermal metastasis 3 months after surgery and died. 6 patients had local recurrence and underwent to laryngectomy; 4 of them survived. From the 245 patients submitted to frontal lateral laryngectomy, 20 of them were not followed-up after surgery and 225 were: 105 of them had lesions type T1AN0M0; 79 type T1BN0M0 and 41 presented more extensive lesions with reduction or fixation of vocal fold (T2N0M0) and (T3N0M0), but limited to that. These patients underwent surgery by a frontal lateral widen technique. This technique consists of removing both vocal fold and false vocal fold and removing part or all line of thyroid cartilage of the sick side. If there is not enough mucous flap, the rebuild of this hemilarynx is done in a way that the mucosa is taken to the pyriform sinus and sutured it to the remaining end. The remainders in each group were: 80 patients (76.1%) with lesion type T1AN0M0, 59 patients (76.6%) with T1BN0M0 and 24 patients (56%) with more advanced lesions (T2N0M0) and (T3N0M). One patient with (T1AN0M0) died of cardiac-respiratory paralysis during surgery and three died in five years after surgery: one of cerebral vascular accident and two of acute myocardial infarction. Four patients presented a second primary tumor: one with pulmonary carcinoma and another with esophagus carcinoma, both were irradiated but died. One patient with lip carcinoma underwent surgery and is alive. Another patient presented colon carcinoma (diagnosed 13 year after laryngeal surgery), underwent surgery and died of recurrence of such tumor one year later.
15 patients with T1AN0M0 lesions presented local recurrences. One did not come back, 9 were submitted to comprehensive laryngectomy, 1 was re-operated and 4 were irradiated. 7 patients are still alive more than five years after surgery. One patient died of acute myocardial infarction and the others died of either lymph node metastasis or distant metastasis. 5 patients came back with cervical lymph node metastasis and 4 were submitted to a cervical lymph node emptying. One patient was irradiated, 1 did not come back and 2 are alive. One patient presented recurrence and underwent laryngectomy and died with recurrence on pharynx.
From the patients with lesion type T1BN0M0, 1 died of digestive hemorrhage in the post-surgery period, 2 died of acute myocardial infarction in five years after surgery, 2 presented distant metastasis: one with dermal metastasis and the other with cerebral metastasis. One patient presented a second primary esophagus tumor, was irradiated but died. Twelve patients presented local recurrence, 2 did not return. Seven underwent laryngoctomy, 1 did not have a follow-up, 2 were irradiated and 1 had a second surgery. From this group, 4 patients are alive. 2 presented cervical lymph node metastasis, were submitted to a radical lymph node emptying and are alive. The others died of distant metastasis.
From the 52 patients with more advanced lesions (T2N0M0 and T3N0M0), 41 had a five-year-follow-up at least, and 24 (58.5%) are alive. 13 patients presented local recurrence, 12 underwent laryngectomy and 1 had a second surgery. 7 patients are alive. 3 develop pulmonary metastasis, 2 had recurrence on pharynx and did not come back and one died of cardiac insufficiency in the post-surgery period. 2 patients came back with cervical lymph node metastasis, were submitted to a radical cervical lymph node emptying and are alive. One patient died of second primary pulmonary tumor and another one, two years after surgery, presented a lesion on the side of epiglottis facing larynx.
In the frontal lateral laryngectomy technique, after separating anterior muscles we isolated the prelaryngeal ganglion, removing it for histological examination. In 6 patients (2.4%) the pre-laryngeal ganglion was endangered. In 8 patients (3.2%) with lesions T1A and T1B, the surgical specimen did not present any sign of malignant lesion at histological exam. Picture 1 shows surgical specimen from a widened frontal lateral laryngectomy.

Picture 1. Surgical specimen from a widened frontal lateral laryngectomy.
In the first twelve hours after surgery, one patient presented subcutaneous emphysema. Placing drainner in different parts of the neck reduced it and patient was released from hospital in good condition. 3 patients needed to be drained of an anterior subcutaneous abcess, another on presented a post-surgery bleeding, requering an opening of the wound to hemostasy. 3 patients presented fistula on cartilage joints, which was closed through daily dressing. 2 patients presented laryngeal stenosis, requiring dilatation, so the tracheostomy canula could be removed. 14 patients presented granulomas at the anterior angle of the larynx, which were removed through direct laryngectomy. In 19 patients the covering of surgery wound was done with a bipedicled graft from hyoid sternum muscle. Therefore, such procedure was disregarded, though results were not sufficient.
From the 655 patients submitted to a comprehensive laryngectomy, 24 presented lesions type T2N0M0, 472 presented lesions type T3N0M0 and 45 type T4N0M0. In the first visit 114 patients already had cervical metastasis. From those, 6 with T2N1-2M0, 67 with T3N1-2M0 and 41 with T4N1-2M0. From the 24 patients with lesions type T2N0M0, two did not come back to revisions and 16 are alive more than five years (72.7%). One patient died of acute renal failure after digestive hemorrhage in the post-surgery period. 2 patients presented local and ulcerous lymph node recurrences, and died. After 8 months, a third patient presented metastasis at the level of tracheostom and was submitted to a chemotherapeutic treatment, with no results. Two patients died in two years after surgery, one of bilateral pulmonary metastasis and the other of second primary lung tumor.
There were 472 patients with lesions type T3N0M0. From those, 67 did not have a follow-up, so 405 was the number of studied patients. We found 162 transglottic lesions, 123 lesions in theto glottis, 45 glottic lesions with extension to subglottis, 58 glottic lesions that invaded anterior comissure, reaching the anterior third part of the opposed vocal fold, and 17 patients with lesion in the posterior third of the vocal fold and posterior comissure.
From the 405 patients with lesion type T3N0M0 who had follow-up, 226 (55.8%) are alive. From 45 patients with lesions type T4N0M0, 9 did not have a follow-up. From 36 patients who were followed-up 18 (51.4%) are alive. 2 patients with lesion T4N0M0 presented papillary adenocarcinoma of thyroid gland with invasion of the larynx. They were submitted to laryngectomy with comprehensive thyroidectomy and a conservative cervical lymph node emptying. Both survived fro more than five years.
In the 114 patients with cervical lymph node metastasis, comprehensive laryngectomy was performed together with a radial cervical lymph node emptying. From 6 patients with lesions type T2N1-2MO, 1 did not have a follow-up, 4 are alive (80%) and one died of ulcerous cervical metastasis. Among the 67 patients with lesions type T3N1-2M0, 14 were not followed-up. From the 53 remaining patients, 30 of them (56.6%) are alive. From 41 patients with lesions type T4N1-2M0, 12 were not followed-up. Among the 29 remaining patients, 12 are alive (41.3%). There was a need of a partial pharyngotomy in order to remove the lesion completely in 20 patients with lesions type T4NO and T4N1-2MO. In two patients, there was a need of a partial parotidectomy, though tumor was invading parotid gland. Both died, one of recurrence on the pharynx and the other of recurrence on parotid gland. In one patient with T4N1MO, whose lesion was invading valecula, we performed a partial glossectomy. This patient is still alive for more than 5 years.
The technique applied to perform comprehensive laryngectomy was the one by GLUCK- SOERENSEN (15). From 1962 we started to routinely perform a bilateral cervical lymph node emptying. Only in very few cases we made use of nasal-gastric probe for feeding purposes (16). The observation from patients who underwent laryngectomy showed that most of them complained of using probe for being uncomfortable and many withdrew it in the first 24 hours after surgery. In this mentioned group, probe was not reintroduced because such patients had easy swallowing. They were then fed with liquid (tea, 150ml every 3 hours) after 48 hours after surgery. If acceptance was good, we added milk and fruit juice on the following day, and then started with semisolid feeding after 4 or 5 days. This type of procedure reduced days in hospital and provided more comfort to patient.
As mentioned before, in lesion type T3N0M0, T2N0M0 and T4N0M0 we performed a conservative-like cervical lymph node emptying. In 113 cases, histological exam from surgical specimen showed one or more affected lymph node (20.8%). These patients were irradiated after being released (3-to-4-week breaks). From this, 42 patients presented metastasis on cervical lymph node chain in a period ranging from 6 to 18 months after laryngectomy and 5 did not return to treatment. It was performed a radical cervical lymph node emptying in 27 patients, 4 from those were irradiated. From all those, 13 are alive and the others died of either the disease or distant metastasis. From the 37 patients who return with recurrence at pharynx level only 3 could go through surgical resection of the lesion, and just one is alive. The other patients who presented recurrence were submitted to either radiotherapeutic or chemotherapeutic treatment with no results. The 5 patients who presented recurrence on pharynx and cervical lymph node metastasis at the same time died. Four patients presented supraclavicular lymph node recurrence. Surgical resection followed by radical cervical lymph node emptying was possible to be performed in two of them. One is still alive. The other patients with recurrence were submitted to either radiotherapeutical or chemotherapeutical treatment unsuccessfully.
The worst type of recurrences that might occur after comprehensive laryngectomy is the one at the level of tracheostom. It often occurs between 8th and 30th month after surgery, rarely before this period, and its incidence ranges from 5 to 15%. The causes are: a) preciously tracheostomy in obstructed patient, b) lesion extended to subglottis, for the possibility of contamination of paratrachea lymph nodes (17), and c) the permanence of lesion at the margin of surgical specimen.
From 655 comprehensive laryngectomy that we performed, 38 patients presented recurrence at the level of tracheostom (5.8%).We performed a previous tracheostomy in 87 patients, i.e., patients arrived with obstruction and underwent emergency tracheostomy before comprehensive laryngectomy in a period of 7 and 18 days. We observed 18 cases (20.6%) of recurrence on tracheostom (18).Recurrence on tracheostomy occurred in 20 patients (3.5%) out of 568 patients with no previous tracheostomy. From 38 cases of recurrence on tracheostom, the lesion on larynx extended up to the subglottis in 8 of them (21%).
We can suggest that the factors that are more likely to occurr for the recurrence on tracheostom are: lesions that spread to subglottis and patients who are submitted to a previous tracheostomy.
Recurrences surgeries on tracheostom can be performed (19,20), but results are not stimulating. KLEINSSASER (13) believe that lesions on superior or supralateral arch are more recommended to surgery. In most cases of lesion on inferior arch there is an invasion from mediastinal vessels and, according to the author, there are stores in them as for surgical recommendation. We operated 14 out of 38 patients with recurrences on tracheostom. The others had a palliative treatment: irradiation, chemotherapy or both. The surgery consisted of isolating tracheostom; resecting part of manubrium sternal and dissecting trachea (up to the point where it can be resected with two or three rings free of contamination); forming a new tracheostom; drainage and closing. Only 3 patients (21.4%) survived for 5 years. One patient did not return after surgery, other died of a acute renal failure in post-surgery period, and a third one develop a second primary lung tumor after 5 months and was submitted to chest surgery, and we lost contact. The other patients died of recurrence; in 2 cases there were necrosis with loss of substance and carotid fracture. Picture 2 shows a surgical specimen from a transglottic tumor.
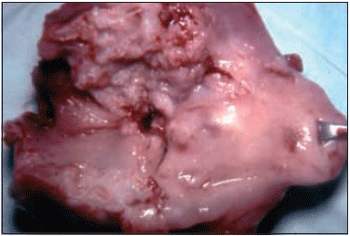
Picture 2. Surgical specimen from a comprehensive laryngectomy, showing transglottic lesion.
Complication during surgeryThree patients died of cardiac-respiratory paralysis (hypoxia during anesthesia) during surgery and although routine procedures were applied, we could not recover them. Another patient suffered from diffuse bleeding and at the end of a radical cervical lymph node emptying. All procedures to control hemorrhage were used, though the patient died of hypovolemic shock on the surgical table. Later blood test, which was collected during surgery, showed an abnormal concentration of fibrolysin in the blood, what prevented a normal coagulation. Surgical death was 0.4%.
Post Surgery ComplicationsOne patient died of cardiac paralysis in 24 hour after surgery, presenting hyperthermia (42.50). There was a need of opening the wound in order to perform hemostasy in 11 patients who presented hemorrage in the post-surgery period and, in 5 patients it was necessary to perform anterior abscess drainage. There was no death in this group of 16 patients.
Pharyngocutaneous Fistula is the most frequent complication after a comprehensive laryngectomy. It generally occurs between the 4th and 10th days after surgery. Most of the times there is a coincidence between dermal and pharynx opening (direct fistulas). There are cases in which dermal opening communicates with pharynx opening through non-epithelized fistuloso track (indirect fistulas). The incidence of larynx fistula ranges from 4 to 50% (18).
We observed 74 pharyngocutaneous fistula (11.2%) among the 655 performed laryngectomyies. 4 fistulas occurred after the opening for hemostasy in bleeding and 5 occurred after anterior abscess drainage.
There are several causes that might lead to a pharyngocutaneous fistula formation: a) tension on suture of pharynx mucosa, especially on surgeries in which there is a need of resecting part of pharynx mucosa. In these cases there is a reduction of mucous flap and suture might become tense; b) previous irradiation with the purpose of healing. We could observe 63 fistulas (23.2%) among the 612 patients who were previously irradiated. Among the 612 who were not irradiated, we found 64 fistulas (10.4%). This suggests precious irradiation as a factor that might lead to a fistula formation. c) The appearing of fistulas is greater in comprehensive laryngectomy followed by a cervical lymph node emptying. We observed 25 fistulas (21.9%) in 114 patients who underwent laryngectomy with radical cervical lymph node emptying.
7 out of 74 patients with pharyngocutaneous fistula presented severe complication.
5 from those had pulmonary complications and died of aspiration. In 2 of them there was necrosis of flap with carotid breakage, though it was possible to accomplish suture in one of them. Therefore, this patient had hemiplegia and died in hospital.
In a period raging from 12 to 45 days it was performed closing of 63 fistulas but only under daily dressing care. In 4 cases there was a need of surgical closing, and in one of them a deltopectoralis flap was placed though in two surgeries.
Three patients presented lymphatic fistula. In two cases closing was done through daily dressing, and in the third case through suture of thoracic duct.
In 3 patients the hypoglossal nerve was damaged during cervical lymph node emptying. 2 of them had tongue paralysis with dysphagia.
After three months such patients swallowed in normal way; with the third patient we performed anastomosis of the two ends of the nerve and the function was kept.
From the patients who were previously irradiated with the purpose of healing, 63 patients presented recurrence in a period raging from 8 to 20 months, and a surgery was need. In 20 of them we performed a patial laryngectomy, though in 43 we had to remove the larynx.
In the cases of laryngeal cancer, most of distant tumor manifestations addresses to lungs. From 55 patients (5.2%), 28 of them (2.6%) had pulmonary metastasis and 27 (2.5%) had second primary lung tumor. Prognosis in these cases is not very stimulating.
Analysing the cases submitted to surgery, we could observe an expressive difference on surviving between male and female patients. Considering all types of surgery performed, 968 patients were male and 135 did not have a proper follow-up after surgery. Among the 833 patients regularly followed-up, 498 are alive 5 years or more after surgery (59.7%). 87 female patients underwent surgery. From those, 5 did not have a proper follow-up after surgery. Among the 82 remaining, 67 are alive 5 years or more after surgery (81.7%).
Rehabilitation of a laryngectomyRehabilitation process must start before surgery when histological diagnosis of lesion becomes known. Patient should be informed on disease origin, which is not benign any longer, and on larynx removal surgery. At first, patients can become anxious and might show a little of resistance, but having a clear explanation and being aware of healing results, they take the Idea of surgery easily. Parents' relatives should take part of this awareness, though they are the ones who will be with the patient afterwards, without ignoring post-surgery situation. Patient will only be aware of his/her disability when back to everyday life with family and friends.
It is important to mention that patient will lose their natural voice due to larynx removal, but recovery has a great chance to be achieved with a proper rehabilitation. It is also essential an explanation of how larynx produces its sound in order to articulation of voice in the mouth, and in what esophagus voice consists of. From all his explanation, patients will understand how professionals (speech doctors) will instruct them to dominate this technique used by those who underwent such surgery. Patience, perseverance and much training are important and patient cannot be discouraged if results are not achieved successfully at the beginning of the rehabilitation process. The presence of another patient almost healed would be worthy, so the newly operated patient would be able to see how communication through esophagus voice is possible. And if patients cannot develop this so-called esophagus voice, they should be informed of prosthesis which will help them to speak.
We performed Stafiere's technique (22), "neoglottis" in 10 patients. All of them could produce a good quality voice. Therefore, some aspirated saliva and even food easily. In 4 patients, it was necessary to close the neoglottis and redo tracheostomy.
Patient should be informed that s/he will have a canula of tracheostomy up to the complete healing of tracheostom and also they will be demonstrated how to clean and exchange canula daily. It should be protected with gauze or something similar. This protection should be kept in the first two months after the removal of canula, though there will be an increase of trachea secretion by cough, and secretion will be in the protector. Tracheostom should be clean with wet gauze repetitively every time there is secretion. Swimming is forbidden for the danger of aspiration. During shower, this protection is also important. Some patients make use of a plastic protector covering all anterior neck area. In the first months there is a reduction on smelling and taste. After discharge, patient must visit doctor monthly during the first year and every 2 months in the second year. These intervals will become larger up to the fifth year, when meeting doctor will occur once a year.
Prophylaxis ProceduresAll prophylaxis procedures for laryngeal cancer are important.
The main ones are: a) quit smoking, one of the main irritant that makes changes on the epithelium with malignant lesions; b) reduce alcoholic drinks, not only for its local irritant action but also for its weaken effect; c) avoid working in highly polluted places; d) treat patients with malignant larynx lesions, such as: hyperkeratosis, adult papilloma; e) dysphonia or hoarseness, more frequent symptoms when glotttic tumors (all patients who become dysphonic for more than two weeks with no apparent cause); f) any difficulty on deglutition and blood expectoration are signs which deserve special attention; g) nodes or any hardening on neck tissues.
The first doctor, if a specialist, who will assist one of these patients, will perform an indirect laryngoscopy. A direct procedure, under general anesthesia, will be the next step in order to collect material for histological exam when observing any suspicious lesion. If first doctor is not a specialist, s/he must send patient to one. The agility when taking such procedures is essential, though voice will be preserved if any partial resection possibility.
Acknowledgments - We would like to thank Dc Paulo Pernambuco, General Surgeon (in memoriam) and Dc. Flavio Aprigliano Filho, Head and Neck Surgeon, who helped us not only during surgery, but also after surgery care.
BIBLIOGRAPHY1. Haast, MH, Applied embriology of the larynx. Canadian Journal of Oto-Laryngology 1975;4:412-416.
2. Tucker, GF. The anatomy of the laryngeal cancer- Workshop from the Centenial Conference of Laryngeal Cancer. NewYork: Appleton Century Crafts; 1976:11-25.
3. Alonso, JM. Conservative surgery of the cancer of the larynx. Trans. Amer. Acad. Ophtalm. and Otolaryngology 1947;51:633-642.
4. Bocca E, Pignataro I, Mosciano O. Supra-Glotic Surgery of the Larynx. Ann. Oto Laryngology 1968;77:1005-1026.
5. Burstein ED, Calcaterra C. Supraglotic Laryngectomy: series report and analysis of results. Laryngoscope 1985;95:833-836.
6. Auerbach, C. Hammond,EC, Garfinkel, L. Histologic Changes in the Larynx in relation to smoking habits. Cancer 1970;25:92-104.
7. Broders, C. Carcinoma in situ contrasted with benign penetrating epithelium. J.A.M.A 1932;99:1670.
8. Altmann, F. et al. Intraepithelial cancer (cancer in situ) of the larynx. Archives of Otolaryngology 1952;56:121-123.
9. Lynch, RC. Intrinsic carcinoma of the larynx with a second report of cases operated on by suspention and dissection. Trans. Amer.Laring. Ass. 1920;42:119-126.
10. Kleinssaser O, Seiferth L. Microlaringoscopia y Microcirurgia Endolaringea Barcelona, Editorial Cientifico-Medico; 1968.
11. Aprigliano Filho F. Carcinoma in situ da laringe. Tese apresentada a Faculdade Medicina da UFRJ para a obtenção do grau de Mestre, Rio de Janeiro; 1987.
12. Mac Gravan, MH et al. The incidence of cervical lymph node metastases from Epidermoid Carcinoma of the Larynx and their relationship to certain characteristics of the primary tumor. Cancer 1961;14:55-66.
13. Kleinssaser, O. Tumors of the larynx and hypopharynx. New York: Thieme Medical Publications; 1988:87-88.
14. Leroux Robert, A. Statistical study of 620 Laryngeal Carcinomas of the Glotic region, personally operated upon more than five years ago. Laryngoscope 1975;5:1440-1452.
15. Gluck T, Soerensen Y. Handbuch der Speziellen Chirurgie des Ohres und Oberen Luftwege. Wurzburg: 1911;1-70.
16. Aprigliano, F. Use of the nasogastric tube after total laryngectony. Is it truly necessary ? Ann of Oto Rhino and Laryngology 1990;99(7):513-514.
17. Bonneau, RA, Lehman, RH. Stomal Recurrence following Laryngectomy. Archives of Otolaryngology 1975;101:408-412.
18. Halfpenny, W, MacGurk, M. Stomal recurrence following temporary tracheostomy. J. Laryngology Otol 2001;115:202-204.
19. Rockley, TJ, Powell, J, Robin, PF, Reid, AP. Post Laryngectomy stomal recurrence: Tumor implantation or paratracheal lymphatic metastasis? Clin Otolaryngology 1991;16:43-47.
20. Gluckman, JL, Hamaker, RC, Schuller, DE, Weissler, MC, Charles, GA Surgical salvage for stomal recurrence a multi-instituticional experience. Laryngoscope 1987;97:1025-1029.
21. Papazouglou, G, Doundoulakis, G, Terzakis, G, Dokianakis, G. Pharingocutaneous Fistula after Total Laryngectomy: incidence and treatment. Ann. of Oto Laryngology 1994;103:801-805.
22. Staffiere M, Serafine I. La reabilitazione Chirurgica della voce e della Respirazione dopo Laringectomia Totale. Bologna: Atti del XXIX Congresso Nazionale; 1976.
1. Teacher of Bronchoesophagology - Federal University - Rio de Janeiro.
2. Current Responsible for Peroral Endoscopy and Head and Neck Surgery - Bonsucesso Hospital - Rio de Janeiro.
This study was done at Bonsucesso General Hospital (Healthy Department).
Mail address: Flavio Aprigliano - Rua Almirante Tamandaré 32 - Apto 501 - Flamengo - CEP 22210-060 - Rio de Janeiro / RJ. Phone: (021) 2225-1546 - Fax: (021) 2225-5037.
Article received on February 10, 2006 and accepted on February 24, 2006.